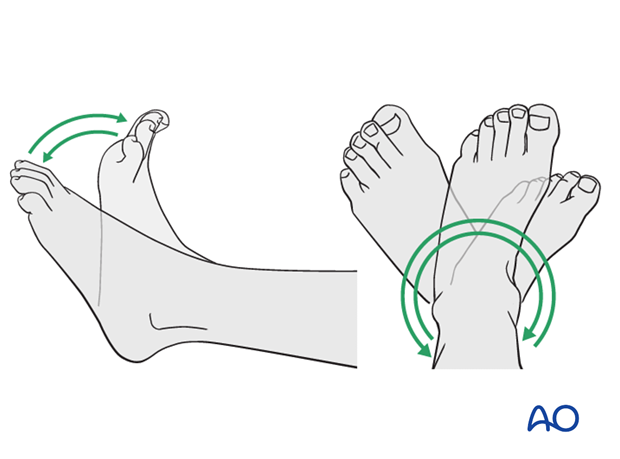
ORIF - Lag screw and protection plate
1. General considerations
Principles
The soft-tissue conditions usually dictate the choice of procedure: early single-stage or multiple-stage surgery.
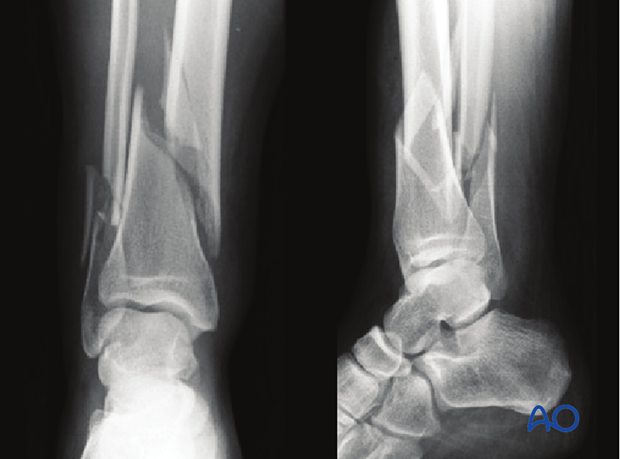
Displaced fractures with minimal, closed soft-tissue injury
(Tscherne classification, closed fracture grade 0, rarely grade 1)
These injuries may be reduced and fixed primarily, as a single stage procedure, if the soft tissues are in truly excellent condition. A distractor or external fixator may aid reduction. Fibular reduction and fixation is the usual next step, but this reduction must be accurate, so that it does not prevent tibial reduction. Finally, the tibial plate is introduced, and final reduction of length, alignment and rotation is achieved.
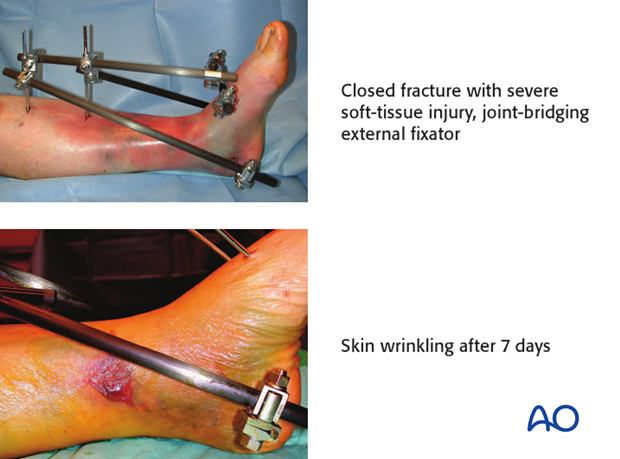
Grossly displaced fractures and/or fractures with severe, closed soft-tissue injury
(Tscherne classification, closed fracture grade 2 or 3)
It is generally advisable to proceed in two or more stages:
- Closed reduction and joint bridging external fixation
- Definitive MIO reconstruction after 5-10 days (wait for the appearance of skin wrinkles)
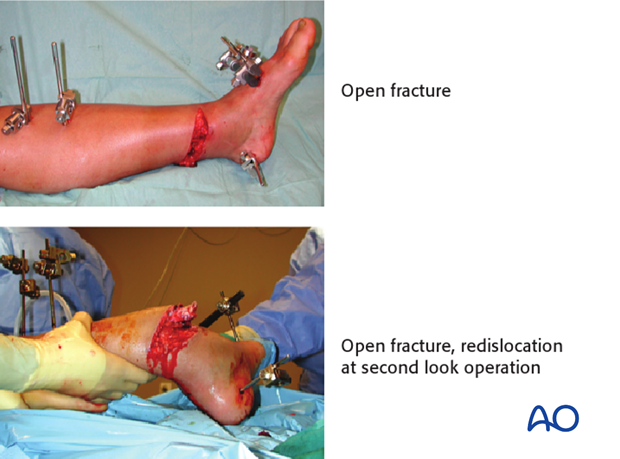
Open distal tibial fractures
These are very severe injuries which may require plastic surgery for soft-tissue reconstruction. The management includes several stages:
- Emergency management: Wound debridement and lavage. Joint-bridging external fixation and stabilization of the fibula (if needed and soft tissues allow). Where possible, closure or coverage of any opening into the joint should be achieved.
