Compression plate and screw fixation
1. Principles
Unstable simple fractures around or distal to stable femoral stems are amendable to traditional compression plating techniques.
The goal is to create a stable environment for the arthroplasty and for the femoral diaphysis.
These fractures include:
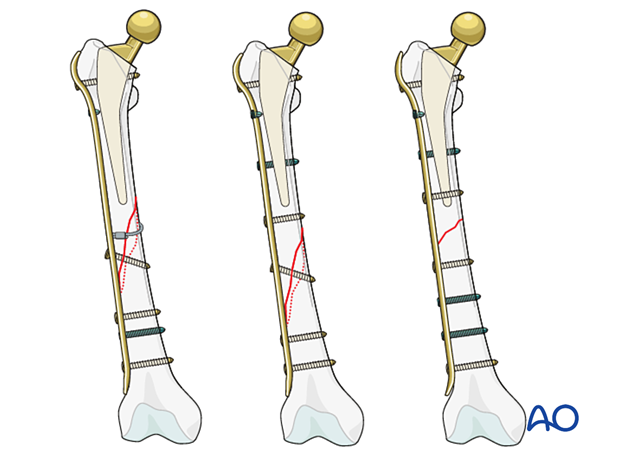
- Short oblique
- Spiral
- Transverse
2. Approach
Direct lateral approach
Direct lateral approach to the femoral diaphysis is typically utilized. This can be performed in a minimally invasive fashion for some fracture patterns and proximal and/or distal extension of deep surgical approach can be utilized in a fracture specific manner.

Other approaches
Other approaches that can be used to perform this procedure are:
- Anterolateral approach
- Direct anterior approach
- Iliofemoral (Smith-Petersen) approach
- Posterolateral approach
- Trochanteric osteotomy
- Extended trochanteric osteotomy
These approaches can be performed with the patient in a lateral or supine position.
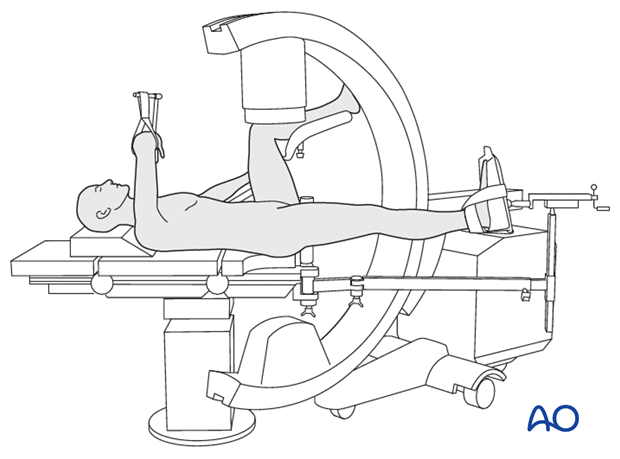
Option: use of a radiolucent or fracture specific table
A radiolucent table or a fracture specific table may be used.
The choice depends on surgeon experience and preference. The control of the fracture may often be more difficult on a traction table.
3. Reduction
Direct reduction
Reduction is typically carried out using a combination of direct and indirect methods. Limb manipulation will help in an indirect manner. Direct reduction with clearance of fracture hematoma and stabilization with pointed bone reduction clamps can then be completed.
The Collinear reduction clamp can be extremely helpful in facilitating reduction. It is applied from the direct lateral incision with proximal extension.
