Open reduction
1. General considerations
Bleeding
Nasal fractures can cause significant bleeding. Proper techniques for hemostasis should be applied before any diagnostic procedure and any definitive treatment of nasal fractures.
Read more about hemostasis here.
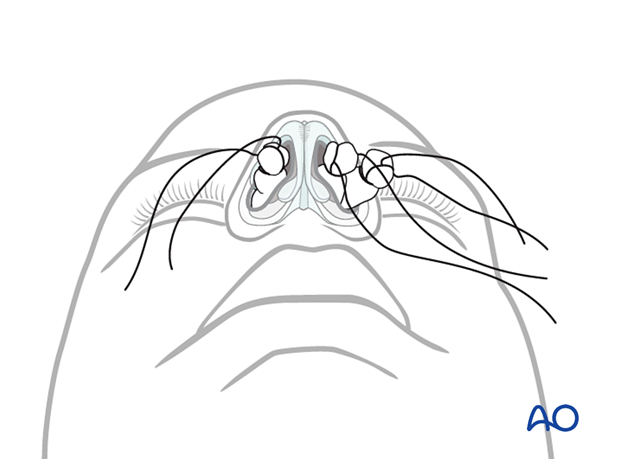
Choice of anesthesia
Open reduction is generally performed under general anesthesia.
2. Choice of approach
In case of severely comminuted or open fractures, existing lacerations can be used. When associated with other facial fractures (eg, NOE, frontal sinus), the coronal approach can be used. Otherwise, depending on the surgeon’s preference and the particular case, an external rhinoplasty or an endonasal approach may be used.
3. Open reduction
Reduction of the nasal bone
The blades of an instrument (eg, Lempert rongeur) are inserted on each side of the depressed nasal bone and used to mobilize and reduce the bone to its correct position.
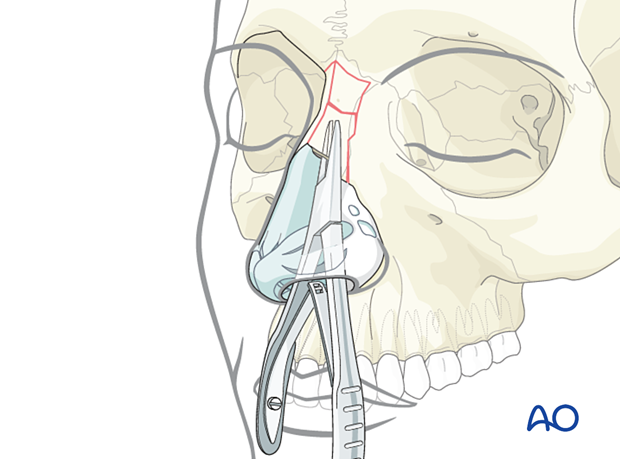
Reduction of cartilages
The cartilaginous segments are exposed and reduced. Sometimes, segments of cartilage must be resected. If needed, a vomer osteotomy is performed to allow the septum to go back into its normal position.
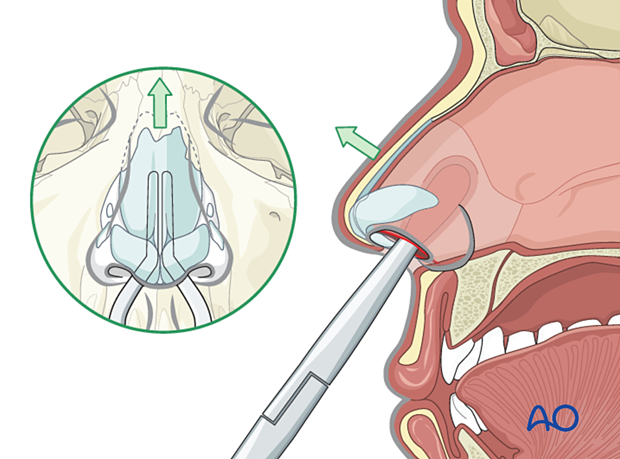
Midline repositioning of quadrangular cartilage of the septum and the vomer
The septum is repositioned in its original midline position together with the quadrangular cartilage and vomer. A small suture may be placed from the anterior nasal spine to the anterior portion of the septum to maintain its reduction.
