Open reduction internal fixation
1. Principles
NOE type II represents a comminuted fracture. The larger bone fragments need to be reduced and stabilized. This will often require 2- or 3-point fixation.
The canthal-bearing bone fragment requires exact repositioning.
The intercanthal distance should be restored.
In severely displaced bilateral NOE fractures, the nasal projection should be restored by open reduction of nasal bone fractures as well as adding a dorsal nasal bone graft for height correction if necessary.
Rule out a CSF leak, particularly in bilaterally displaced fractures to minimize the risk of early or delayed meningitis. Injuries to the eyes and the lacrimal apparatus must also be ruled out.
Great care should be taken when placing plates anterior to the medial canthal ligament, as these may be visible through the thin overlying skin.
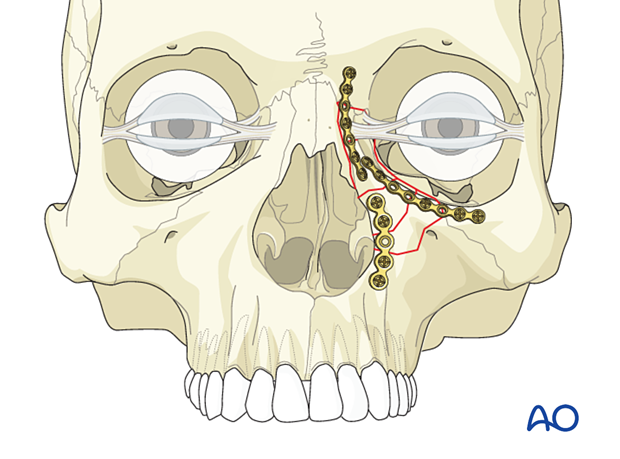
Nasal bone involvement
If nasal bones are also fractured, they should be addressed and reduced. Fixation with plates may be necessary.
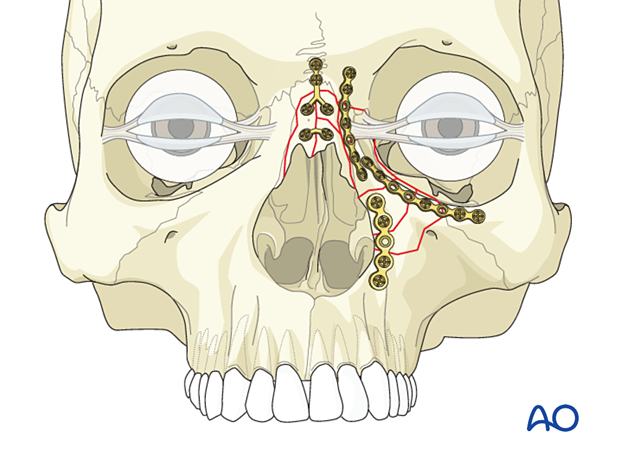
If the dorsum of the nose is comminuted or it cannot be fully reduced, reconstruction with a dorsal nasal bone graft is performed. Dorsal nasal bone grafts are obtained from the calvarium or the rib.
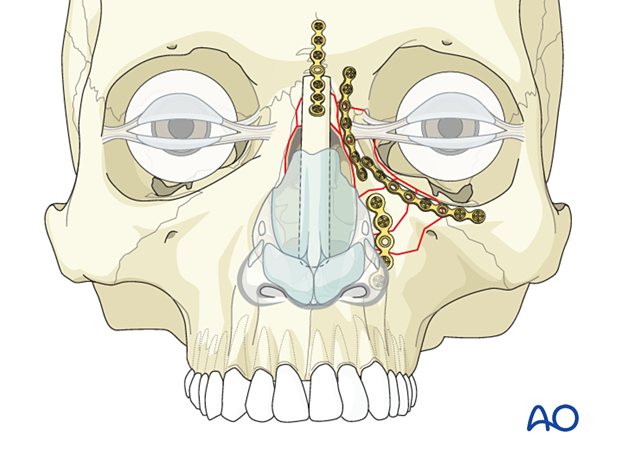
Bilateral NOE fracture with nasal bone involvement
One third of NOE type II fractures are unilateral and two thirds are bilateral. In bilateral cases, transnasal wiring of the medial canthal-bearing bone fragment on each side is indicated. Slight overcorrection of the intercanthal distance is recommended.
Intercanthal distance is 33–34 mm for white males and 32–33 mm for white females. Little data is available for other ethnic groups.
Numerous modalities may be used to hold the transnasal wire in the appropriate posterior position.
Drill holes in the canthal bearing bone fragment. They should be above and behind the canthal ligament insertion, slightly superior and posterior to the superior edge of the lacrimal fossa.