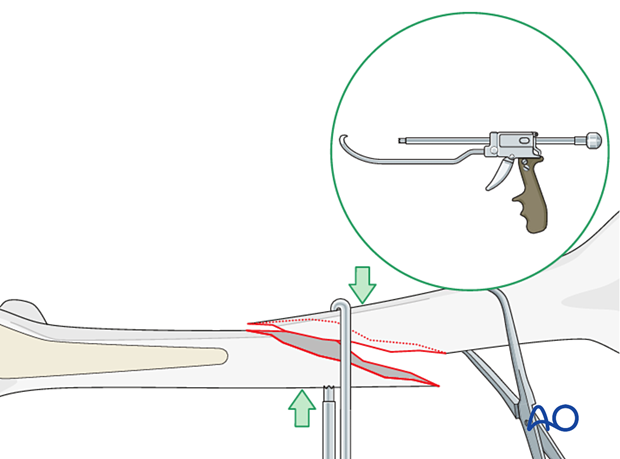
For short oblique or spiral fractures, provisional wire stabilization can be extremely helpful. Care must be taken to avoid applying wires in the pathway of planned definitive stabilization.
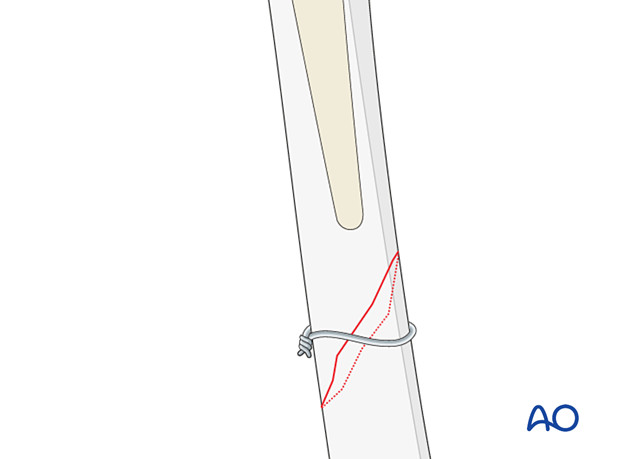
Option: traction aids
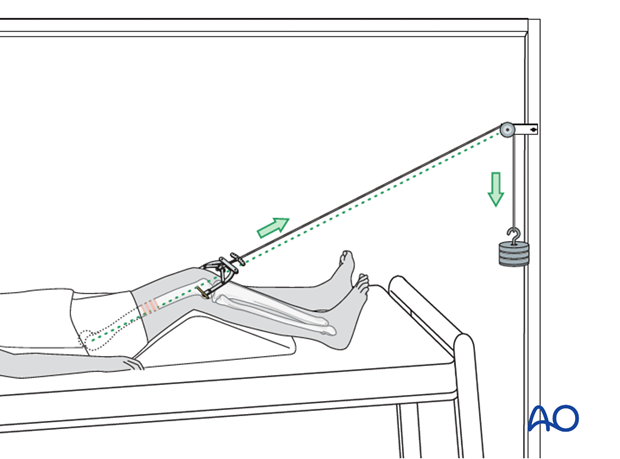
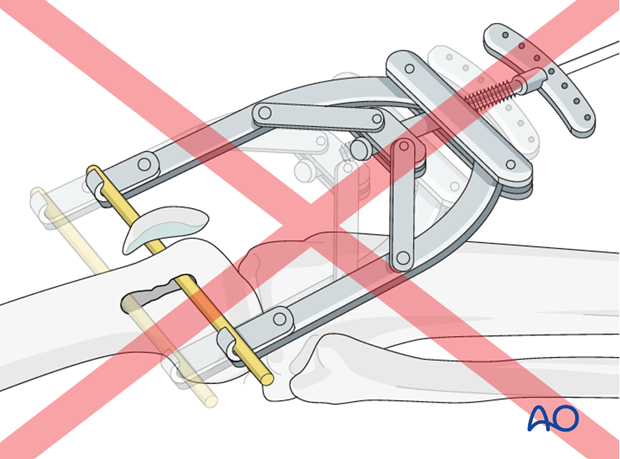
The reduction can be facilitated with manual traction and/or distal femoral skeleton traction.
Skeletal traction may be placed in the distal femur or the proximal tibia, depending on surgeon's preference. However, the distal femur is much more effective in facilitating direct reduction of periprosthetic femur fractures.
4. Fixation
Implant selection
In most cases, the fracture can be compressed with lag screws and neutralized with a long plate.