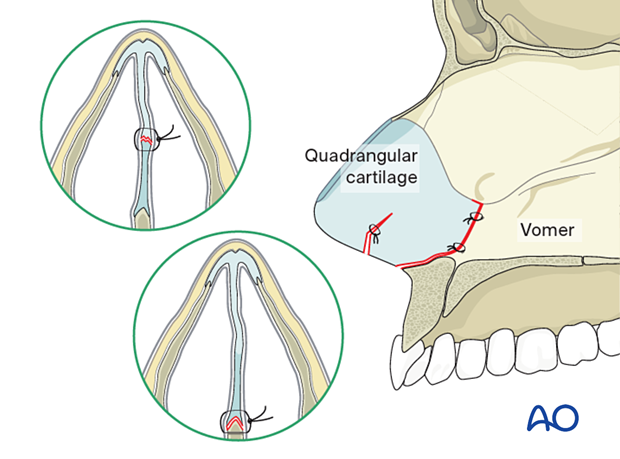
Comminuted fractures
Severely comminuted fractures should not be treated via an open approach. In this case, the fractures are addressed via closed reduction, and residual deformities are treated in a secondary procedure.
Overaggressive stripping of the periosteum may cause devitalization of the bone with subsequent necrosis/resorption. The use of miniplates or wires in comminuted fractures is not recommended because extrusion of the plate, wound dehiscence, and unsightly appearance of the dorsal nasal skin over the plates or wires may occur.
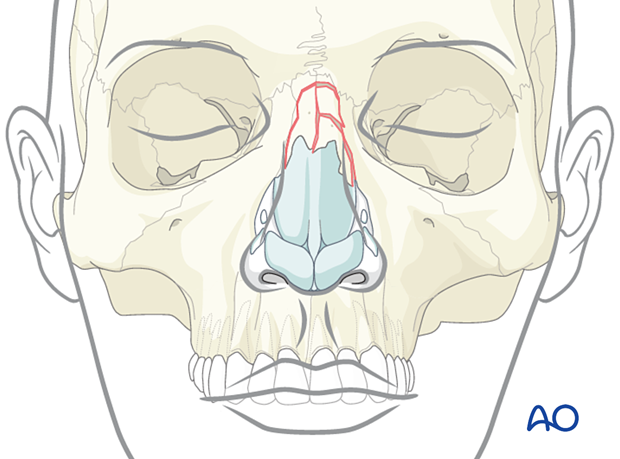
Associated fractures
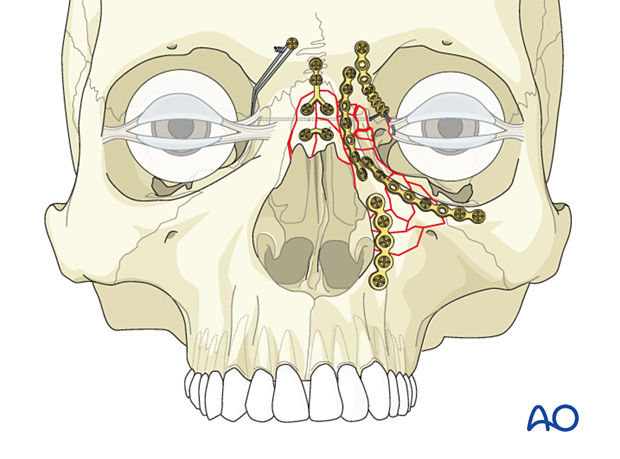
In the case of associated NOE, frontal sinus, Le Fort II, or Le Fort III fractures, the use of microplates may be necessary to fix nasal bones and the frontal process of the maxilla.
Great care should be taken when considering placing plates anterior to the medial canthal ligament, as these may be visible through the thin overlying skin.