A plate placed medially superior to the canthal ligament and extending into the orbit can be used as a guide for positioning a transnasal canthopexy wire.
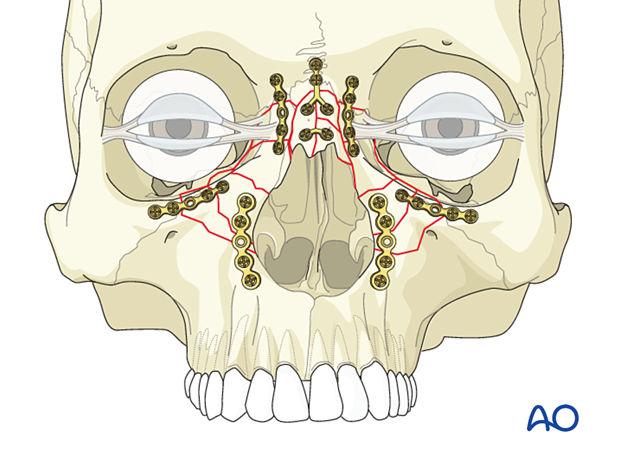
Transnasal wire
The transnasal wire technique may be required to properly reposition and fix the bone fragments.
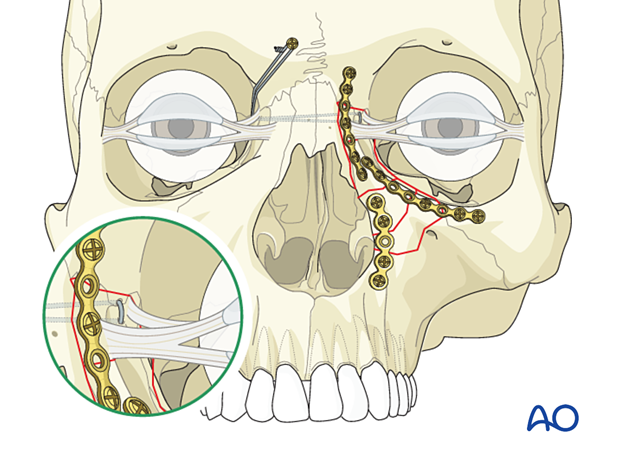
2. Selection of approach
The most common access for reduction of NOE fractures includes a combination of surgical approaches such as coronal, lower eyelid transcutaneous, lower eyelid transconjunctival, and a maxillary vestibular incision. This combination of surgical approaches is often required to visualize, reduce and stabilize extensively comminuted fractures. Additionally, the coronal approach may be useful in treating concomitant fractures of the frontal bone, nasal bones, zygomas, cranium, etc. It also provides access for harvesting calvarial bone grafts.
The glabellar approach alone does not allow enough exposure to an NOE type II fracture. The extended glabellar approach can be used with the maxillary vestibular approach in many cases.
In cases where there is a significant laceration over the nasal/NOE region, this can greatly facilitate in the access and reduction of the NOE fractures.
3. Reduction
NOE type II fractures can be challenging to reduce. This may be because of the size of the fractured fragments and poor direct access, requiring multiple surgical approaches. Great care needs to be taken to ensure that the bone fragment containing the canthal ligament is appropriately reduced and fixed into position.
While visualizing the reduction of the fractured segments through one surgical approach, the surgeon must continually recheck the reduction through the other surgical incisions. Some surgeons have used temporary plates or wires to stabilize the comminuted segments before placing the final plates.
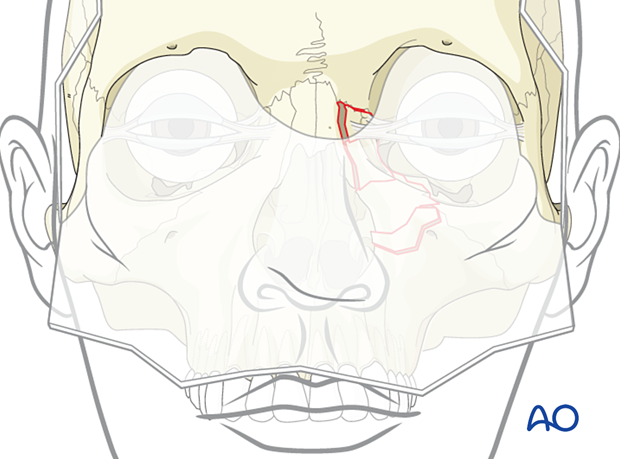
4. Fixation
General considerations
NOE type II fractures represent a comminuted fracture where the medial canthus is still attached to a small fragment of bone.
