Intralesional resection (L1 to L5)
1. Introduction
Preoperative management
Proper planning is instrumental in the management of primary spine tumors. A multidisciplinary approach may be required depending on the localization of the tumor.
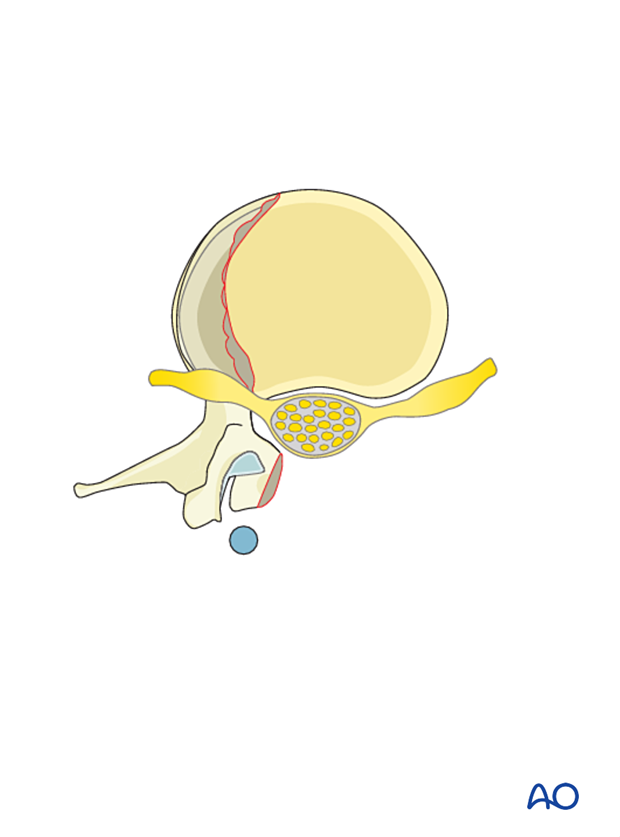
This picture shows an L1 aneurysmal bone cyst.
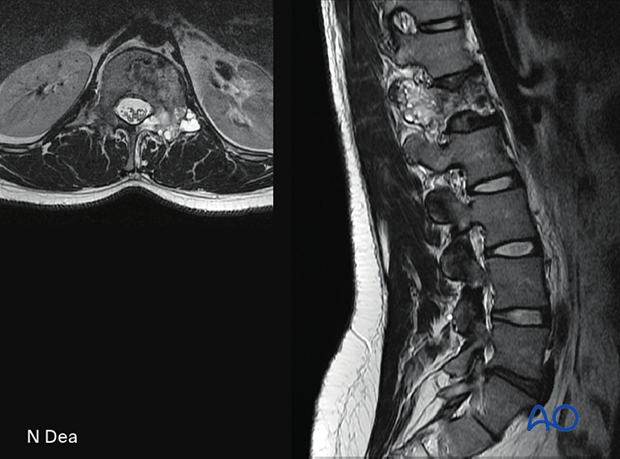
Embolization
Embolization procedures are recommended to reduce operative blood loss in hypervascular tumors, especially during more extensive resections.
Embolization should be considered for hypervascular tumors, such as giant cell tumors, aneurysmal bone cysts, and hemangiomas.
The role of the embolization is:
- To reduce the vascularity of the tumor
- To facilitate dissection around the tumor
- Mapping of spinal cord vascular supply
Embolization on its own may also have a therapeutic effect.
This image shows the embolization of a hypervascular tumor.

Resection strategy
Most benign primary tumors will be localized in the posterior element with variable extension into the vertebral body. These tumors are approached and resected through a posterior approach only.
A wide visualization is essential in these cases, and a laminectomy involving half a level above and below the tumor is recommended.
The goal is to achieve:
- Good visualization of normal and abnormal anatomy
- Safe decompression of the neural elements
Reconstruction strategy
In patients requiring posterior lateral decompression but no anterior column reconstruction, at least two levels above and below the involved segment should be instrumented. In cases of multilevel tumors or poor bone quality, this construct can be extended.
Short segment constructs lead to increased stress on the posterior implants, which increases the risk of implant failure (screw pullout/fracture).
The risk of implant failure may be decreased by cement augmentation of fenestrated screws and reconstitution of the anterior column using cement augmentation or a cage.
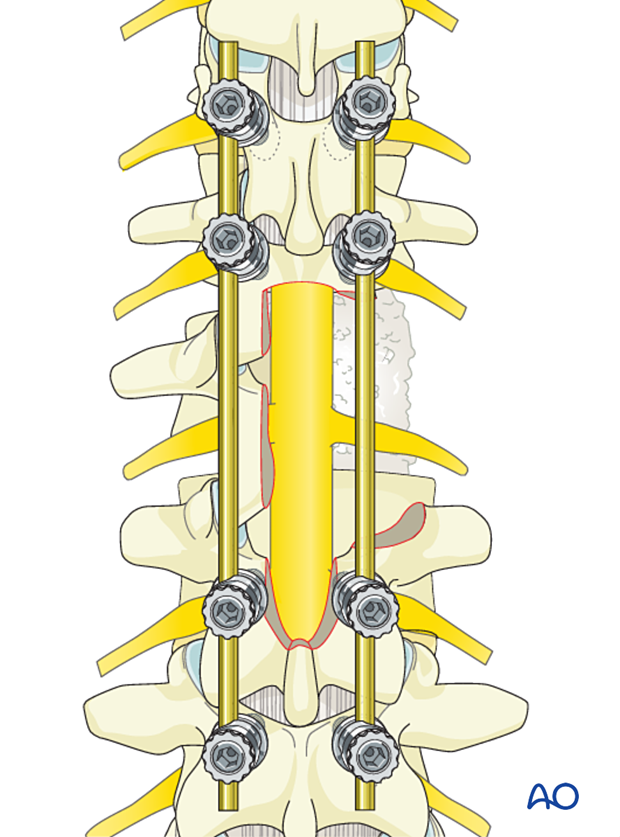
Depending on the extent of the vertebral body resection, anterior reconstruction may be required. Reconstruction can be achieved posteriorly using PMMA or anteriorly using an expandable cage.
If anterior vertebral body reconstruction is chosen, the posterior instrumentation, resection, and fusion are first performed before the patient is turned, and vertebral body reconstruction is performed anteriorly.
As the procedure is often curative, it is important to verify that the spine is reconstructed in good alignment, and a solid bony union should be attempted.
