Revision arthroplasty with ORIF
1. Principles and strategy
It is important to reconstruct a stable hip joint and to achieve rigid stem fixation in the distal fragment. Restoration of leg length, alignment, and rotation are equally important.
The arthroplasty revision should be preferably addressed first to reconstruct a stable hip joint. Internal fixation is then performed to reestablish bone stock.
2. Approach
The surgeon should use the surgical approach that is the most familiar to him/her for any total hip arthroplasty, such as:
- Anterolateral approach
- Direct anterior approach
- Iliofemoral (Smith-Petersen) approach
- Posterolateral approach
- Trochanteric osteotomy
- Extended trochanteric osteotomy
An extensile approach is necessary to access the fracture site for reduction and placement of additional fixation devices, such as cerclage wires, cables, strut graft, and/or plates.
These approaches can be performed with the patient in a lateral or supine position.
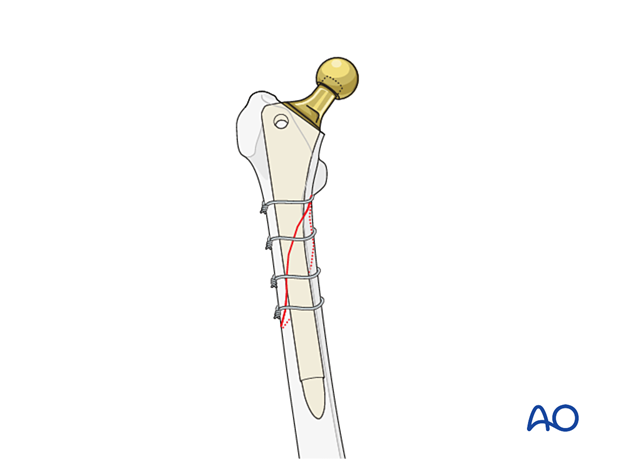
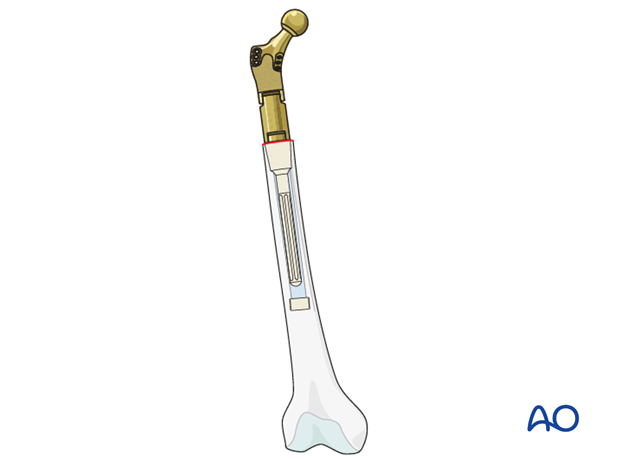
3. Revision arthroplasty
Different options are available based on surgeon's preference and classification of periprosthetic fractures:
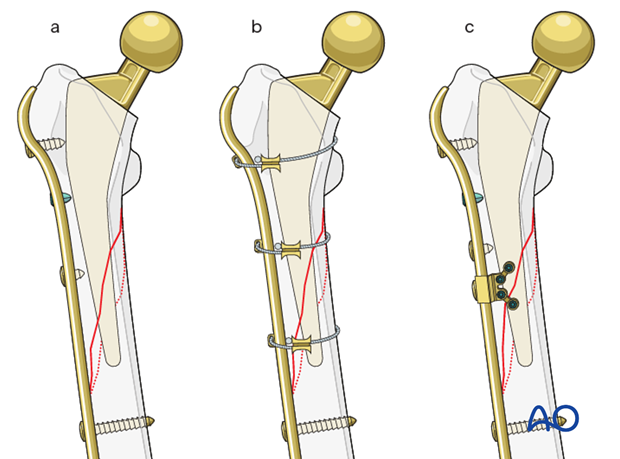
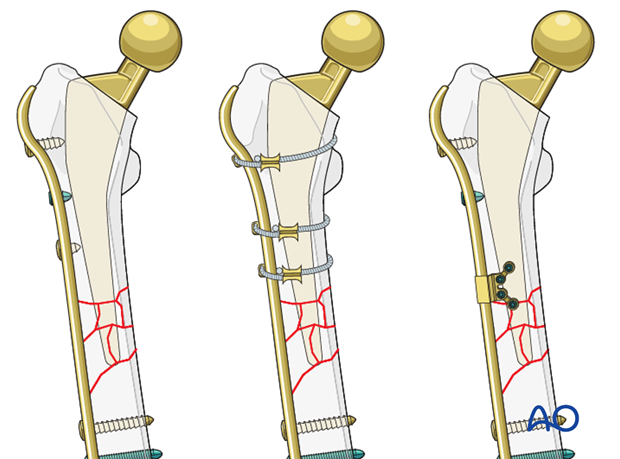
4. Fixation (ORIF)
Different options are available based on surgeon's preference and fracture pattern:
5. Aftercare following a femoral revision
Physiotherapy guidelines
Routine physiotherapy protocols for elective total hip arthroplasty is followed.
Early mobilization is recommended. Weight bearing status is individualized based upon fixation and implant stability.
Hip dislocation precautions are given to the patient.
Imaging
Postoperative radiographs can be made at 2 to 3 weeks to determine maintenance of satisfactory fracture reduction and fixation, no evidence of stem subsidence, or fracture displacement.
Follow-up radiographs can be made at 6 to 8 weeks after surgery to determine sufficient fracture fixation to increase the weight bearing status, and physical activities.
Future follow-up is similar to the routine and standard protocol for total hip arthroplasty.