Commonly, a minimum of three points of fixation will be needed. This will include plating at the NOE/frontal bone (1), a plate along the orbital rim (2), and a plate along the piriform aperture (3). Additional plates may be needed to stabilize the comminuted fracture segments.
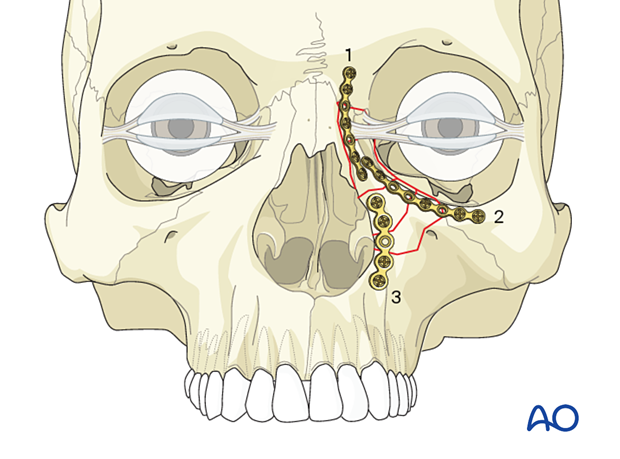
One suggestion is to place the first plate where the surgeon has the best visualization and access, with the most well-defined landmarks. If a surgeon has good visualization at all three points, it may be beneficial to fixate from the more stable fractures to the least stable fractures. A consideration is to first stabilize the NOE fracture to the frontal bone, achieving stabilization to the calvarium, with the second plate placed along the orbital rim, and the third plate placed along the piriform aperture. This prioritizes plate placement according to the order of esthetic importance and buttress stability.
Placement of first plate
In the accompanying illustration, the first plate is applied to the fracture between the NOE and the frontal bone through the coronal approach. (This can also be achieved through an extended glabellar approach.)
When possible, the surgeon must ensure that the canthal ligament and associated bony fragment are incorporated into the reduction of the comminuted segments and fixed appropriately. Otherwise, a transnasal canthopexy will be performed to resuspend the medial canthal ligament.
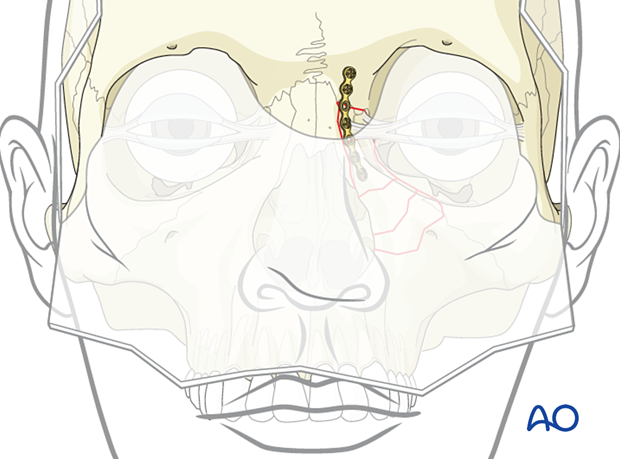
Placement of second plate
The second plate is then placed along the orbital rim through an inferior lid approach.
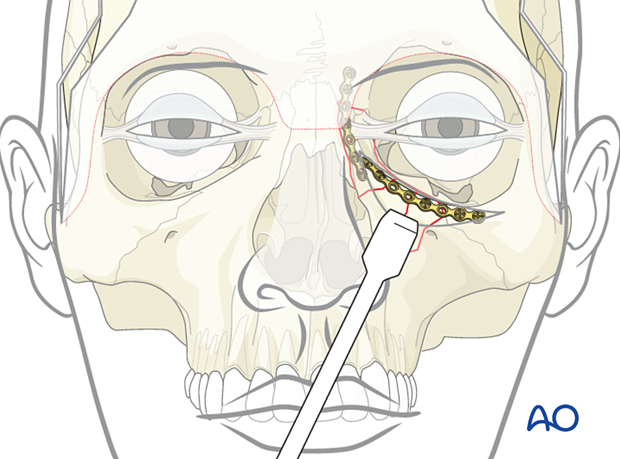
Placement of third plate
A third plate is placed along the piriform aperture through the maxillary vestibular approach.