If a posterior element tumor only involves segments 1 and/or 12, resection can be performed without the need for an instrumented fusion.
In unilateral cases, instrumentation of the unaffected side may be performed, especially if radiation is not being considered.
Case-based scenario
Every case is unique.
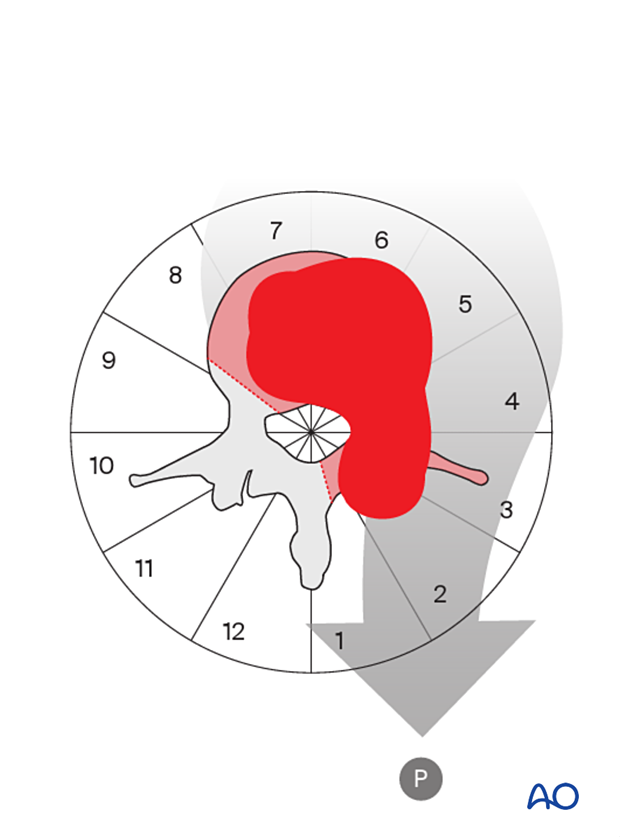
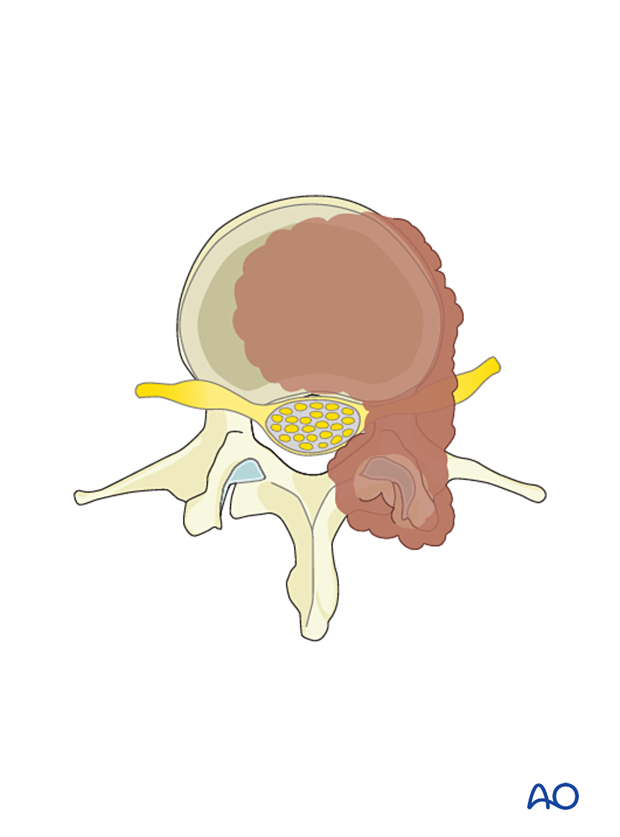
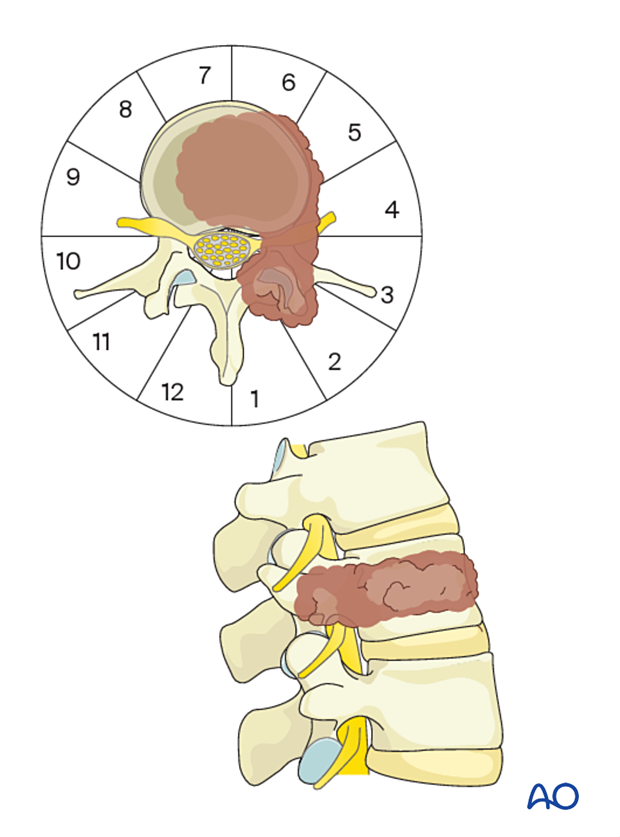
To illustrate the surgical principle of a posterior intralesional resection, including a significant portion of the vertebral body, we will use an L2 tumor located in segments 1–8 of the WBB classification.
2. Patient preparation and surgical approach
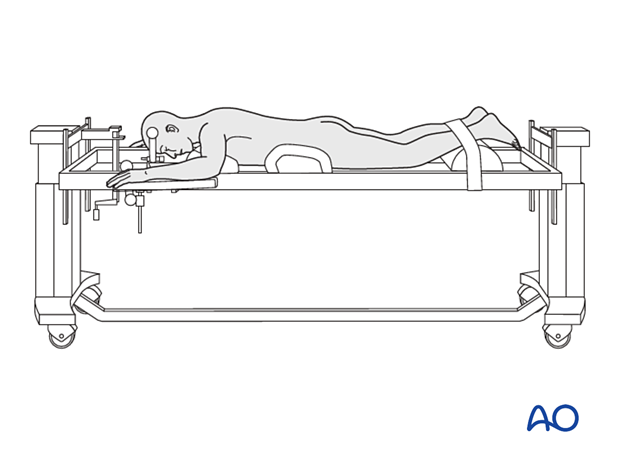
Patient preparation
The patient is placed prone.
