Angular stable plating
1. Principles
Angle stable fixation has evolved from a technique using self-drilling, self-tapping unicortical screws. The original concept largely centred on using the implant as an internal fixator, often intended as being placed using minimally invasive insertion and associated with indirect reduction methods.
Currently, numerous angle stable fixation devices demonstrate improved periarticular design, the ability to use combinations of both cortical and variable-angled locking screws, and placement can be done using open or minimally invasive/percutaneous methods. These features allow the plate to be used as a reduction tool helping to achieve metadiaphyseal alignment, facilitating buttressing of meta-epiphyseal fracture fragments, while still allowing angular stability to provide enhanced stability and fracture bridging when needed or desired.
Stability created by conventional plating requires friction between the surface of the bone and the plate. This requires conventional screws to create tension along the screw axis. The more the screw can be tightened, the greater the axial tension in the screw, and the greater the friction created between the plate and bone. In osteoporotic bone, where the screw cannot create enough axial tension, the friction of the plate to the bone is decreased and screws loosen easily, jeopardizing stability between the plate and the bone.
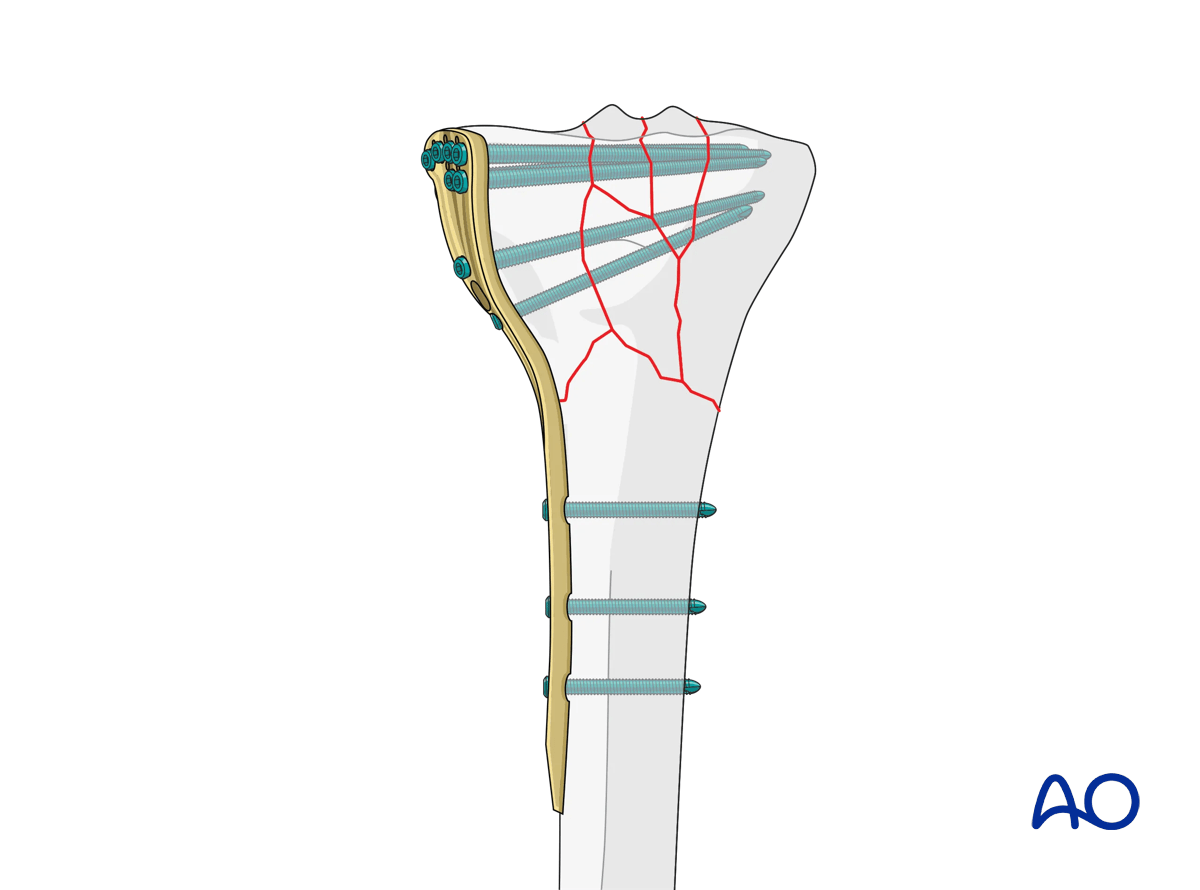
In contrast to conventional plates, displacement of fracture fragments with locked screw plate devices requires a large swath of bone to be destroyed to allow fragments to displace, or for there to be catastrophic failure of most or all the locking screws in a segment happening simultaneously. Therefore, the best indications for angle-stable plating are in situations with poor quality bone, for any reason, or those situations where inherent fracture stability is non-existent, or cannot be achieved (bone loss, segmental comminution), and situations with prolonged anticipated time to union where prolonged and secure stability is required.
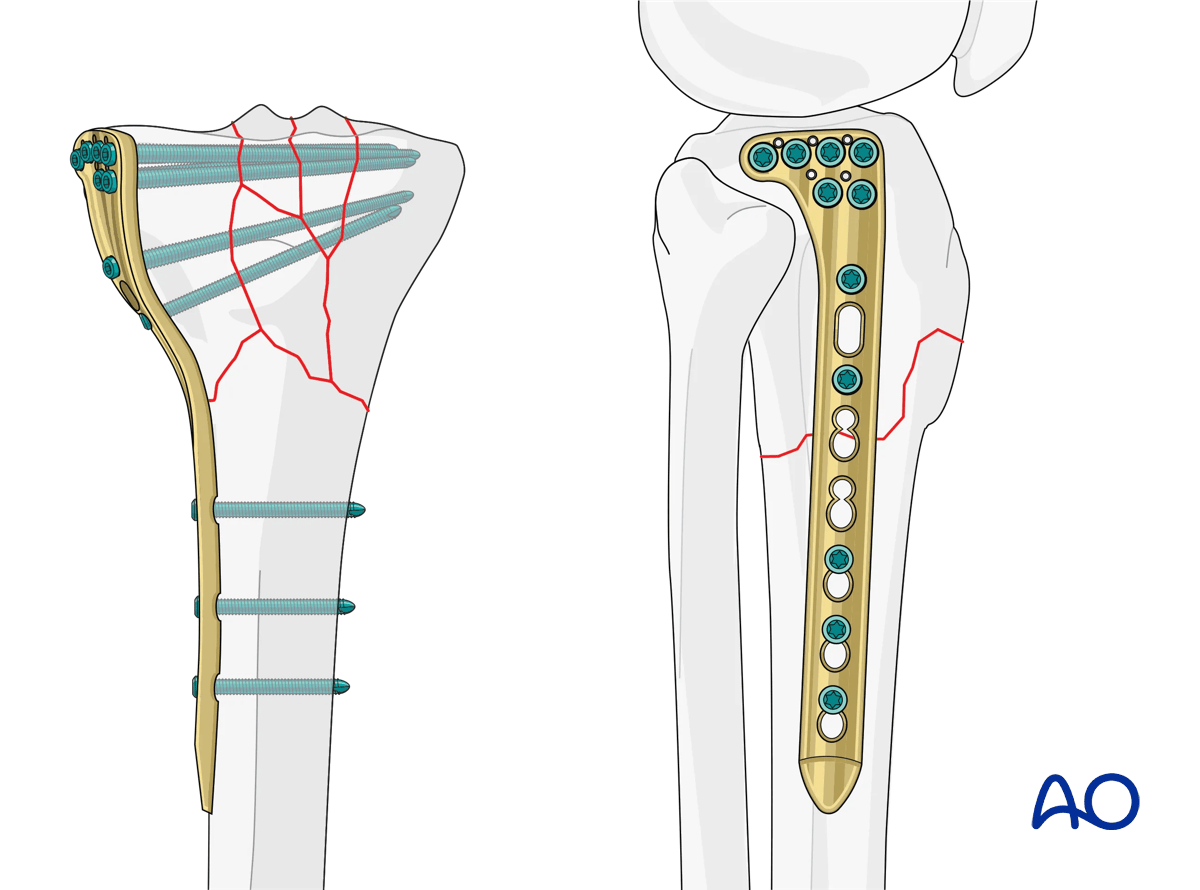
Many angle-stable plates now offer variable angle locking, which allows the surgeon to have some determination of screw trajectory, yet still have the ability to lock. It is worth noting that there will be a nominal position where the locking mechanism has optimal stability. Deviations from this often result in a decrease in stability of the locking mechanism but allow the freedom of avoiding predetermined screw trajectory.
Angle-stable plating can be done using minimally invasive, percutaneous, and open techniques.
Fracture patterns where angle-stable plating is most useful are typically those with significant comminution. In these situations, indirect reduction, secondary stability, and bridge plating concepts are utilized.
