Bridge plate and screw fixation
1. Principles
Comminuted periprosthetic fractures in the setting of stable total hip arthroplasties require techniques like those that would be employed for a fracture of the femur without a prosthesis. The difficulties include fixation and bone stock. The goals of surgical intervention are to maintain a competent total hip arthroplasty and to achieve healing of the fracture zone.
Comminuted periprosthetic fractures in the setting of stable total hip arthroplasties are exceedingly rare. However, when they do occur it typically involves a proximal ingrowth prosthesis with comminution about the stem distally.
It is important to review prior radiographs of the total hip replacement to evaluate whether or not the stem is stable.
2. Approach
Direct lateral approach
Direct lateral approach to the femoral diaphysis is typically utilized. This can be performed in a minimally invasive fashion for some fracture patterns and proximal and/or distal extension of deep surgical approach can be utilized in a fracture specific manner.

Other approaches
Other approaches that can be used to perform this procedure are:
- Anterolateral approach
- Direct anterior approach
- Iliofemoral (Smith-Petersen) approach
- Posterolateral approach
- Trochanteric osteotomy
- Extended trochanteric osteotomy
These approaches can be performed with the patient in a lateral or supine position.
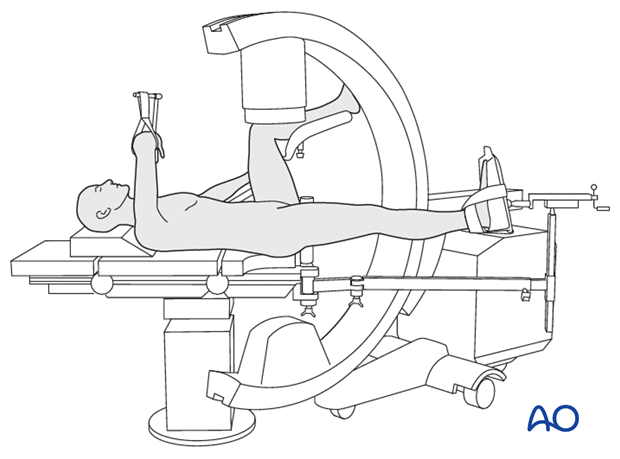
Option: use of a radiolucent or fracture specific table
A radiolucent table or a fracture specific table may be used.
The choice depends on surgeon experience and preference. The control of the fracture may often be more difficult on a traction table.
3. Indirect reduction
Distal femoral skeleton traction or table traction is critically important for restoration of limb length and rotation.
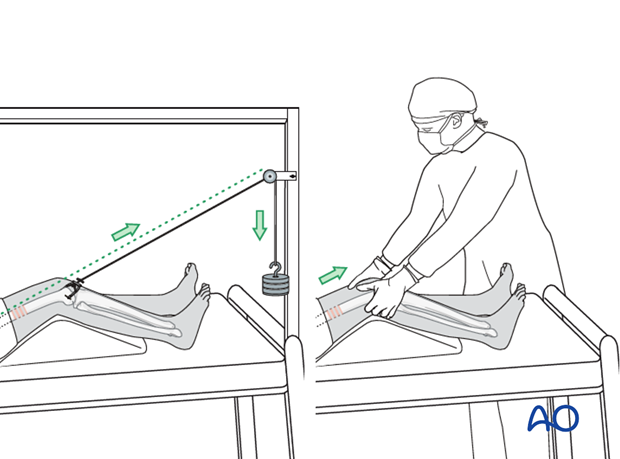
Reduction techniques
Adjunctive methods of reduction include: the utilization of a large femoral distractor, or a push-pull technique.

Reduction tools include percutaneous bone hooks, ball spike pusher, and Hohmann retractors.
For additional details about indirect reduction please refer to the femur shaft section of the AO Surgery Reference.
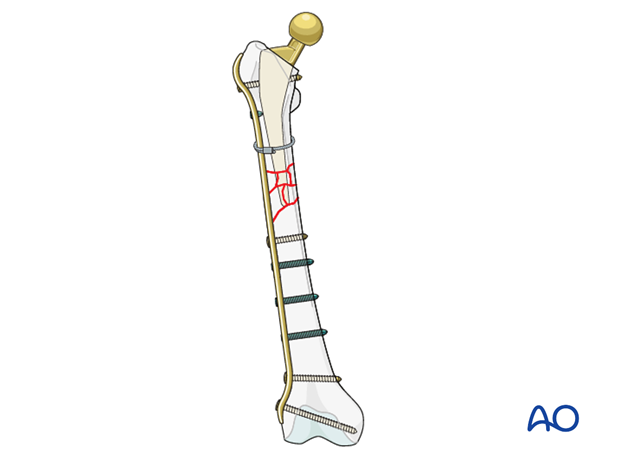
4. Fixation
Implant selection
A plate with locking screw options and a sagittal bow is typically used.
Depending on the fracture type and bone quality, extension to the distal or proximal femur may be desired.
Critical to plate selection is to not leave any area of the bone unprotected.

