In situ fixation with K-wires or screws
1. Preliminary remarks
Avascular necrosis
Complete, unstable proximal femoral fractures carry a significant risk of avascular necrosis (AVN) of the femoral head. AVN can result from entrapping or rupturing the retinacular vessels during a closed reduction maneuver.
Decompression of hemarthrosis may reduce the risk of AVN. Detailed knowledge of the vascular supply of the femoral head is a prerequisite for safe treatment and the management of femoral neck fractures in children ideally requires experience in hip surgery.
If reduction is not required, in situ stable fixation may be applied.
Note: Care must be taken to rule out slipped capital femoral epiphysis (SCFE). Fractures can be distinguished from SCFE by a detailed history supplemented by appropriate x-ray examination and assessment; in unclear situations, an MRI is indicated.
Hardware selection
6.5, 7.0, or 7.3 mm cannulated screws are used for adolescents.
4.0, or 4.5 mm cannulated screws may be selected for younger children. Be aware that these screws are considerably weaker and prone to breakage if used in too heavy a child.
If cannulated screws are not available, modification of this technique allows standard screws to be inserted.
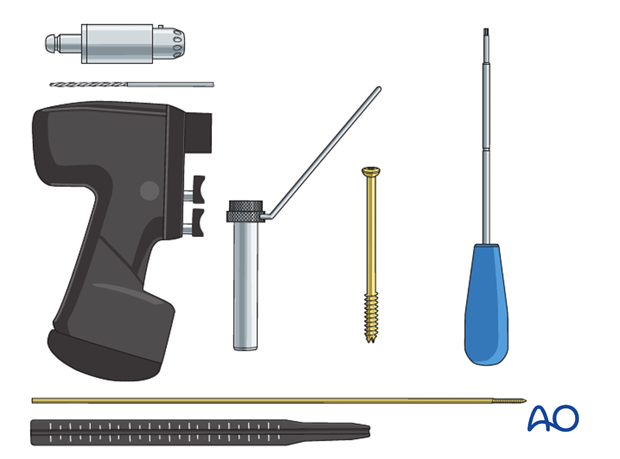
If the child is too small for screw fixation, 2.0, 2.5, or 3.0 mm K-wires can be selected depending on the size of the child.
Larger K-wire diameters are preferred for stability. Threaded K-wires also increase stability.
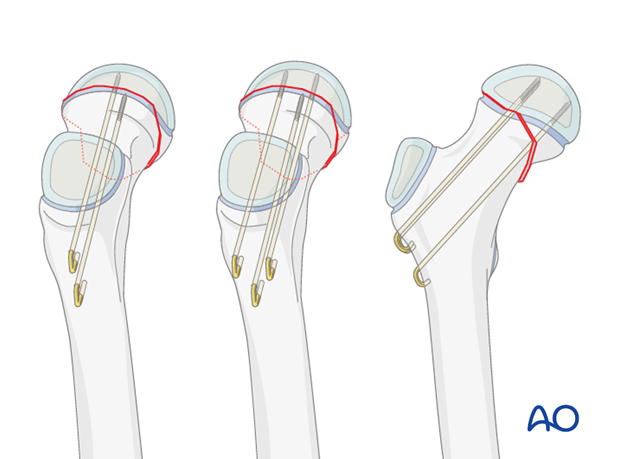
Implant insertion
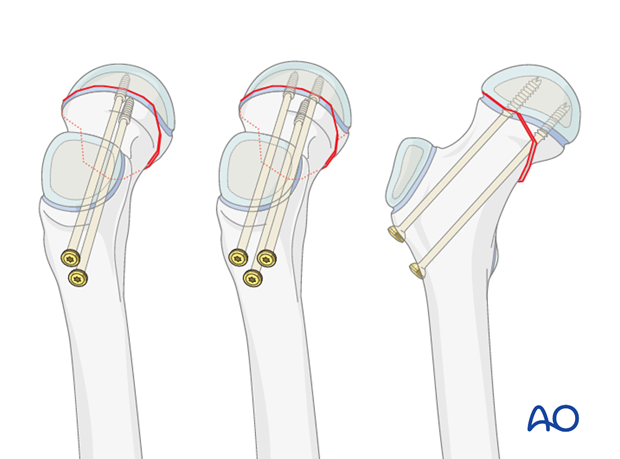
Typically, two screws (or K-wires) separated vertically are inserted. This configuration may be more suitable in smaller bones.