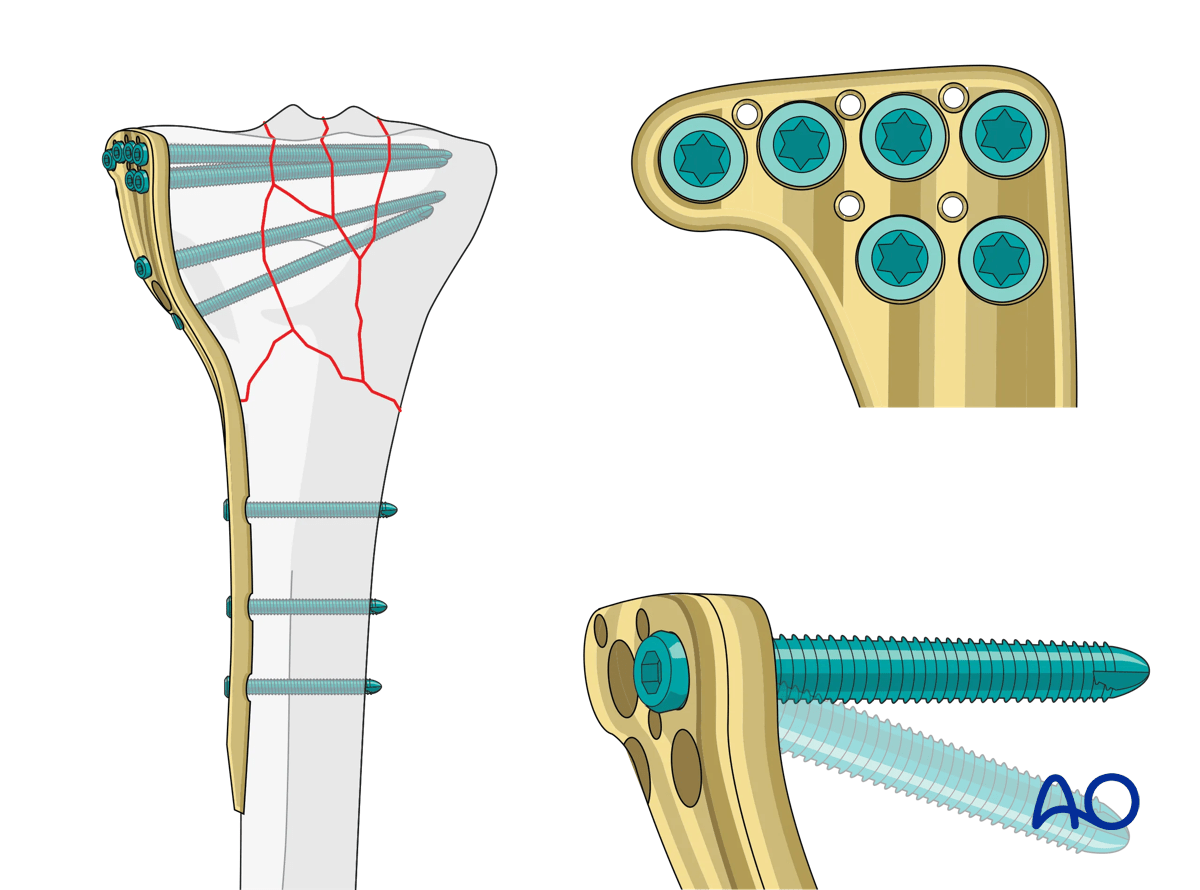
The original device (LISS) was particularly helpful for percutaneous minimally invasive indirect reduction treatment, and this will be shown illustrated in coverage of A-type injuries. Current locking designs are illustrated in partial and complete articular fractures.
Load bearing
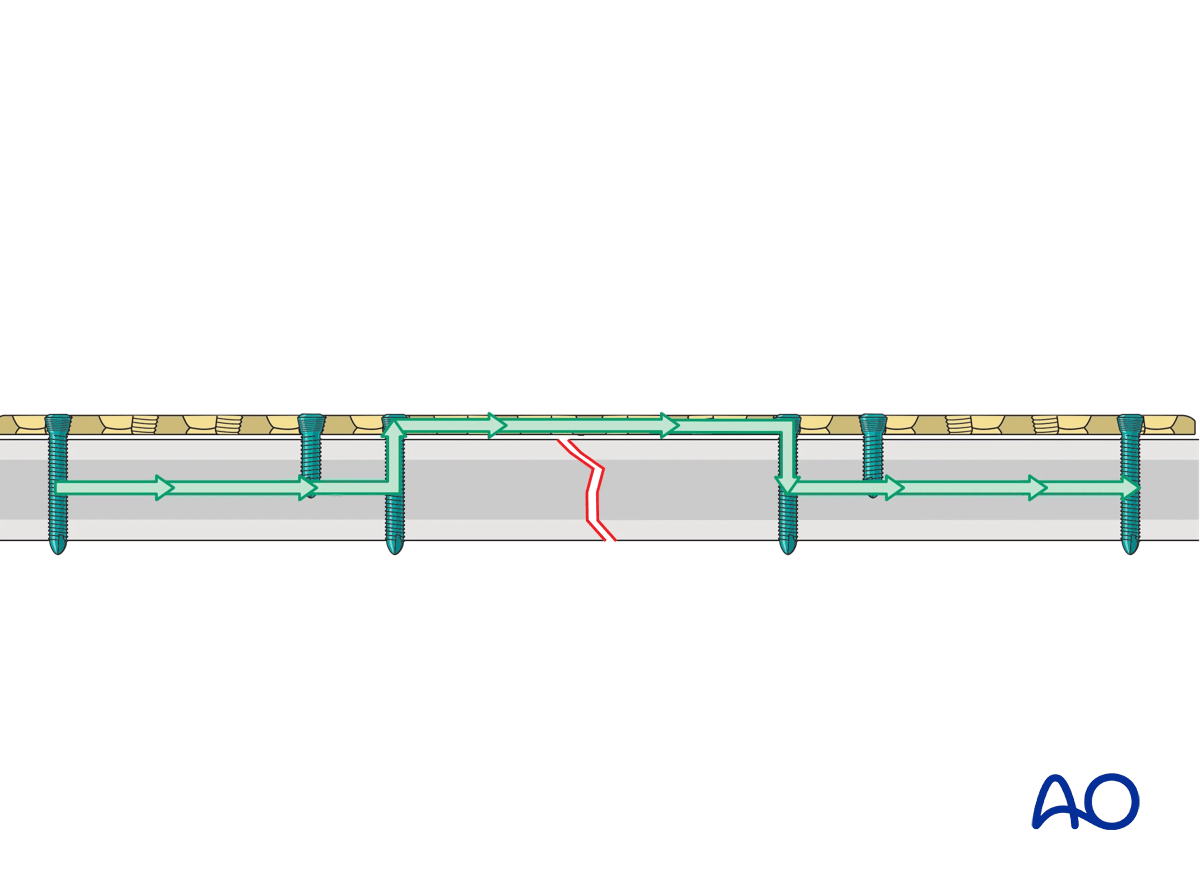
The load from one fracture fragment to the other may be completely borne by the implant unless the fracture is reduced and loaded prior to locking.
2. Preoperative planning
Plate length
When using a bridge-plating technique, which assumes that there is comminution that will be indirectly reduced, the plate length should be approximately three times the length of the zone of comminution, balanced on either side of the fracture area. In the vast majority of instances, however, the comminution is located in the proximal portion of the tibia. Therefore, a general concept is that the distal portion of the plate at least equals the length of the zone of comminution, preferably ending at least at the junction of the middle and distal third of the tibia, with a minimum of 2-3 screws. The screw density in this distal segment should approximate 2.5 screws.
Proximally, given the fact that we cannot take advantage of plate length because of the proximity to the articular surface, the screw density should be increased maximally.
A preoperative x-ray planning template is useful in determining the length of the plate and the position of the screws.