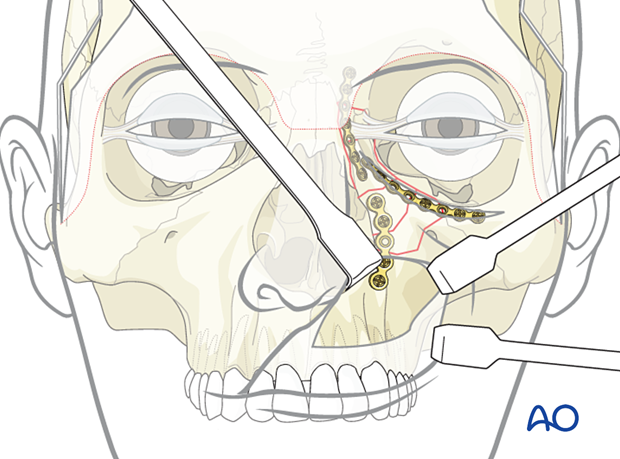
5. Option: Placement of a transnasal canthopexy wire
In some cases, transnasal wire placement may be necessary to properly reduce and stabilize the bony fragment to which the medial canthal tendon is attached.
The transnasal wire needs to be placed before any other plates.
The illustration shows the completed osteosynthesis.

Drill holes in bony fragment
Step 1: Identify the bone fragment with the attached medial canthal tendon.
Step 2: While holding the fragment with forceps, drill two holes in the bony fragment posterior to the attachment of the medial canthal ligament.
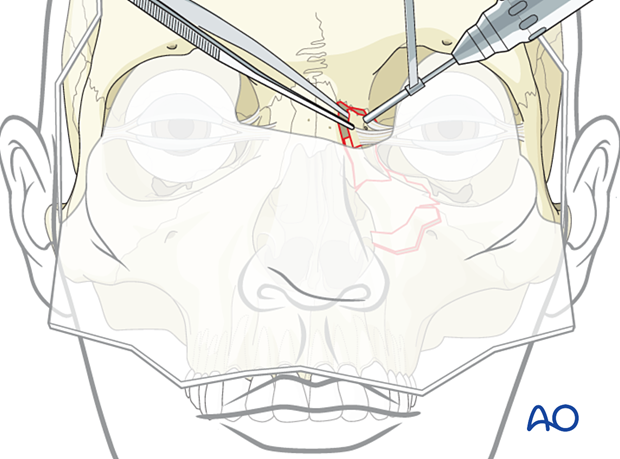
Insert the transnasal wire
Pass one end of the wire through each hole.
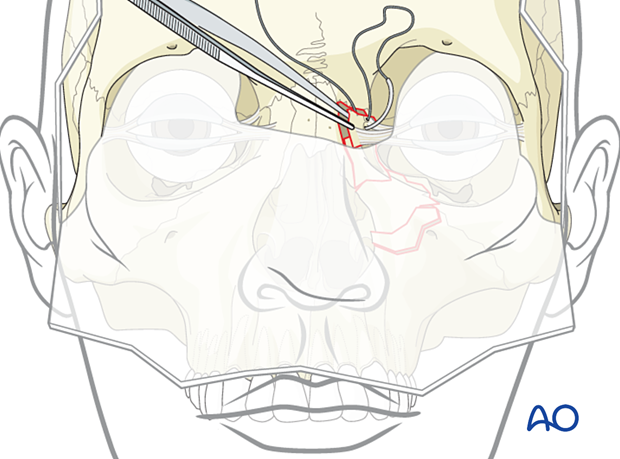
Drill hole through the NOE area
Many different techniques have been used to accomplish this. These include the use of a drill, spinal needle, or awls.
Depending on the stability of the bone in the NOE area, the surgeon may need to drill a hole from the contralateral side or use an awl to create a passageway.
Extreme caution must be used to ensure that the spinal needle or drill bit does not advance too far, injuring the contralateral globe. It is important to use a malleable retractor or spoon retractor to protect the globe.
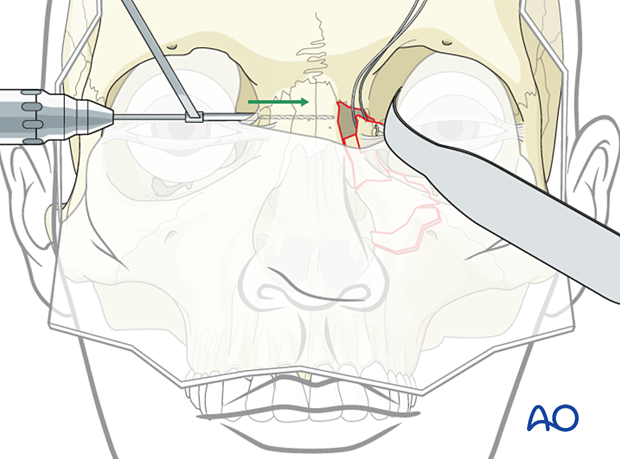
Pull the two ends of the wire transnasally
While the spinal needle is still in place, the two ends of the wire are placed through the lumen of the needle, and both the spinal needle and wire are pulled out of the contralateral side of the NOE.