An alternative is three screws (or K-wires) used in an apex-distal, triangular configuration, with the lower central screw (or K-wire) abutting the calcar.
Inserting a single central screw (or K-wire) does not provide rotational stability and is, therefore, less applicable for fractures, even though it is a common choice for SCFE.
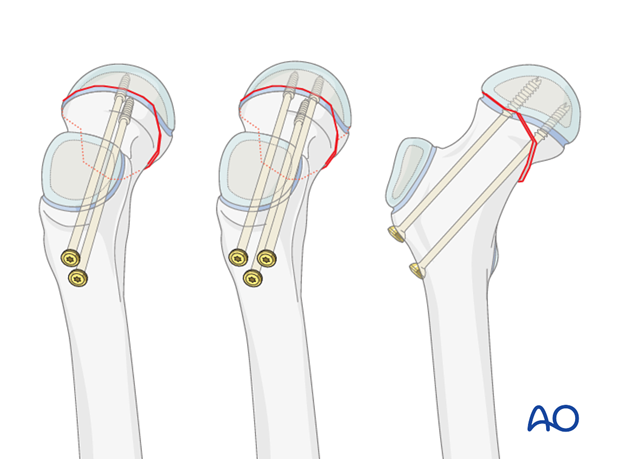
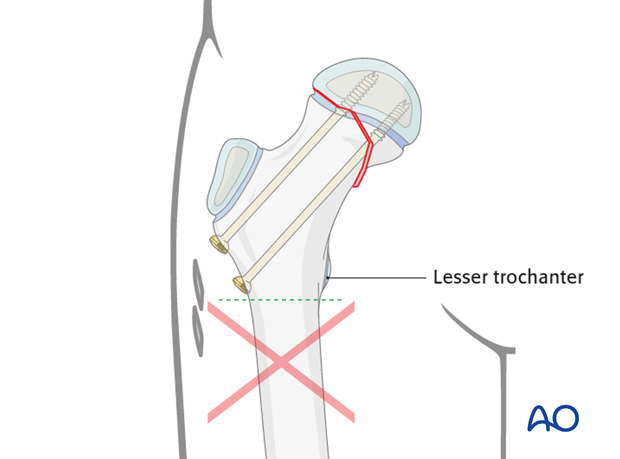
Pitfall: Secondary subtrochanteric fractures may occur if screws are inserted with an entry point distal to the level of the lesser trochanter.
2. Approach and positioning
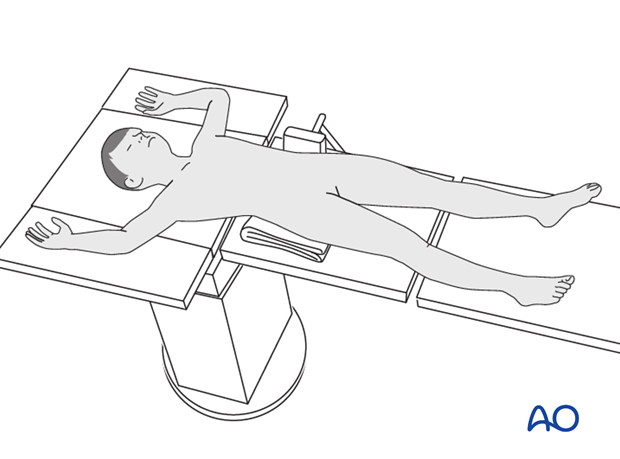
In situ fixation is performed either through stab incisions or a single short incision. The patient may be supine on a fracture table, or on a radiolucent table.
