En bloc resection of a posterior tumor (L1 to L5)
1. Introduction
En bloc resection of a primary tumor is a significant undertaking, even in the most experienced hands. We therefore recommend referring these cases to quaternary centers with experience in primary spine tumor surgery.
En bloc resections
Terminology is essential in primary tumor management.
An en bloc resection refers to a surgical attempt to remove a tumor in one piece without violating it.
On the other hand, an intralesional resection or a curettage refers to a deliberate intralesional resection.
An en bloc resection needs to be associated with a pathological margin description to be correctly defined.
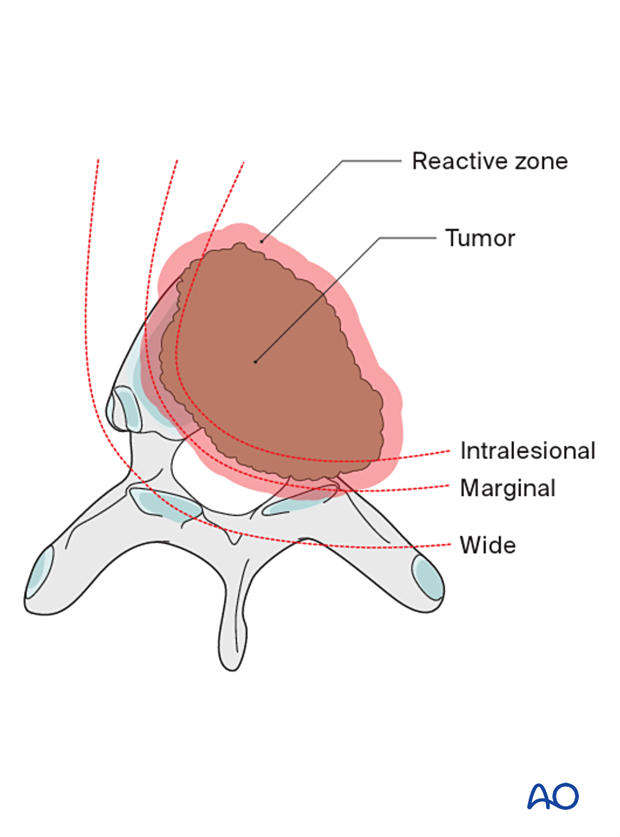
Four types of margins are described:
- Intralesional – resection margin is within tumoral tissue
- Marginal – resection margin is within a reactional zone or pseudocapsule (in the spine, the epidural margin is often marginal)
- Wide – resection margin is within normal tissue
- Radical – this is extracompartmental resection and, as such, does not apply to spine tumors
Feasibility
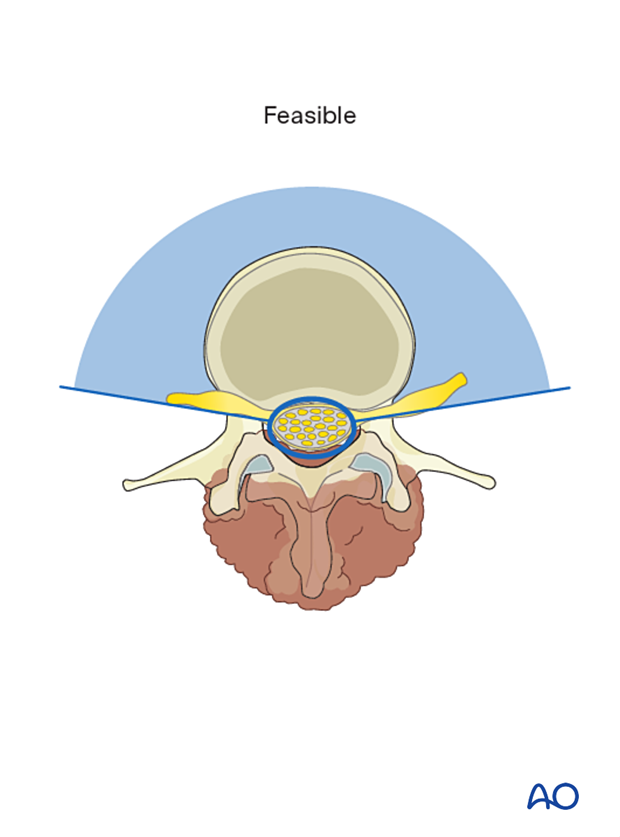
Two conditions need to be met for an en bloc resection to be deemed possible.
- If we consider the spinal canal as a ring, there needs to be enough circumference of that ring to be removed piecemeal to allow delivery of the neural element
- Access to the nerve root sleeve at its dural origin is required
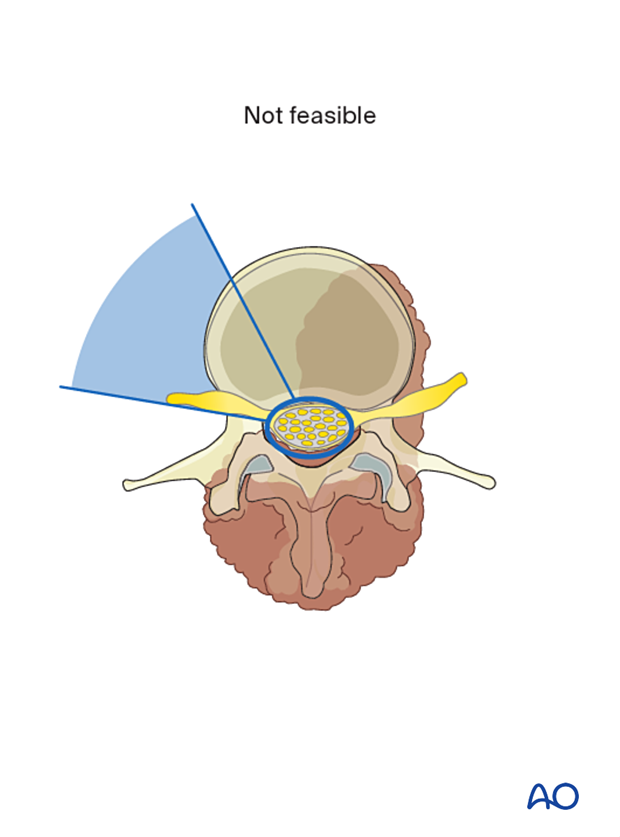
If these conditions are not met, an en bloc resection will not be possible without a planned transgression of the tumor.
