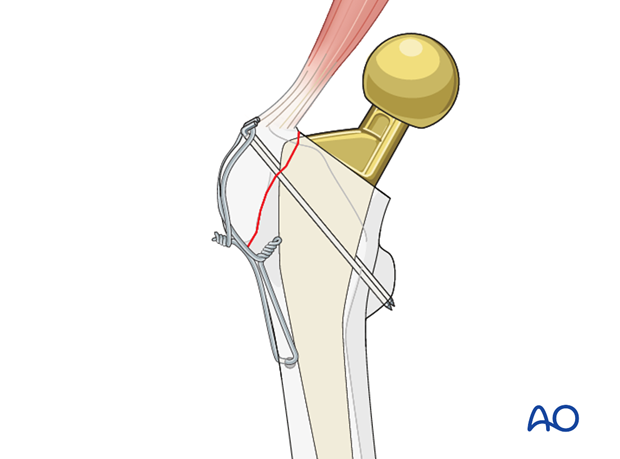
Tension band wiring
1. Principles
In the setting of a stable femoral prosthesis, the goals include pain control, fracture healing, restoration of abductor mechanism, and maintaining a stable hip prosthesis.
Large fractures of the greater trochanter may compromise the abductor function. A tension band construct may adequately restore the abductor mechanism.
2. Approach
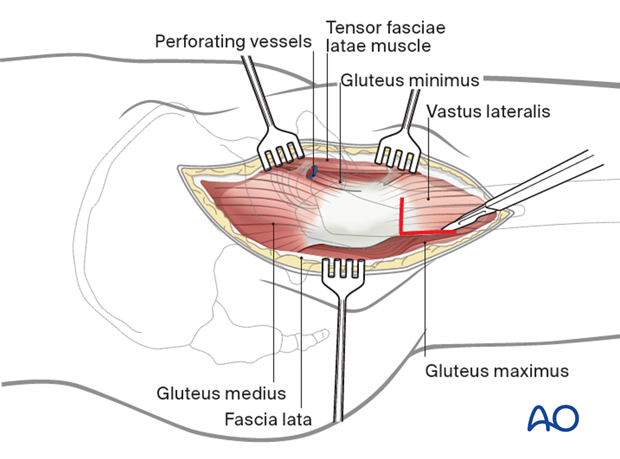
Direct lateral approach extension
Direct lateral approach to the femoral diaphysis is typically utilized. This will require an extension to the proximal femur. Depending on the location of the greater trochanteric fracture, the vastus lateralis origin may need to be released and repaired after stabilization.
Other approaches
Other approaches that can be used to perform this procedure are:
- Anterolateral approach
- Direct anterior approach
- Iliofemoral (Smith-Petersen) approach
- Posterolateral approach
- Trochanteric osteotomy
These approaches can be performed with the patient in a lateral or supine position.
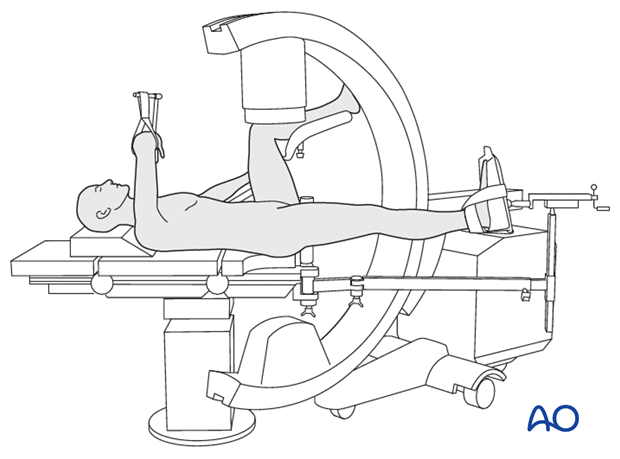
Option: use of a radiolucent or fracture specific table
Option: A radiolucent table or a fracture specific table may be used.
An isolated greater trochanteric fracture can be reduced and stabilized in either the supine or lateral position on either table.
3. Reduction
Reduction is typically carried out using a combination of direct and indirect methods. Limb abduction will help in an indirect manner. Direct reduction with clearance of fracture hematoma and stabilization with pointed bone reduction clamps can then be completed.
The Collinear reduction clamp can be extremely helpful in facilitating reduction. It is applied from the direct lateral incision with proximal extension.
