Direct anterior approach
1. Preliminary remarks
The anterior approach provides the most direct access to the anterior aspect of the hip. Many surgeons prefer this approach for reduction of femoral head and neck fractures. Often the primary surgical approach can be utilized for treatment of periprosthetic fractures. This is considered a greater challenge from the direct anterior approach, however it can be easily extended to perform most fracture surgeries effectively, while maintaining the posterior capsule and short external rotators.
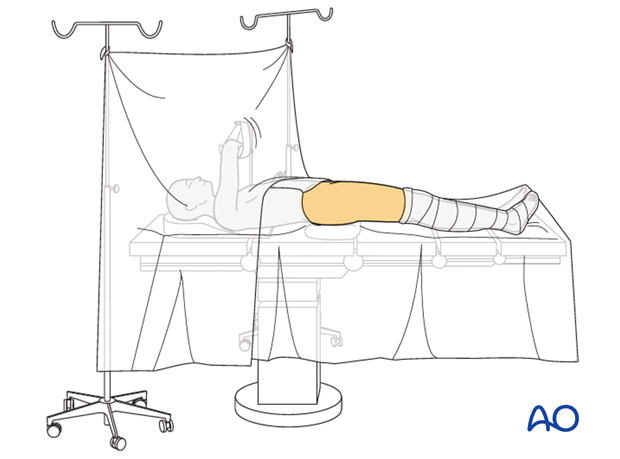
2. Table and positioning
Standard table or Orthopaedic specialty table can be used depending on surgeon preference.
The ipsilateral upper extremity is prepared across the chest on a well-padded bolster.
The sterile field should include the xiphoid process to the pubic symphysis and the entirety of effected extremity.
If an orthopedic specialty table is utilized, care should be taken to include the possible extensions of this approach within the sterile field. This typically extends to the linea aspera posteriorly.
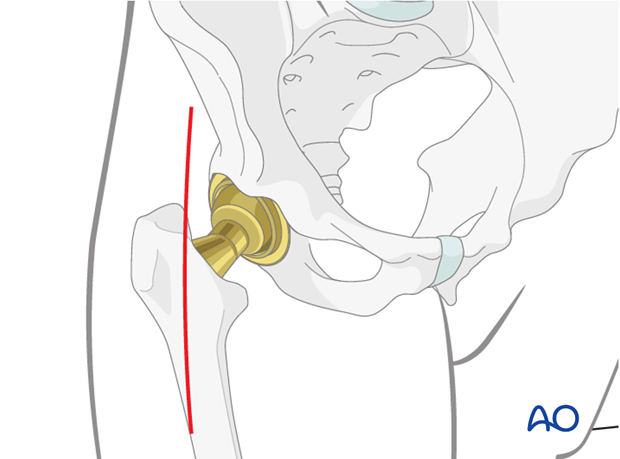
3. Skin incision
A standard approach the hip joint is performed through a 10 cm incision extending over the tensor fascia latae from the ASIS towards the lateral epicondyle. It represents the distal vertical limb of the Smith-Petersen approach.

4. Deep dissection
After incision of the skin and fat, the deep fascia is encountered.
An incision is made over the TFL and the musculature is dissected off of the medial fascia bluntly and a retractor is placed around the superior aspect of the neck of the femur.
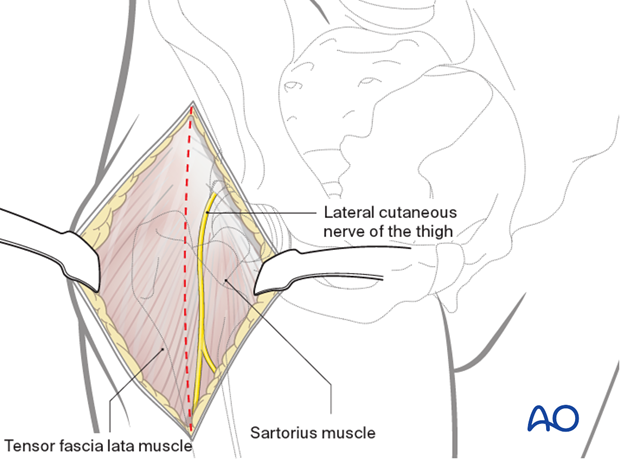
The lateral femoral cutaneous nerve of the thigh should be protected within the sartorial fascia. It might perforate the fascia prematurely and have branches within the subcutaneous fat that should be identified.
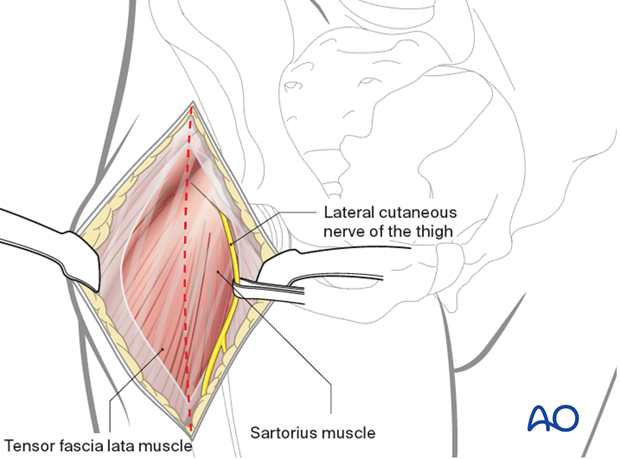
5. Deep surgical dissection
Lateral femoral circumflex vessels are isolated and coagulated. The fascia overlying the rectus can then be opened and blunt dissection carried across the anterior capsule. A blunt retractor is then introduced on the medial aspect of the femoral neck outside of the hip joint.