In this illustration, the spinal canal is circumferentially surrounded by a tumor. There is not enough uninvolved portion of the ring to allow an en bloc resection.
2. Planning
Preoperative management
Proper planning is instrumental in the management of primary spine tumors. A multidisciplinary approach may be required depending on the localization of the tumor.
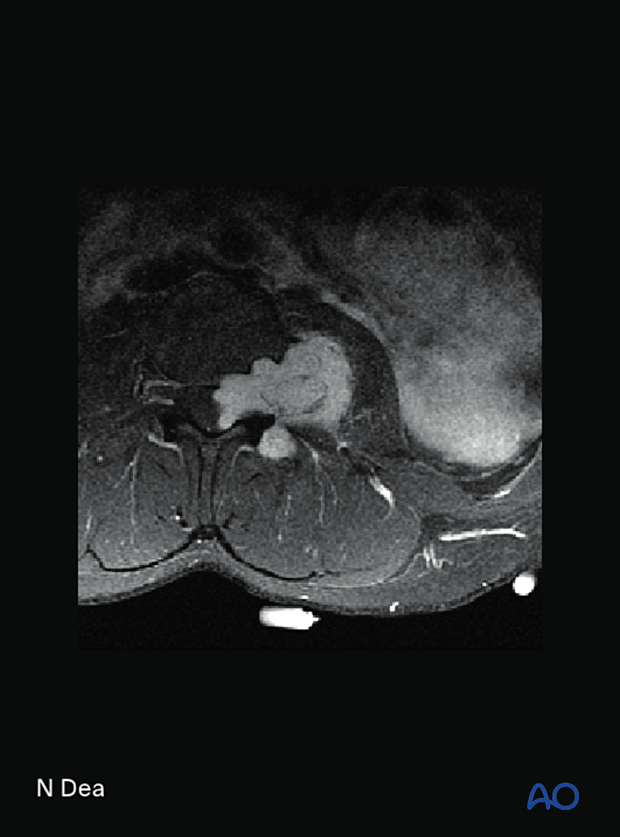
This picture shows an example of an L3 posterior element solitary fibrous tumor.
Embolization
Embolization procedures are recommended to reduce operative blood loss in hypervascular tumors, especially during more extensive resections.
Embolization should be considered for hypervascular tumors, such as giant cell tumors, aneurysmal bone cysts, and hemangiomas.
The role of the embolization is:
- To reduce the vascularity of the tumor
- To facilitate dissection around the tumor
- Mapping of spinal cord vascular supply
Embolization on its own may also have a therapeutic effect.
This image shows the embolization of a hypervascular tumor.

Resection strategy
A posterior approach is recommended for a lumbar tumor involving the posterior element.
The goal will be to disconnect the tumor from the intact vertebral body and deliver the tumor posteriorly.
A wide visualization is essential in these cases, and a laminectomy involving half a level above and below the tumor is recommended.
The goal is to achieve:
- Good visualization of normal and abnormal anatomy
- Safe decompression of the neural elements
A posterior-only approach may also be used if a posterior element tumor is unilateral and involves up to segment 3 or 10.
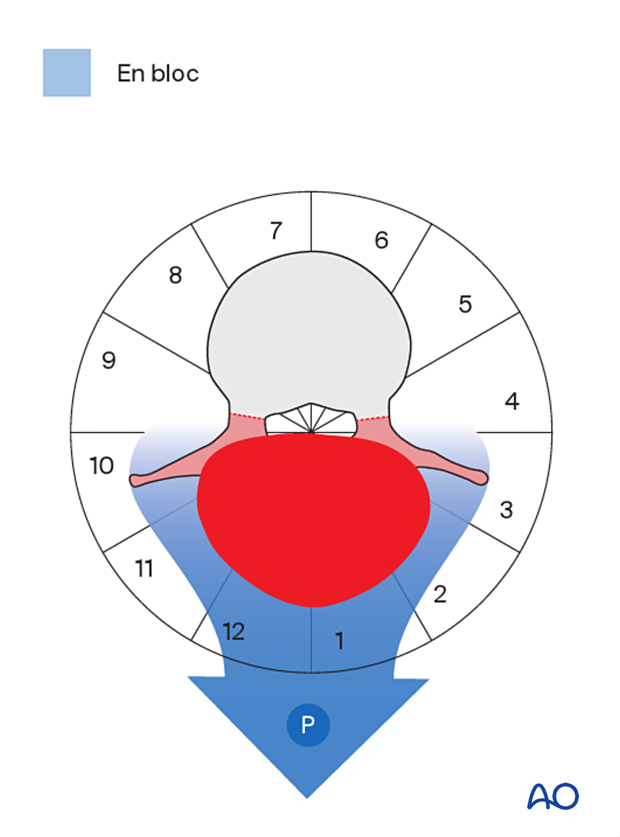
Reconstruction strategy
A posterior element resection is less destabilizing than a vertebrectomy. A fixation of two vertebrae above and below is sufficient.
The risk of implant failure may be decreased by cement augmentation of fenestrated screws in patients with poor bone quality.
As the procedure is often curative, it is important to verify that the spine is reconstructed in good alignment, and a solid bony union should be attempted.
If a posterior element tumor only involves segment 1 and/or 12, an en bloc resection can be performed without the need for an instrumented fusion.
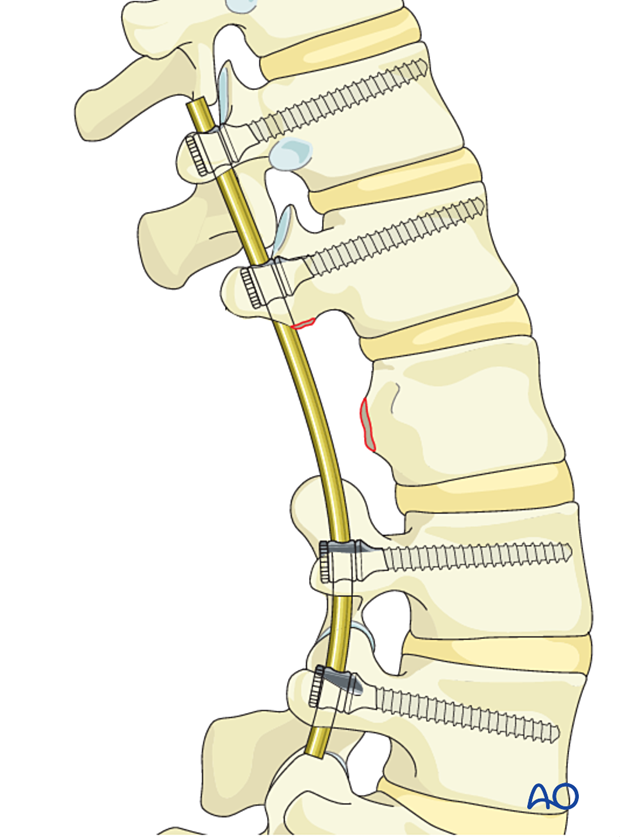
Case-based scenario
Every case is unique.