Surgical access
A posterior midline approach is used.
A wider dissection will typically be performed for primary tumors compared to a trauma case.
Careful analysis of the preoperative imaging is important to avoid tumor violation during the approach.
Following a midline incision, the subcutaneous tissues are dissected down to the chosen dorsal plane of dissection.
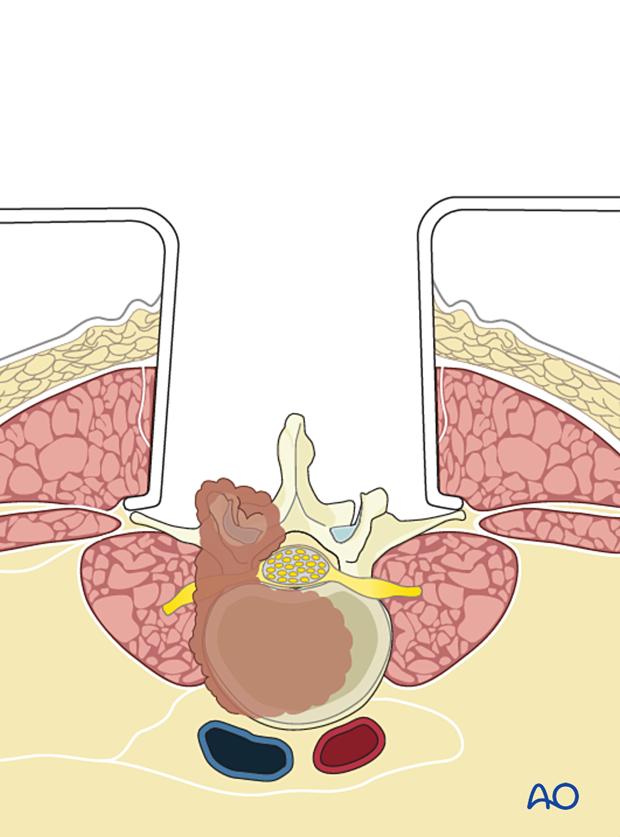
The incision may need a caudal extension when the tumor involves the lower lumbar spine.
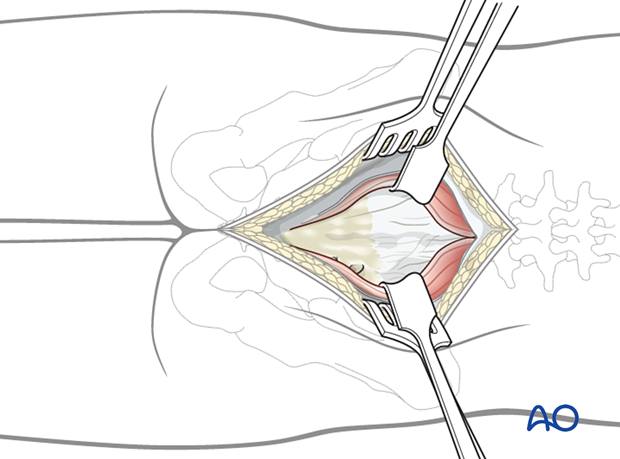
3. Screw insertion
Insert all screws according to the preoperative plan.
Optimal pedicle screw purchase will, in order of importance, be achieved by:
- Selecting the largest possible screw diameter according to the pedicle diameter
- Selecting the longest possible screw
- Positioning of the screw under the cranial endplate
- Cement augmentation of the screw
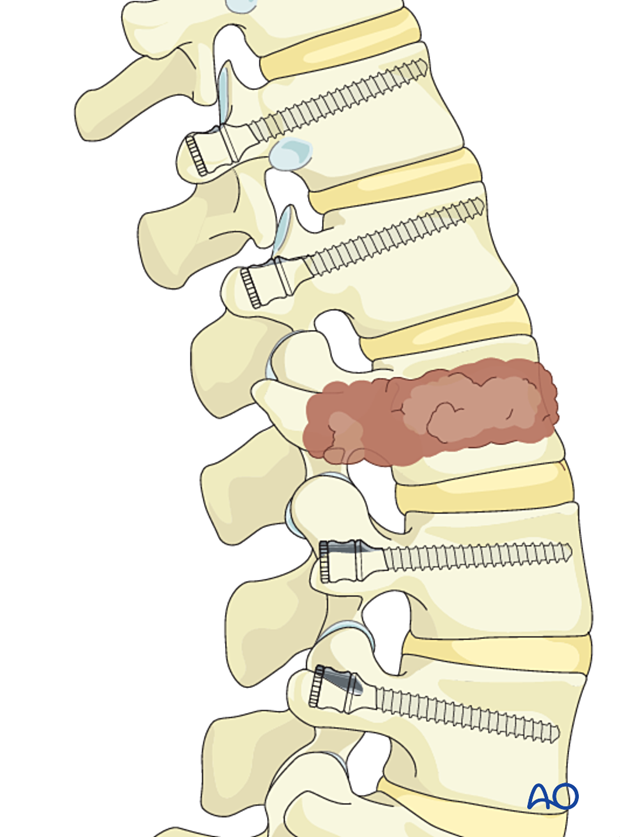
Lumbar pedicle screws are inserted according to the standard technique.
