Revision of cup to multihole pressfit cup with augments
1. Principles
Cup fixation stability is critical to ensure durable fixation.
One of the goals is to minimize fracture progression and comminution.
For further information about standard techniques for ORIF in native acetabular fractures, please refer to the acetabulum section of the AOSR.
Cup stability
Cup stability is determined by visual and manual examination.
Intraoperative X-ray should be utilized.
Removal of the cup should be considered if there is any question about stability.
2. Approach and exposure
The surgical management of these periprosthetic acetabular fractures involves using the standard surgical approaches for total hip arthroplasty, such as:
- Anterior intrapelvic approach
- Anterolateral approach
- Direct anterior approach
- Posterolateral approach
- ASIS osteotomy
- Kocher-Langenbeck approach
- Ilioinguinal approach
These approaches can be performed with the patient in lateral or supine positioning.
The surgeon should have full visualization of both the anterior and the posterior walls/columns of the acetabulum. This is critical to fully assess the extent of the fracture lines and patterns.
This would also allow for the most safe and efficient removal of the failed cup.
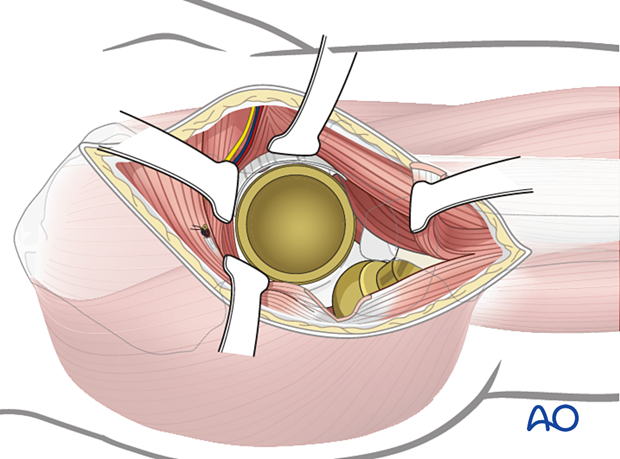
Take care to protect the neurovascular structures that are at risk, such as the sciatic nerve, and those structures in the greater sciatic notch.

3. Cup removal
Liner removal
The cup liner is removed prior to cup removal.
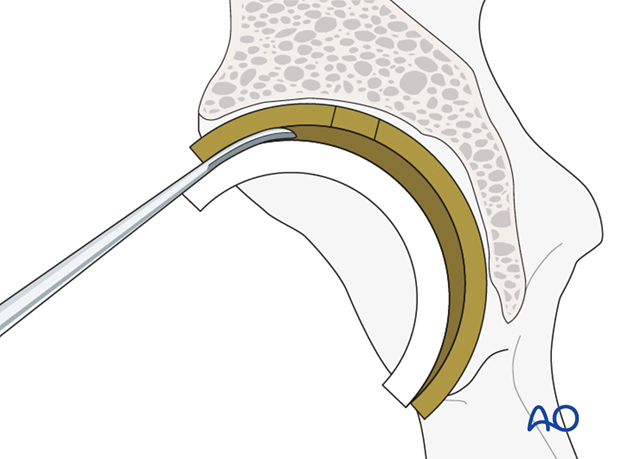
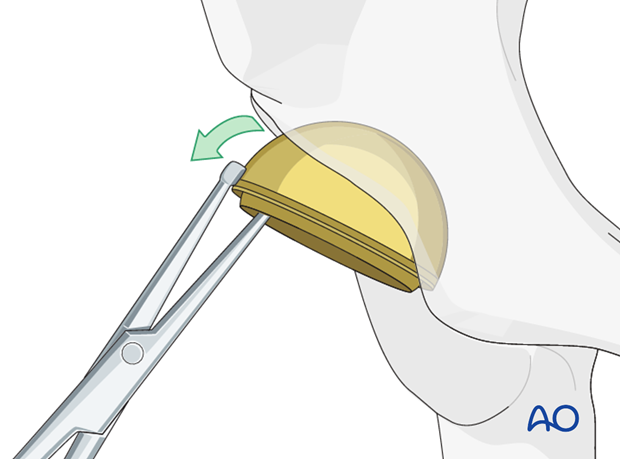
Acetabular component removal
The acetabular component is removed. Details on how to remove an acetabular cup, and any associated screws, are described in the basic technique for acetabular cup removal.