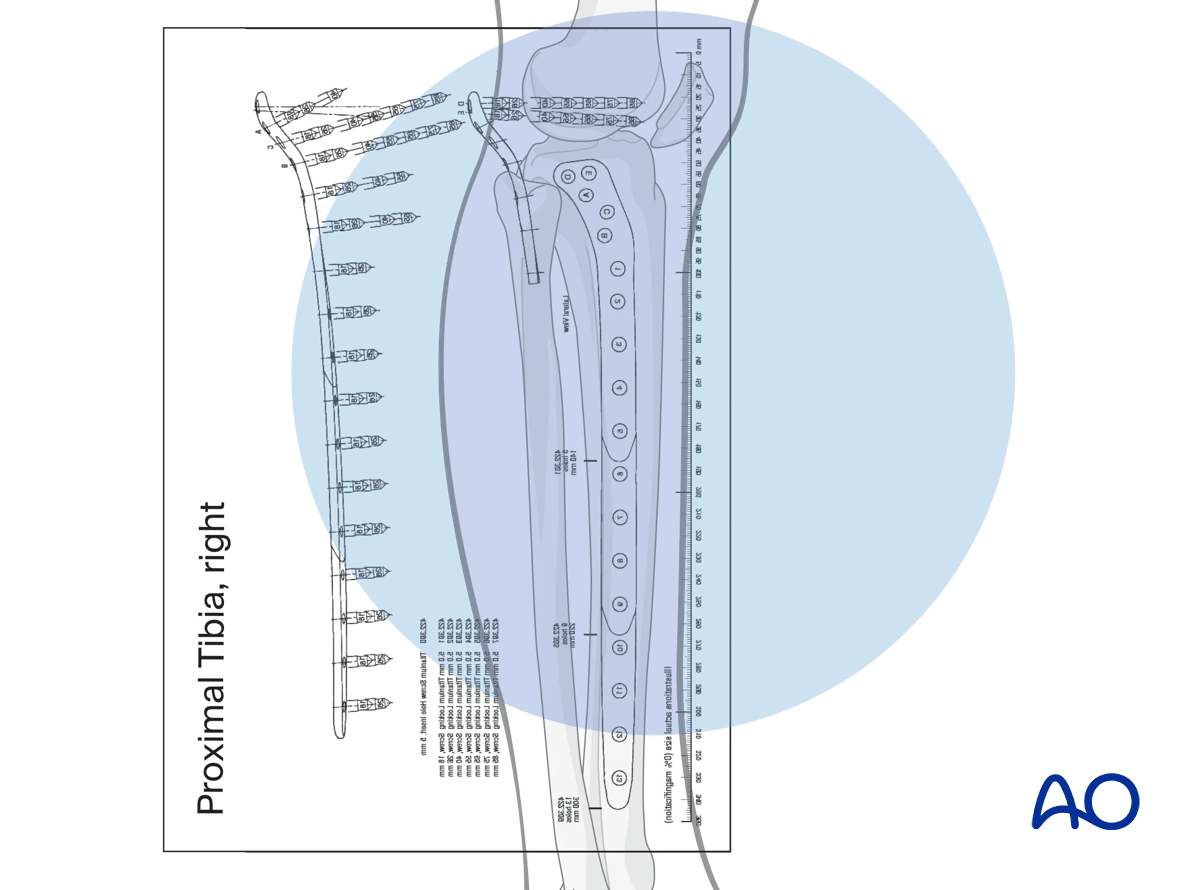
Screw type
In cases of healthy bone structure, unicortical angle-stable screws seem to provide clinically satisfactory stability when cortical bone is normal. However, with significant osteoporosis the torsional and angular stability of the unicortical screw is compromised, as there is a short working length of the screw in the bone. Placement of bicortical screws increases the torsional and angular stability substantially, regardless of the density of the cortex in all situations.
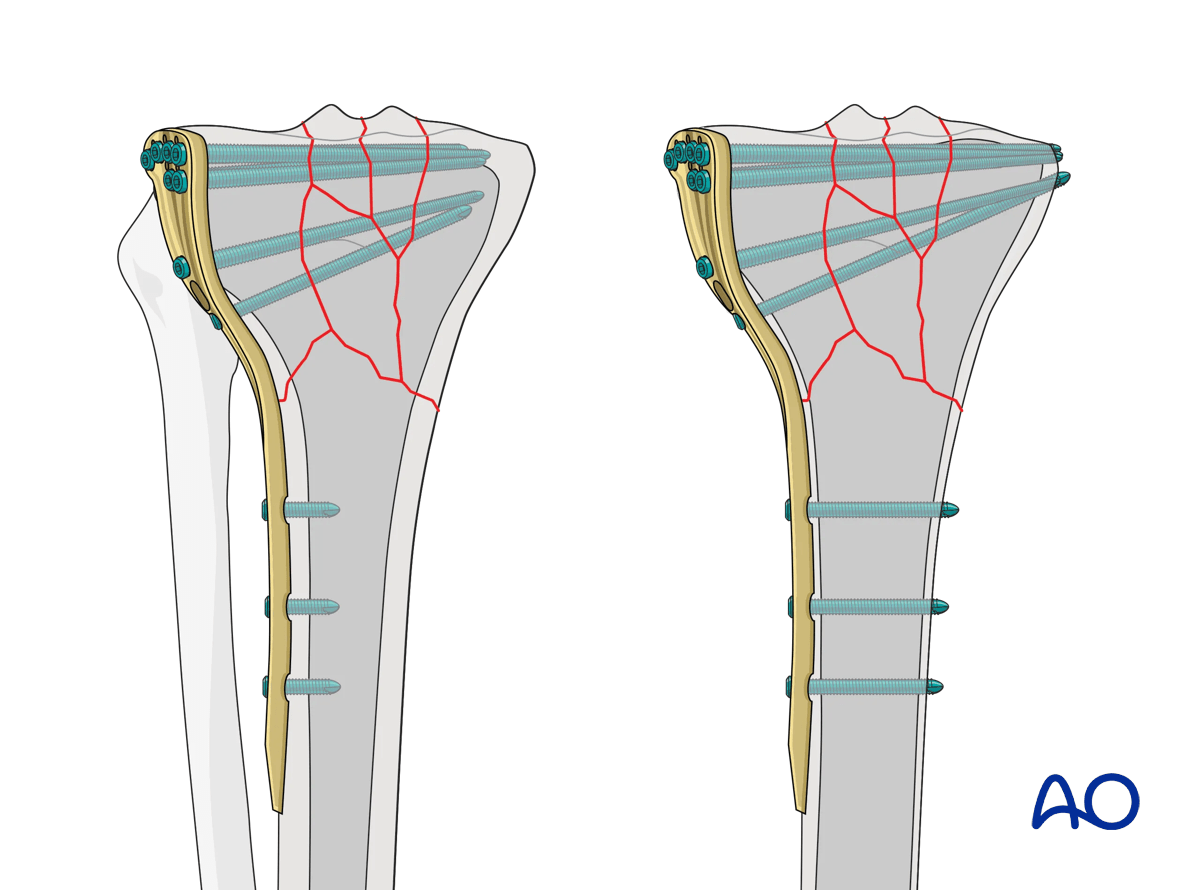
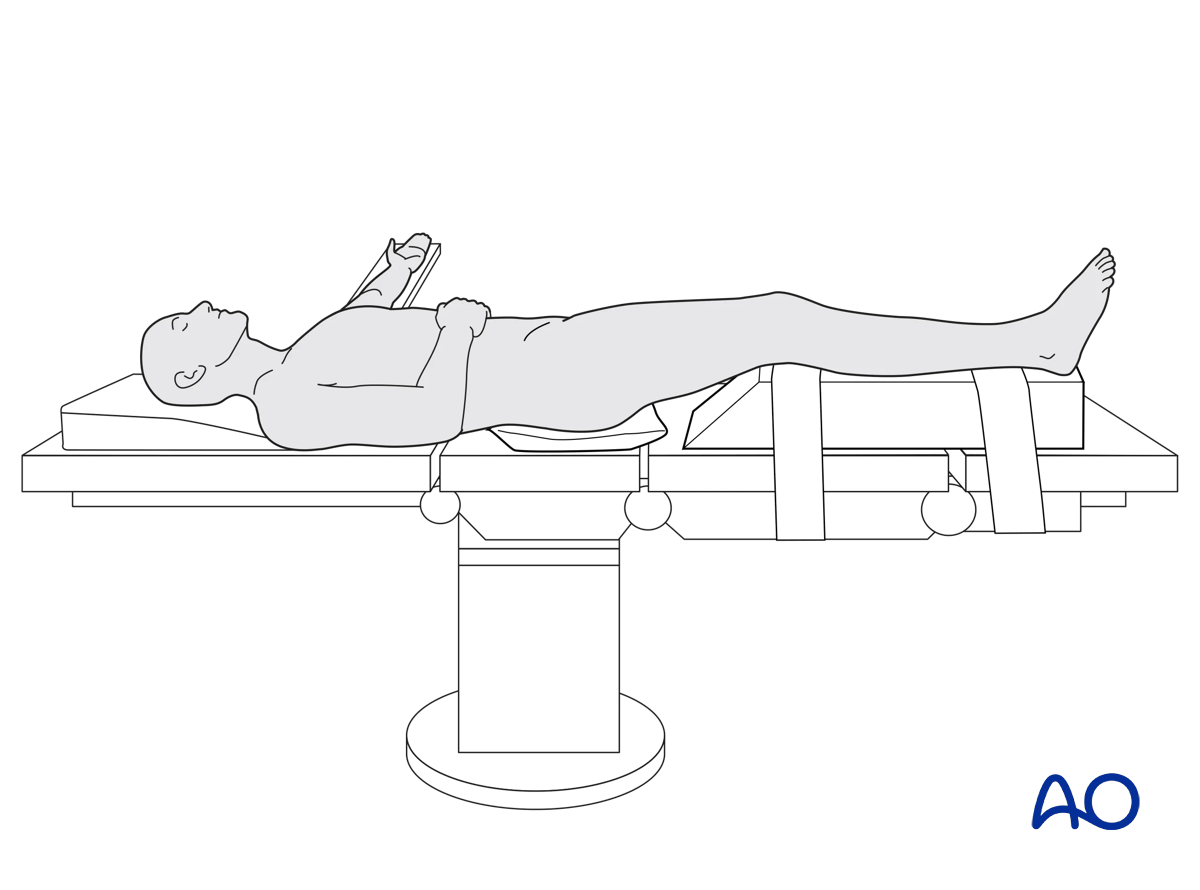
3. Patient preparation
This procedure is normally performed with the patient in a supine position.