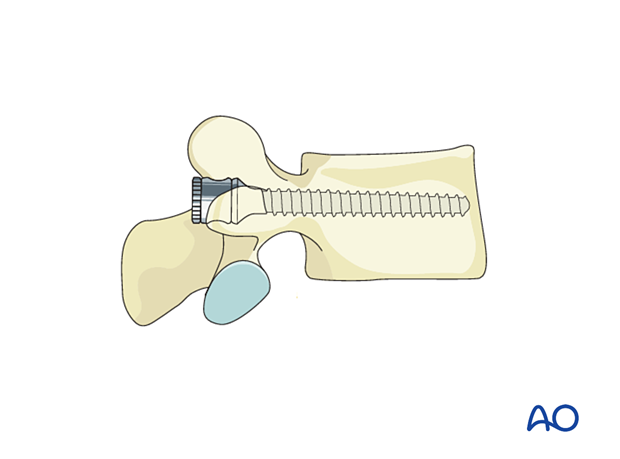
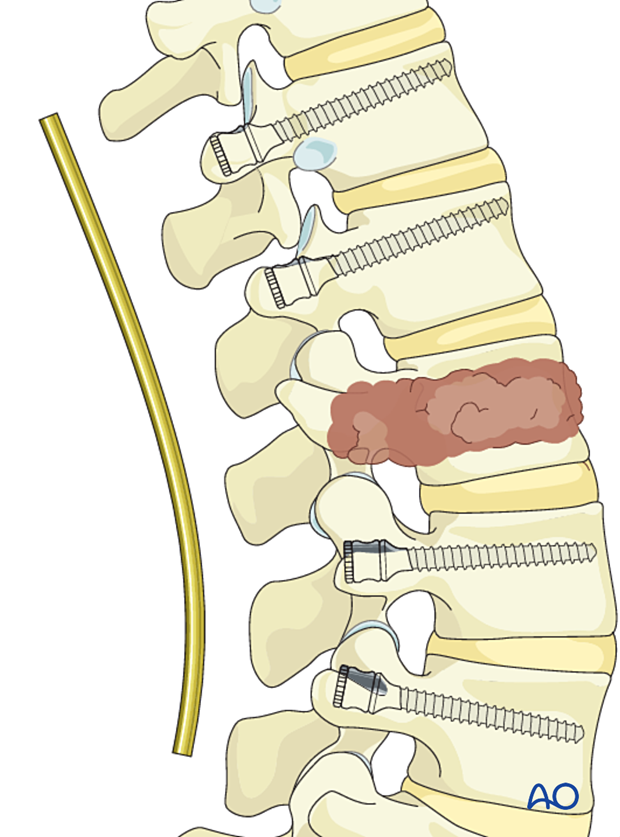
Rod preparation
Every effort should be made to contour the rod to decrease the risk of induced sagittal or coronal malalignment.
For further details about sagittal spinal alignment, refer to this section.
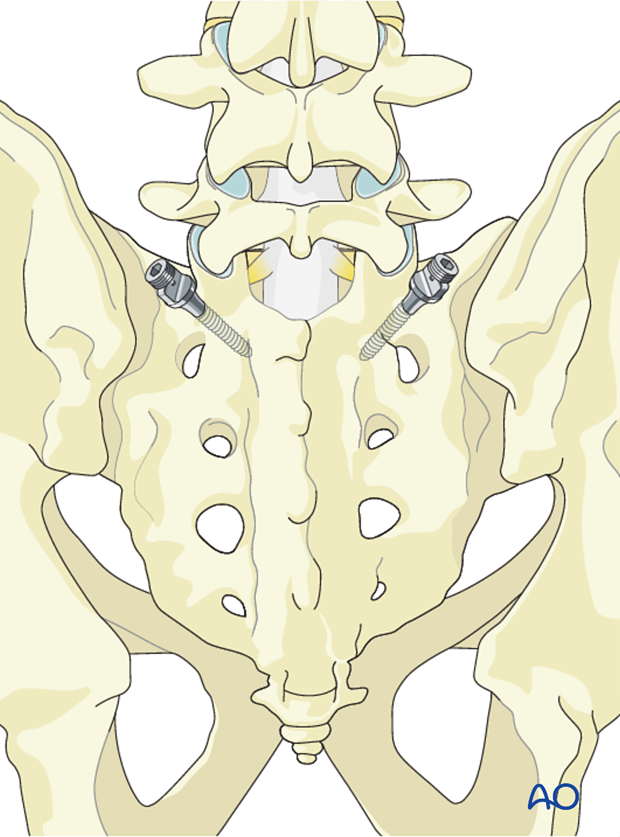
Sacral and iliac instrumentation
When the tumor involves the lower lumbar spine, extending instrumentation to S1 and the iliac may be necessary.
4. Decompression
Laminectomy
Perform a laminectomy according to the preoperative plan.
Dissection should progress from normal to abnormal tissues to protect normal neurological elements and facilitate dissection.
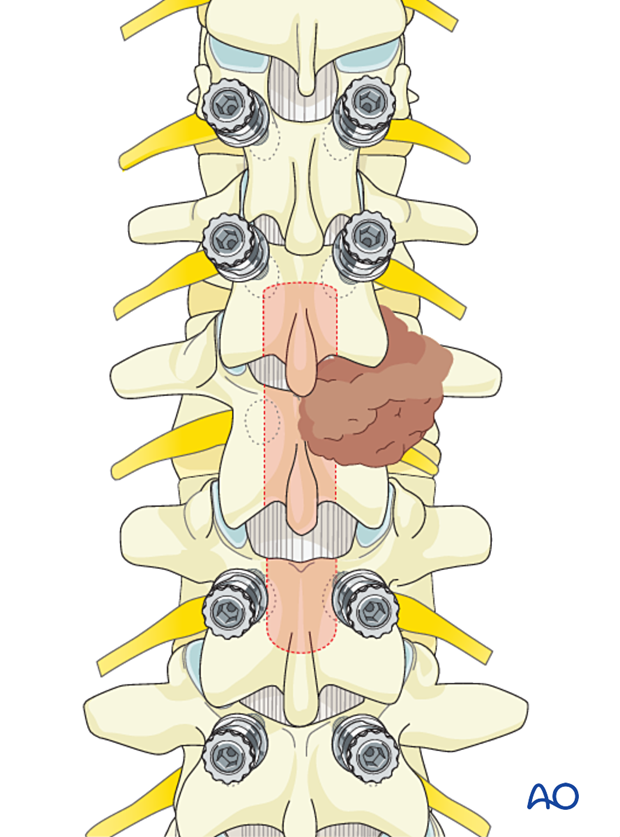
Removal of facet joints
Remove the inferior portion of the facet joint of the vertebra above and the superior portion of the facet joint of the vertebra below.
Depending on the position of the tumor, a complete resection of the facet joint and the pedicle may be required.