- After 48 hours: Soft-tissue coverage (local or free flap). Plan for definitive stabilization at this time.
- Definitive stabilization: Direct reduction and absolute stability with plate and lag screw fixation
2. Fibula or tibia first? Sequence of bone stabilization
Introduction
If the fibula is fractured, it usually needs to be stabilized.
Simple fibular fractures
This fracture is usually addressed first with open anatomic reduction and plate fixation. Alternatively, for transverse fractures, consider a small diameter, flexible intramedullary nail. Fibular reduction helps realign the tibia fracture.
Multifragmentary fractures of the fibula
Some fibular fractures are complex, and reduction may be difficult. Any malreduction of the fibula will impede anatomic reconstruction of the tibia. In this situation, fibular ORIF is better performed after the tibia has been fixed. The syndesmotic ligaments are usually intact, so gross realignment of the fibula occurs with reduction and fixation of the tibia. For comminuted fibular fractures a MIO technique with a long bridging plate, or intramedullary fixation of the fibula with a small diameter, flexible nail is easily achieved after tibial reduction and fixation. Fibular nailing is particularly applicable if the soft-tissue injury or complexity of the fracture makes extensive exposure for internal fixation hazardous.
3. Preoperative planning
Planning of reduction and fixation
Preoperative planning is an essential part of treatment of all distal tibial fractures. It consists of:
- Careful study of the x-rays and CT scan
- Drawing of both the fracture fragments and the desired end result
- Consideration of intraoperative reduction techniques
- Choice of implants
Reduction can be achieved by ligamentotaxis alone with indirect manipulation. A precise anatomical reduction is required for absolute stability. This may require open reduction. If bridge plating and relative stability are chosen, the reduction of this extraarticular fracture is somewhat less critical, but better reduction may still be beneficial if soft-tissue attachments can be preserved.
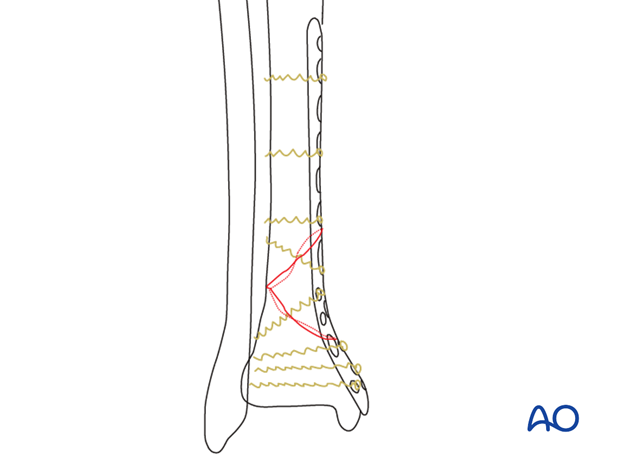
4. Patient preparation and approaches
Patient preparation
This procedure is normally performed with the patient in a supine position.

Anteromedial approach
The anteromedial approach is used for open reduction and internal fixation of the articular part of the tibia. It facilitates accurate articular reduction combined with submuscular and subcutaneous plate applications.