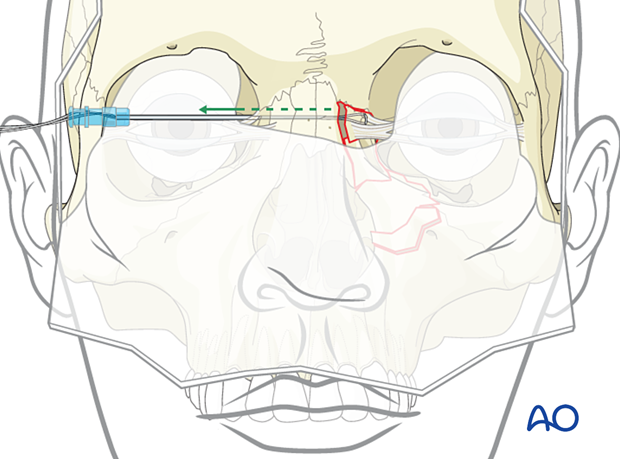
Alternative: using an awl
In this illustration, an awl has been placed through the contralateral side and then advanced to the side of the type II NOE fracture. The wire has been placed through the fragment attached to the medial canthus.
The two ends of the wire are then passed to the contralateral side using the awl.
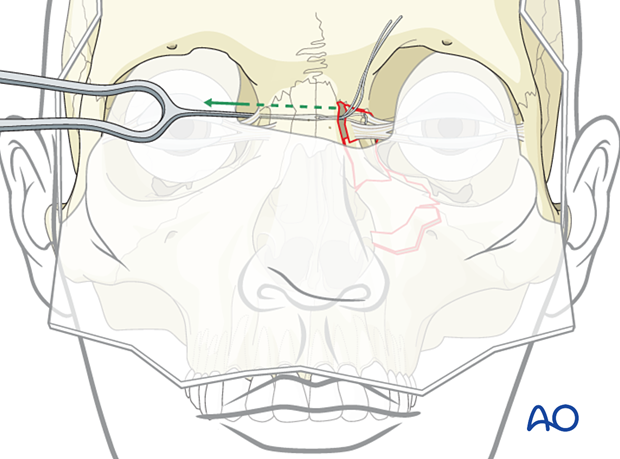
Rechecking medial canthal area
It is recommended that the surgeon perform a final check to confirm the correct position of the medial canthus.
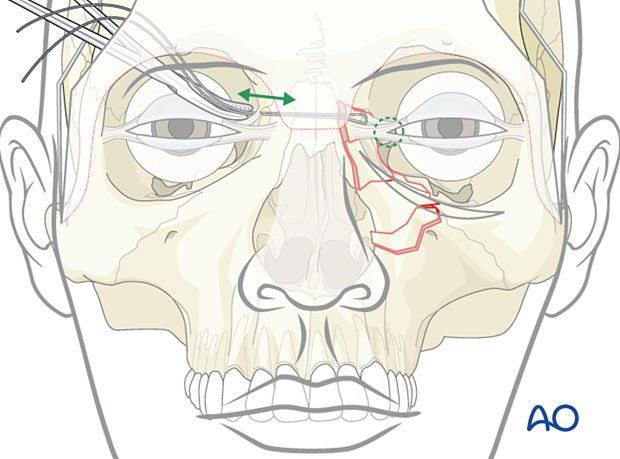
Video demonstrating how to check the correct position of the medial canthus.
Plate application
Fix the fracture by plate application as previously described.
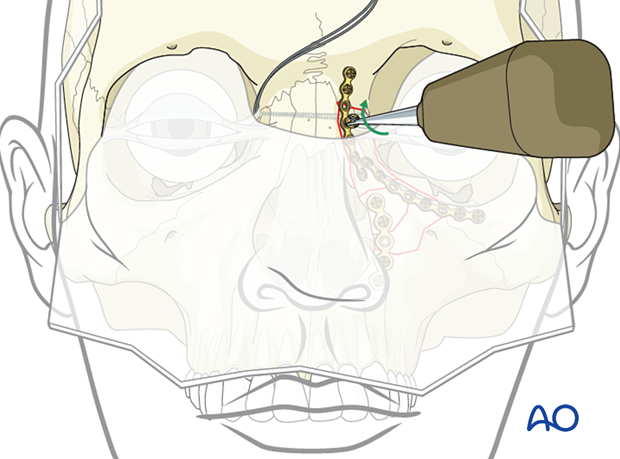
Securing transnasal wire
The transnasal wire is secured to a screw placed in the frontal bone on the contralateral side (see illustration) and tightened with the appropriate tension needed to secure the medial canthus in its proper position.