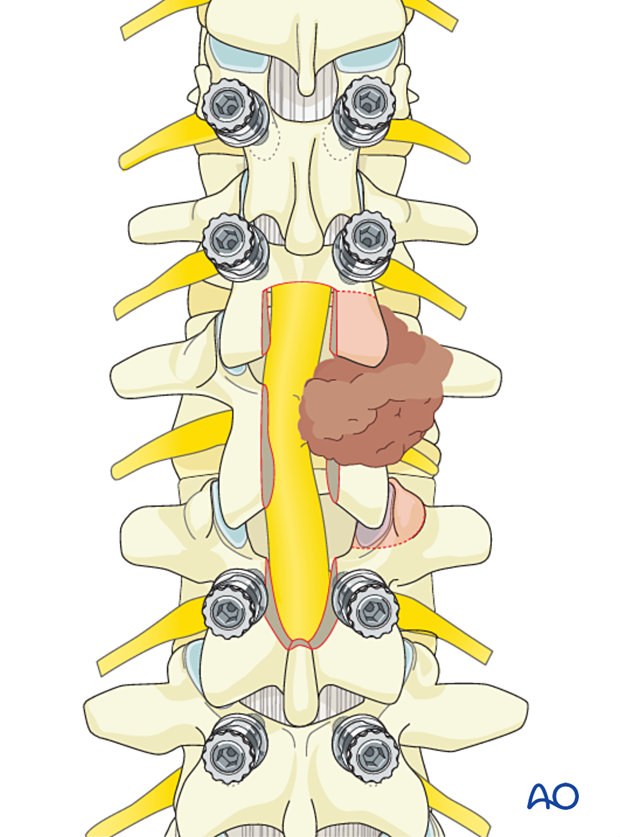
5. Tumor resection
Dissection of the tumor should progress from normal to abnormal tissues to protect normal neurological elements and facilitate dissection.
Use reverse-angle curettes and pituitary rongeurs to debulk the tumor.
Spinal cord mobilization should be minimized to reduce the risk of neurological injury.
The goal is to achieve gross total resection.
Intraoperative navigation can be used as an adjunct to maximize resection accuracy.
If the resection results in significant instability, a contralateral temporary rod is inserted to avoid neural element injury/distraction.
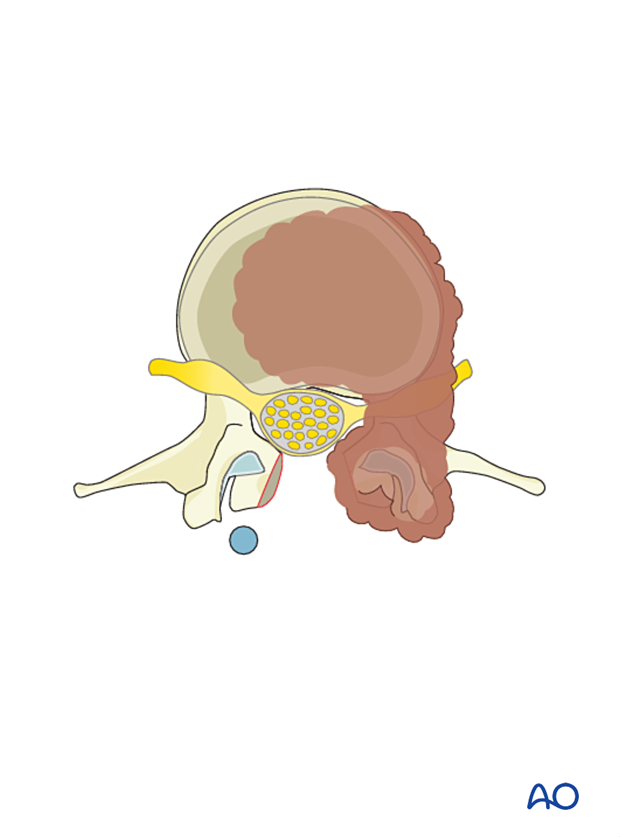
Once the tumor is entirely resected, the goal of the surgery is met.
6. Vertebral body reconstruction from posterior (if chosen)
Preparation of endplates
Remove any remaining disc fragments and prepare the endplates using curettes and a rongeur.
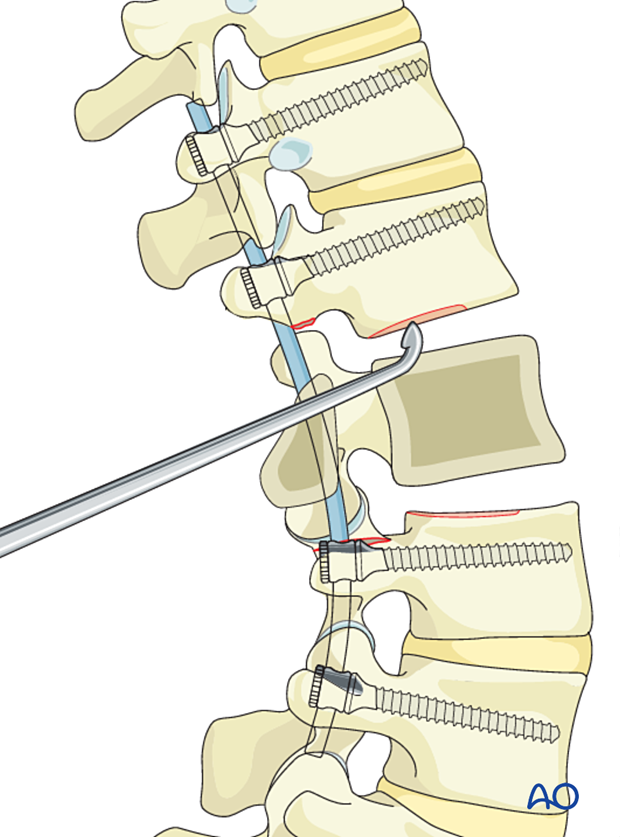
Rebar is first put in place.
The rebar can either be a chest tube that will later be filled with PMMA or K-wires inserted in the vertebral body above and below.
Alternatively, an expandable cage can be used.
