ORIF - Conventional plates
1. Principles
General considerations
These fractures are the most severe. They require a great deal of expertise and judgment and if possible should be referred to someone who has the expertise and resources to cope with them. Anatomical reduction of the articular fracture component is mandatory. When dealing with the metaphyseal component of the fractures, it is more important to retain vascularization of the multiple fracture fragments than to reduce them anatomically.
In order to illustrate the difficulties that may be encountered, we have included a full discussion under the respective sections.
Main steps in treatment include:
- Temporary reduction and immobilization until definitive surgery (eg, external fixator)
- Adequate preoperative planning (is a bone graft necessary, what type of approach, the number and type of implants, and any additional equipment).
- Make an arthrotomy between the meniscus and the tibia. This will allow for adequate visualization of the articular fracture. Inspect the meniscus for any tears. These will have to be repaired at the end.
- Anatomical reduction of the articular surface with disimpaction of fracture fragments.
- Bone grafting of the metaphyseal defect once the fragments are disimpacted and the articular component elevated.
- Reduction of the metaphysis and provisional fixation with K-wires.
- Definitive stable fixation of the metaphysis using screws and plate(s) with preservation of the blood supply of the metaphyseal fragments.
Timing of surgery
Surgery should be delayed until full recovery of soft tissues (swelling, blisters, abrasions, etc). This takes usually 3 to 10 days.
Until surgery, length of the leg should be maintained (eg, external fixator, traction, etc).
Plate location
Plate location depends on the fracture morphology. The plate is used to buttress the fragments. On the medial side, if the fracture morphology allows, the plate may be placed on the anteromedial surface. Most commonly, the wedge fragment is split off in such a way that to buttress it adequately the plate must be positioned posteromedially.
Double plating
To prevent collapse these fractures require buttressing on the medial as well as lateral side. The position of the medial plate will depend on the fracture pattern. Most often it is positioned on the posteromedial crest of the tibia.
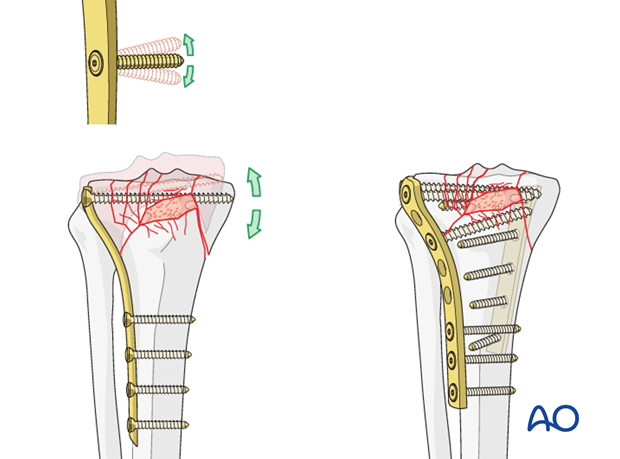
Medial or lateral side first?
Most often the medial fragment is less comminuted and should be addressed first in order to restore the anatomical relationship of the medial joint surface, original length and rotation. Therefore, in the majority of cases the medial approach is carried out first and the medial fracture is reduced and fixed provisionally with a buttress plate with the minimum number of screws necessary. Because occasionally the reduction and fixation of the medial side has to be readjusted as the lateral side dealt with.
The lateral fracture is addressed next. Once a satisfactory reduction and fixation is reached on the lateral side, the fixation on the medial side is completed and the wounds are closed in a routine fashion.
Potential complications
- Articular damage
- Vascular and nerve injury (peroneal nerve)
- Compartment syndrome
Check for these during surgery. Do not close the fascia to prevent compartment syndrome.
2. Preparation
Patient positioning
Depending on the approach, the patient may be placed in the following positions:
Use of a tourniquet
A tourniquet should be applied in every case. Whether the tourniquet is used depends on the amount of bleeding. Exsanguinate the limb by elevating it.
Use of a radiolucent table
To allow for intraoperative radiographic control of reduction and fixation, the use of a radiolucent table is mandatory.
Preparation for bone graft
In complete articular fractures with multifragmentary metaphyseal and multifragmentary articular fractures, preoperative planning should include computer tomography in every case. This will help to evaluate the size of the defect and to determine the need for bone grafting.
If autologous bone grafting is planned the anterior iliac crest should be prepared and draped as well as the limb.