3. Fixation
Guide wire insertion
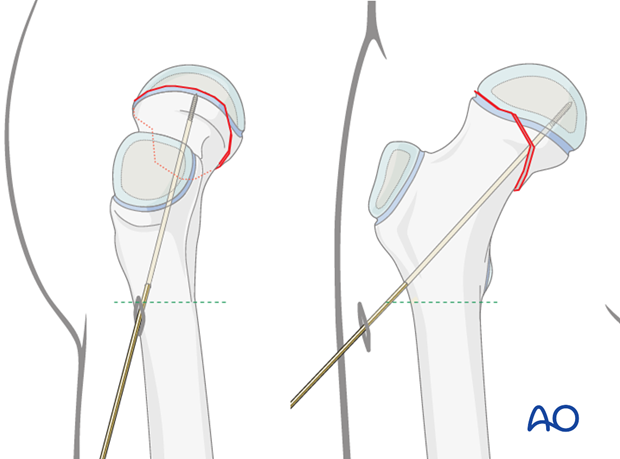
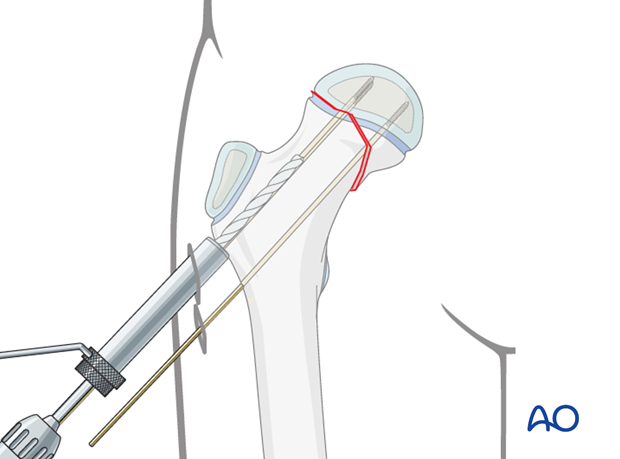
Under image intensification, the first guide wire is inserted via the lateral cortex above the level of the lesser trochanter, to pass just above the calcar and into the center of the inferior half of the femoral head epiphysis.
A wire can be placed along the anterior surface of the femoral neck as an indication of the anteversion.
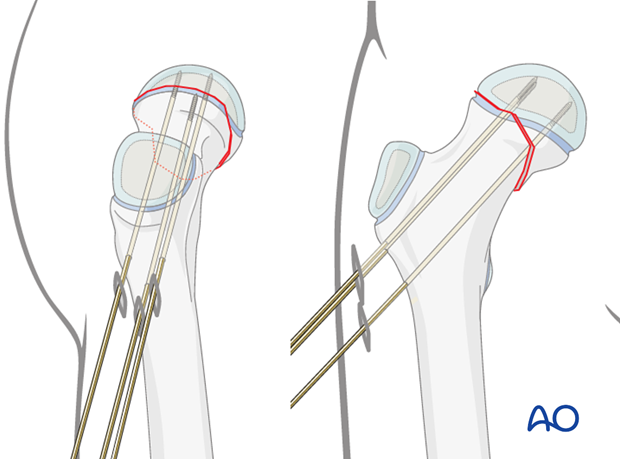
Additional wires are inserted under image intensification according to the two- or three-screw configuration chosen.
X-ray control
The wire positions are confirmed on AP and lateral x-ray images, using image intensification.