4. Fracture assessment
Assess the location, stability, and extension of the fracture(s) by visual inspection. If necessary, intraoperative imaging may also be used.
The most common fracture pattern involves the posterior wall of the acetabulum. If the posterior column is not involved, this type of fracture is managed with revision to a multi-hole porous cup.
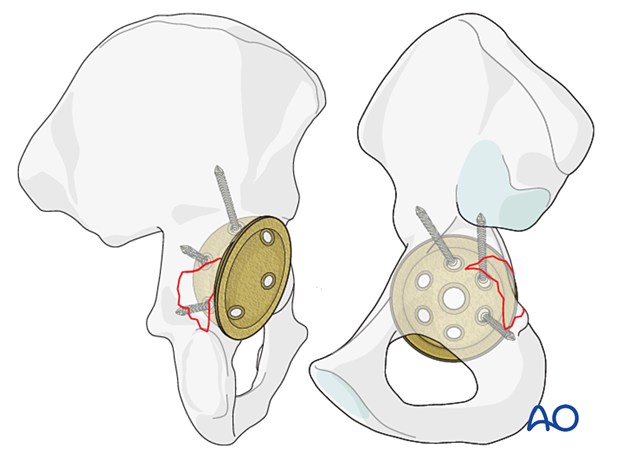
The fracture patterns may be difficult to classify. However, the treatment principles are identical to the management of any acetabular fracture.
It is important to maintain and to reestablish column stability and acetabular containment of the cup.
5. Cup revision and fracture fixation
Restoration of segmental defect(s) in the acetabulum can be performed using bone grafts, metal augments, or in combination.
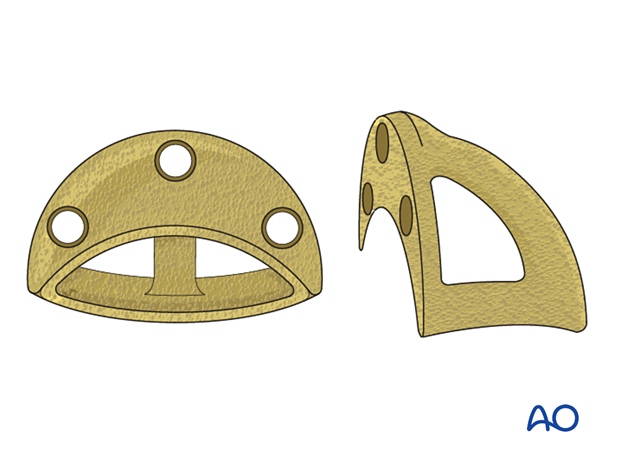
Implant sizing
The surgeon should select the cup size that would provide optimal contact with the anterior and the posterior columns.
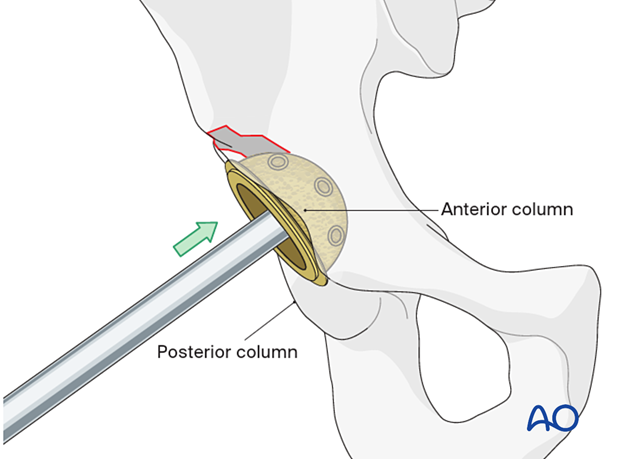
Pitfall: Cup oversizing
The new cup should have stable and sufficient contact with the anterior and the posterior columns. Oversizing of the cup could create fracture extension and displacement without gaining additional cup press-fit stability.
If a significant increase in cup size seems to be indicated (more than one cup size larger than pre-planned), the need of ORIF or augment should be suspected.
Option 1: Metal augment fixation
Restore the acetabulum integrity using metal augment prior to new cup insertion according to the manufacturer's specifications.