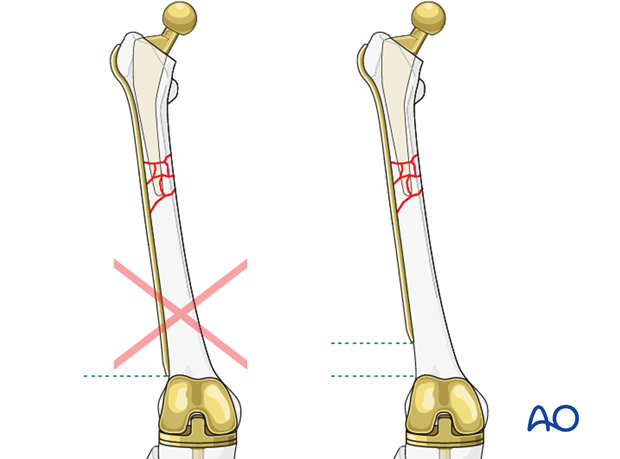
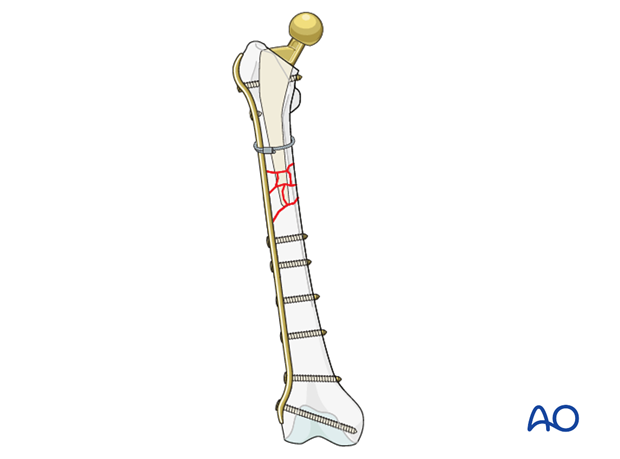
Plate application
The plate can be applied to the bone on the lateral cortex utilizing nonlocking screws. Multiple adjunct methods can then be used to achieve hybrid fixation.
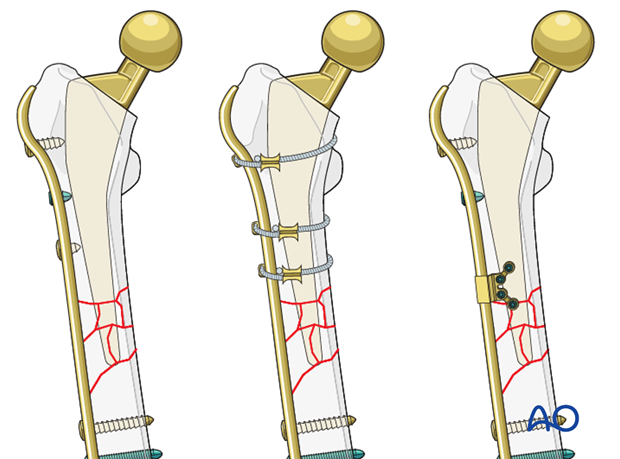
Options for additional stability
Additional stabilization can be achieved with locking and nonlocking screw fixation above and below the fracture site. Around the femoral stem, if there is no room for bicortical screw fixation, the options include:
- Unicortical locking screw fixation
- Cerclage cables integrated into the plate
- Locking attachment plate
Note: Attachment plates require small fragment locking screw fixation
For additional details on these implants please refer to adjunct plate options.
5. Aftercare following ORIF
Postoperative management
Postoperative management should include careful monitoring of hematocrit and electrolytes particularly in the elderly patients.
Postoperative IV antibiotics should be administered up to 24 hours.
Consideration should be given to anticoagulation for a minimal course of 35 days. If there are thromboembolic complication this treatment is extended.
Drains can be discontinued when output is less than 30 to 50 cc per 12 hours.
Patient mobilization
Immediate mobilization of the patient should commence. If fracture stability will allow, the patient should be made weight bearing as tolerated as soon as possible. Long periods of limited weight bearing are extremely detrimental to patient recovery.
Wound healing
Avoidance of edema postoperatively is critical for both wound healing and patient mobilization. This can be aided by pneumatic compression devices. If negative pressure wound therapy is utilized, it can be discontinued after 5 to 7 days. Staples or sutures are typically removed at 14 to 21 days.