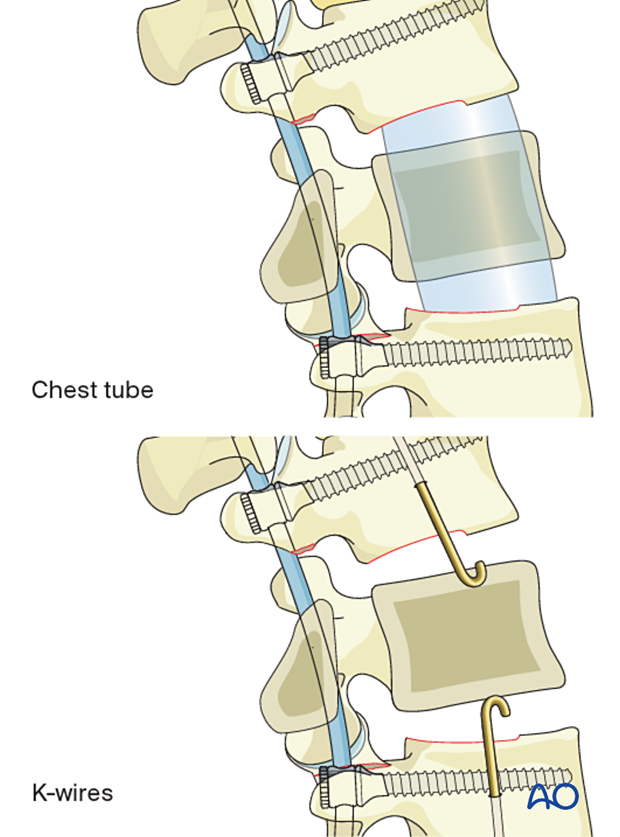
When the PMMA has reached its desired consistency, use it to fill the defect.
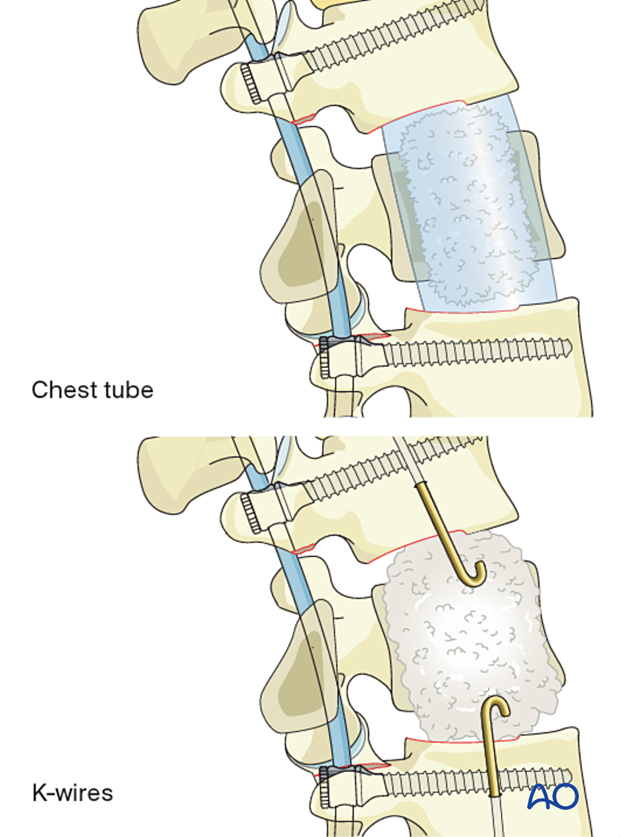
During the hardening process of the PMMA, there is an exothermic reaction that could damage the neural elements.
It is, therefore, important to irrigate and continuously mold the PMMA to keep it in place until it is solid and the exothermic reaction is completed.
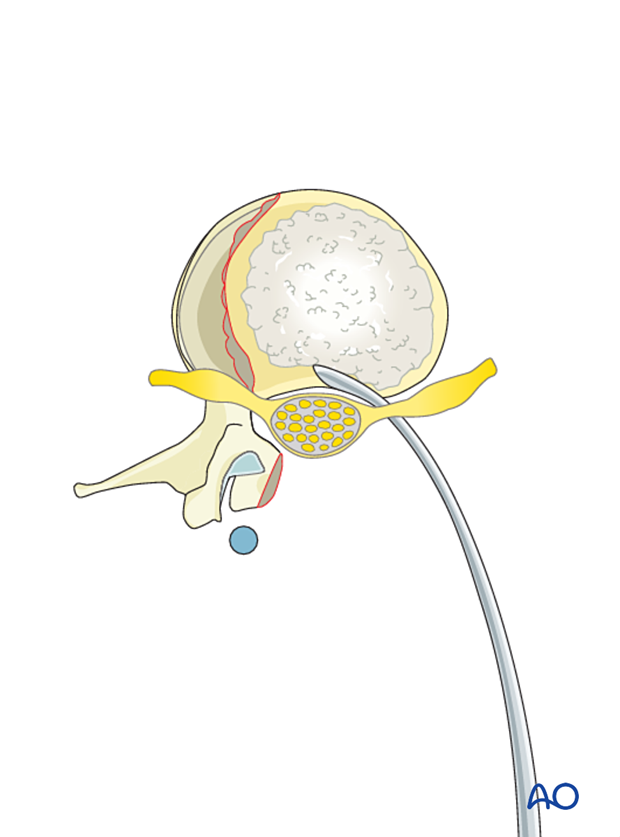
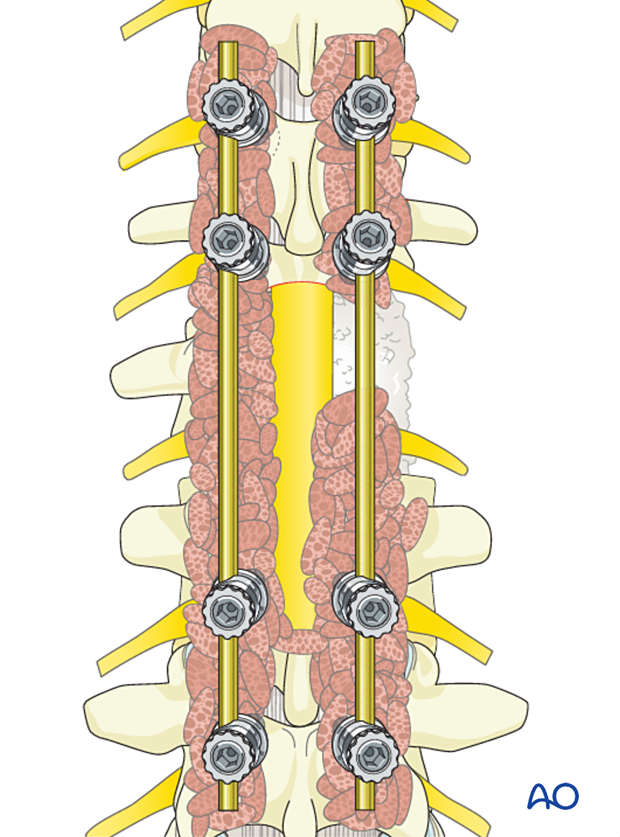
7. Final rod insertion
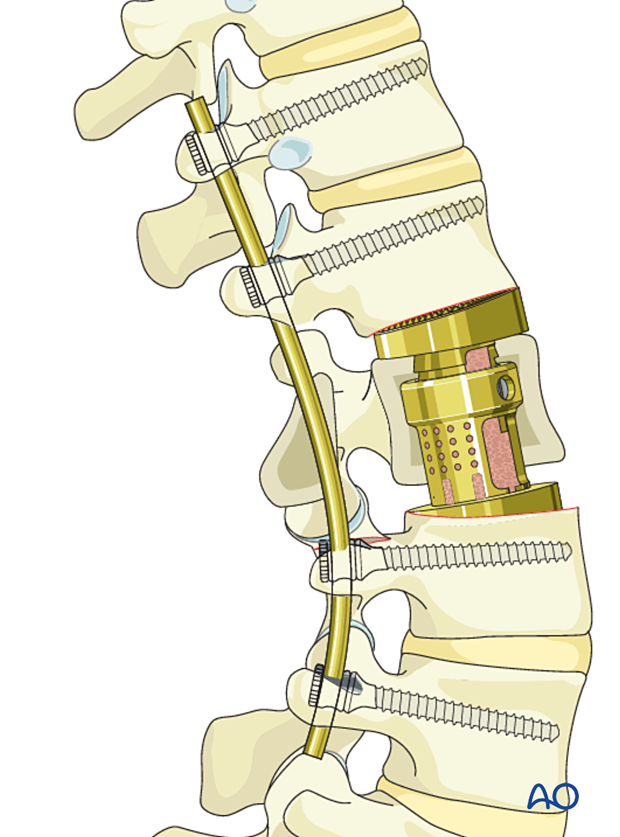
Complete the rod insertion.