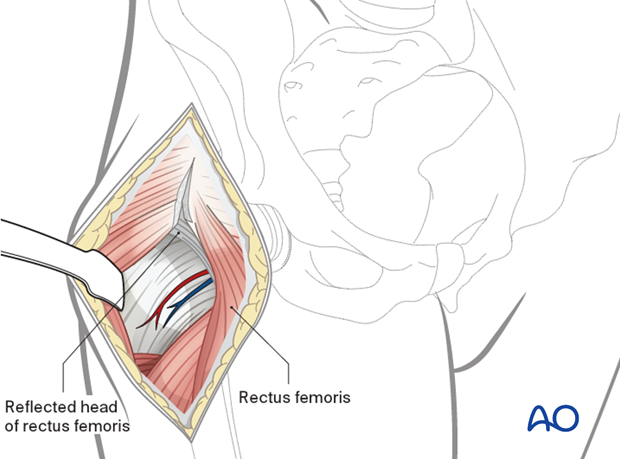
A T-shaped capsulotomy, with stay sutures medially and laterally, allows exposure of the femoral head and neck. The direct head of the rectus femoris can usually be maintained over the top of the hip capsule but some surgeons might choose to divide it with the capsule and reapproximate it at the conclusion of the surgery.
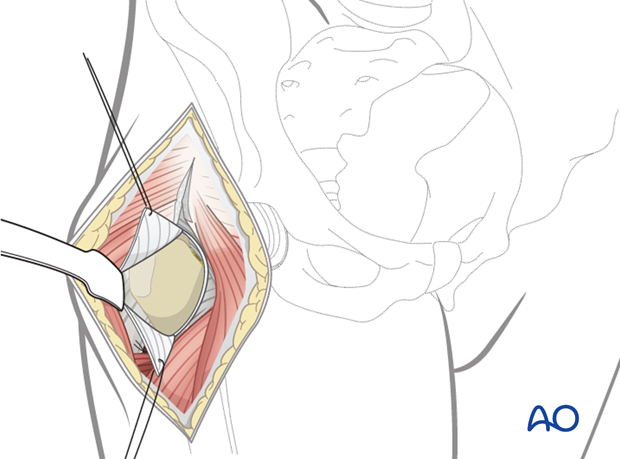
The joint can be dislocated at this time using traction and external rotation in extension. The acetabulum can then be exposed. In order to do this, the rectus femoris tendon should be incised allowing for reflection of the muscle belly from its position over its anterior aspect over the hip joint and acetabulum. Limitations of exposure of the acetabulum includes some posterior wall and column fractures. The ilium can be exposed from the gluteal pillar anteriorly along the outer table to the level of the superior pubic ramus.
The proximal aspect of the femur can be exposed along the calcar and remnant femoral neck with hip extension and external rotation. A bone hook can be utilized to elevate a proximal femur within the wound, and hand-held retractors can be used to further visualize the zone of interest.
In marked internal rotation, the greater trochanter can be visualized and exposed for potential reduction and internal fixation.
6. Extension of surgical approach
Periprosthetic Femur Fracture
The incision can be extended distally on the lateral aspect of the proximal femur and fascial incision brought laterally. The vastus lateralis can then be either released from its origin on the intertrochanteric ridge or retracted bluntly to allow for visualization of the proximal femur. With the hip dislocated the prosthesis can be removed or the maintained and fixation of the proximal femur can be carried out via described techniques.
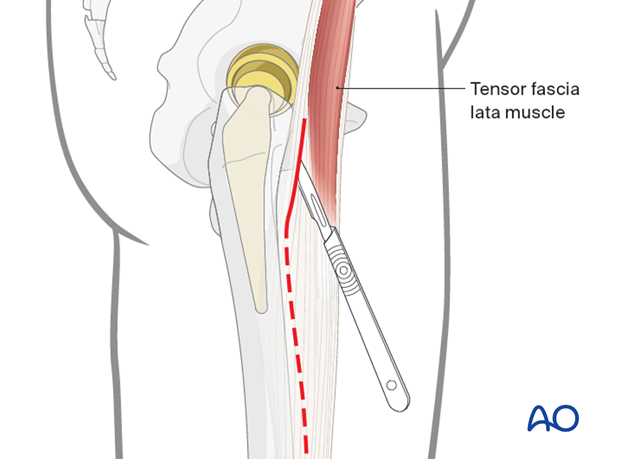
Extended trochanteric osteotomy
If stem extraction requires an osteotomy either due to ingrowth or presence of cement, this can be performed through the extension of the direct anterior approach.
With the limb markedly internally rotated, drill holes can be placed from the posterior cortex to the anterior cortex across the lateral aspect of the stem to a point 1 cm distal to the femoral prosthesis or cement mantel.
An osteotome can then be used to connect these drill holes such that the greater trochanter is elevated anteriorly off of the femoral component with the lateral cortex of the femur.
7. Closure
A layered closure following irrigation is preferred for periprosthetic fractures. The capsule of the hip, if it has been maintained, should be closed using non resorbable sutures. The rectus femoris tenotomy can be repaired followed by a watertight closure of the fascia. A subfascial drain should be considered as blood loss can be significant and periprosthetic fracture patients are at high risk of requiring anticoagulation immediately postoperatively. A hematoma requiring evacuation must be avoided. The wound is closed in layered fashion according to the surgeon's preference.
Sterile dressing should be applied, and negative pressure incisional wound care can be considered.