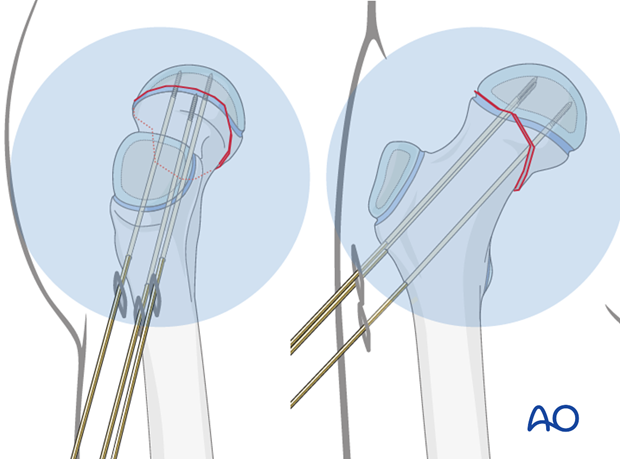
If using a standard radiolucent table, the K-wire fixation is generally stable enough to allow positioning for a “frog” lateral view.
K-wires are repositioned as necessary.

Images at multiple angles are used to confirm that the K-wires do not penetrate into the hip joint.
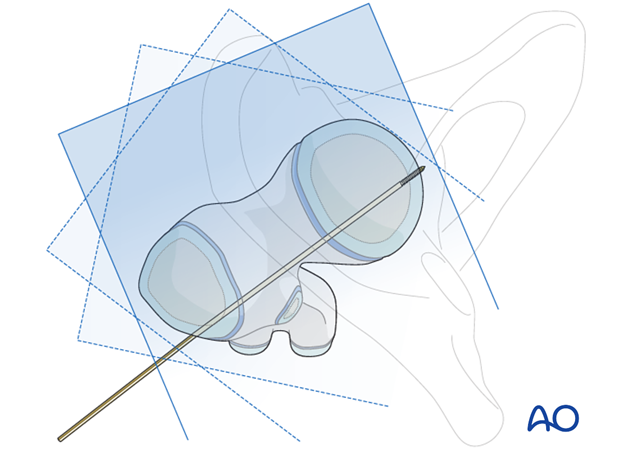
4. K-wire fixation alone
If K-wire fixation alone is used, the K-wires are cut and bent leaving them deep to the fascia lata.
Capsular decompression should be considered.

5. Screw fixation
Enlarging stab incisions
The stab incisions are enlarged to allow for screw insertion. The incision is deepened down to bone by spreading the tissues with an artery forceps or blunt scissors.
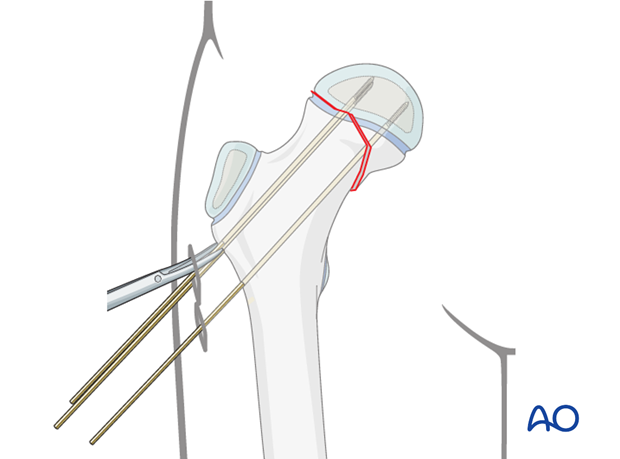
Measuring screw length
A depth gauge is used to measure screw length.
If a dedicated cannula/depth gauge set is not available, then a K-wire, of the same length as that inserted, is placed onto the lateral cortex adjacent to the inserted wire, and the difference measured to determine the screw length.