To illustrate the surgical principle of an en bloc resection with posterior release and delivery in the lumbar spine, we will use an L2 tumor located in segments 10–3 of the WBB classification.
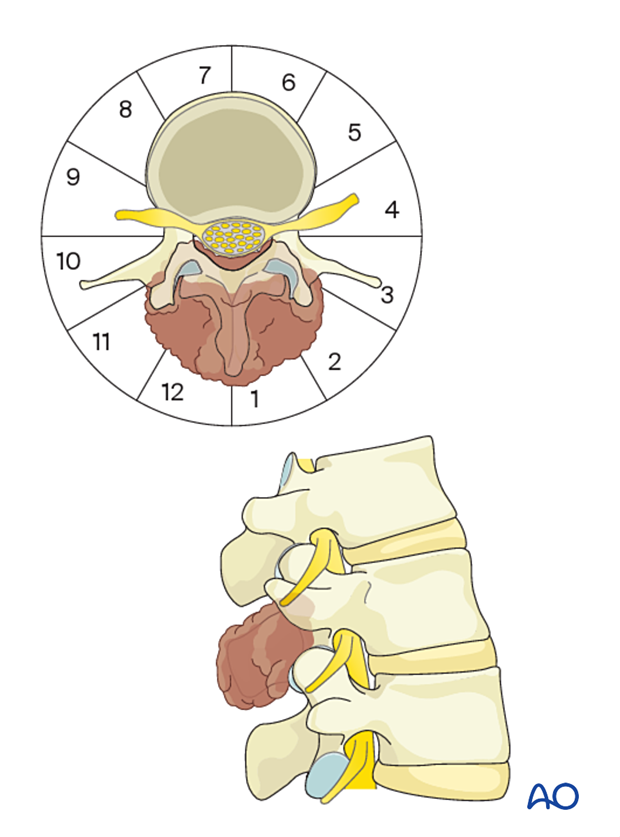
3. Patient preparation and surgical access
Patient preparation
The patient is placed prone.
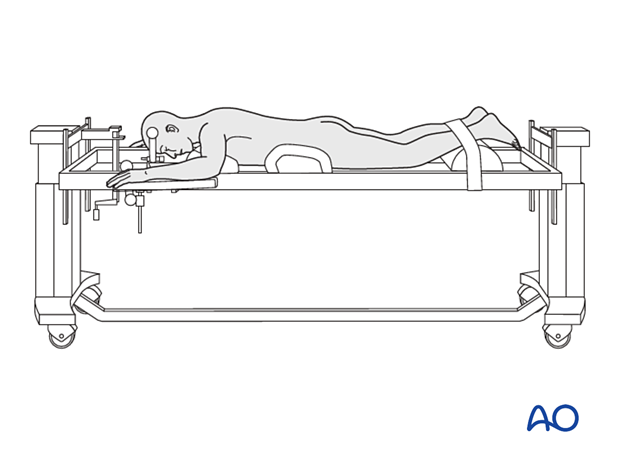
Surgical access
A posterior midline approach to the lumbar spine is performed.
A wider dissection will typically be performed for primary tumors compared to a trauma case.
Careful analysis of the preoperative imaging is important to avoid tumor violation during the approach.
Following a midline incision, the subcutaneous tissues are dissected down to the chosen dorsal plane of dissection.
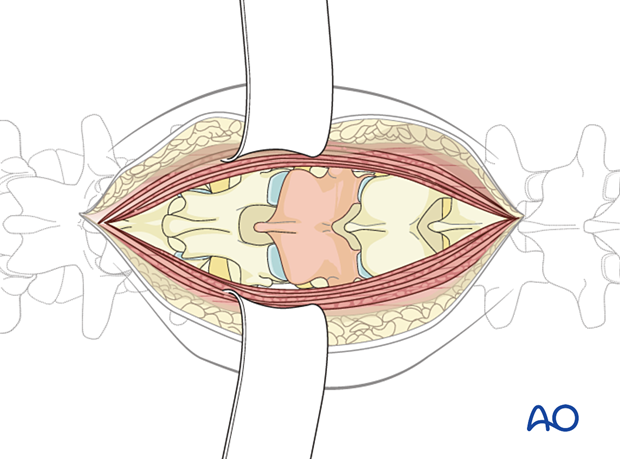
The dissection is carried laterally through the soft tissues around the tumor until the normal bone is reached.
Review preoperative images to verify whether the tumor invades the lamina. In such cases, exposure of the posterior elements should be performed with great care, and the use of Cobb elevators should be avoided.

A cuff of normal muscle will be left on the tumor during the dissection to ensure a negative margin is achieved.