3. Approaches
Not all complete articular fractures can be perfectly reduced through a medial/posteromedial and/or an anterolateral approach. Sometimes fractures with a flexion injury mechanism need to be addressed through a posterior approach as well.
4. Preliminary reduction
General consideration
Rotation, length and axial alignment should be restored first by axial traction (distractor, external fixator or manual traction).
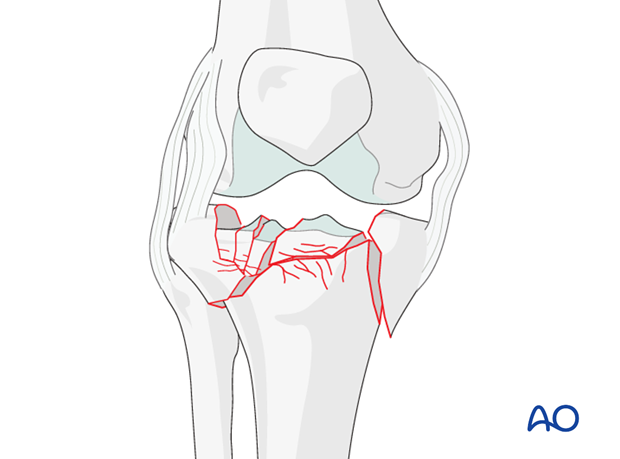
Ligamentotaxis
Ligamentotaxis helps to achieve preliminary reduction of the main fracture fragments and helps to maintain length during the operation. It is also used preoperatively to maintain provisional reduction.
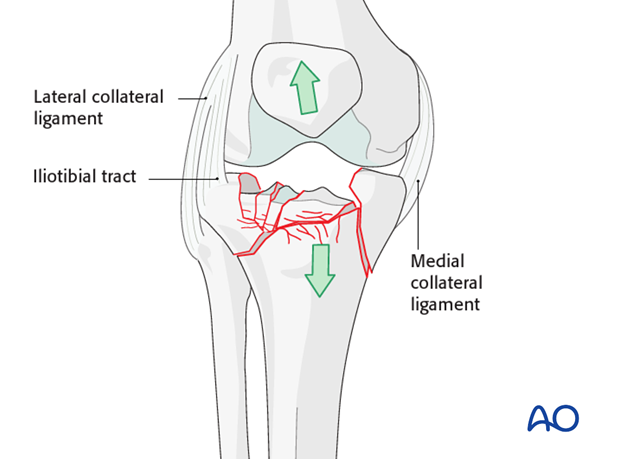
Use of distractors and external fixators
In order to reduce these complex fractures one may need to use two femoral distractors one on the medial and one on the lateral side. To do this place the knee in slight flexion.
One can also achieve the same with the use of two external fixators or one distractor and one external fixator. The use of the external fixators makes intraoperative adjustments almost impossible because they do not allow for rotational or angular correction.
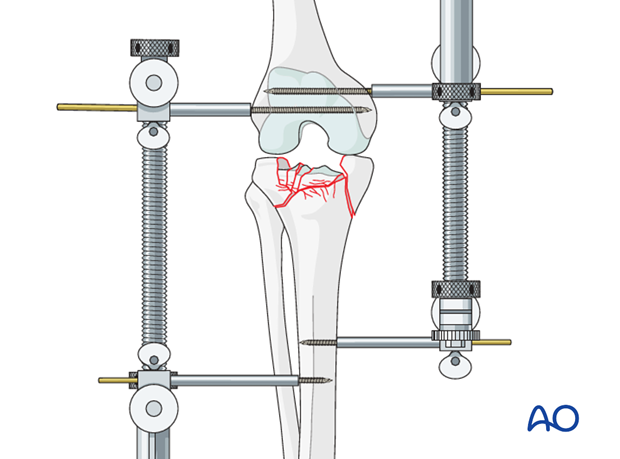
Distractors, because they apply the force directly to the bone, are very powerful and make distraction easy. Use the distractor on the side with more comminution. Usually, the medial side can be managed with an external fixator because it is usually less comminuted. If only external fixators are available, place one on the medial and one on the lateral side or span the knee joint anteriorly with a unilateral frame.