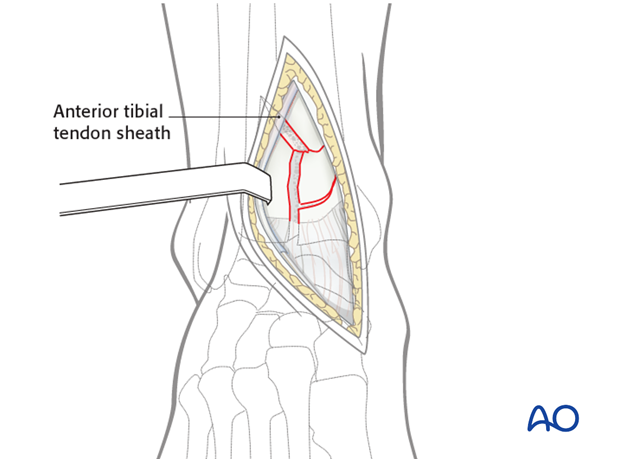
Anterolateral approach
The anterolateral approach is useful in the majority of complete articular pilon fractures, anterior and anterolateral partial articular pilon fractures, and some extraarticular distal tibia fractures.
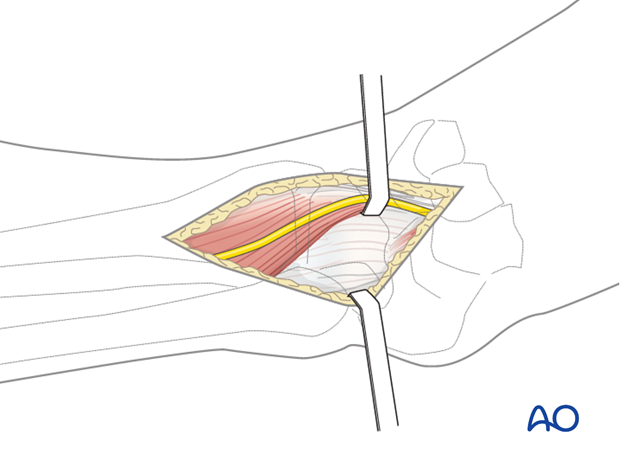
5. Implant choice and plate preparation
Implant choice
A variety of precontoured distal tibial plates are available.
Plate contouring
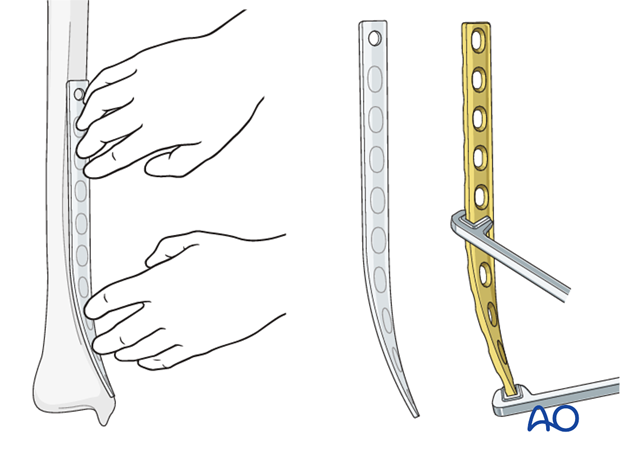
If precontoured implants are not available, a non-contoured plate can be shaped prior to sterilization, using a sawbones model as a template. Determine the length of the plate from preoperative x-rays. It should be placed as distally as possible and long enough to place at least four holes proximal to the fracture (with screws in at least three of them).
The most distal 8-12 cm of the plate must be bent to form a concave arc with a radius of curvature of about 20 cm and twisted to fit the distal tibia. As illustrated, the medial tibia is internally rotated distally (20 degrees) and lies closer to the sagittal plane.
A small or large fragment plate, or contoured periarticular plate is chosen based on patient size.
If locking head screws must be perpendicular to the plate, their orientation in the distal segment may not be satisfactory. Thus, conventional screws may be better in at least some distal plate holes.
With ORIF of metaphyseal wedge distal tibia fractures, enough of the tibial surface may be exposed to aid and assess plate contouring.
6. Reduction
Indirect reduction with a distractor
An appropriately positioned “femoral” distractor or external fixator is a very helpful tool for reduction.
Medial positioning allows subcutaneous access to the tibia. A laterally based distractor requires a pin through the anterior muscular compartment but provides more efficient distraction of any associated fibular fracture, and correction of valgus deformities.