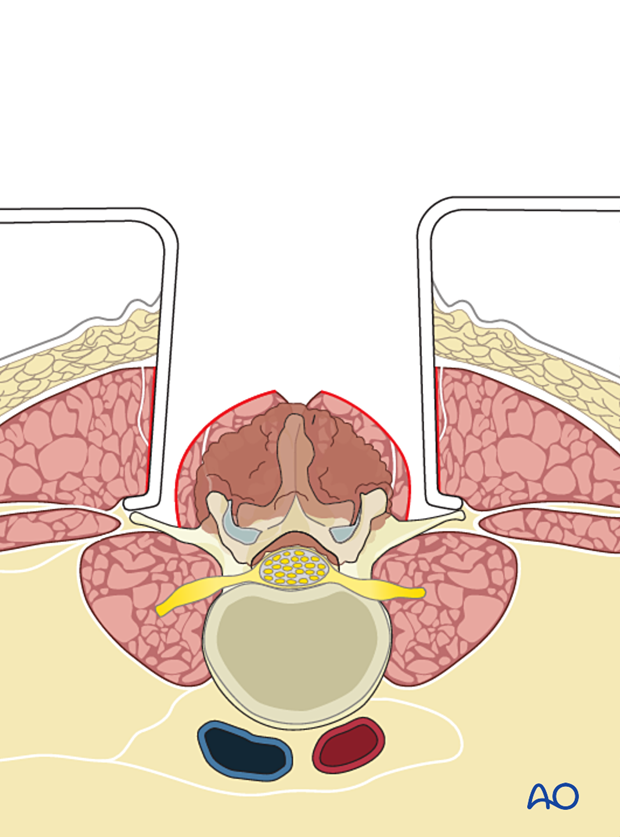
The incision may need a caudal extension when the tumor involves the lower lumbar spine.
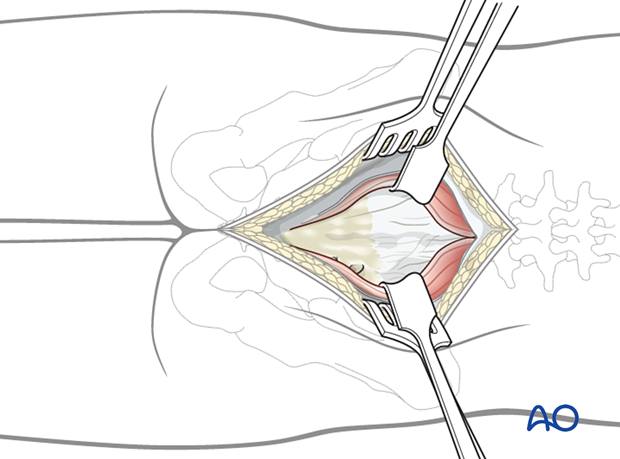
4. Instrumentation
Screw insertion
Insert all screws according to the preoperative plan.
Optimal pedicle screw purchase will, in order of importance, be achieved by:
- Selecting the largest possible screw diameter according to the pedicle diameter
- Selecting the longest possible screw
- Positioning of the screw under the cranial endplate
- Cement augmentation of the screw
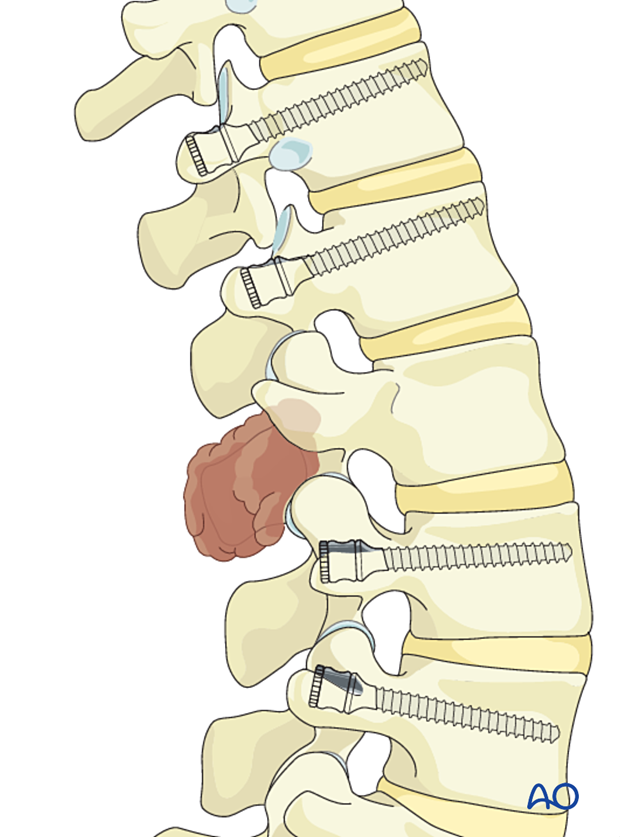
Lumbar pedicle screws are inserted according to the standard technique.
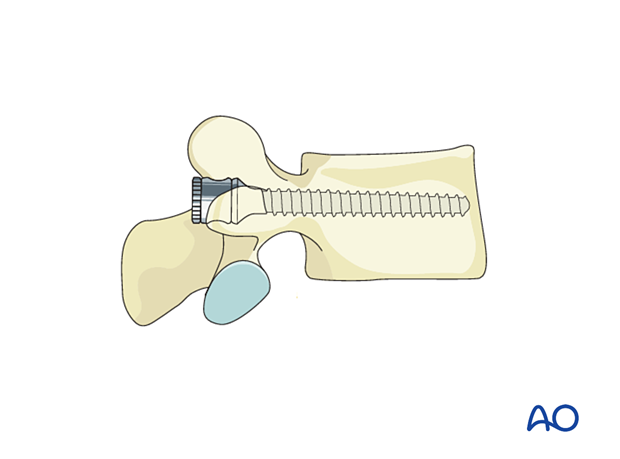
Rod preparation
Every effort should be made to contour the rod to decrease the risk of induced sagittal or coronal malalignment.
For further details about sagittal spinal alignment, refer to this section.
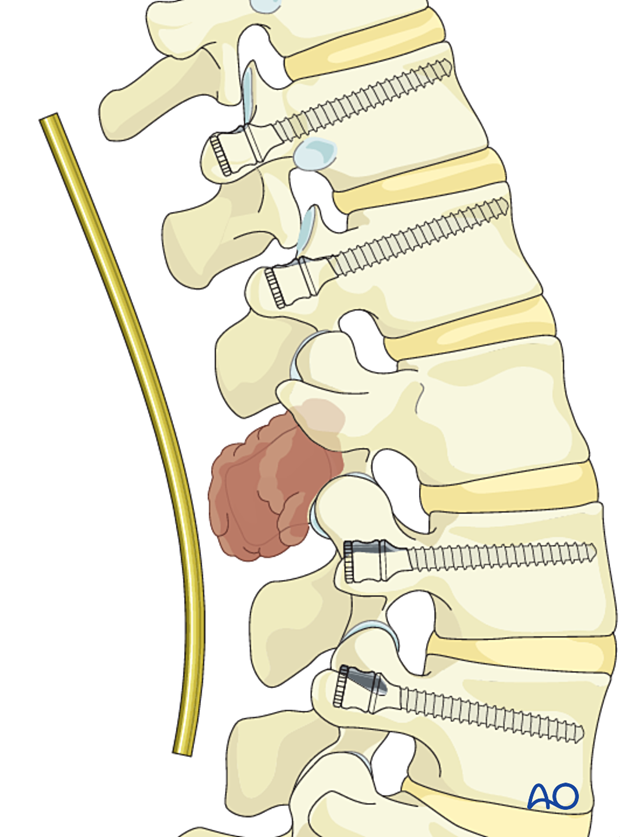
Sacral and iliac instrumentation
When the tumor involves the lower lumbar spine, extending instrumentation to S1 and the iliac may be necessary.