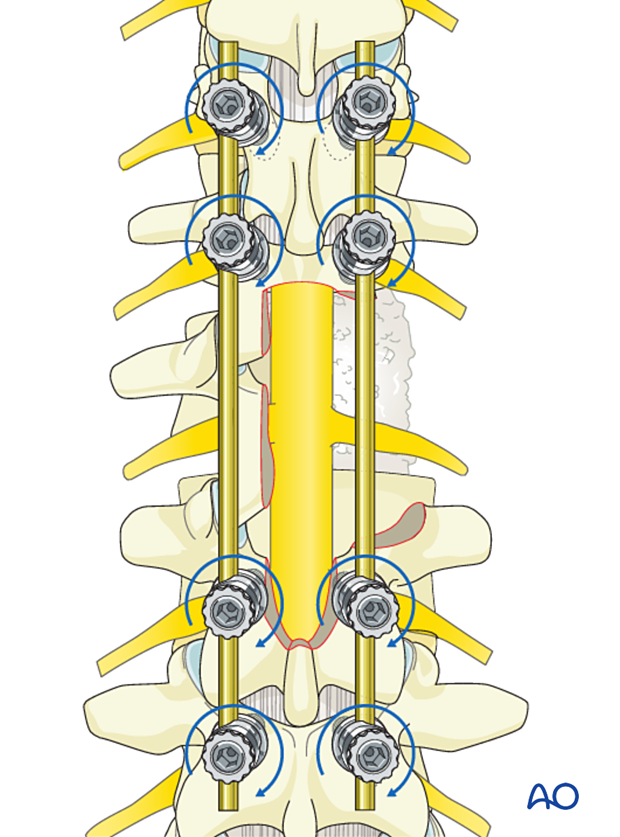
The final construct is shown from a lateral view.
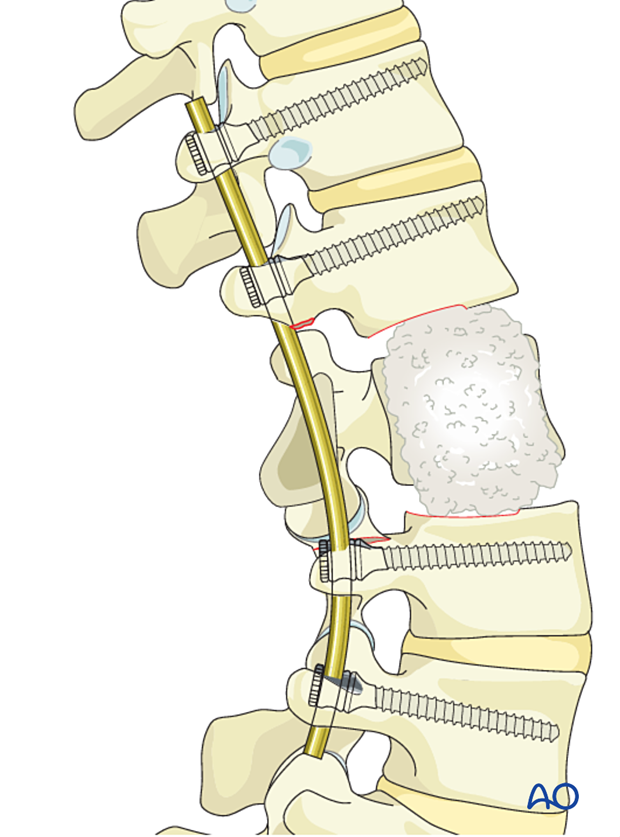
8. Posterior fusion
Preparation for fusion
Excise the facet capsule and denude/curette the joint surface cartilage surfaces and the posterior cortex.
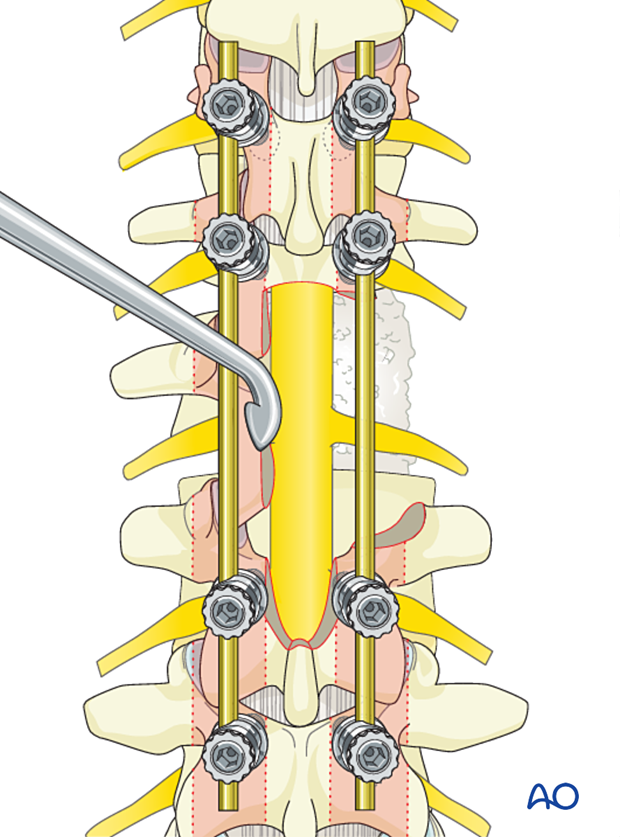
Grafting
Insert pieces of bone graft (autograft, allograft) into the decorticated facet joint for fusion.