Distraction can be used for the open reduction and plate fixation of the fibula as first step (in case of simple fracture pattern of the fibula) and for the reduction of the tibia.
Schanz screws are positioned in safe zones of the tibial shaft and talar neck (or the calcaneal tuberosity). In case of previously applied joint-bridging fixator, the already existing Schanz screws can be used.
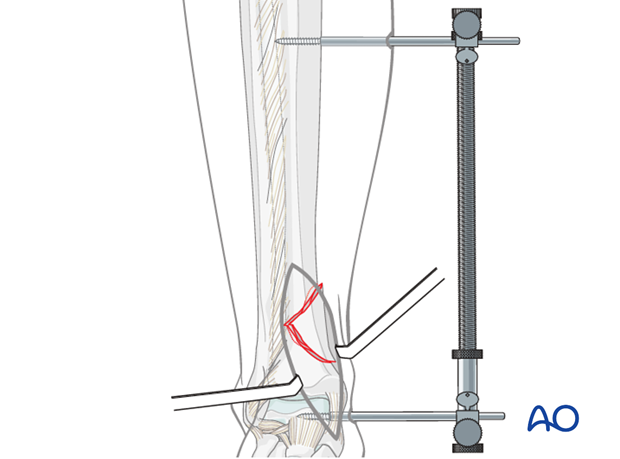
Direct reduction
Once the fracture has been exposed, taking care to preserve soft-tissue attachments, the fracture can be reduced anatomically.
Incarcerated or displaced fragments can usually be reduced directly. Pointed reduction clamps, dental picks, small Hohmann retractors, or joysticks are some of the instruments available.
Provisional fixation with K-wires is usually required.
Note: K-wires should not interfere with planned plate and screw position. See also the content on assessment of reduction.
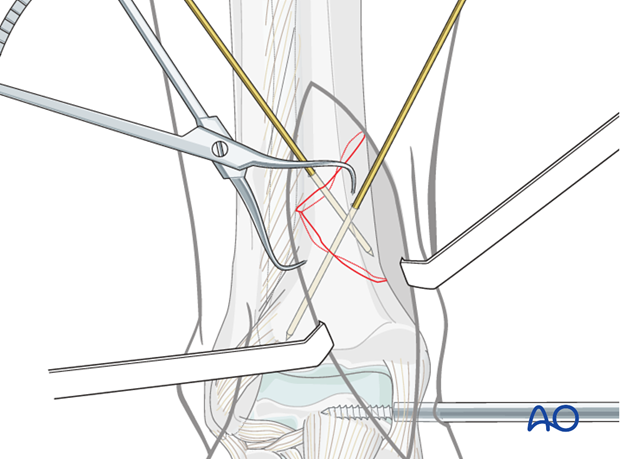
7. Plate insertion and provisional stabilization
Insertion of the plate
The plate is inserted from distally through the existing incision. Depending on the fracture situation, the plate is usually positioned on the anteromedial aspect, or seldom, on the anterior crest of the tibia. If possible, the plate should be positioned so that the fracture can be lagged with screws passing through the plate. Occasionally it is necessary to insert the lag screws prior to plate application.
It is often possible to pass the proximal end of the plate in a minimally invasive fashion and insert the screws percutaneously at the end of the procedure.
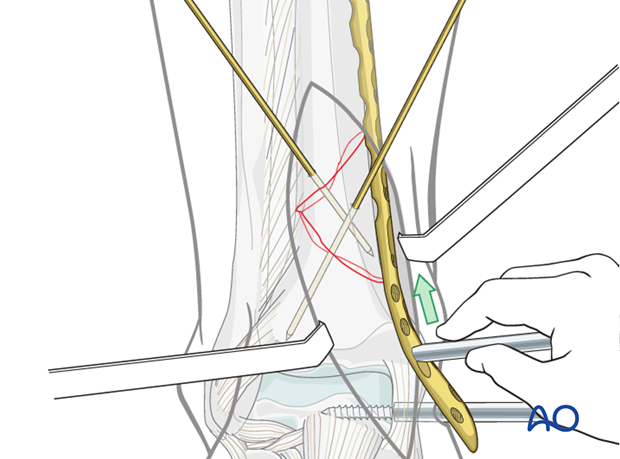
Provisional plate stabilization
Once accurate reduction has been confirmed, a conventional screw can be inserted to provide initial plate stabilization and confirm satisfactory contouring (see the content on assessment of reduction).