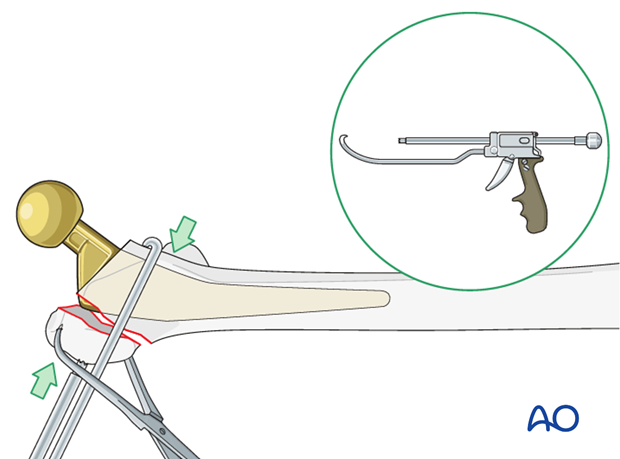
4. Fixation
K-wires insertion
2.0 mm K-wires are drilled from the greater trochanteric piece to the intact lesser trochanter.
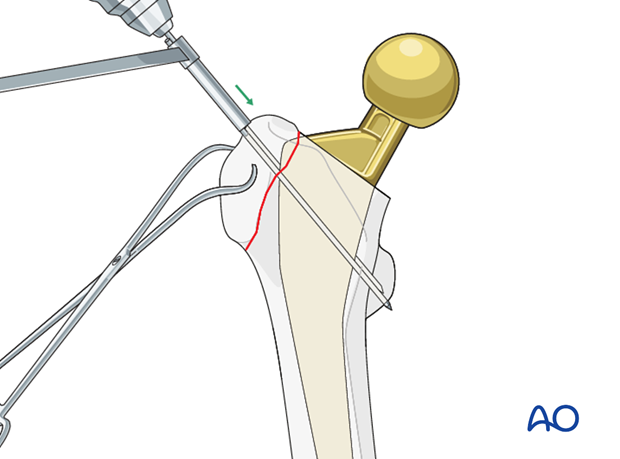
Wire positioning
A hole is created in the lateral cortex of the femur, from anterior to posterior in the intact diaphysis.
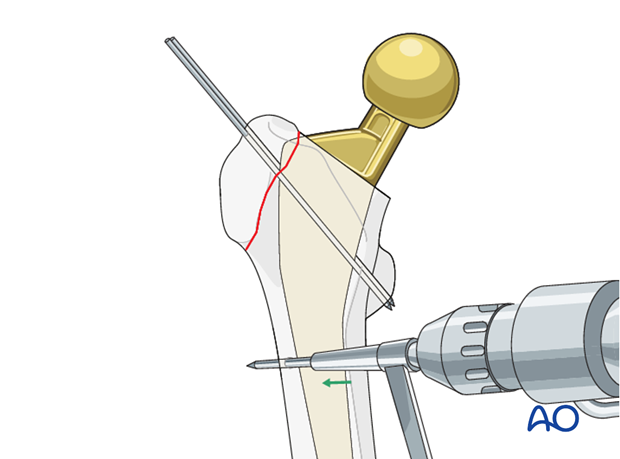
18 gauge wire is passed through the hole and brought proximally in a figure of eight fashion around the origin of the K-wires.
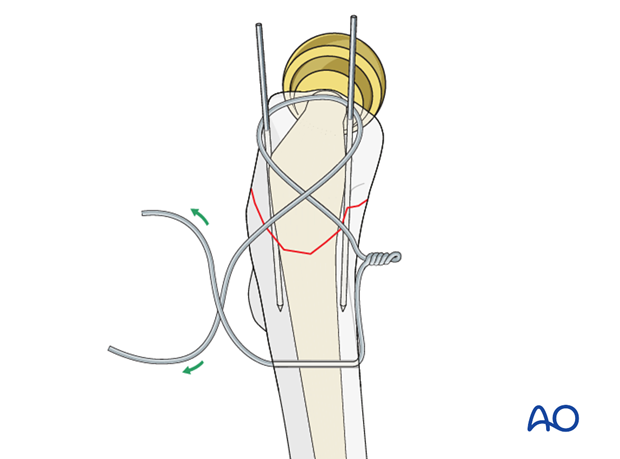
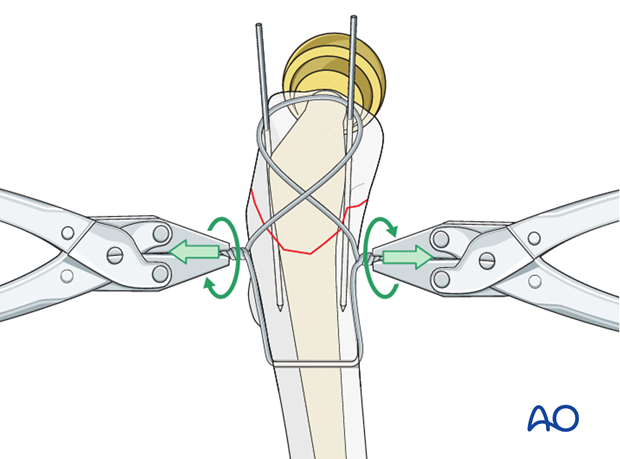
Wire tensioning
The wire is tensioned on either side of the figure of eight in a helical manner for a minimum of four rotations.