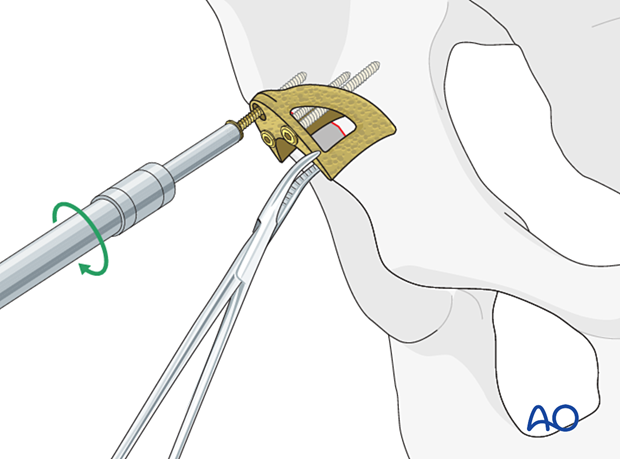
Option 2: Segmental cortical bone graft augmentation
If the surgeon chooses to use bone graft rather than metal augment, the graft may be either obtained from the resected femoral head in primary total hip arthroplasty, or banked allograft inventory.
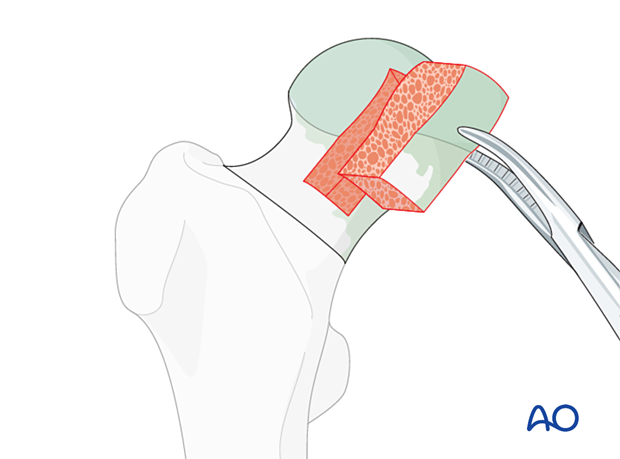
The size and geometry of the graft, autograft or allograft, should be modified to the proper dimensions to augment the defect.
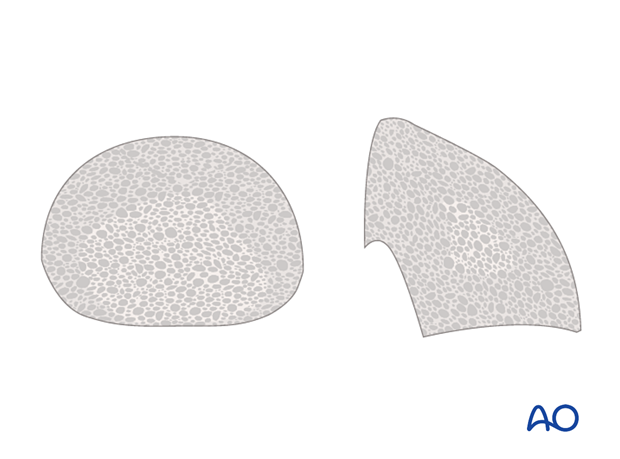
New cup insertion
The new multi-hole cup is inserted into the acetabulum against the augment.
