Anterior Superior Iliac Spine (ASIS) osteotomy
1. Introduction
The Anterior Superior Iliac Spine (ASIS) osteotomy can be performed through the lateral window of an anterior pelvic approach such as:
- Anterior intrapelvic approach plus lateral window
- Ilioinguinal approach
This can be used for ORIF of periprosthetic acetabular fractures or revision arthroplasty.
Scar tissue due to previous exposure might obscure typical landmarks.
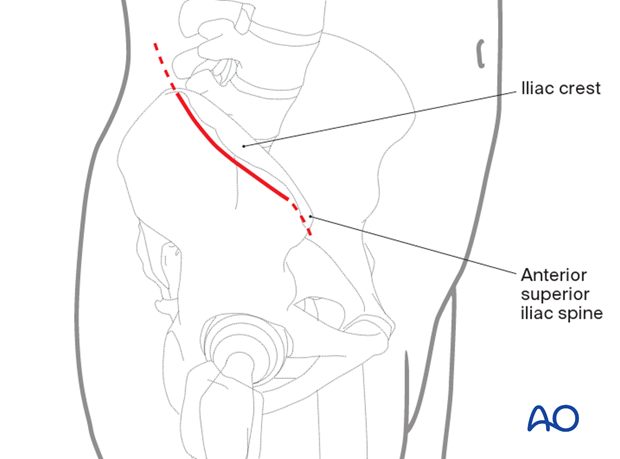
2. Skin incision
An incision is made along the iliac crest. Be aware of the lateral femoral cutaneous nerve in the region of the ASIS. The length of the incision is determined by the amount of area that needs to be accessed in the iliac fossa.
The incision can be extended intraoperatively depending on the necessary exposure.
For fractures involving the posterior aspect of the ilium, or the SI joint, the exposure needs to be extended posteriorly almost to the table.
3. Superficial surgical dissection
Divide the subcutaneous tissues in line with the skin incision in order to expose the fascia overlying the external oblique muscle.
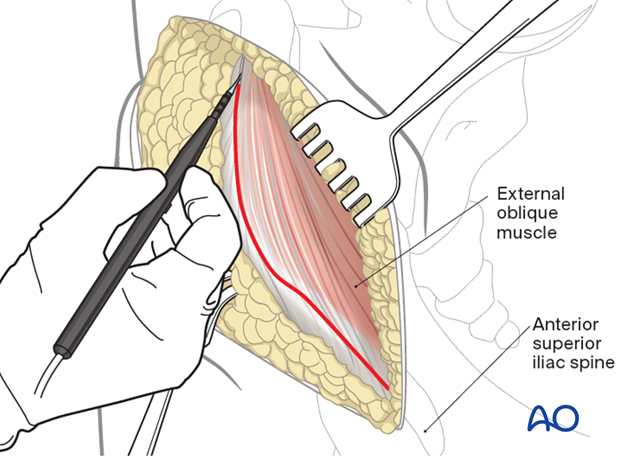
Identify the border between the gluteus muscles and external oblique muscles. Incise the muscular interval with electrocautery.
The external oblique muscle is subperiosteally elevated from the iliac crest.
With a small elevator, the iliac muscles are elevated using the same subperiosteal layer.
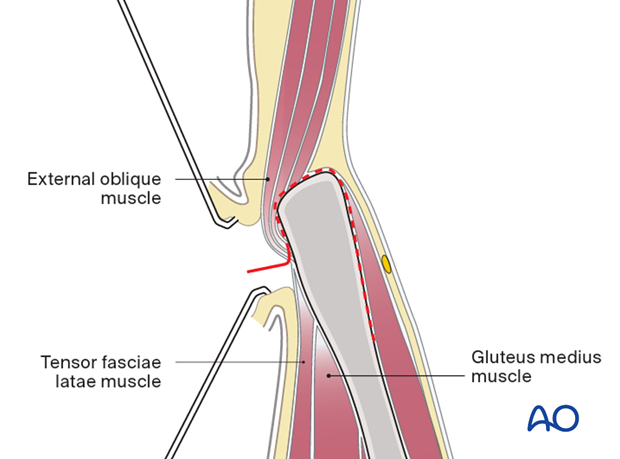
4. Deep dissection
When elevating the iliacus muscle, bleeding from nutrient vessels can occur and should be stopped with bone wax.
Continue with careful blunt dissection to the interior part of the SI joint medially to the pelvic ring.
Proceed anteromedially at the pelvic rim as far as to where the iliopectineal eminence begins.