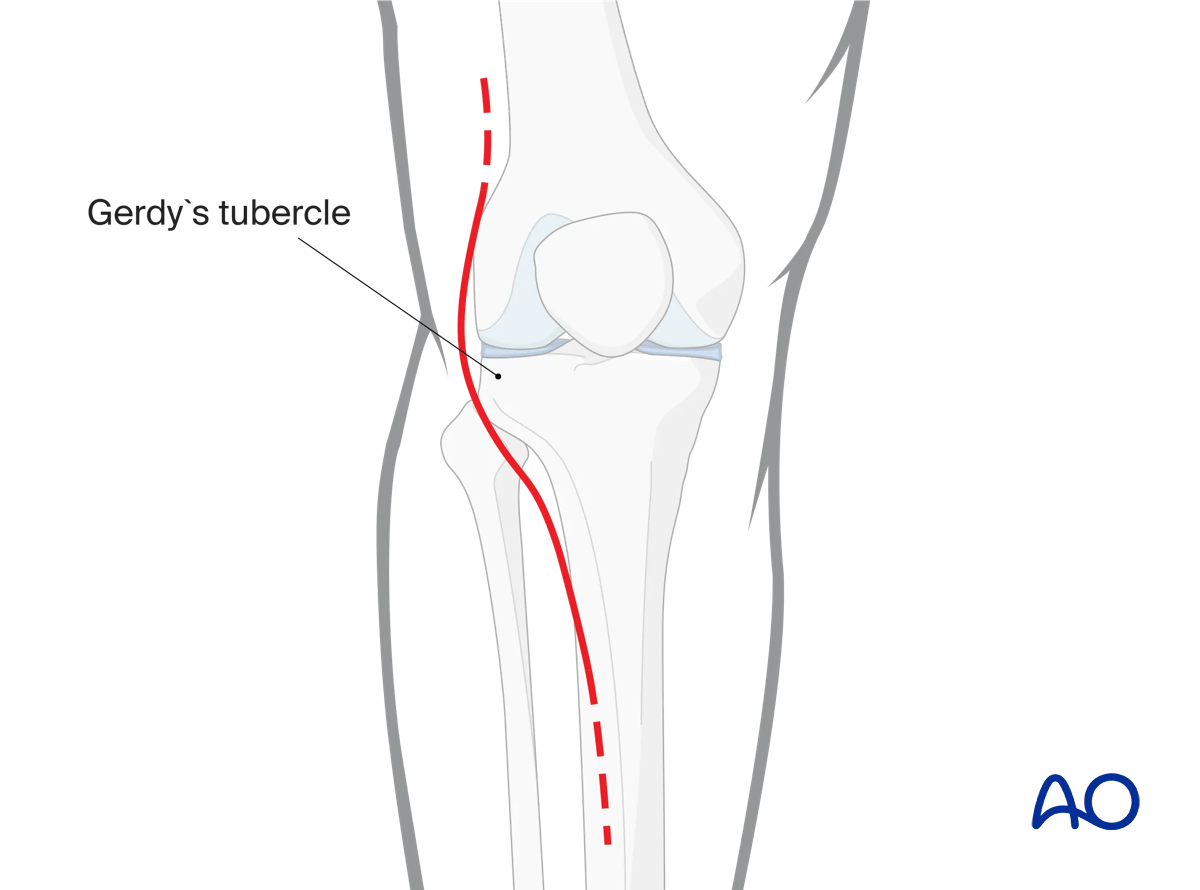
4. Approach
Anterolateral approach
For a more open reduction an anterolateral approach is used. For a minimally invasive technique, the proximal portion of the anterolateral approach is utilized, limiting the incision and deep dissection to just proximal and just distal to Gerdy’s tubercle. Undue skin tension or prolonged soft tissue compression should be avoided. Screws placed distal to the proximal exposed portion of the plate are necessarily placed percutaneously, or with small incisions. Many systems offer external targeting jigs and soft-tissue sleeves to protect the soft tissues during drilling, measuring, and screw placement.
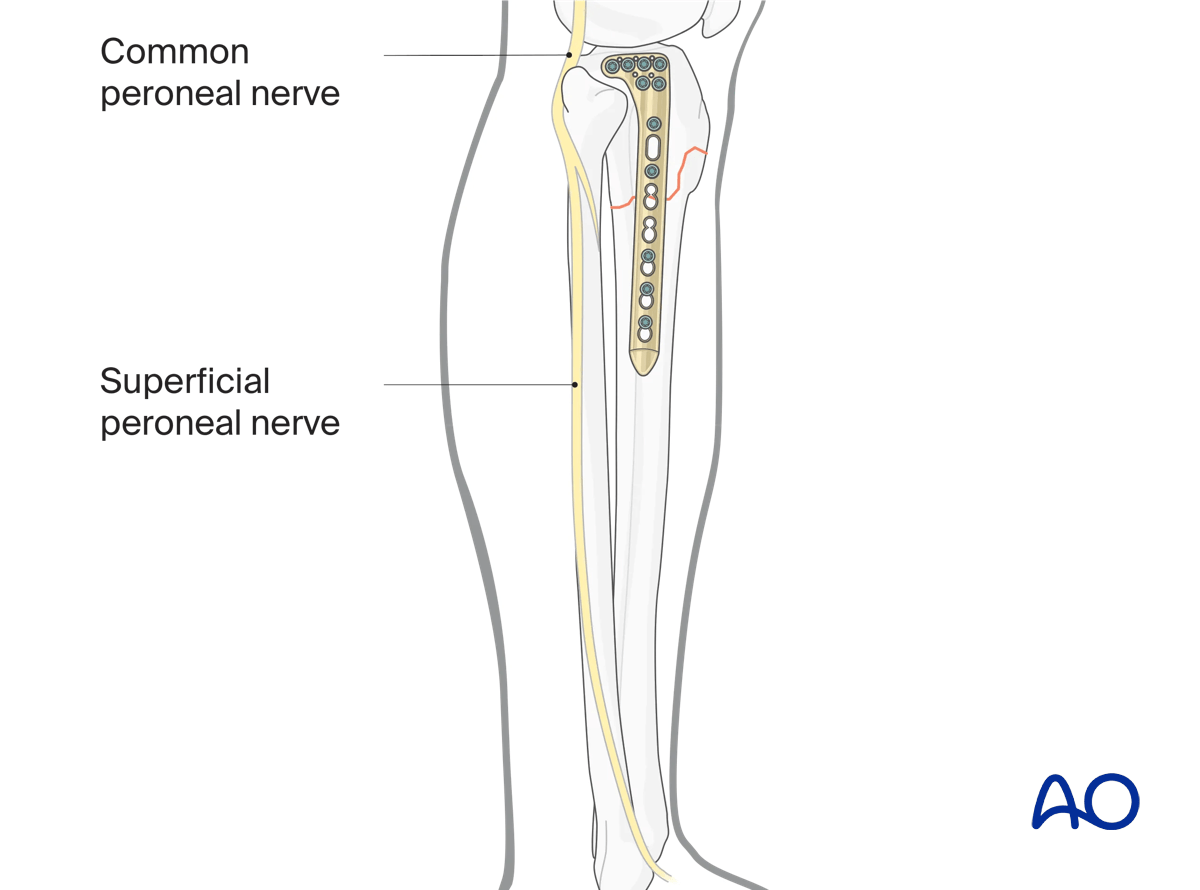
The surgeon must still be aware of local anatomical hazards, particularly the anterior neurovascular bundle and superficial peroneal nerve.