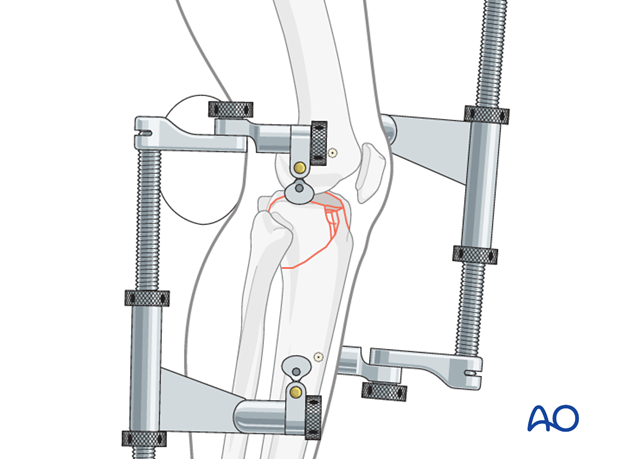
5. Reduction of the articular surface
General consideration
Generally, the medial plateau is reduced first because it is usually less comminuted and allows the surgeon, once reduced, to reestablish normal length, rotation, and alignment of part of the articular surface.
It is then provisionally fixed and one turns one’s attention to the lateral side which is accessed through an anterolateral parapatellar incision. After elevation and reduction of the depressed articular surface, bone graft (autologous, allograft, or bone substitute) the defect in the metaphysis to prevent future collapse of the reduced articular surface, reduce the metaphysis, secure provisional fixation with K-wires, check radiographically and if satisfactory complete the fixation with a lateral buttress plate.
Open book technique
Hinge the main fragments back on their soft-tissue attachments and visualize the depression of the articular fracture. Reduce the impaction by gentle elevation. Once this is completed, reduce the metaphyseal fracture by indirect or direct manipulation. The metaphysis, if possible, should be reduced anatomically to restore inherent stability.
A pointed reduction forceps is a very useful tool in securing reduction of the main fragments and their provisional fixation.
In these complex fracture patterns, arthroscopy is not helpful.
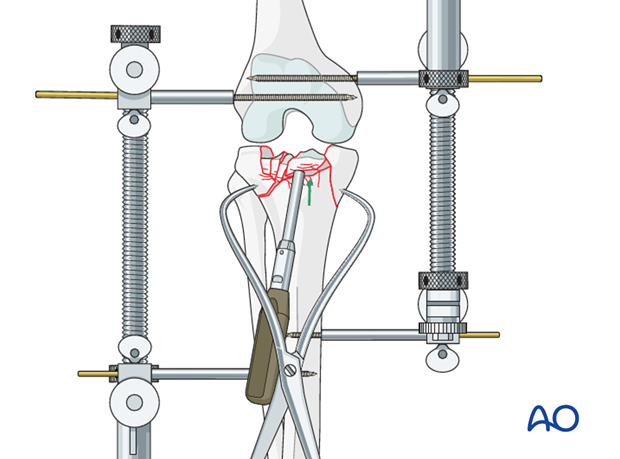
Secure reduction
In multifragmentary proximal bicondylar articular fractures, be careful when you insert lag screws so as not to narrow the width of the proximal tibia.
The same holds true when one is using the pointed reduction clamps for provisional fixation.
Once the fracture is reduced, further provisional fixation is achieved with K-wires and the reduction checked with image intensification.
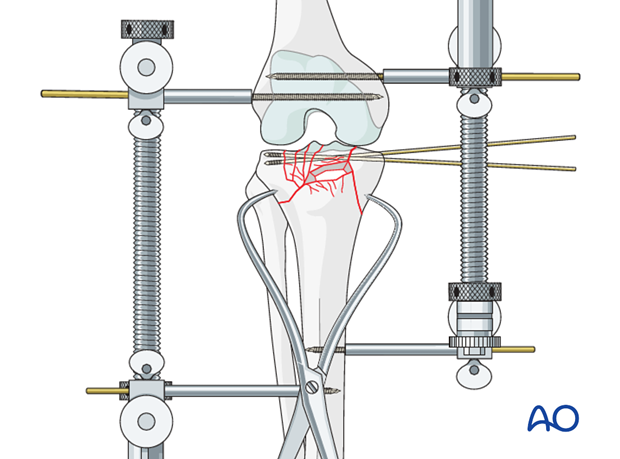
Bone grafting
After elevation and reduction of the depressed articular surface, bone graft (autologous, allograft, or bone substitute) the defect in the metaphysis to prevent future collapse of the reduced articular surface. Occasionally, the fragments may be sufficiently large so that re-displacement is prevented by the lag screw fixation. Under those circumstances, a bone graft can be omitted.