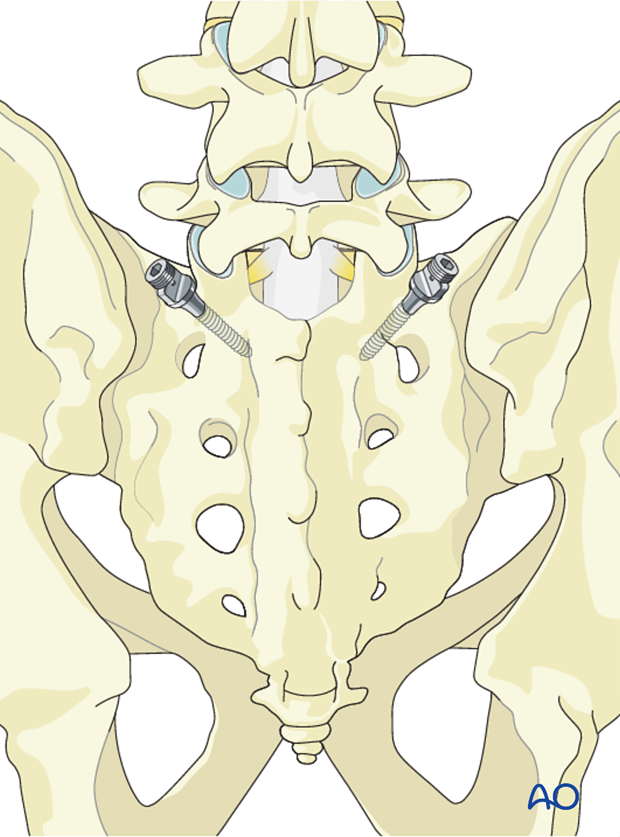
5. Decompression
Laminectomy
Perform a laminectomy according to the preoperative plan.
Dissection should progress from normal to abnormal tissues to protect normal neurological elements and facilitate dissection.
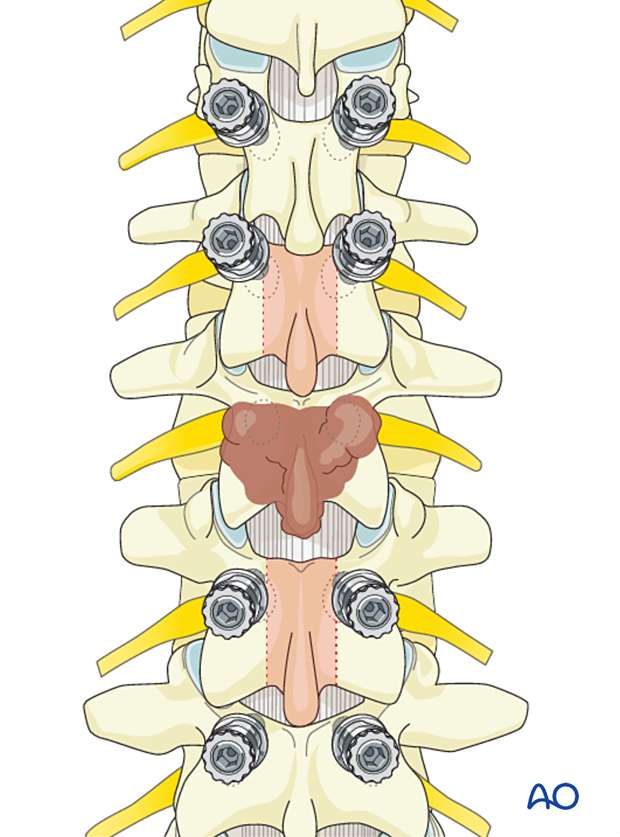
The inferior facet of L1, the superior facet of L2, the transverse processes, and the uninvolved portion of the inferior facet of L2 are then removed in a piecemeal fashion to isolate the L2 pedicles.
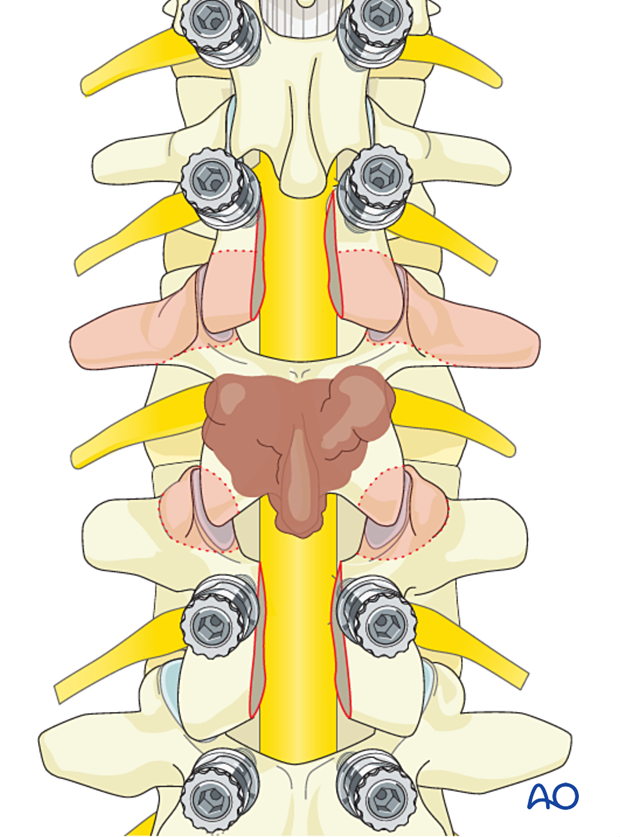
Isolation of nerve roots
Isolate the L3 nerve roots and follow them laterally.