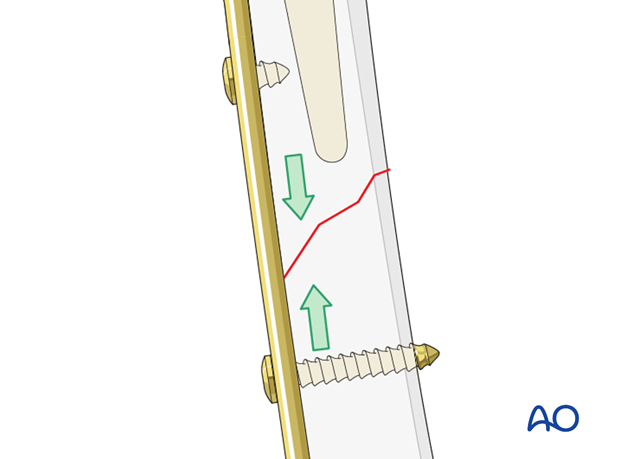
The femur has a sagittal bow and proximal or distal fixation may be desired. If available, a precontoured or anatomic plate should be selected.
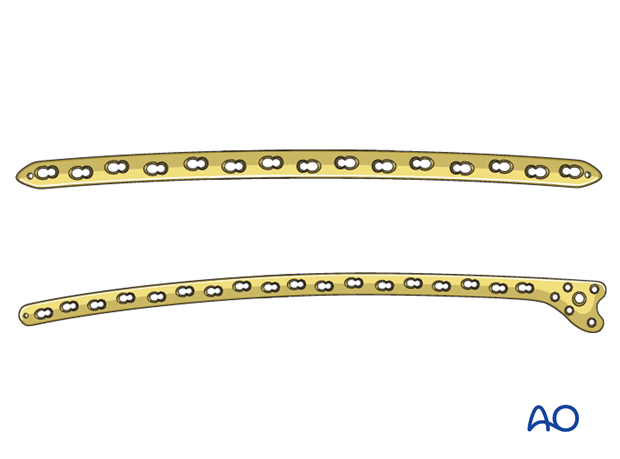
Compression by lag screws
The fracture is reduced and compressed with lag screws. Typically, 3.5 mm screws are utilized.
For more details regarding compression by lag screws with protection plate please refer to the dedicated section of the distal femur in the AO Surgery Reference.
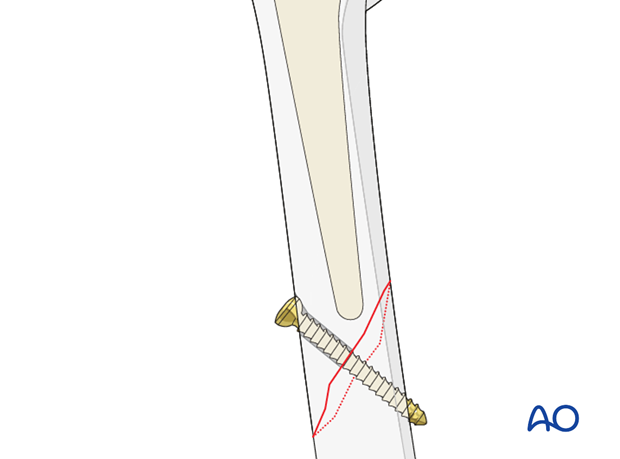
Alternative: compression plate
Alternatively, the plate may be applied on the lateral cortex of the femur in compression mode by creating an axilla and then compressing the bone utilizing the plate.

A screw is applied at the site of the fracture which will allow for the creation of an axilla.