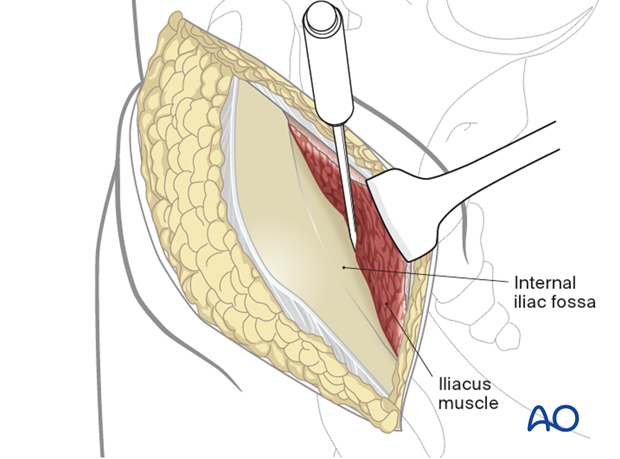
Continue the dissection with an instrument such as a Cobb elevator.
The SI joint capsule should be identified. Place a Hohmann retractor into the superior portion of the SI joint.
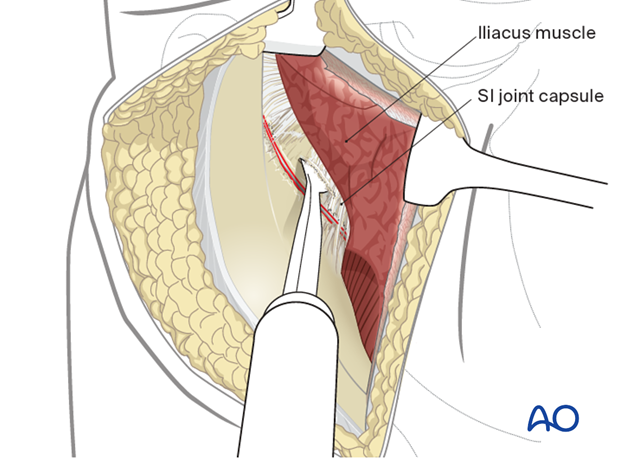
5. Expose the SI joint (if needed)
The dissection is carried further medially as far as the sacral ala, which visualizes the upper part of the anterior column. Move the Hohmann retractor medially carefully onto the sacral ala.
Note the L5 nerve root traversing this region.
Place a second Hohmann retractor more anteriorly on the sacral ala if required.
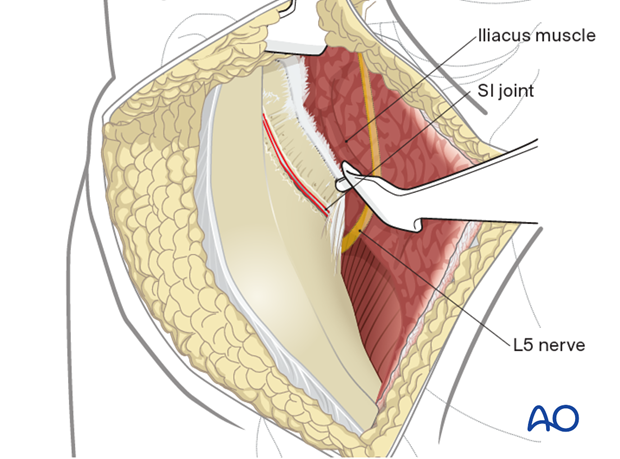
Place an additional Hohmann anterior to the SI joint for additional exposure. Take care when placing this anterior retractor as it may injure the superior gluteal artery and nerve as they exit the greater sciatic notch.
The anterior column as far as the SI joint is now exposed.
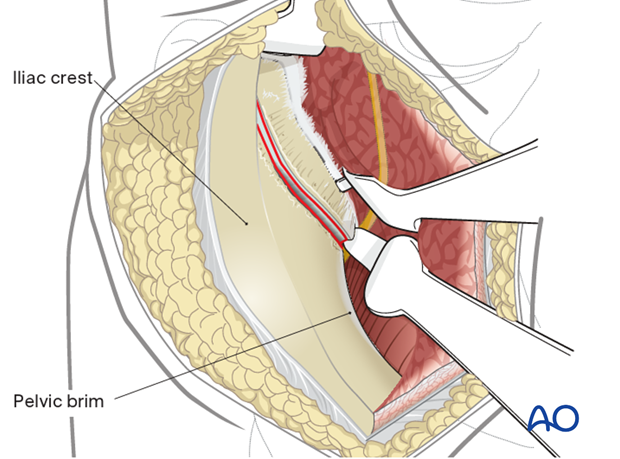
With medial retraction of the abdominal wall and contents, exposure is extended anteriorly towards the ASIS.
Ensure to leave the insertion of the external oblique and sartorius on the ASIS intact.