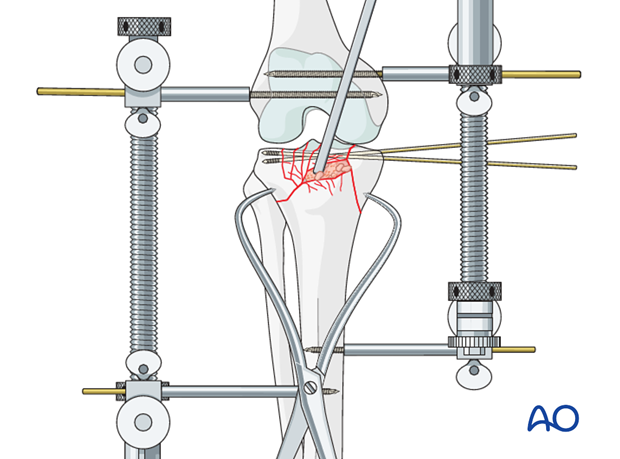
6. Medial column fixation
Plate application on medial side
Definitive fixation of the medial plate is secured whenever possible with bicortical screws but care must be taken that these do not interfere with the antero-lateral plate placement.
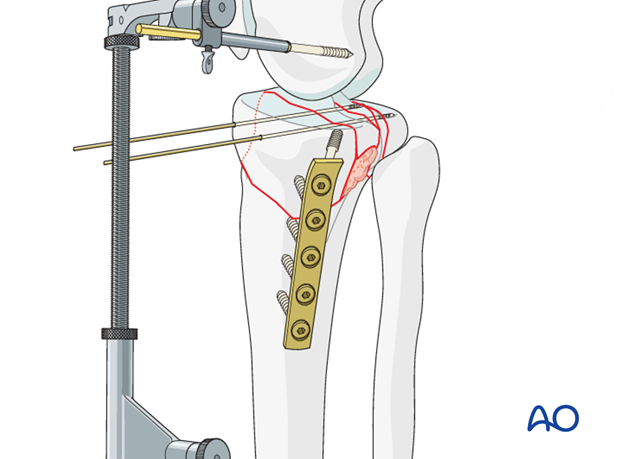
7. Lateral column fixation
Placement of lag screw and buttress plate
The placement of the lag screw or screws used to achieve absolute stability of the articular surface is determined by the fracture pattern. Ideally, these screws should be inserted at right angle to the fracture plane.
In multifragmentary fractures of both the medial and lateral tibial plateaus, one must be careful in using lag screws so as not to narrow the proximal tibia by overtightening. If this risk exists, use fully thread screws because when you tighten them as long as they have adequate purchase in the lateral and medial fragment a lag effect will be avoided.
The buttress plate, once properly contoured, is inserted on top of the periosteum deep to the muscle envelope. The most proximal screw if it fits with the fracture morphology may be a lag screw.
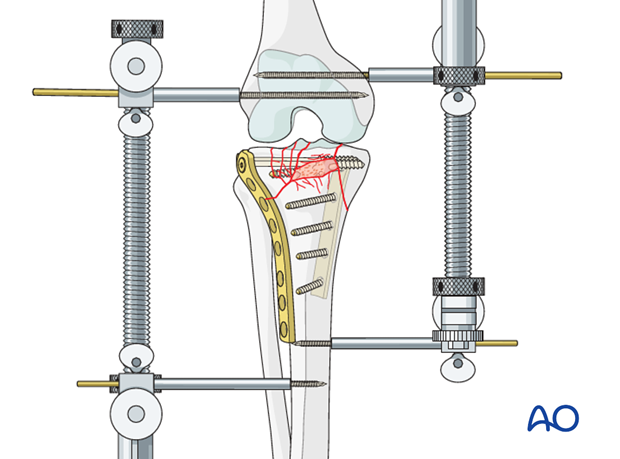
Additional screw placement
Once fixation is completed, remove the K-wires. If some fragment would benefit from further screw fixation, insert a screw (or screws) in such a way that it/they do not interfere with the screws inserted through the plate.
