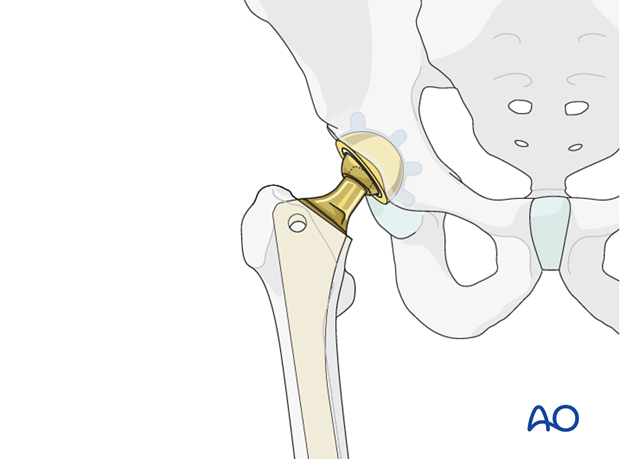
Polyethylene liner revision
1. Principles
It is important to achieve appropriate fracture reduction to restore length, alignment, and rotation and fixation of the femur around the implant.
Revision of the femoral component can require polyethylene exchange or revision of the bearing surfaces to enhance hip stability and improve longevity of the prosthesis.
The goal is to achieve:
- Secure seating and engagement of the new polyethylene bearing into the retained acetabular cup
- Secure engagement of new femoral head on previous femoral prosthesis
2. Surgical strategy
The fracture fixation should be addressed first to reconstruct a stable femur. Revision of the femoral head and polyethylene is then performed to reconstruct the hip joint.
3. Approach
The surgeon should use the surgical approach that is the most familiar to him/her for any total hip arthroplasty.
Extensile approach is necessary to access the fracture site for exposure, reduction, and placement of fixation devices, such as cerclage wires, cables, strut grafts, or plates for fracture fixation.
4. Acetabular cup assessment
Following completion of the stem removal and the femoral canal preparation for the new stem, assessment of the acetabular cup should be done.
The surgeon should assess the position and the fixation stability of the acetabular cup.
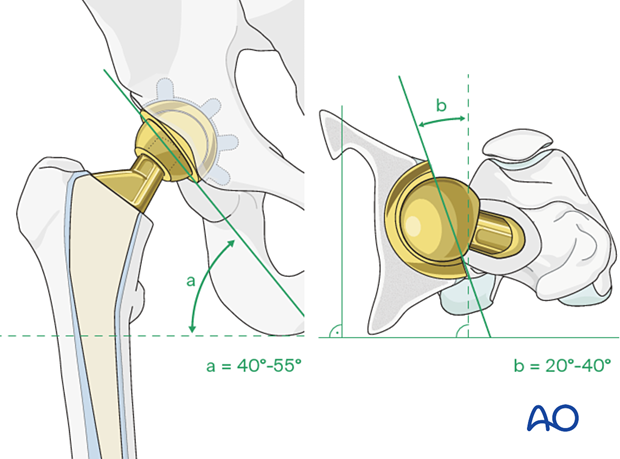
The accepted "safe zone" is:
- cup inclination 40° to 55° (a)
- cup anteversion 20° to 40° (b)
If constrained component is necessary, the cup orientation may need to be modified.
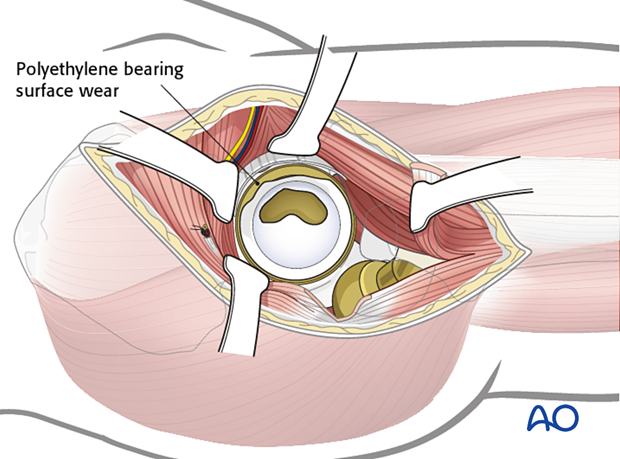
The surgeon should also assess for liner surface wear. If there is significant wear, liner revision should be performed.
5. Femoral head revision
If the femoral stem is not revised, it may be necessary to exchange the head, in order to couple to the acetabular bearing, and to reduce the risk of dislocation after surgery.
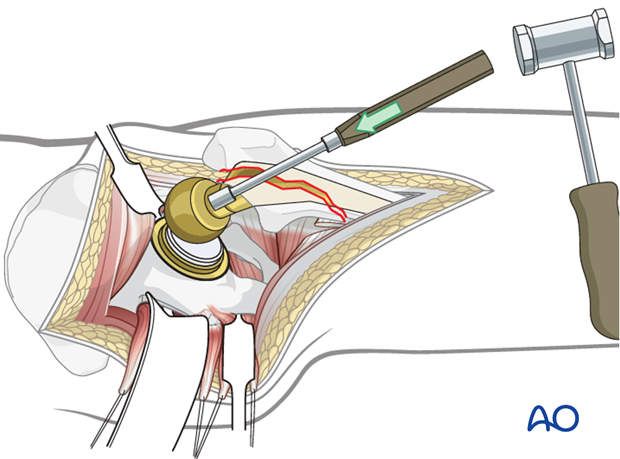
Femoral head removal
The hip is dislocated.