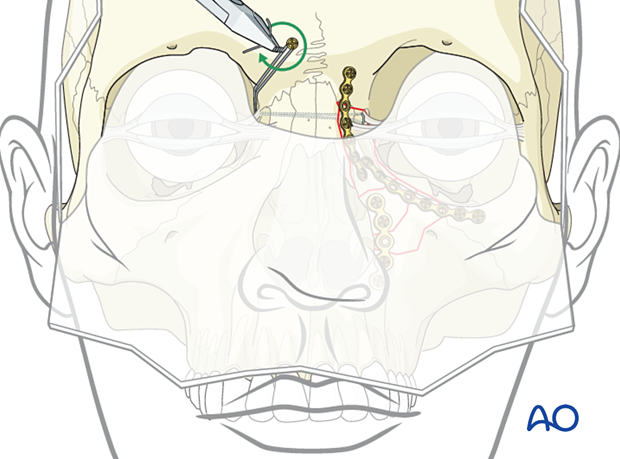
Proper position of transnasal wire
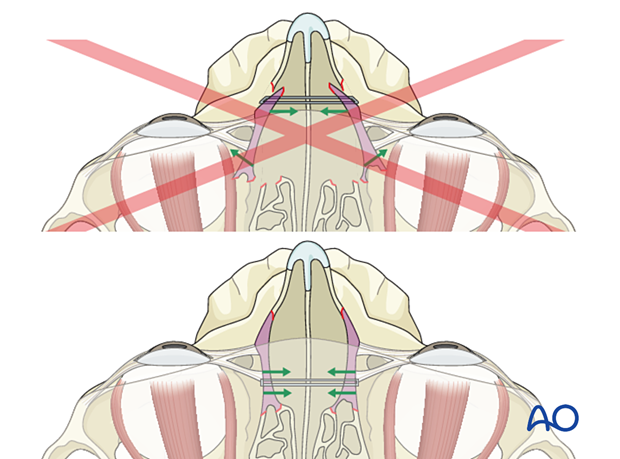
AP position of the transnasal wireNOE fractures often result in a lateral splaying of the medial canthi, resulting in telecanthus. The placement of a transnasal wire can usually correct this.
When confronted with an NOE fracture requiring a transnasal wire, it is important to place the wire fixation in its proper posterior position. The upper illustration represents a wire that has been placed too anteriorly, resulting in a further lateral splaying of the bone supporting the medial canthus and a worsening of the telecanthus.
The lower illustration represents the proper posterior placement of the transnasal wire with an adequate reduction of the bone attached to the medial canthus.
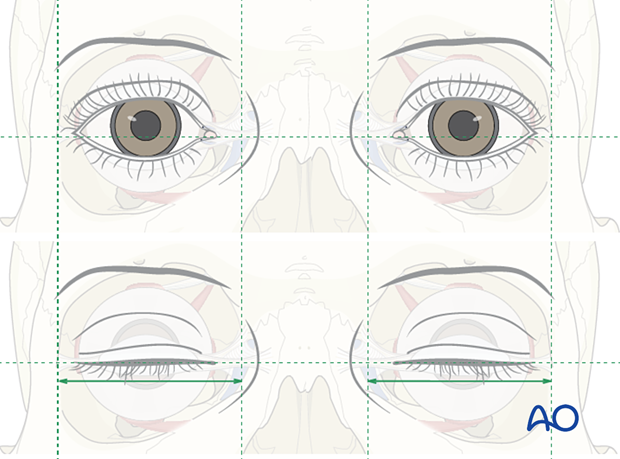
While the AP projection of the medial canthi is important, the horizontal position of the canthi is also critical.
With the eyelids closed and in a relaxed position, the lateral canthi should fall into a horizontal position with the medial canthi.
6. Soft tissues
A problem with NOE fractures is that even with a perfect bony reduction, there may be a lack of definition of the soft tissue in the medial canthal area. Many surgeons advocate placing external nasal splints at the end of the procedure to ensure close adaptation of the soft tissue to the underlying bone.
A soft tissue "bolster" pad is applied to the sides of the nose to recreate the correct angle of the soft tissue between the base of the nose and the medial cheek. Soft tissue bolsters are fixed with a wire passing through the bone to the contralateral side and tightened into place.
This technique becomes more relevant with increasing complexity of the NOE fracture. It is not usually necessary in type I NOE fractures. The more soft-tissue degloving of the nasal and medial maxilla, the more this technique is relevant to recreate the normal soft tissue draping in this region. It is most relevant for achieving the reduction and fixation of the fractured segments in type II and type III fractures where the soft tissue is totally stripped from the bone.