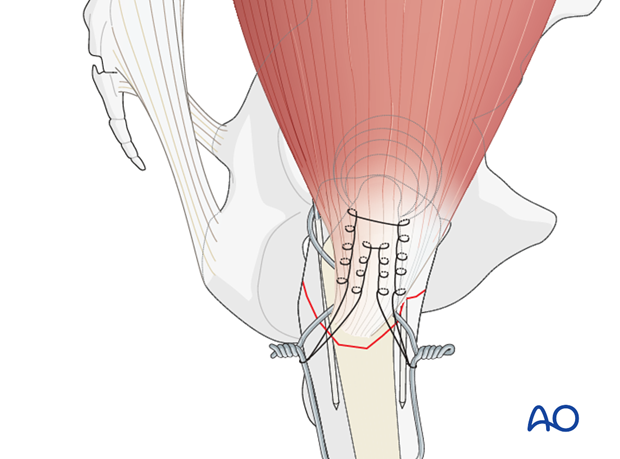
Stitches can be used to augment a tension band construct.
Stitches are sutured in a Krackow fashion on the top of the gluteus medius tendon, and secured under the loop of the wire.
Radiographic verification
Antero-posterior and medio-lateral radiographs of both the fracture sites and the arthroplasty are obtained at the end of the procedure, to ensure that:
- There is no displacement
- The joint articulation is preserved
- There is no dislocation, that may be caused by excessive distraction of the limb or a malreduction of the femur
5. Aftercare following ORIF
Postoperative management
Postoperative management should include careful monitoring of hematocrit and electrolytes particularly in the elderly patients.
Postoperative IV antibiotics should be administered up to 24 hours.
Consideration should be given to anticoagulation for a minimal course of 35 days. If there are thromboembolic complication this treatment is extended.
Drains can be discontinued when output is less than 30 to 50 cc per 12 hours.
Patient mobilization
Immediate mobilization of the patient should commence. If fracture stability will allow, the patient should be made weight bearing as tolerated as soon as possible. Long periods of limited weight bearing are extremely detrimental to patient recovery.
Activity limitations following greater trochanteric fracture treatment
If a greater trochanteric fracture has been treated, the patient should not be allowed to perform active abduction exercises until at least 6 weeks postoperatively. An abduction brace may be considered.
Traditionally, extended periods of limited weight bearing were utilized, however increasing stability of the fracture should be a priority to facilitate mobilization.
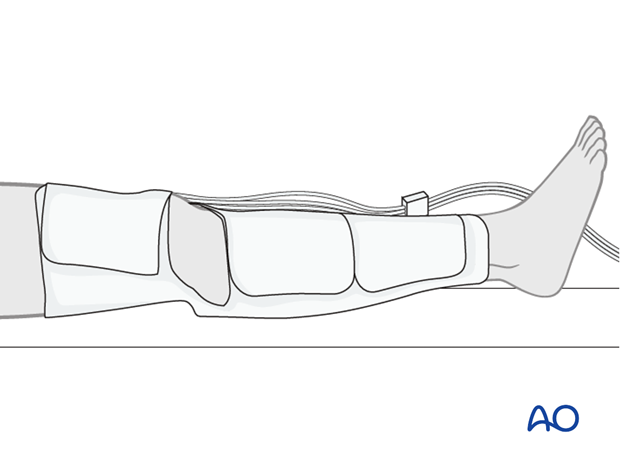
Wound healing
Avoidance of edema postoperatively is critical for both wound healing and patient mobilization. This can be aided by pneumatic compression devices. If negative pressure wound therapy is utilized, it can be discontinued after 5 to 7 days. Staples or sutures are typically removed at 14 to 21 days.