5. Reduction
Indirect reduction
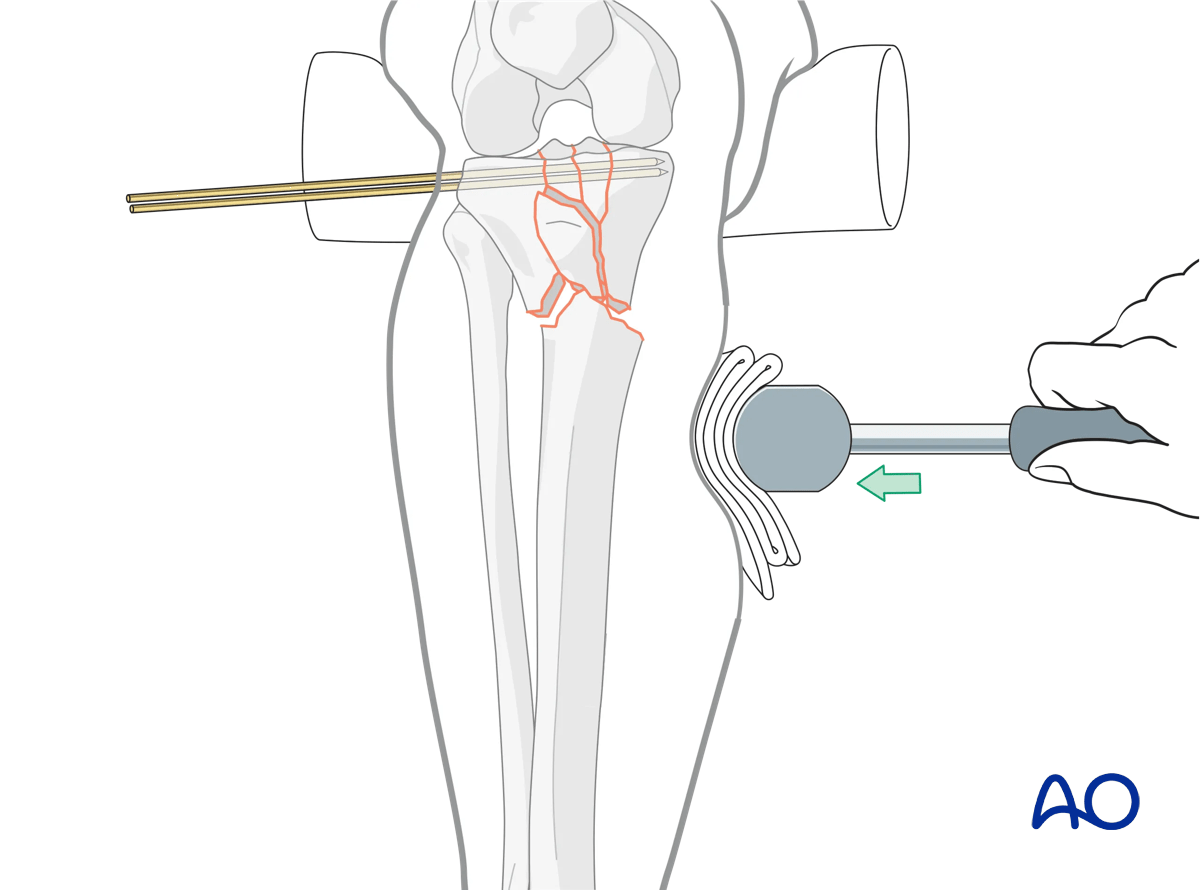
Indirect reduction techniques are typically used for comminuted metadiaphyseal fractures. In these situations, preservation of soft-tissue attachments is paramount. The end result should be vascularized fracture fragments that heal with secondary bone healing as they are subjected to a relative stability construct. A manual reduction, therefore, can be achieved by manipulation of the limb with tractional, rotational, and bending forces. In some cases, reduction may be easier with the help of soft instruments to apply direct forces to the fracture site (eg, a mallet with a towel). Care must be taken not to produce additional soft-tissue damage.
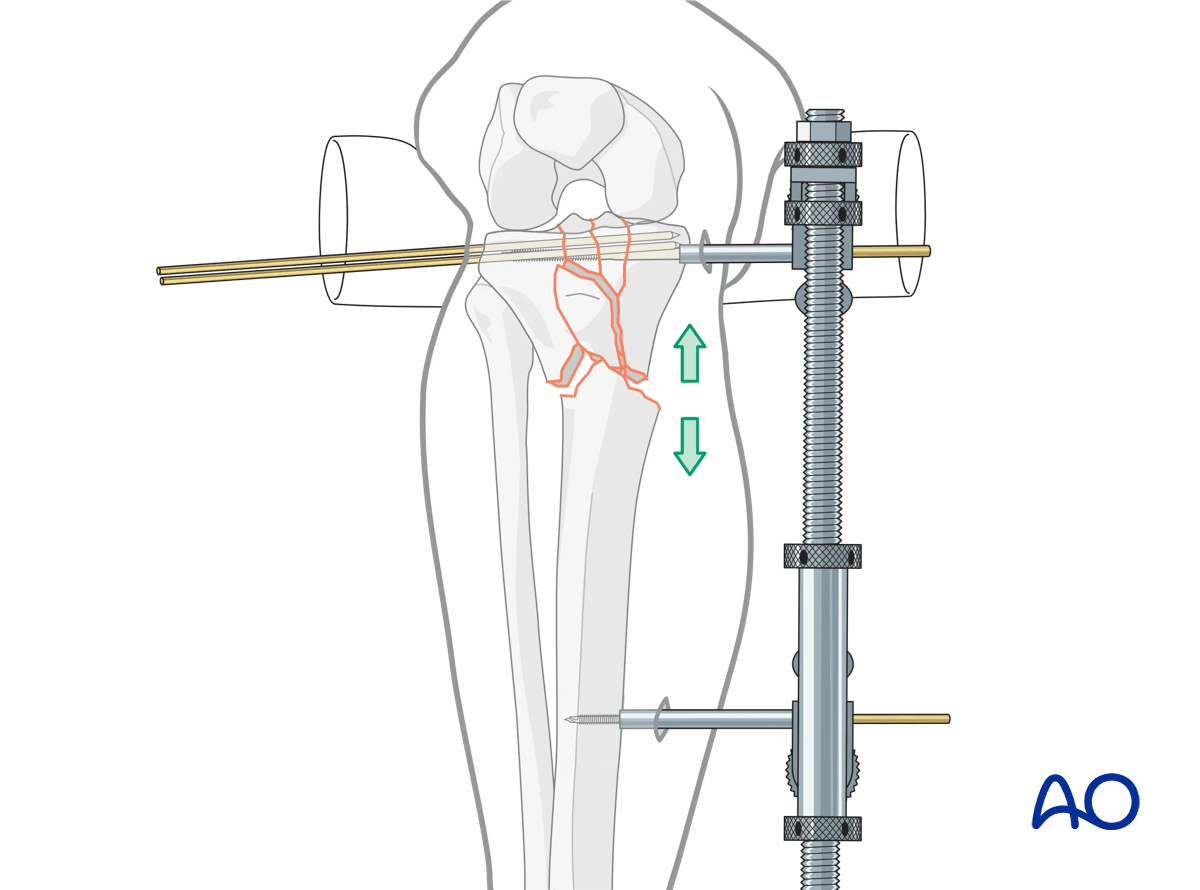
Indirect reduction with external devices
If manual reduction is unsuccessful, indirect reduction can be achieved with the use of external fixation, and/or a universal distractor.
The pin insertions should be planned carefully to avoid conflict with the subsequent placement of screws of the plate used for fixation of the fracture.
If the proximal fragment is small, place the proximal Schanz pins for either the universal distractor or external fixator into the femur, in order to avoid difficulties.
Direct reduction
As a fundamental principle, any articular displacement should be reduced and provisionally stabilized under direct visualization and/or radiographic confirmation. This is typically performed prior to metadiaphyseal reduction. This includes elevating, bone grafting, and provisionally stabilizing any impacted articular fragments.
There may be some situations where relatively simple metadiaphyseal fracture patterns benefit from angle-stable fixation. In these cases, an open exposure and direct visualization of the fracture should be performed. The fracture is reduced in a soft-tissue friendly manner, using the appropriate clamps, and direct reduction maneuvers, the same as one would do with conventional plating. Any interfragmentary compression should be performed prior to inserting locking screws on either side of the fracture.
6. Plate insertion
Once the fracture is provisionally reduced the plate may be placed in an antegrade, submuscular fashion. Plates with a blunt, beveled distal end do not require pathway preparation along the lateral aspect of the tibia. In some situations, the passage of a Cobb elevator may facilitate subsequent plate placement.