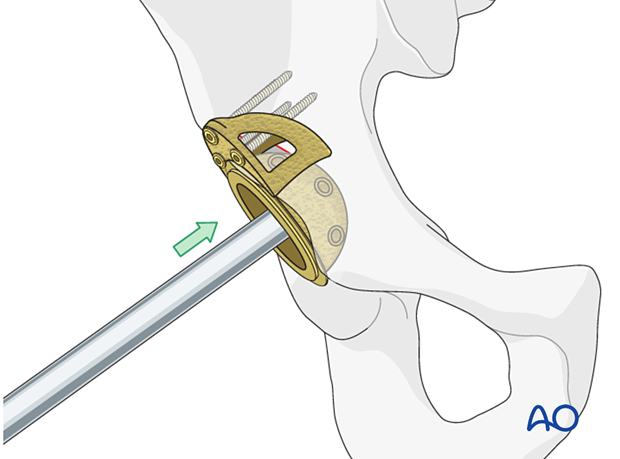
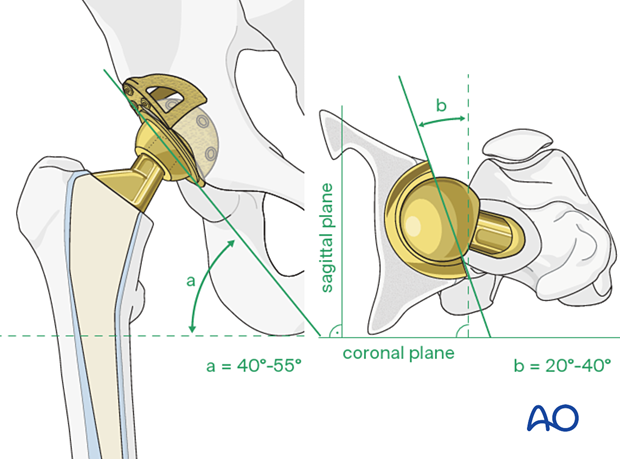
Insert the new cup following the recommended position (inclination) and orientation (anteversion) guidelines.
The accepted "safe zone" is:
- cup inclination 40° to 55° (a)
- cup anteversion 20° to 40° (b)
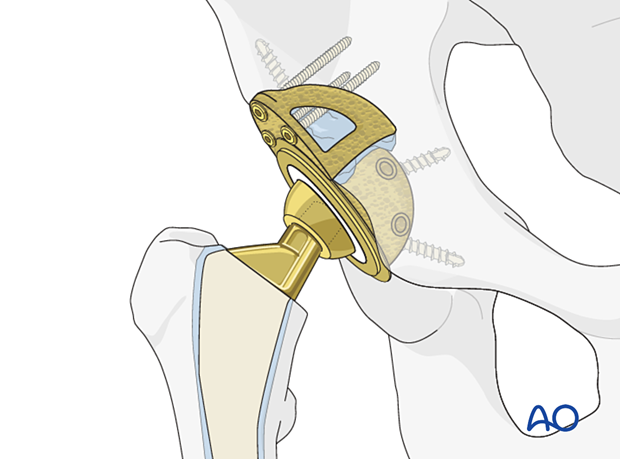
Screw fixation
The cup is secured with multiple screws that than engage both the anterior and posterior columns, on each side of the fracture.
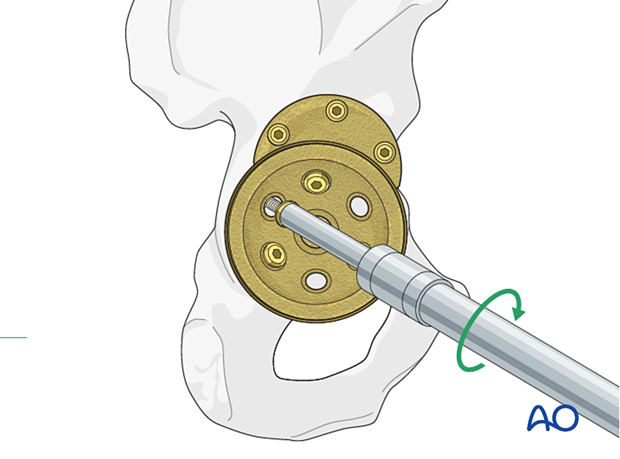
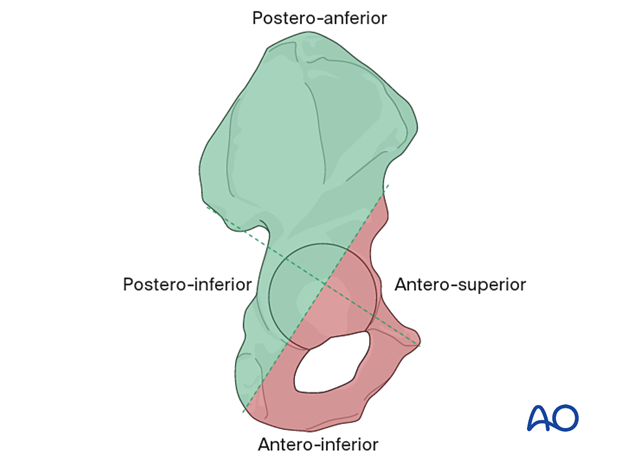
Safe zones for screw implantation
Avoid placing screws into the antero-superior and antero-inferior zones when possible, and towards the medial wall of the acetabulum.