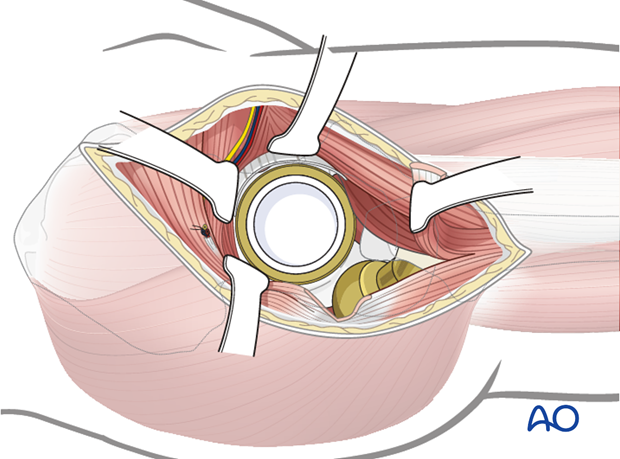
Bone tamp and mallet is used to disengage the femoral head from the Morse taper of the femoral prosthesis.
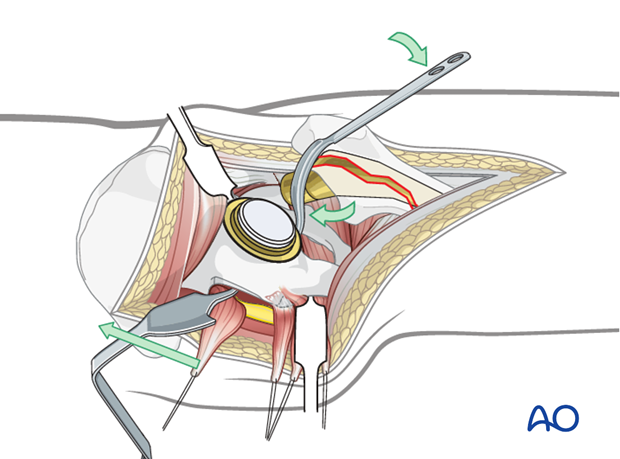
Cup exposure
Following removal of the head, the surgeon can place the acetabular retractors to retract the femur with the femoral prosthesis and to retract the surrounding soft tissues.
Once exposed, debride the scars and the soft tissues covering the polyethylene/acetabular component interface.
6. Polyethylene liner removal
There are two commonly used techniques for liner removal:
- Use of an osteotome at the liner-cup junction to lever and to remove the liner
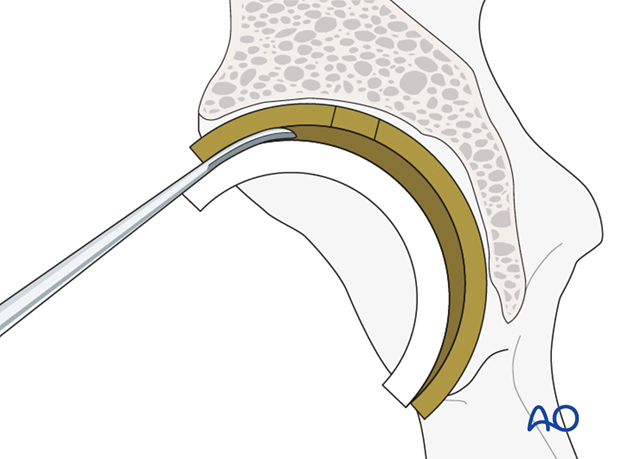
- Use of a threaded extraction tool or cancellous screw to push out the liner
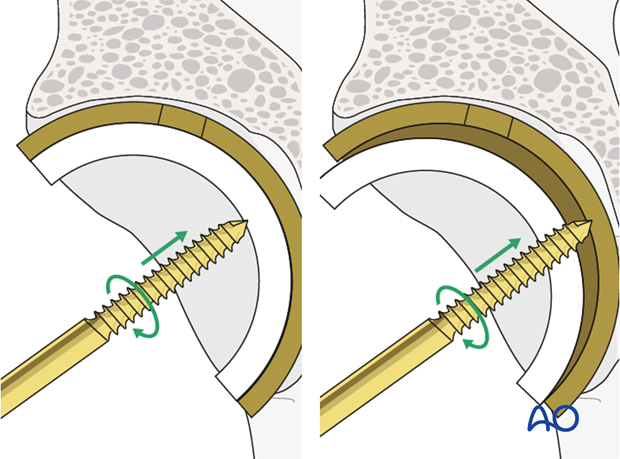
7. New liner selection and implantation
Coupling with the acetabular cup
The new liner must have the correct locking mechanism and geometry for the acetabular cup.