Every effort should be made to protect and preserve lumbar nerve roots if they are uninvolved with the tumor.
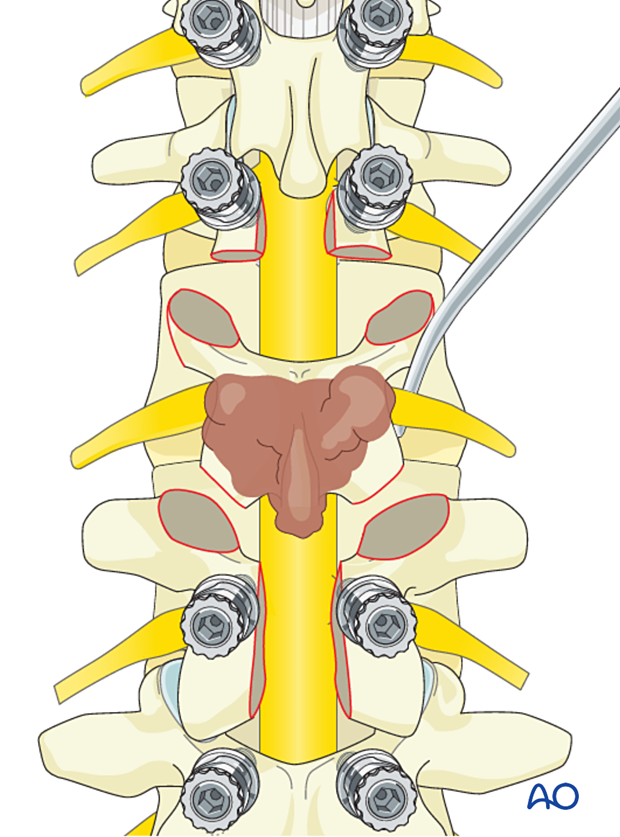
Bony release
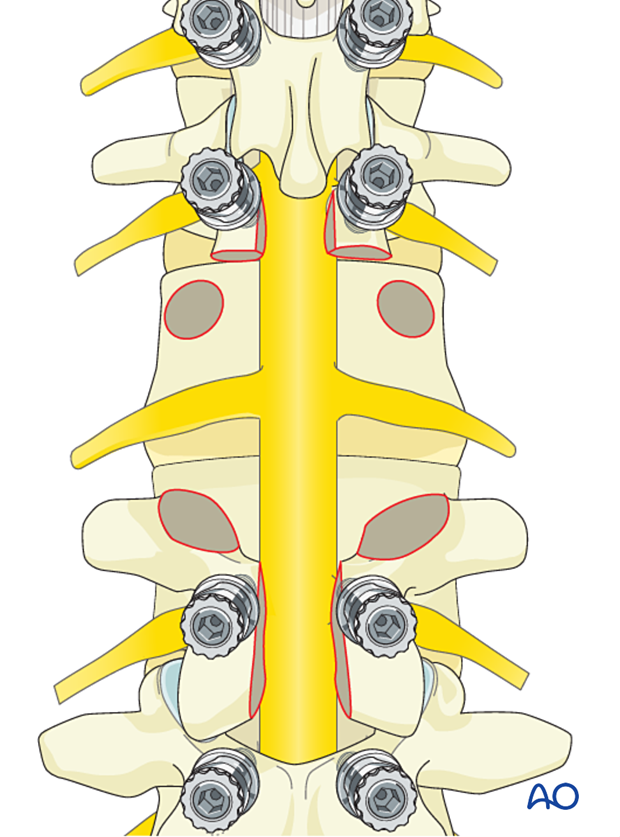
Disconnect the posterior element from the anterior element by performing an osteotomy. Start the osteotomy where the lateral soft-tissue dissection reaches normal bone and continue until the spinal canal is reached.
It is essential to plan the osteotomy through normal bones with adequate negative margins.
In this case, the osteotomy is made through the pedicles.
The osteotomy can be achieved using a curved osteotome coming from the superior, lateral, and inferior until the posterior element is fully disconnected.
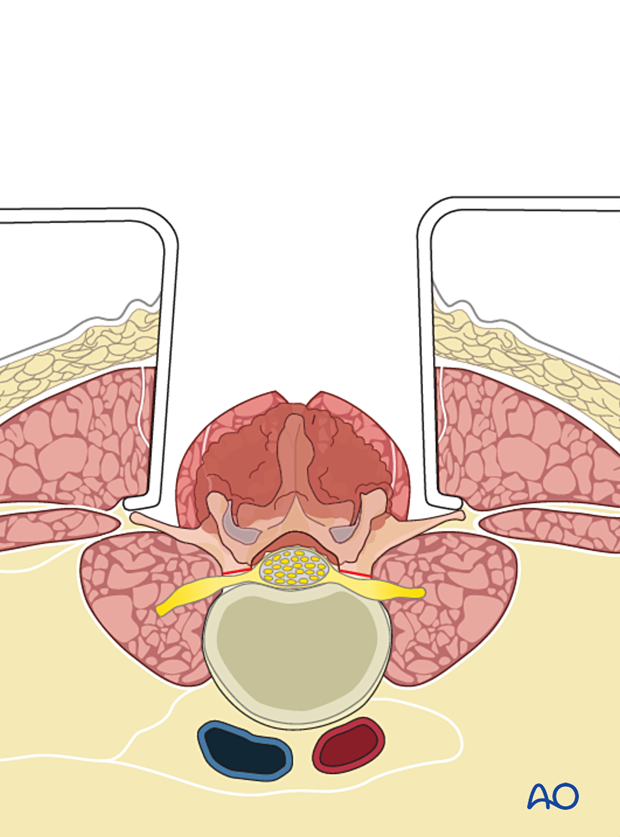
Alternatively, a Tomita saw passed around the pedicle can be used.