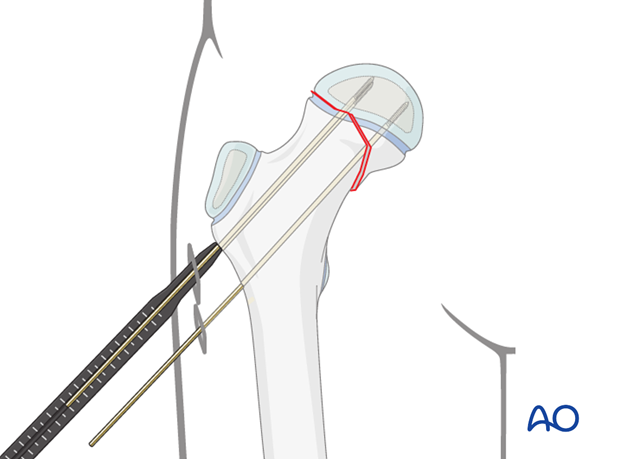
Drilling screw holes
The K-wires are overdrilled, through a soft tissue protector, with an appropriate sized cannulated drill bit.
Intermittent screening with an image intensifier is recommended to ensure that the guidewire does not penetrate into the hip joint as the drill advances.
Adolescents in particular have very dense, strong bone in the metaphysis near the growth plate and predrilling is recommended.
If cannulated screws are not available, then guide wires should be removed one at a time and an appropriate drill used.
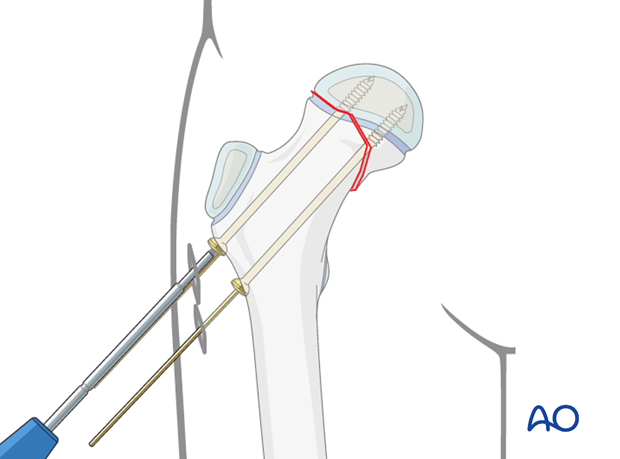
Screw insertion
Two, or three, cannulated screws are then inserted over the K-wires.
Note: Fully threaded cannulated screws are easier to remove later.
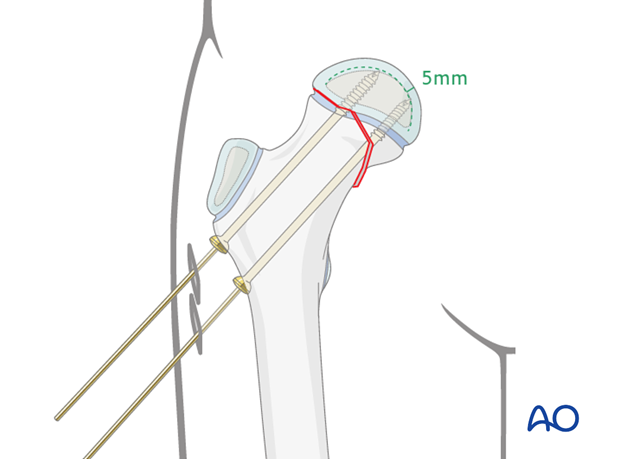
X-ray control
Image intensification is used to confirm that the screw tip does not penetrate into the joint. Typically, 5 mm of epiphyseal bone/cartilage should remain between the screw tip and joint surface. Three, or four, threads lying within the epiphysis provides adequate fixation.
Pitfall: Screw penetration can occur, especially with eccentrically placed screws, even if not apparent on AP or lateral x-rays.
Dynamic, real-time image intensification, with a full range of internal and external rotation at different degrees of flexion, is useful to see how close the screw-tip is to the joint surface of the head.
Observing an approach/withdrawal of the screw tip helps in judging its position. Some surgeons supplement this examination with 3-D image intensification for confirmation.
Arthrography is useful to confirm correct wire and screw placement in the younger patient.
Guide wire removal
The guide wires are removed, once the full complement of screws has been shown to be ideally positioned.
Capsular decompression should be considered.