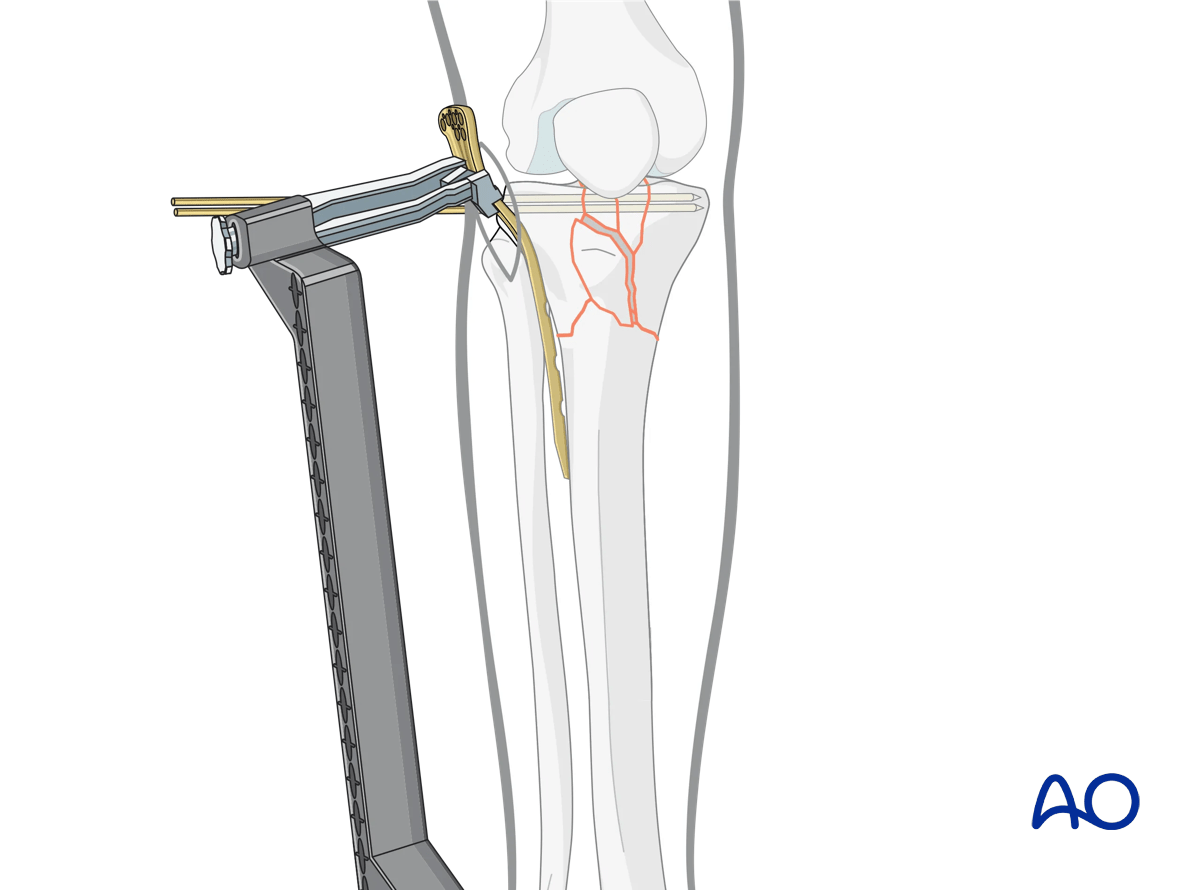
The medial plateau is the larger of the two articular surfaces and is concave in both transverse planes. The lateral plateau is smaller and convex and lies slightly higher than the medial joint surface, which helps in identifying it on the lateral x-ray.
Positioning of the plate
Ideal positioning of the plate depends on several factors. The plate should allow proper fixation of all components of the fracture including the articular segment, and have enough fixation, both proximally and distally. The plate should closely fit the proximal meta-epiphysis to minimize plate prominence.
When inserting screws from lateral to medial the anatomy of the plateau must be taken into consideration in order to avoid penetrating the concave medial joint surface.
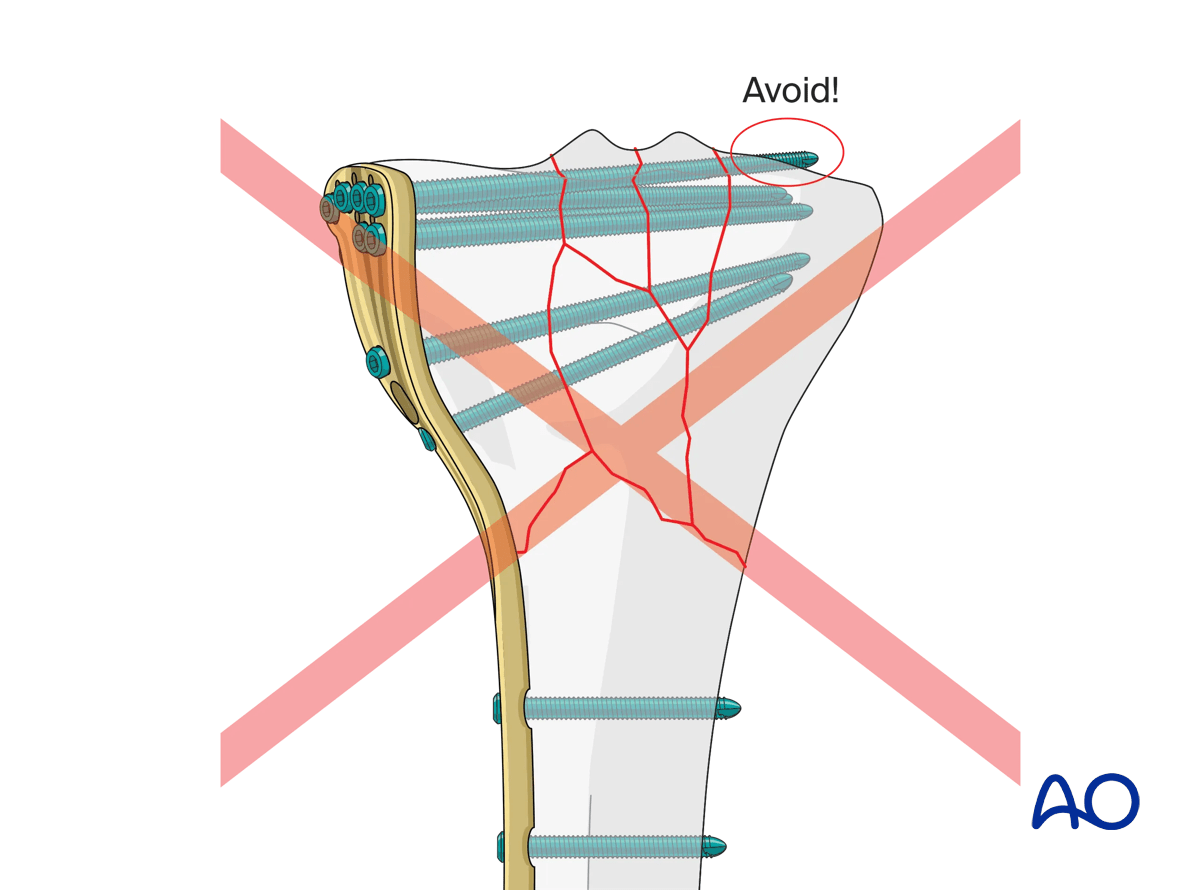
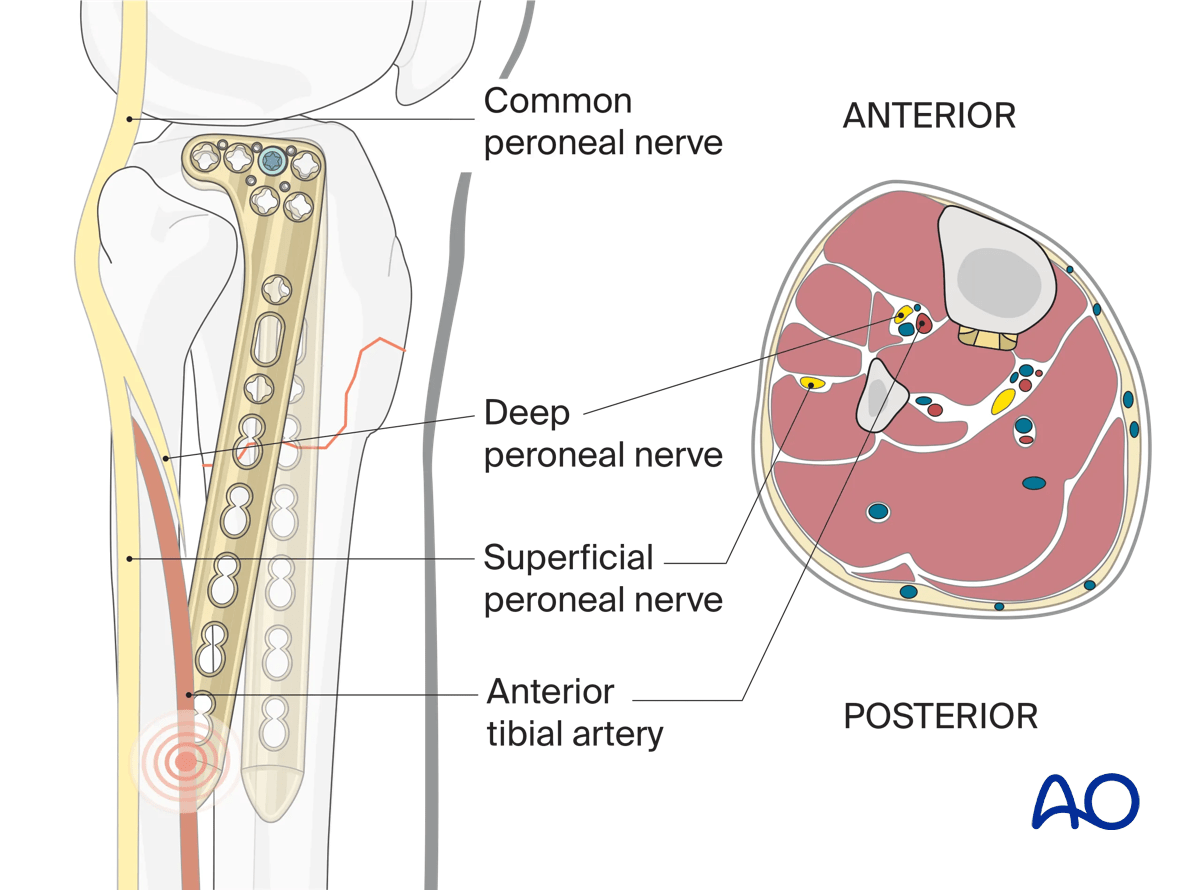
Superficial peroneal nerve
The superficial peroneal nerve is a structure at risk when plating reaches the distal quarter of the tibia laterally. When using percutaneous techniques in this region, a slightly elongated distal incision is useful both to check plate location and avoid damage to the superficial peroneal nerve.