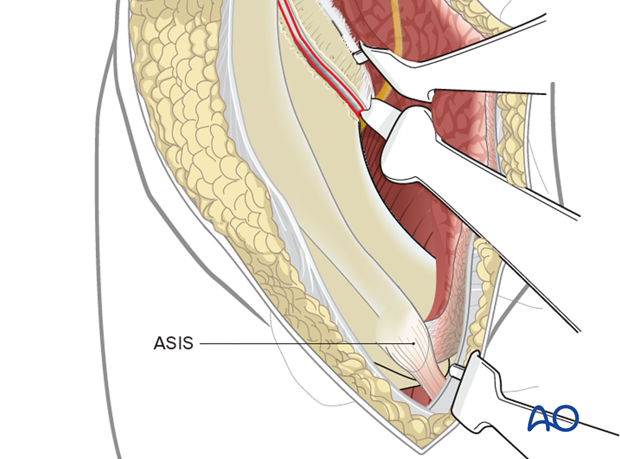
6. Osteotomy
With ASIS exposed, a digastric osteotomy of the ASIS is performed using an osteotome or a sagittal saw.
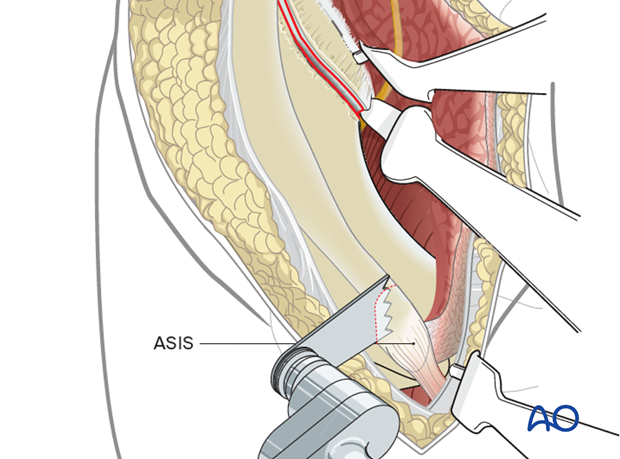
Retract the ASIS along with the sartorius and the external oblique medially to further expose the inner table of the pelvis and pubic root.
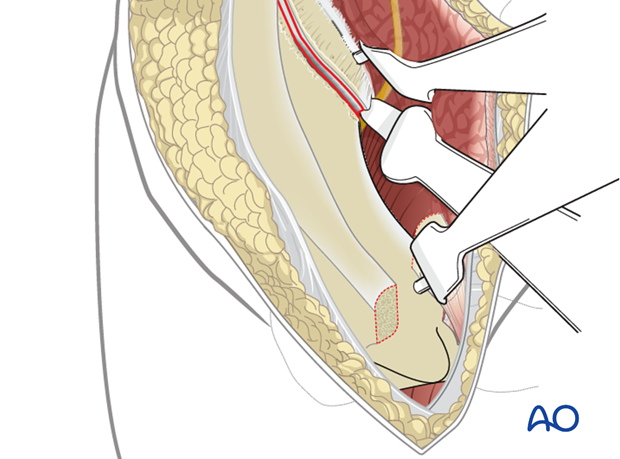
7. Reattachment
The osteotomy is repaired using a single lag screw.
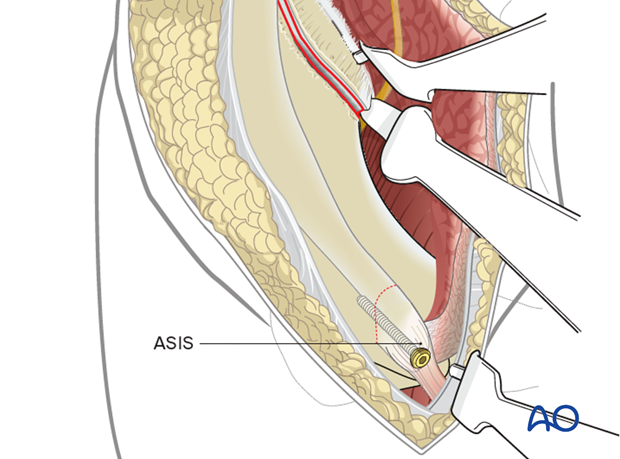
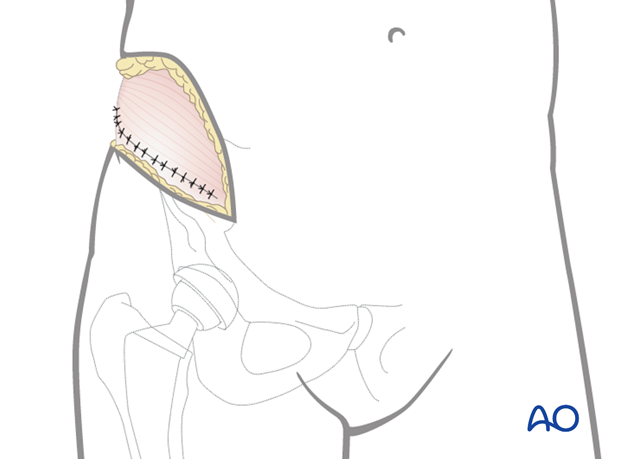
8. Wound Closure
The lateral window is also closed in layers reconstructing the fascial layer preserved in the approach.
These may be performed simultaneously.