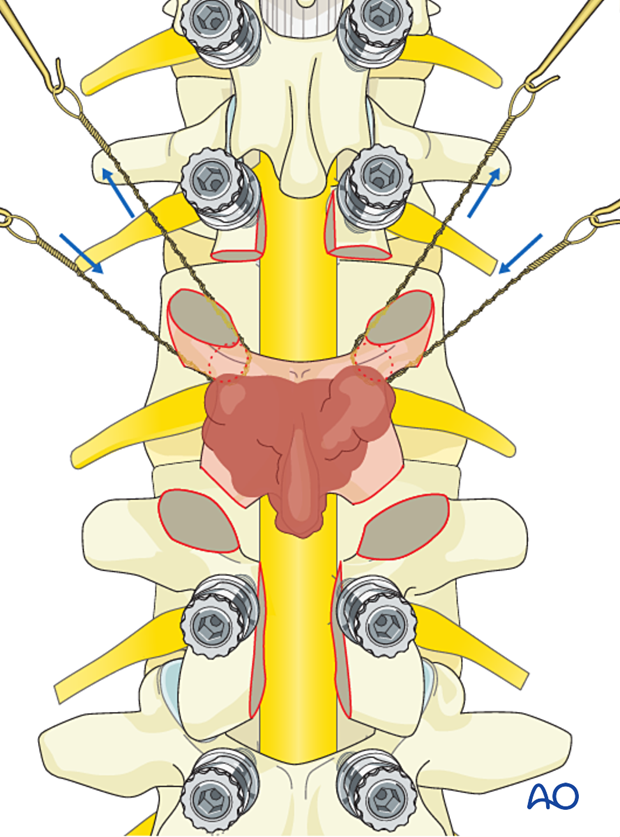
Once the tumor is fully released, it is delivered.
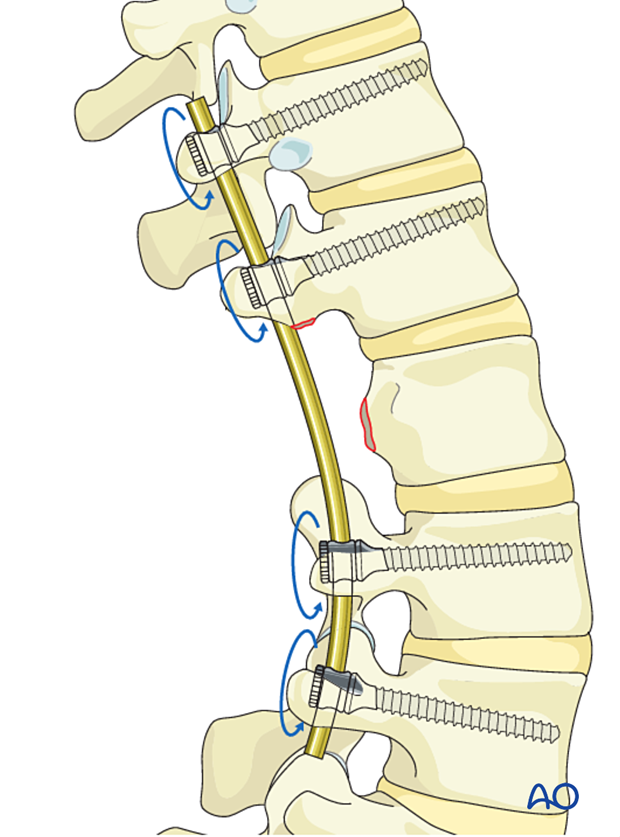
Rod insertion and fixation
Insert the rods into the screw heads and secure them by tightening the inner nuts.
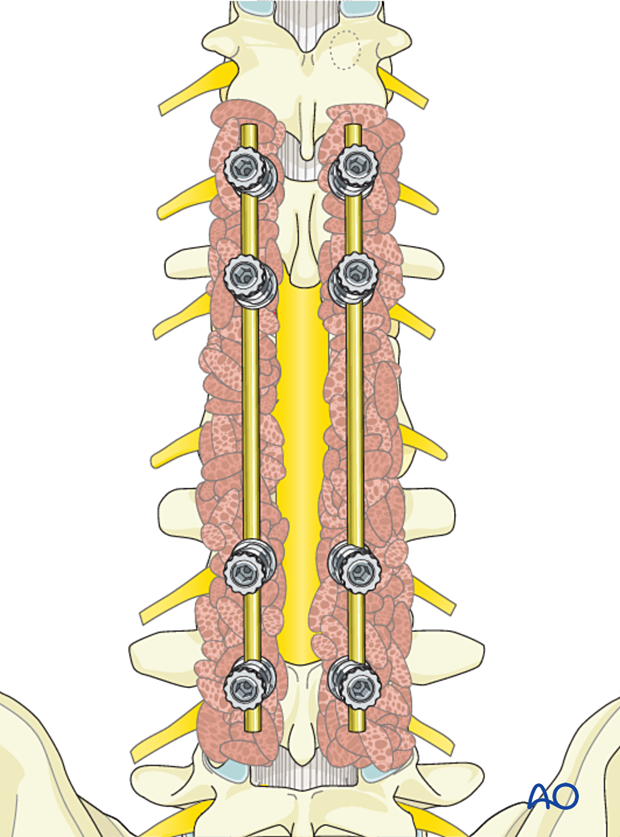
6. Reconstruction
Fusion
Excise the facet capsule and denude/curette the joint surface cartilage surfaces and the posterior cortex.

Insert pieces of bone graft (autograft, allograft) into the decorticated facet joint for fusion.
7. Intraoperative imaging
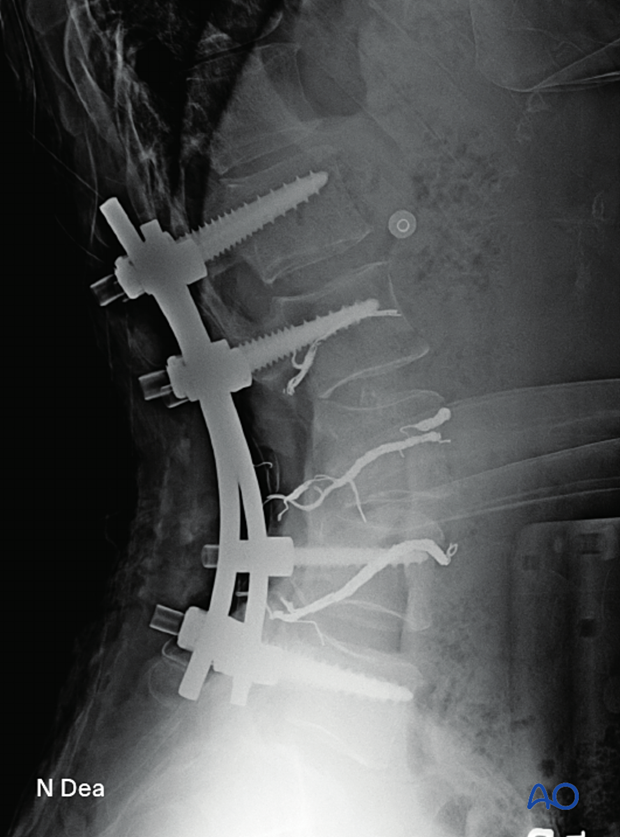
Before wound closure, intraoperative imaging is performed to check the adequacy of reduction, position, and length of screws, and the overall coronal and sagittal spinal alignment.