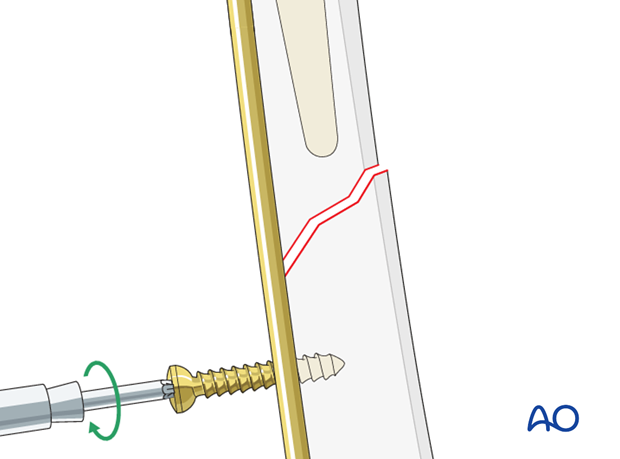
A screw is then applied at the other side of the fracture in compression mode.
A surgeon may choose to plate the entirety of the femur from the intertrochanteric ridge to the epicondyles of the distal femur.
For more details regarding compression plating please refer to the dedicated section of the distal femur in the AO Surgery Reference.
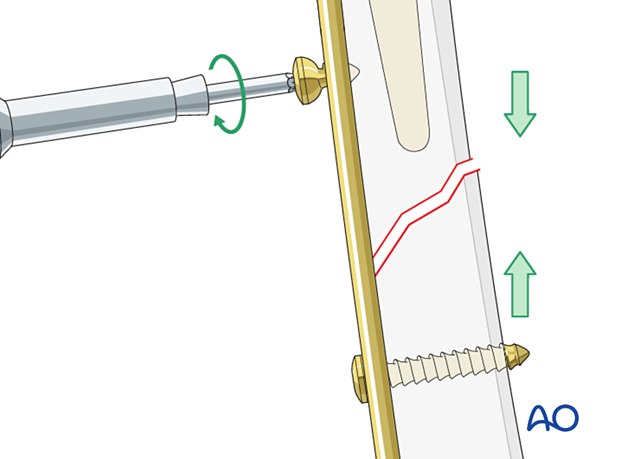
Osteoporotic patients
In osteoporotic patients the plate should not end at the distal metaphysis, to avoid distal femur peri-implant fractures.
It is advisable to utilize smaller screw diameters as lag screws, to minimize the risk of screw damage to the femoral cortices.
Options for additional stability
Additional stabilization can be achieved with locking and nonlocking screw fixation above and below the fracture site.
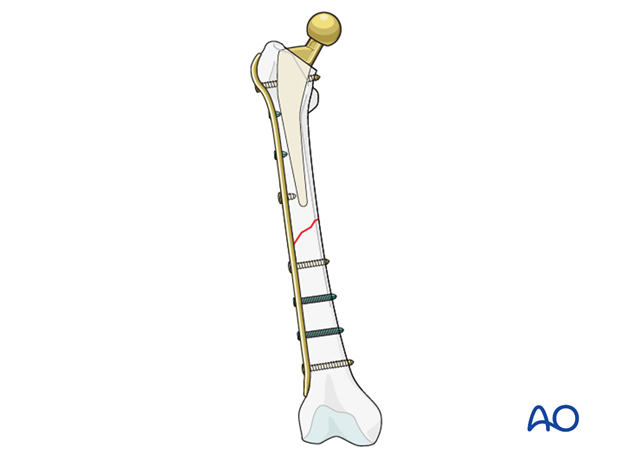
Transverse fractures
In the setting of a transverse fracture, a compression technique may be the only option to achieve fracture healing.