6. Hip spica
If solid fixation has been obtained with screws, and the patient/family can reliably comply with toe-touch weight bearing, then a cast is not necessary.
For patients below 5 years of age, a hip spica cast can be used if desired.
Click here for details of hip spica application.
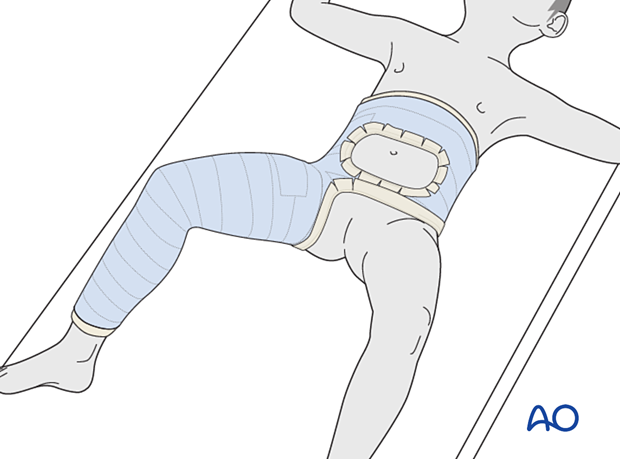
Aftercare following hip spica application
After application, the spica should be trimmed to allow adequate space for bodily functions. The edges of the spica should be padded and waterproofed.
Generally, a hip spica should allow space for a small diaper inside the plaster and a large one outside the plaster. The diapers should be positioned to prevent soiling of the spica.
The spica is not waterproof. Bathing and showering should not be attempted. Hair washing should be done very carefully.
No skin products should be put inside the spica. Only skin that can be seen should be moisturized.
7. Aftercare
Introduction
After surgical stabilization, the construct should be sufficiently robust to allow protected weight bearing. Smaller children may not be able to comply with this and may need immobilization.

Infection
See the additional material on postoperative infection.
Mechanics
Forces through the hip are less with toe-touch weight bearing than with non-weight bearing. Therefore, toe-touch is normally recommended for initial mobilization. This needs to be taught to children by a physiotherapist.
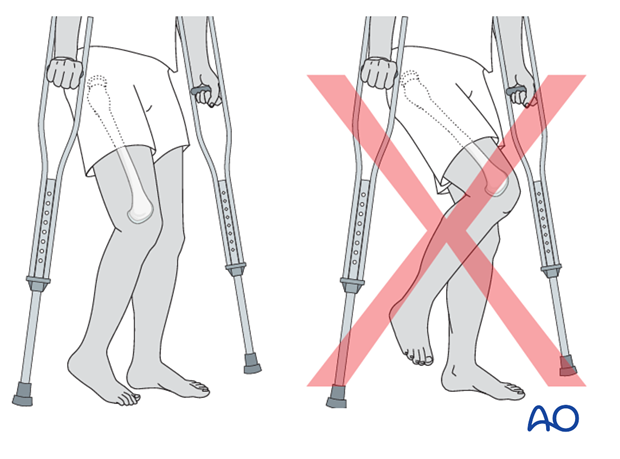
Range of movement
Range-of-movement exercises should start in the immediate postoperative period to prevent stiffness. Surgeons should indicate if any extremes of movement are forbidden.
Weight bearing
Having started with toe-touch weight bearing, children progress to partial weight bearing and then to full weight bearing according to their age and the predicted rate of healing of their fracture.
Even older adolescents should be fully weight bearing without aids at three months.
Sports
Swimming can be allowed as soon as partial weight bearing is permitted.
Contact sports should be avoided for at least six months.
Follow-up x-rays
X-rays are generally taken immediately after the surgery and at 6 and 12 weeks.
Implant removal
Implants that cross the physis should be removed if there is significant growth remaining. The fracture should be healed and consolidated prior to removal (see Healing times).
Implants in young children should always be removed to prevent them from being covered by bony overgrowth.
Implant removal is not compulsory in adolescents.