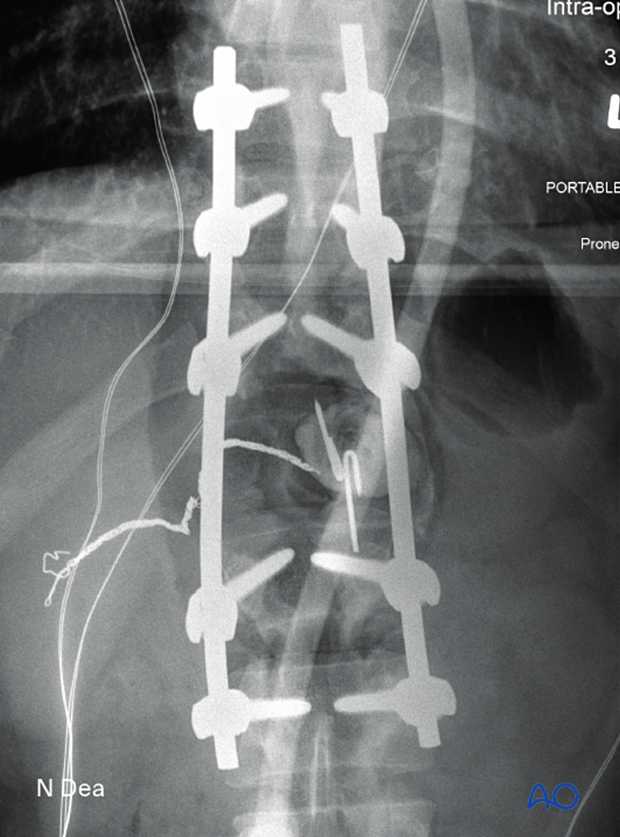
9. Intraoperative imaging
Before wound closure, intraoperative imaging is performed to check the adequacy of reduction, position, and length of screws, and the overall coronal and sagittal spinal alignment.
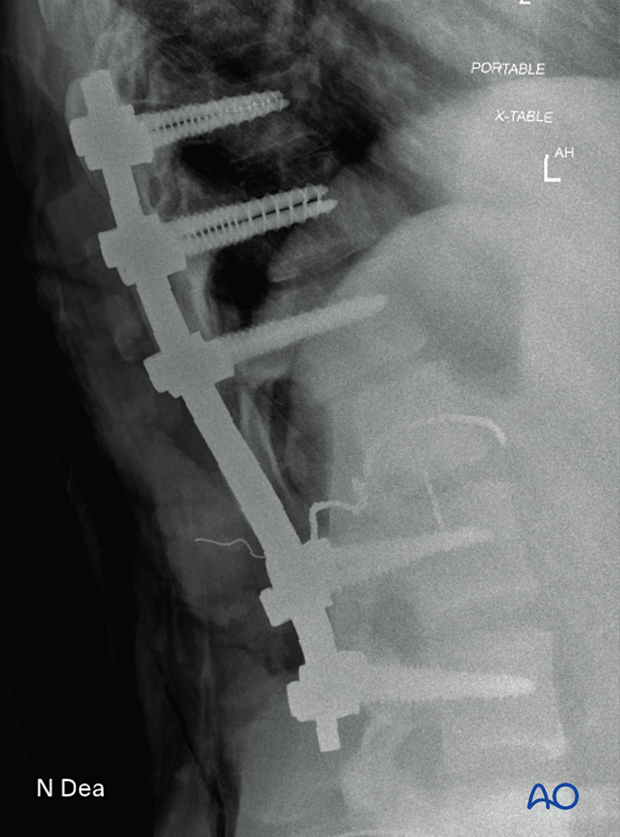
Lateral view of the above case
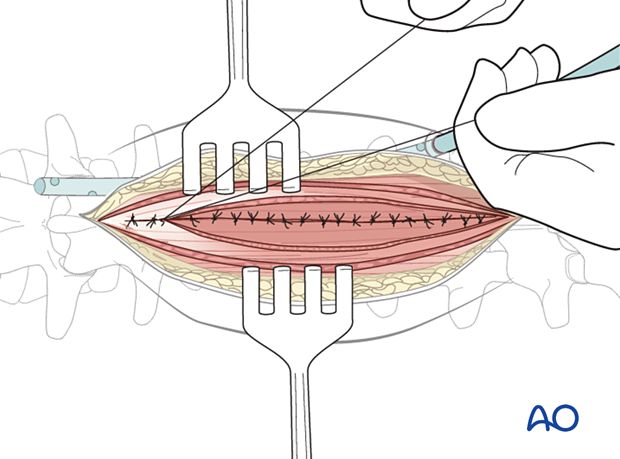
10. Posterior closure
Perform a multilayer closure as described in the approach.
For patients undergoing tumor surgery and/or with a history of radiation:
- Plastic surgery should perform soft-tissue reconstruction to decrease the risk of wound complications.
- Intrawound vancomycin can be applied to decrease the risk of postoperative wound complications.
11. Aftercare
Patients are made to sit up in bed on the first day after surgery. Patients with intact neurological status are made to stand and walk on the first day after surgery.
Patients can be discharged when medically stable or sent to a rehabilitation center if further care is necessary.
Throughout the hospital stay, adequate caloric intake of a high-quality diet should be monitored.
Patients are generally followed with periodical x-rays at 6 weeks, 3 months, 6 months, and 1 year to monitor for hardware failure and with an MRI every 6 months for tumor surveillance.
Some primary benign tumors of the spine can recur years after surgery, and long-term tumor surveillance is important.