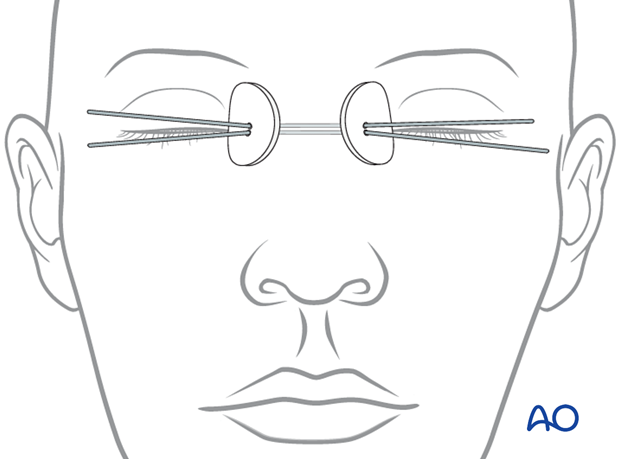
The percutaneous bolster dressing can be fixed in place with the use of transnasal wires or sutures.
The #28 full-length wires are passed through a 16-gauge spinal needle across the nasal bones. They are tightened into place to stabilize the bolster and maintain the coaptation of the soft tissue snugly onto the bone.
Due to the comminuted fractures the wires can be passed through drill holes or gaps between fracture segments.
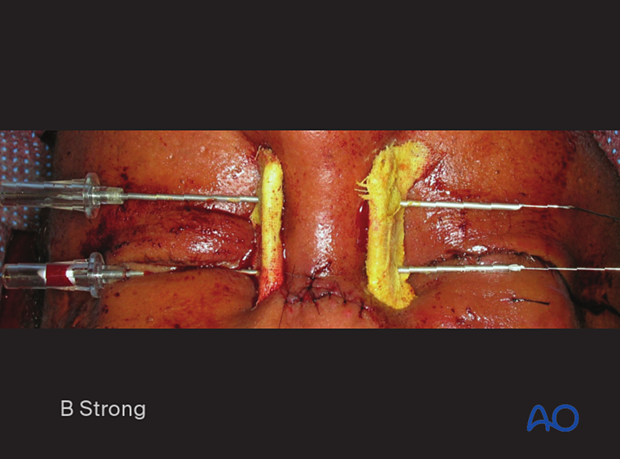
Clinical photograph showing a percutaneous bolster dressing.
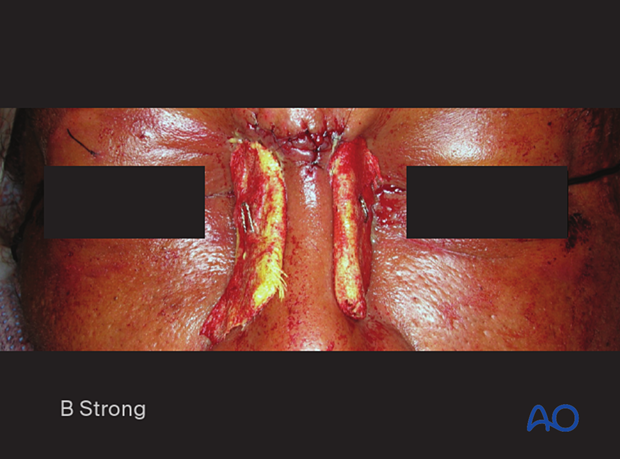
The bolsters consist of a half-thickness of orthopedic felt wrapped with Xeroform and stabilized by 2.0 mm thick Supramid plastic sheeting.
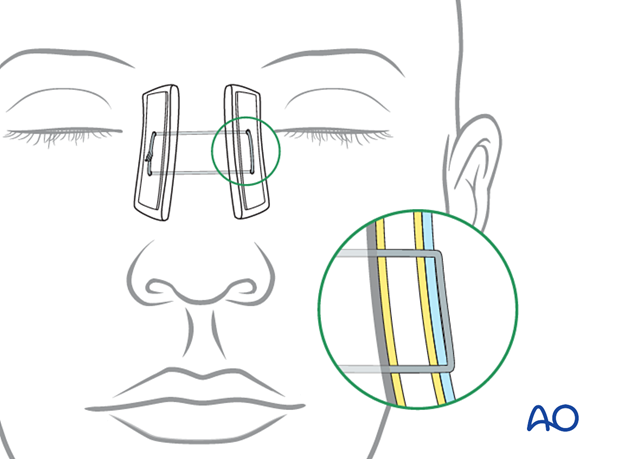
7. Aftercare
Evaluation of the patient’s vision
Patient vision is evaluated on awakening from anesthesia and then at regular intervals until hospital discharge.