Grafting
Bone or cartilage grafting may be necessary for severely comminuted nasal bone fractures. When inserting the graft, the following points should be respected:
- The nasofrontal angle should be reconstructed in a normal relationship (105–120°)
- The collapsed septum should be suspended to the graft using nonresorbable sutures
- The graft should be long enough to resuspend the lower lateral cartilages
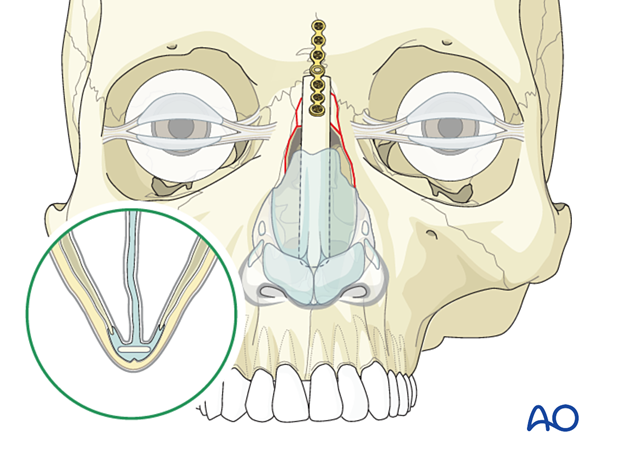
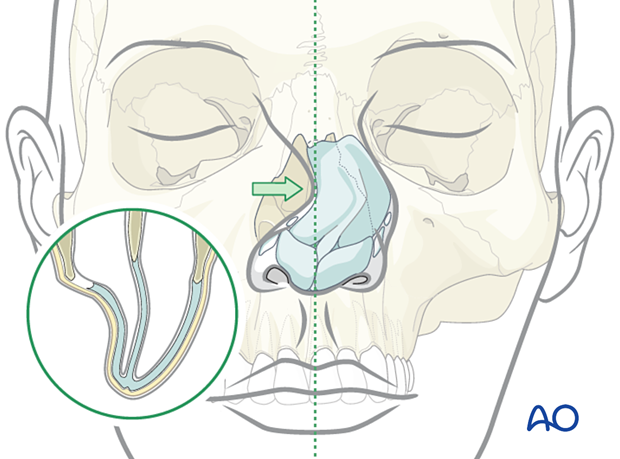
Disarticulation of upper lateral cartilage
Treatment of disarticulation of the upper lateral cartilage is via lacerations or open approaches and is aimed at suturing the cartilages back to the nasal bone. Long term outcome is usually poor and often requires secondary procedures to correct the deformities.
Internal packing of the nose to support the upper lateral cartilage should be performed to reestablish the preinjury relationship between the nasal bone and the upper lateral cartilage.
4. Splinting
Nasal bones
After reduction, adhesive strips are placed over the skin of the nasal dorsum, and the nasal bones are splinted using an external splint that conforms to the patient’s nose. If the nasal bones are comminuted or loose, they should be supported with intranasal packing, which should be placed before placing the external splint.
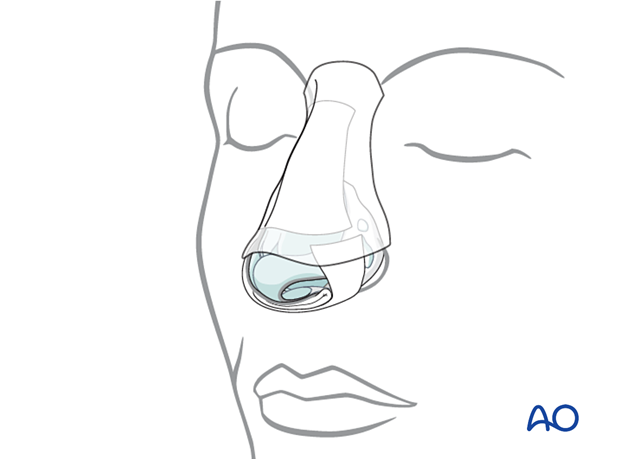
Nasal septum: Doyle splint
The nasal septum can be stabilized with splints (Doyle) or packs.
Doyle splints are made from silicone and are placed on either side of the septum, secured by one or more sutures. They are designed to prevent the formation of a septal hematoma, splint septal cartilage, and maintain an open airway.