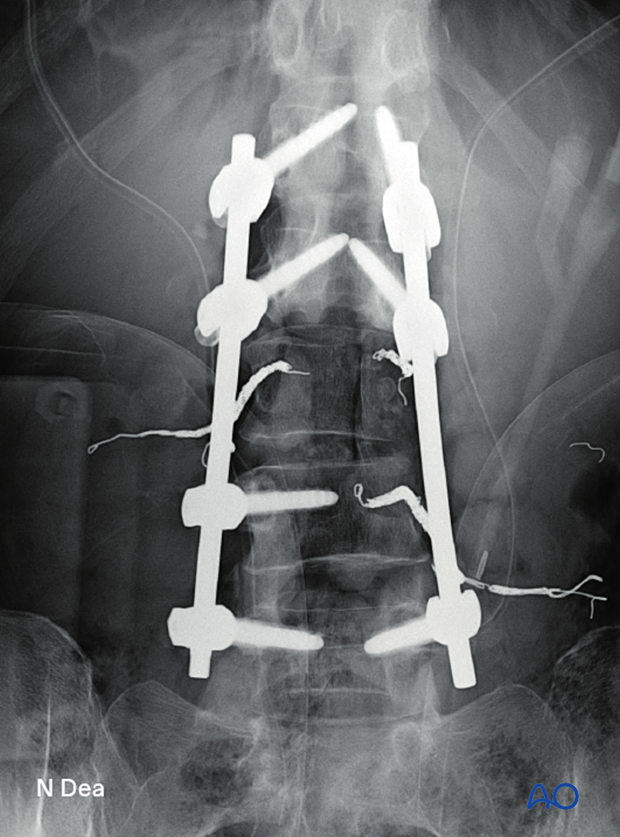
Lateral view of the above case
Lateral view of the specimen
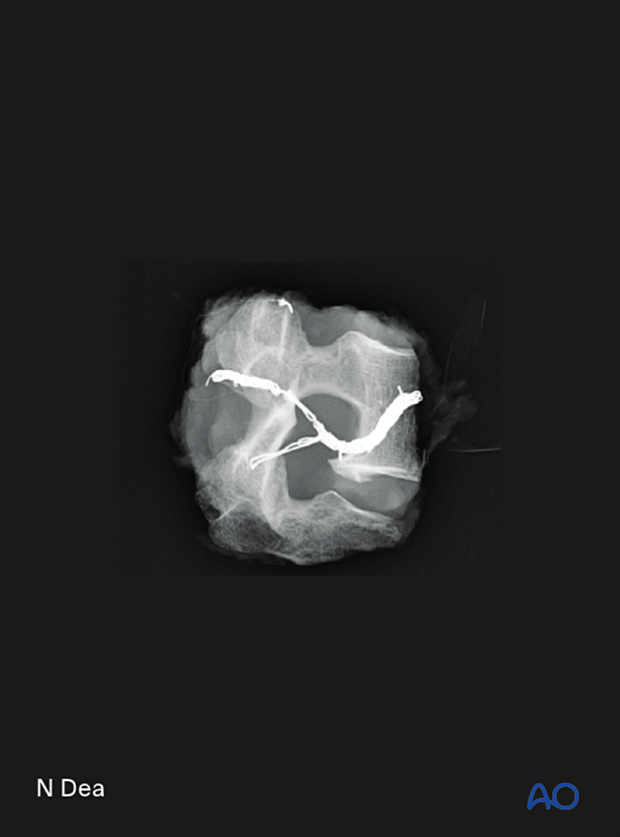
8. Posterior closure
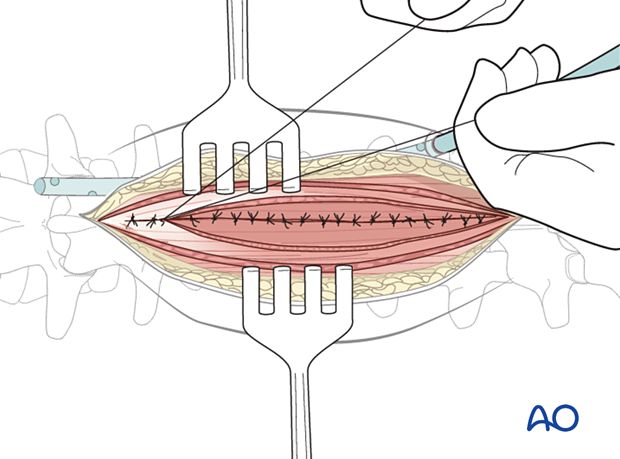
Perform a multilayer closure as described in the approach.
For patients undergoing tumor surgery and/or with a history of radiation:
- Plastic surgery should perform soft-tissue reconstruction to decrease the risk of wound complications.
- Intrawound vancomycin can be applied to decrease the risk of postoperative wound complications.
9. Aftercare
Patients are made to sit up in bed on the first day after surgery. Patients with intact neurological status are made to stand and walk on the first day after surgery.
Patients can be discharged when medically stable or sent to a rehabilitation center if further care is necessary.
Throughout the hospital stay, adequate caloric intake of a high-quality diet should be monitored.
Patients are generally followed with periodical x-rays at 6 weeks, 3 months, 6 months, and 1 year to monitor for hardware failure and with an MRI every 6 months for tumor surveillance.
Some primary benign tumors of the spine can recur years after surgery, and long-term tumor surveillance is important.













