Anterolateral approach to the distal tibia
1. Introduction
The anterolateral approach is useful for:
- Many complete articular pilon fractures
- Anterior and anterolateral partial articular pilon fractures
- Some extraarticular distal tibia fractures stabilized with a submuscular anterior compartment plate
The anterolateral approach offers excellent visualization of the tibial articular surface as far as the medial malleolus, while avoiding dissection of the anteromedial tibial face. It is well suited for an accurate articular reduction, as well as submuscular and subcutaneous plate applications spanning metaphyseal comminution. However, access to the medial ankle joint is poor, and proximal extension is limited. Advantages also include good soft tissue cover, ability to get to both tibia and fibula and if there is an open wound on the medial side.
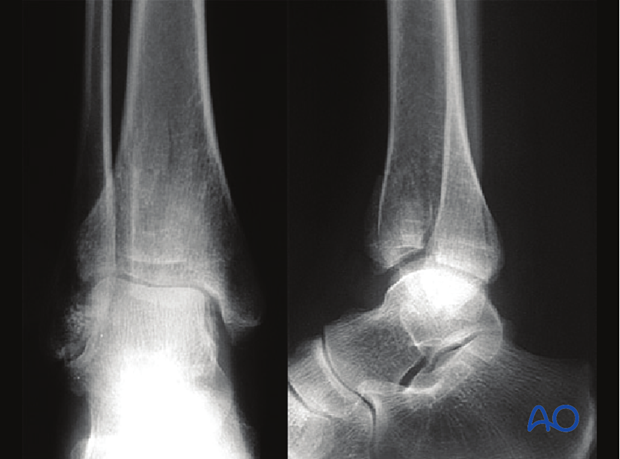
The three radiographic views show a distal tibial complete articular fracture
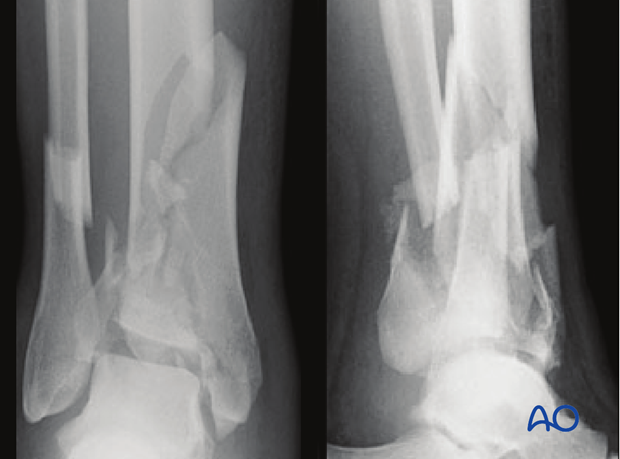
Illustration shows a partial articular distal tibia fracture.
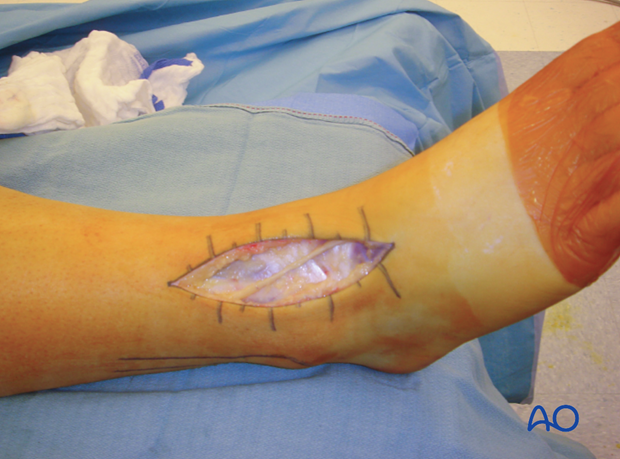
2. Skin incision
This incision is centered at the ankle joint, parallel to the fourth metatarsal distally, and parallel to and between the tibia and fibula proximally. Dissection through the skin and subcutaneous tissues should proceed sharply with maintenance of full thickness skin flaps. Since the anterior compartment muscles arise from the anterior fibula, the incision is usually not extended more than seven centimeters above the ankle joint. Distally, the incision can extend as far as the talonavicular joint.
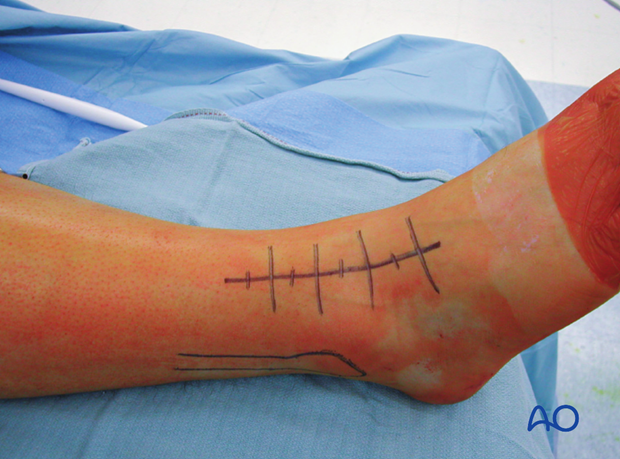
Take care not to damage the superficial peroneal nerve which lies directly beneath the skin. This nerve invariably crosses the surgical incision proximal to the ankle joint. It should be identified, mobilized, and protected throughout the surgical procedure.