Plate location and rotation determine (fixed angle) locking screw trajectory. Inadvertent internal rotation of the plate risks premature posterior extrusion and neurovascular compromise.
Variable angle locking designs allow for slight changes in screw trajectory if necessary.
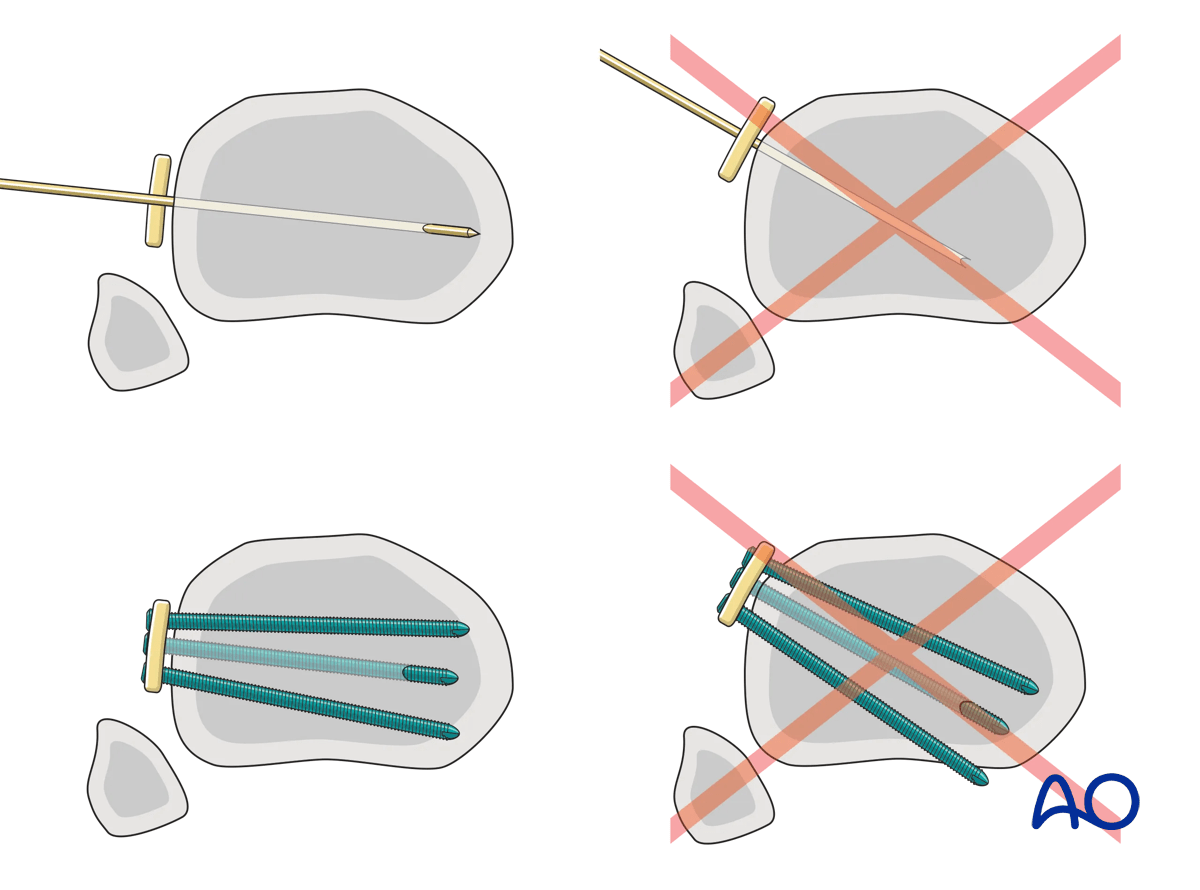
Distally the trajectory of the screws should be into the medullary canal. This cross-section illustration shows incorrect and correct screw placement.
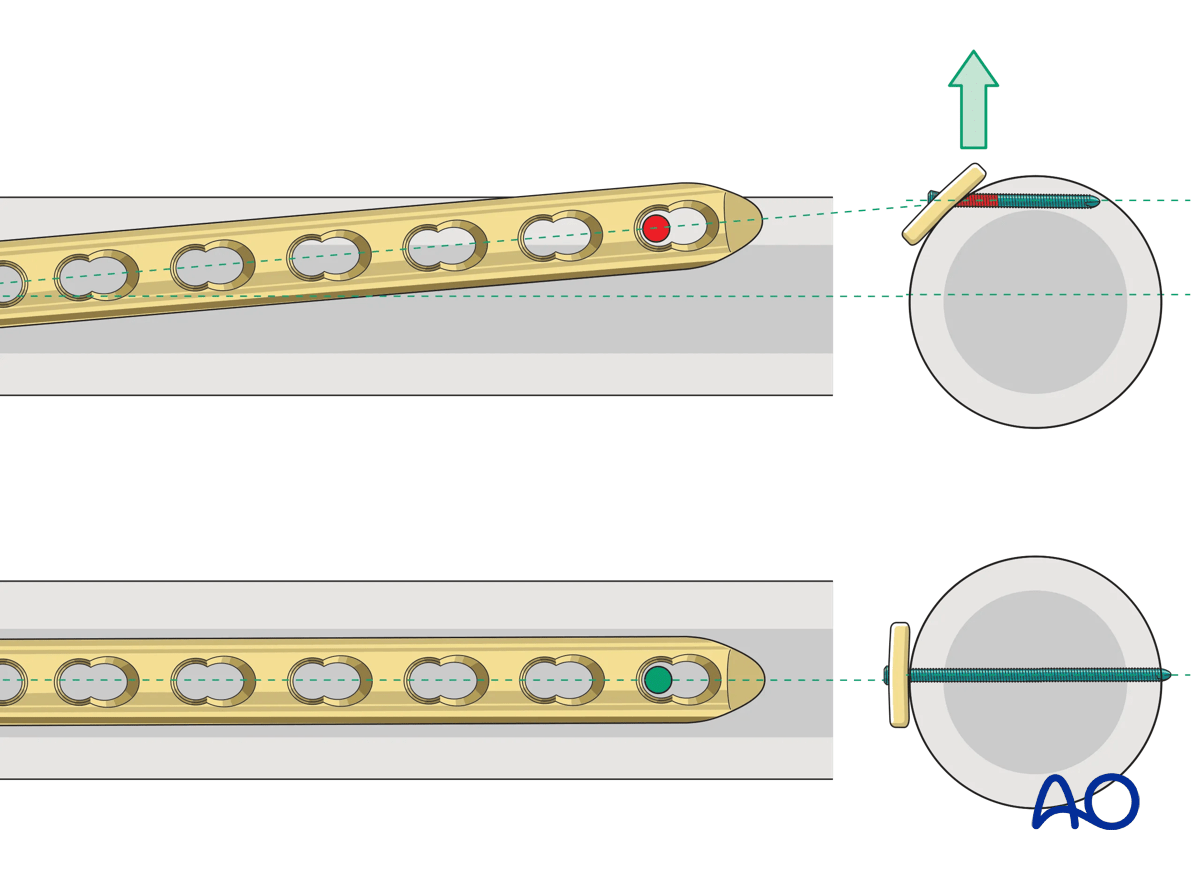
Correct screw placement is confirmed fluoroscopically. Once positioned, the plate can be held proximally with wires and clamps. This can similarly be done distally in a percutaneous or small open technique, using the targeting jig or supplemental percutaneous K-wires.
7. Finalized reduction and screw placement
At this point, any articular surface reduction should have been completed. Any residual translational or angulatory malreductions can now be improved using the plate as a guide for reduction. This can be performed using clamps, or push-pull screws through the plate. In some situations, a full-length plain x-ray is advisable to ensure alignment. Screw placement depends on the type of fracture. The positions of the locking head screws should be chosen in accordance with the established biomechanical principles for internal fixation. The locking head screws should be inserted remote from the fracture gap in the main diaphyseal fragment. Three to four plate holes in the region of the fracture zone should remain free of screws to ensure sufficient elasticity of the construct.
It should be noted that once the initial locking head screws have been inserted into each main fragment, length and rotation are fixed. Antecurvatum and recurvatum deformities can still be adjusted within narrow limits. For this reason, it is recommended to start by inserting the first locking head screw in the proximal fragment- the plate can slightly rotate along this axis to fine tune sagittal alignment.