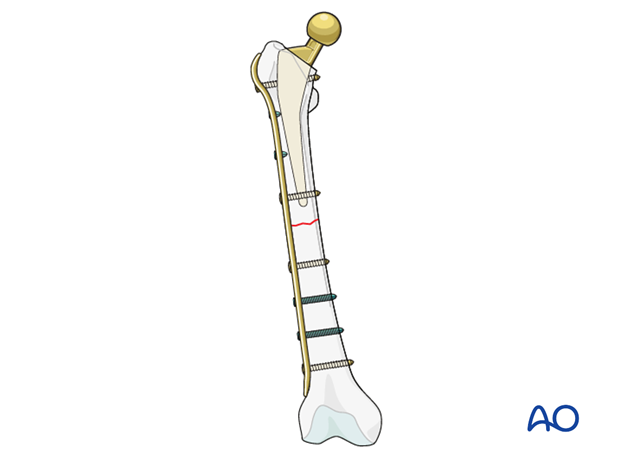
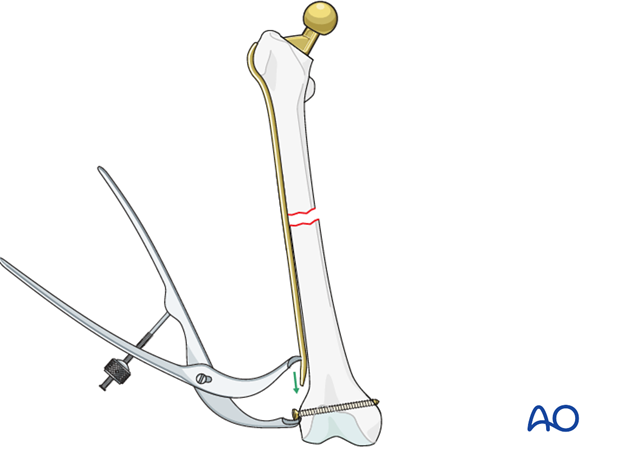
Fracture compression is performed utilizing a sagittal bow plate and traditional an articulated tensioning device or a Verbrugge clamp.
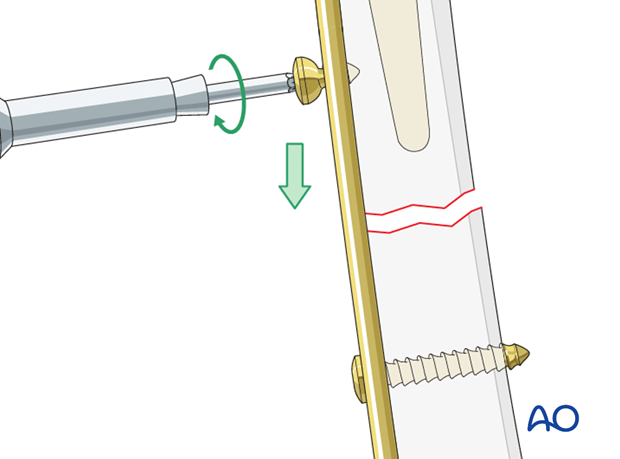
Another option to achieve compression is to use the dynamic compression holes within the plate.
5. Closure
A layered closure is preferred for periprosthetic fractures. If the vastus lateralis has been released, it should be primarily repaired with a nonabsorbable braided stitch. A subfascial drain should be considered as blood loss can be significant and periprosthetic fracture patients are at high risk of requiring anticoagulation immediately postoperatively. A hematoma requiring evacuation must be avoided. The wound is closed in layered fashion according to the surgeon's preference.
Sterile dressing should be applied and negative pressure incisional wound care can be considered.

6. Aftercare following ORIF
Postoperative management
Postoperative management should include careful monitoring of hematocrit and electrolytes particularly in the elderly patients.
Postoperative IV antibiotics should be administered up to 24 hours.
Consideration should be given to anticoagulation for a minimal course of 35 days. If there are thromboembolic complication this treatment is extended.
Drains can be discontinued when output is less than 30 to 50 cc per 12 hours.
Patient mobilization
Immediate mobilization of the patient should commence. If fracture stability will allow, the patient should be made weight bearing as tolerated as soon as possible. Long periods of limited weight bearing are extremely detrimental to patient recovery.
Wound healing
Avoidance of edema postoperatively is critical for both wound healing and patient mobilization. This can be aided by pneumatic compression devices. If negative pressure wound therapy is utilized, it can be discontinued after 5 to 7 days. Staples or sutures are typically removed at 14 to 21 days.