3. Surgical dissection
The fascia over the anterior compartment of the distal tibia is incised sharply, beneath the superficial peroneal nerve. Distally, the extensor retinaculum is incised, and the anterior compartment tendons are all retracted medially. Proximally, the entire anterior compartment musculature, including the peroneus tertius, can then be mobilized and retracted medially. These muscles and tendons are usually easy to mobilize from the underlying anterior tibiofibular ligament, the periosteum of the distal tibia, and the joint capsule.
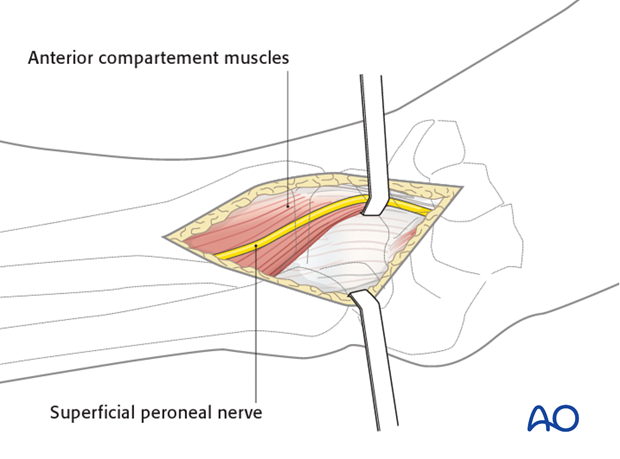
The fascia of the extensor digitorum brevis can be incised, with the muscle carefully dissected and retracted medially. This allows exposure of the talar neck for pin placement and distractor application. Proper location of the arthrotomy, preplanned to lie over the fracture, is critical to avoid unnecessary and damaging devascularization of fracture fragments. Proximally, the dissection is limited by the origin of the anterior compartment muscles from the fibula and from the interosseous membrane.
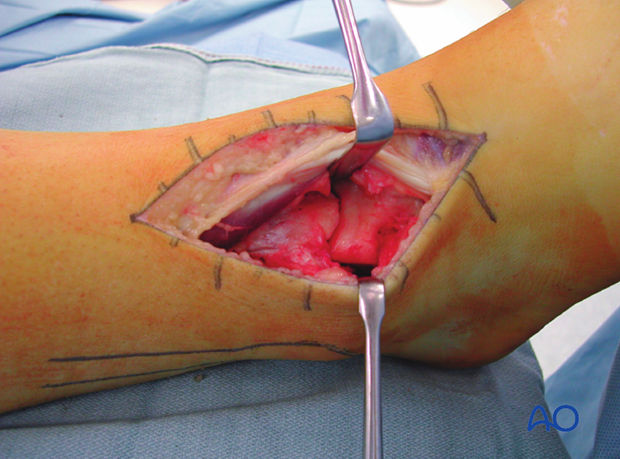
Application of a distractor
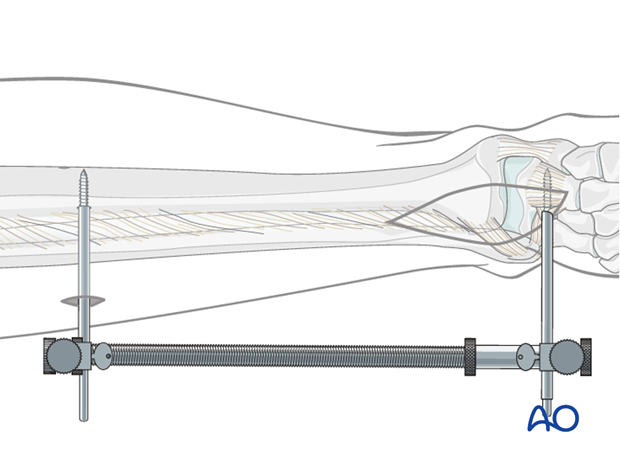
Application of a distractor intraoperatively greatly assists with articular visualization. Additionally, the distractor helps to align several of the major articular fragments. A 4 mm Schanz pin is placed transversely from lateral to medial at the talar neck through the surgical incision.
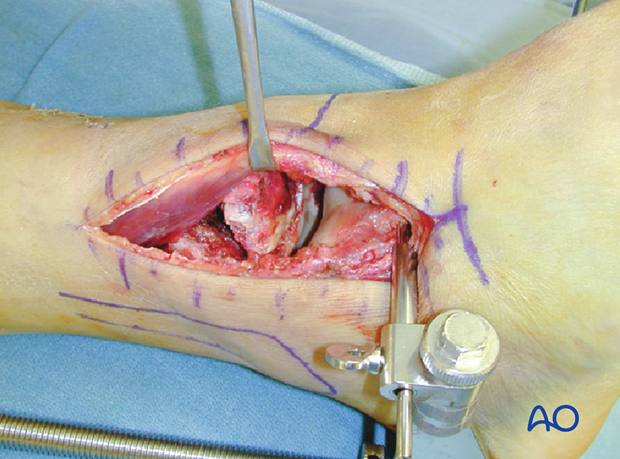
A second 4 mm Schanz pin is placed from lateral to medial at the tibia, proximal to the anticipated plate application. The pin placement in the talar neck, which is anterior to the axis of rotation of the talus, will produce ankle joint distraction and plantarflexion, maximizing articular visualization. The threaded rod of the small distractor is placed posterolaterally to avoid interference with reduction and implant placement.