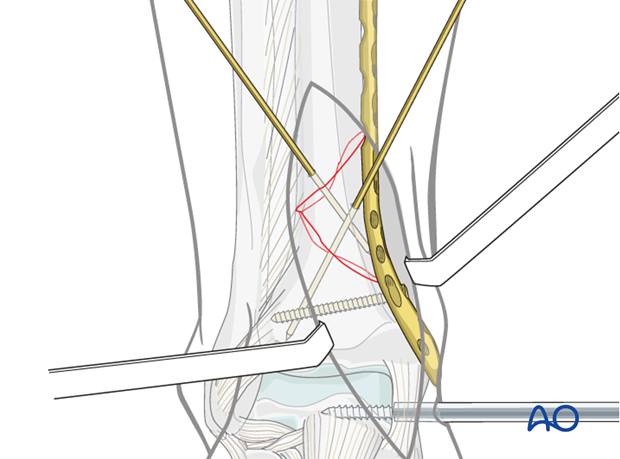
8. Applying interfragmentary compression
Most larger butterfly fragments are suitable for reduction and stabilization with lag screw(s). Usually two screws are required. The goal is to achieve perfect reduction and compression with a lag screw either through the plate or separate to it.
Screw placement and direction are important:
- The ends of the wedge fragment should be avoided
- Each lag screw should be aimed perpendicular to the fracture plane
- Fully threaded screws should be inserted through overdrilled glide holes
See also the additional material on lag screw principles.
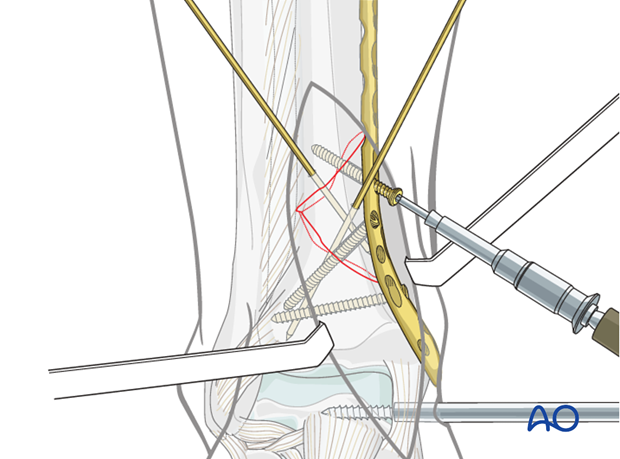
9. Definitive plate fixation
Further proximal and distal screw insertion is completed. The number and position of the screws is dependent on the individual fracture pattern. Ideally, the concept of “balanced” fixation should be achieved with an equal number of screws on either side of the fracture.
Place screws in at least three of the four (minimum) proximal holes, including the most proximal. The chosen distal tibial plate should allow placement of at least three or four screws distal to the fracture.

Wound closure
The wound is closed in layers over the plate and fracture. Skin sutures alone are sufficient for proximal screw incisions. A suction drain is optional.
Final assessment
X-rays at the end of the operation confirm the anatomic reduction and fixation of the fracture.
10. Aftercare following plating
Leg elevation is recommended for the first 2-5 postoperative days. Physiotherapy with active assisted exercises is started immediately after operation. Immobilization is not necessary.
Mobilization
Starts depending on the wound healing with flat footed, weight of the leg weight bearing (10-20kg).
Follow up
Clinical and radiological follow-up is recommended after 2, 6 and 12 weeks. Depending on the consolidation, weight bearing can be increased after 6-8 weeks with full weight bearing usually after 3 months. Supervised rehabilitation with intermittent clinical and radiographic follow-up is advisable every 6-12 weeks until recovery reaches a plateau, typically 6-12 months after injury. Weight-bearing radiographs are preferable to assess articular cartilage thickness. Angular stable fixation may obscure signs of non-union for many months.
Implant removal
Implant removal may be necessary in cases of soft-tissue irritation by the implant (plate and/or isolated screws). The best time for implant removal is after complete remodeling, usually at least 12 months after surgery.