When required, critical evaluation of drill and screw depth is required. Consider oscillation of drill bit to prevent neurovascular injuries.
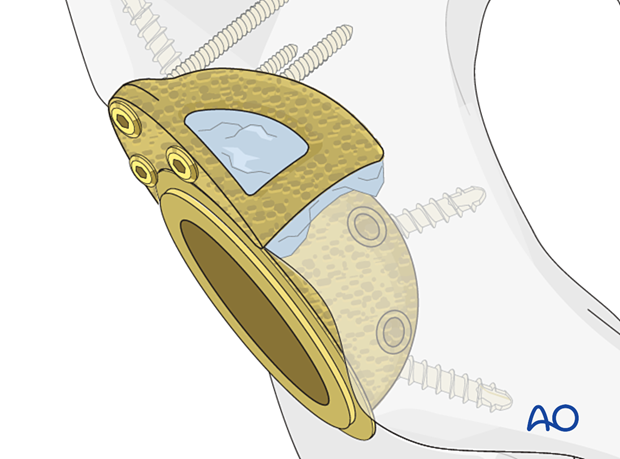
Interface stabilization
The interface between the metal augment and the new cup is stabilized (unitized) with the use of bone cement.
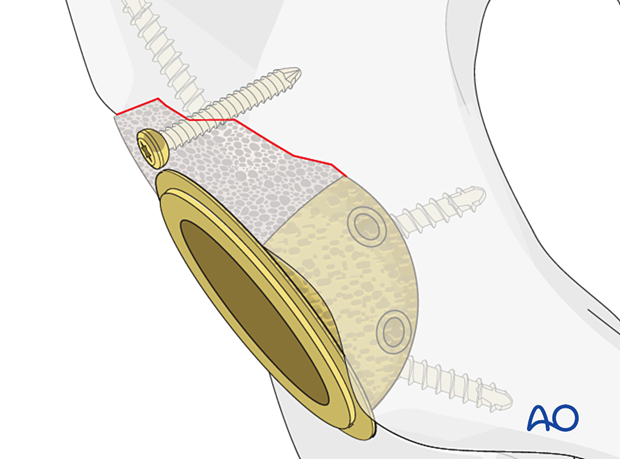
Cement unitization would not be necessary when the structural graft is used.
New liner insertion
The new liner is implanted into the shell using implant system specific instruments.
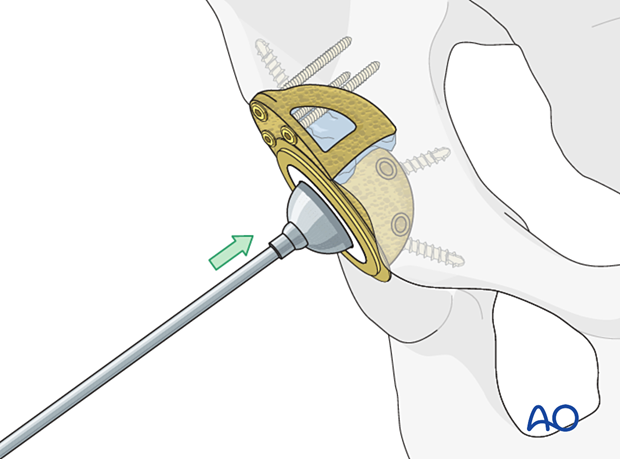
Continue with hip replacement as preoperatively planned.
6. Aftercare following revision to a multihole pressfit cup
Physiotherapy guidelines
Routine physiotherapy protocols for elective total hip arthroplasty is followed.
Early mobilization with protective weight bearing (50%) is recommended for 6 to 8 weeks until sufficient fracture healing.
Hip dislocation precautions must be given to the patient.
Imaging
Postoperative radiographs should be made at 2 to 3 weeks to determine maintenance of satisfactory cup fixation stability and no fracture progression or displacement.
Follow-up radiographs should be made at 10 to 12 weeks after surgery to determine sufficient cup fixation stability and no further fracture displacement to increase the weight bearing status, and physical activities.
Future follow-up is similar to the routine and standard protocol for total hip arthroplasty.