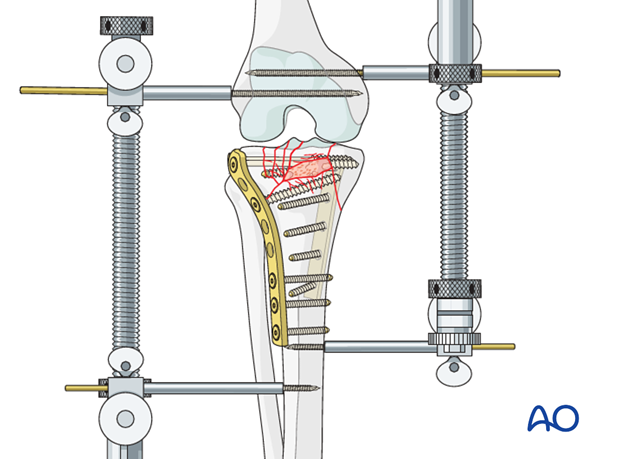
Final osteosynthesis
Once osteosynthesis is completed, make a final check with the image intensifier. If all is well, remove the distractor.
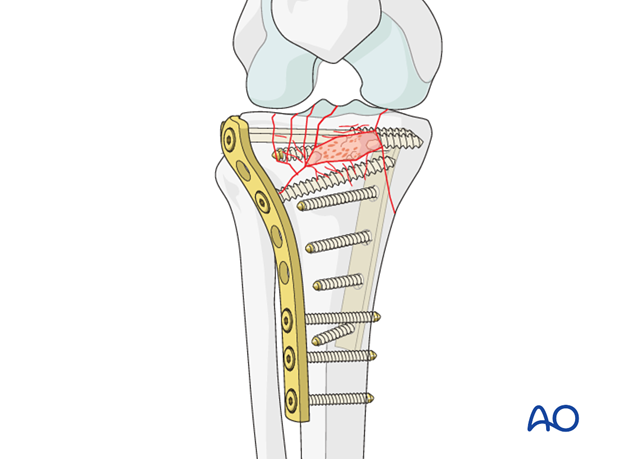
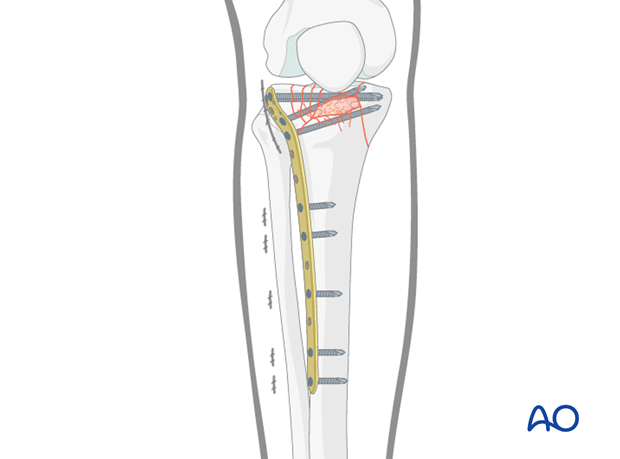
8. Alternative: angular stable plate
If one is using an angular stable implant (eg, lateral tibial plate with locking screws) the application of a medial plate might not be necessary if the medial cortex is not comminuted and is stable after lateral fixation.
9. Aftercare
Compartment syndrome and nerve injury
Close monitoring of the tibial compartments should be carried out especially during the first 48 hours after surgery to rule out compartment syndrome.
The neurovascular status of the extremity must be carefully monitored. Impaired blood supply or developing neurological loss must be investigated as an emergency and dealt with expediently.
Functional treatment
Unless there are other injuries or complications, mobilization may be performed on post OP day 1. Continuous passive motion (CPM) splints are very helpful in the early phase of rehabilitation. Static quadriceps exercises with passive range of motion of the knee should be encouraged. Afterwards special emphasis should be given to active knee and ankle movement.
Following any injury, and also after surgery, the neurovascular status of the extremity must be carefully monitored. Impaired blood supply or developing neurological loss must be investigated as an emergency and dealt with expediently. The goal of early active and passive range of motion is to achieve as full range of motion as possible within the first 4 - 6 weeks. Optimal stability should be achieved at the time of surgery, in order to allow early range of motion exercises.
Weight bearing
No weight bearing in the treatment of articular fractures for a minimum of 10 – 12 weeks.
Follow up
Wound healing should be assessed on a short term basis within the first two weeks. Subsequently a 6 and 12 week follow-up is usually performed. If a delayed union is recognized, further surgical care will be necessary and should be carried out as soon as possible.
Implant removal
Implant removal is not mandatory and should be discussed with the patient.