There are different liner options, including material such as the standard polyethylene liner, lipped/offset liner, and ceramic options.
If the locking mechanism is disrupted a new liner can be cemented into the existing acetabular cup.
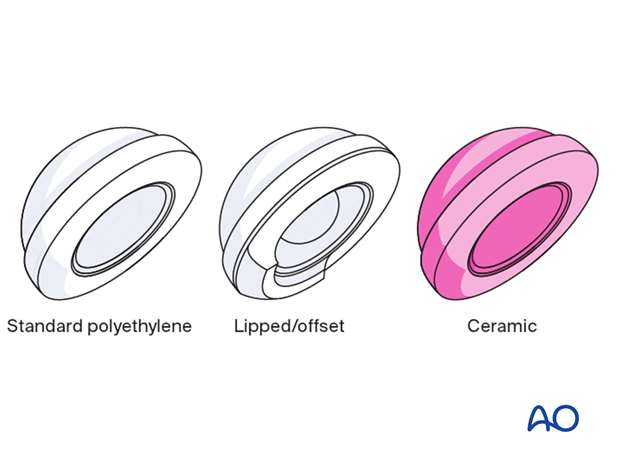
Alternative bearing options
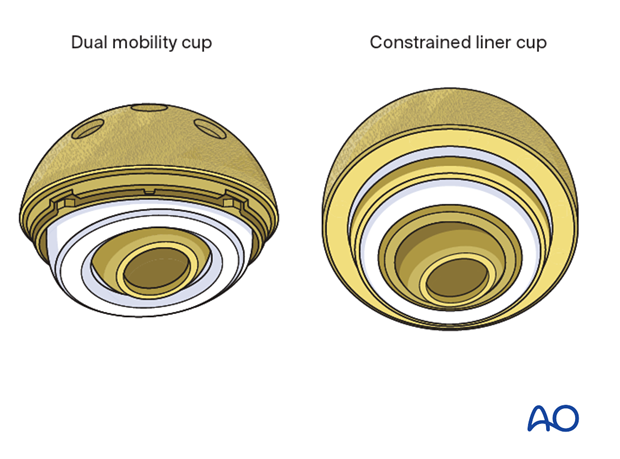
New liner insertion
The new liner is inserted into the cup using implant system specific instruments.
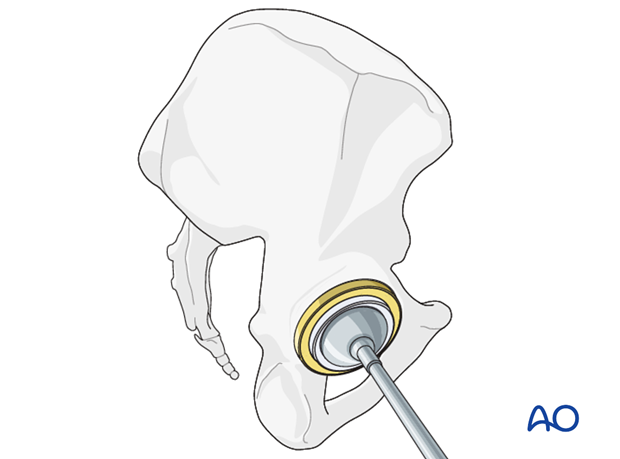
8. Surgical technique of cementation of new liner
If there is no appropriate bearing or the locking mechanism is incompetent, a new polyethylene liner can be cemented into the old acetabular shell.
Trial components can be used to determine the most appropriate size for the retained acetabular cup.
New liner preparation
The backside of the new liner should be scored to allow for proper surface texture for cement fixation.

Cementing technique
Cement mixing is performed following standard protocol for routine hip and knee arthroplasty.
Cement application
Cement is applied to both the liner and the cup.
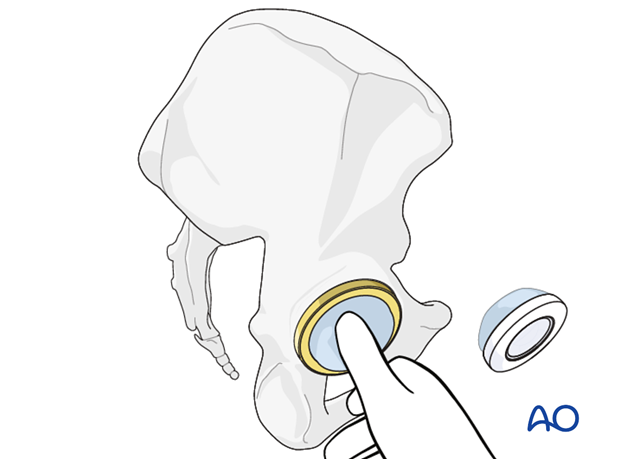
New liner insertion
The liner is inserted into the cup and held in place until the cement hardens.

Hip reduction
Following completion of the liner exchange and insertion of the new stem, the surgeon should do a trial reduction with the proper head (diameter and neck length).
With the hip reduced, confirm the range of motion and hip stability. Adjust the neck and head if necessary.
Once satisfactory, attach the definitive femoral head to the stem, and reduce the hip. Confirm complete reduction, stability, and range of motion.