In some situations, the insertion of cortical screws through the plate will allow the plate to be compressed to the bone and minimize plate prominence and should be done prior to locking the implant. If needed, these cortical screws can be exchanged for locking screws, provided the drill path is within the limits of the trajectories available for locking.
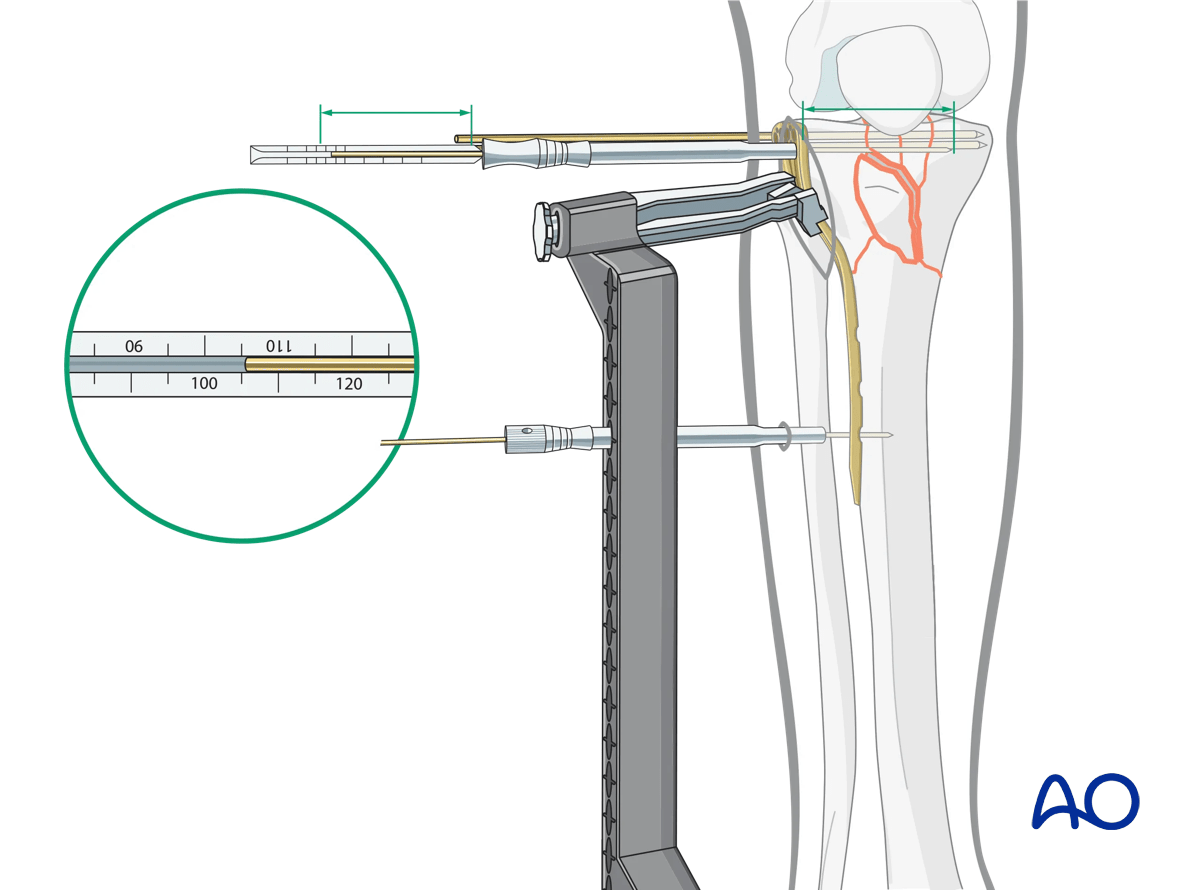
Some systems have an outrigger that facilitates minimally invasive surgery, and allows the insertion of percutaneous self-drilling, self-tapping screws in the metadiaphysis.
Wound closure
The wound should be closed with care taken to reapproximate the iliotibial band at Gerdy’s tubercle over the top of the plate. This will help minimize plate prominence.
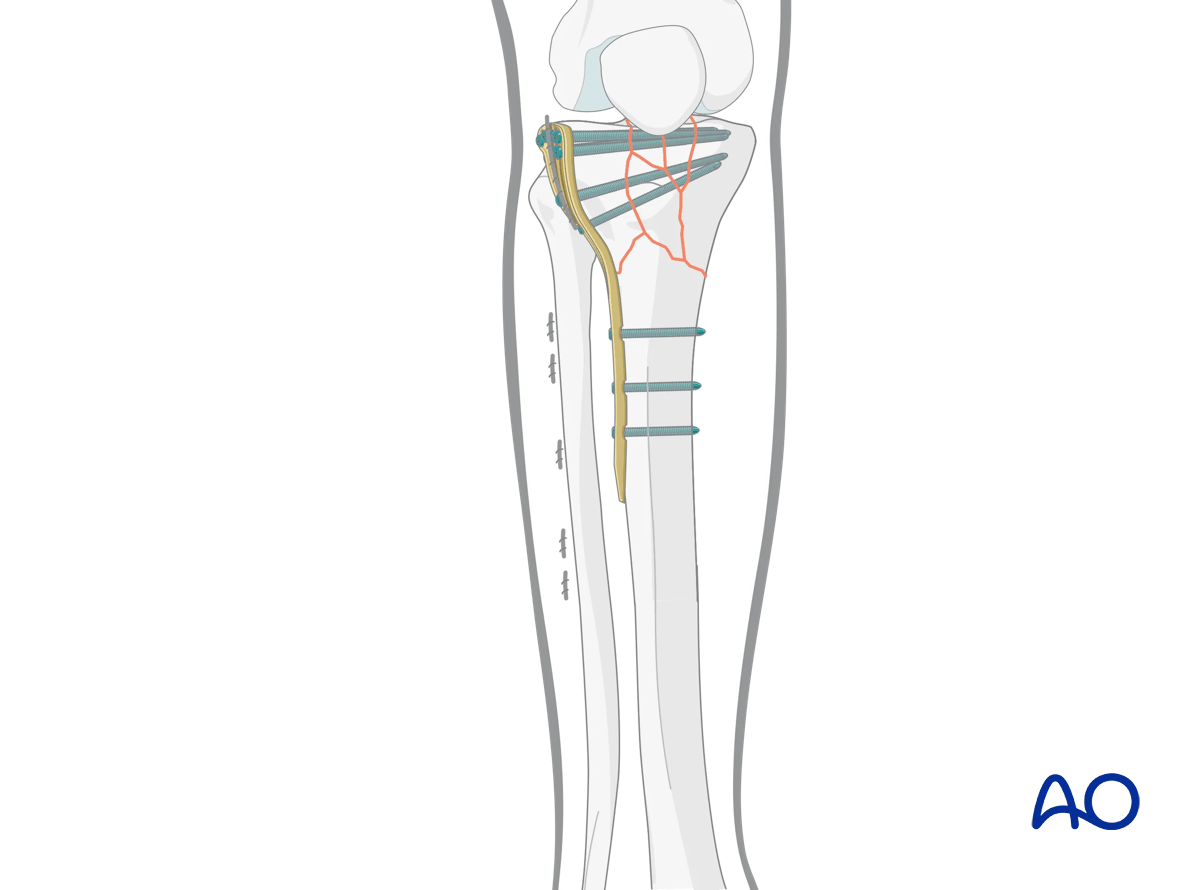
8. Aftercare
Compartment syndrome and nerve injury
Close monitoring of the tibial compartments should be carried out, especially during the first 48 hours after injury and again after surgery to rule out compartment syndrome. More information is provided here:
The neurovascular status of the extremity must be carefully monitored. Impaired blood supply or developing neurological loss must be investigated as an emergency and dealt with expediently.
Consideration for DVT prophylaxis
Oral or subcutaneous administration of DVT prophylaxis for six weeks should be strongly considered.
Functional treatment
Optimal stability should be achieved at the time of surgery, in order to allow early range of motion exercises. Unless there are other injuries or complications, mobilization may be performed on post OP day 1. If available, continuous passive motion (CPM) splints can be very helpful in the early phase of rehabilitation. Static quadriceps exercises with passive range of motion of the knee should be encouraged. Afterwards special emphasis should be given to active knee and ankle movement.
The goal is to achieve as full range of motion as possible within the first 4–6 weeks.
Weight bearing
Weight-of-leg weight bearing is initiated depending on patient comfort. Depending on the severity of the articular displacement, weight bearing can begin as early as 6 weeks postoperatively. In situations where articular displacement was significant weight bearing should be delayed for 10–12 weeks.
Follow up
Wound healing should be assessed within the first two weeks. Subsequently, a 6- and 12-week follow-up with radiographic assessment is usually performed. If a delayed union is recognized, further surgical care may be necessary and should be carried out as soon as possible. Residual knee instability may require delayed reconstruction.
Implant removal
Implant removal is not mandatory and should be discussed with the patient.