A swinging flashlight test may serve to confirm pupillary response to light in the unconscious or non-cooperative patient; alternatively, an electrophysiological examination must be performed but this is dependent on the appropriate equipment (VEP).
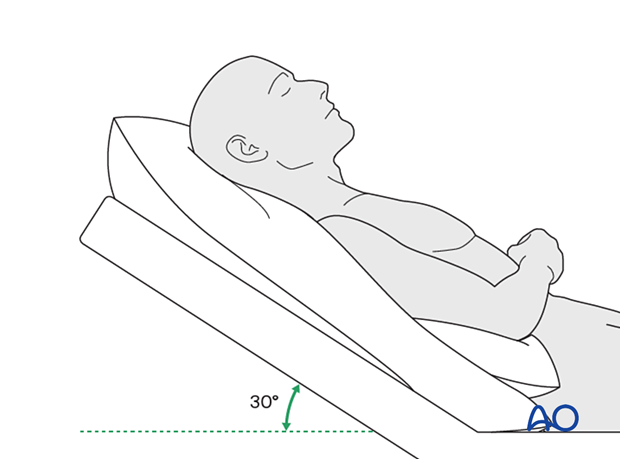
Postoperative positioning
Keeping the patient’s head in a raised position both preoperatively and postoperatively may significantly reduce edema and pain.
Nose blowing
Nose blowing should be avoided for at least 10 days following NOE fracture repair to prevent orbital emphysema.
Medication
The use of the following perioperative medication is controversial. There is little evidence to make solid recommendations for postoperative care.
- No aspirin for seven days (use of nonsteroidal anti-inflammatory drugs (NSAIDs)is controversial)
- Analgesia as necessary
- Antibiotics (Many surgeons use perioperative antibiotics.) There is no clear advantage of any antibiotic, and the recommended duration of treatment is debatable.
- A nasal decongestant may be helpful for symptomatic improvement in some patients.
- Steroids, in cases of severe orbital trauma, may help with postoperative edema. Some surgeons have noted increased complications with perioperative steroids.
- Ophthalmic ointment should follow local and approved protocol. This is not generally required in the case of periorbital edema. Some surgeons prefer it. Some ointments have been found to cause significant conjunctival irritation.
Ophthalmological examination
Postoperative examination by an ophthalmologist may be requested. The following signs and symptoms are usually evaluated:
- Vision
- Extraocular motion (motility)
- Diplopia
- Globe position
- Visual field test
- Lid position
- If the patient complains of epiphora (tear overflow), the lacrimal duct must be checked
- If the patient complains of eye pain, evaluate for corneal abrasion
Postoperative imaging
Postoperative imaging must be performed during the first days after surgery. 3D imaging (CT, cone beam) is recommended to assess complex fracture reductions. An exception may be made for centers capable of intraoperative imaging.
Wound care
Remove sutures from the skin after approximately five days if non-resorbable sutures have been used.
Medial canthal bolster dressings should be kept in place for a minimum of 2–4 weeks to allow proper skin redraping. If bolsters are utilized, one must clean under the bolster daily with peroxide on cotton-tip applicators and a small amount of antibiotic ointment may be applied underneath. The tension on the bolster is frequently adjusted in the early postoperative period to avoid excess pressure on the skin creating ischemia. Ice compresses may be applied to the eyelids to provide comfort, slight anesthesia, and to minimize swelling.
Avoid sun exposure and tanning to skin incisions or periorbital bruising for several months to prevent hyperpigmentation.
Diet
Diet depends on the fracture pattern and the patient’s condition, but there are usually no limitations.
Clinical follow-up
Clinical follow-up depends on the complexity of the surgery and whether the patient has any postoperative problems.In all patients with NOE trauma, all the following should be periodically assessed:
- Globe position
- Double vision
- Other vision problems
- Nasal airway status
Other issues to consider are:
- Facial deformity (including asymmetry and pseudo-telecanthus)
- Sensory nerve compromise
- Problems of scar formation
- Anosmia
- Epiphora and dacryocystitis
Implant removal
Generally, implant removal is not necessary except in the event of infection or exposure.
Special considerations
Travel in pressurized aircraft is permitted 4–6 weeks postoperatively. Mild pain on descent may be noticed. However, flying in a non-pressurized plane should be avoided for a minimum of 6 weeks.
No scuba diving should be permitted for at least 12 weeks. Additionally, the patient should be warned of potential long-term risks.