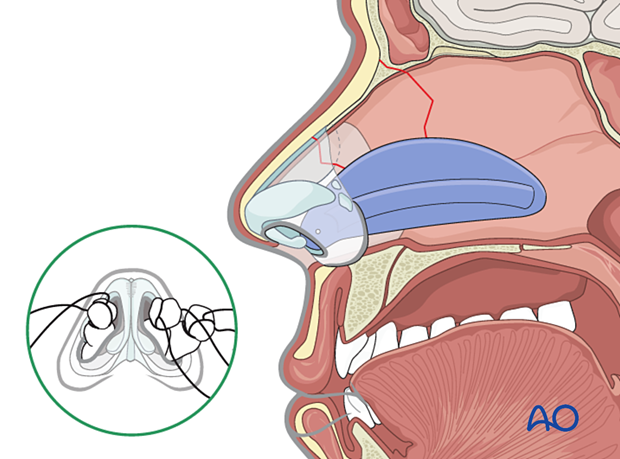
Removal of packing and splints
Packing used for control of acute bleeding can be removed after 24 hours.
Any packing supporting the nasal bones must be left in place for 5–7 days and for as long as the external splint is in place.
The patient should be prescribed antibiotic treatment for as long as the nasal packing is in place to avoid toxic shock syndrome.
5. Aftercare
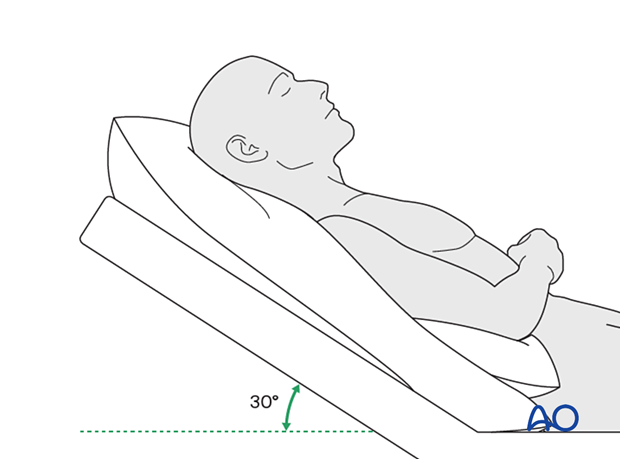
Postoperative positioning
Keeping the patient’s head in a raised position both preoperatively and postoperatively may significantly reduce edema and pain.
Nose blowing
Nose blowing should be avoided for at least ten days following fracture repair to prevent orbital emphysema.
Medication
The use of the following perioperative medication is controversial. There is little evidence to make strong recommendations for postoperative care.
- No aspirin for seven days (nonsteroidal anti-inflammatory drugs (NSAIDs) use is controversial)
- Analgesia as necessary
- Antibiotics (many surgeons use perioperative antibiotics. There is no clear advantage of any antibiotic, and the recommended duration of treatment is debatable.)
- A nasal decongestant may be helpful for symptomatic improvement in some patients.
- Steroids, in cases of severe orbital trauma, may help with postoperative edema. Some surgeons have noted increased complications with perioperative steroids.
Postoperative imaging
For nasal fractures, postoperative CT imaging is usually not necessary except in severely comminuted fractures.
Wound care
Remove sutures from the skin after approximately five days if non-resorbable sutures have been used.
Ice packs are effective in the short term to minimize edema.
Avoid sun exposure and tanning to skin incisions for several months.
Diet
Diet depends on the fracture pattern and the patient’s condition, but there are usually no limitations.
Clinical follow-up
Clinical follow-up depends on the complexity of the surgery and the patient’s postoperative course.
In all patients with nasal bone trauma, all the following should be periodically assessed:
- Nasal airway status
- Excess compression from the splint or intranasal material
- External nasal deformity
Other issues to consider are:
- Facial deformity (including asymmetry)
- Sensory nerve compromise
- Problems of scar formation
- Anosmia
- Epiphora and dacryocystitis













