Operative treatment
1. Introduction
Before proceeding with definitive repairs, the patient must be fully resuscitated, fully evaluated, and fit for anesthesia and surgery by a prepared team.
Risk of bleeding
Open book injuries disrupt the pelvic floor, and often tear the pelvic venous plexus. Displacement increases the pelvic volume, allowing greater blood loss before any self-tamponade.
Because of initial bleeding, the patient may be hypovolemic or anemic at the time of definitive treatment. Intrapelvic surgery may disturb injured vessels and cause bleeding to restart.
Transfusions and blood salvage should be anticipated.
Lumbo-sacral nerve root injury
Before undertaking definitive treatment of pelvic ring injuries, It is essential to know the functional status of the patient's lumbosacral nerve roots. A careful and detailed examination is necessary, to assess perineal sensation, voluntary anal sphincter contraction, and bulbo-cavernosus reflex. Cystometrography may be helpful to assess bladder neuromotor function.
Neurologic abnormalities should be correlated with anatomic site of injury:
- If a lumbo-sacral nerve deficit is present in extra sacral injuries, further investigation and possible treatment must be considered.
- If a sacral nerve deficit is present with a sacral fracture, the nerves should be decompressed with fracture reduction and/or sacral laminectomy.
Posterior injury
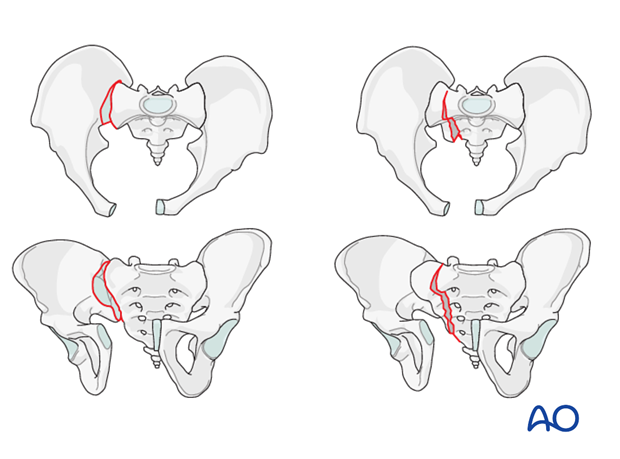
Unilateral open book pelvic ring injuries always involve external rotation of the unstable hemipelvis.
This injury is produced by an impact or compressive force oriented sagittaly (anterior/posterior compression (APC).
Unilateral open book injuries are partially stable because the posterior pelvic arch disruption is partial, with an intact posterior “hinge”, usually the intact posterior S-I ligament.
Occasionally, the “hinge” is an incomplete sacral alar fracture.
Anterior injury
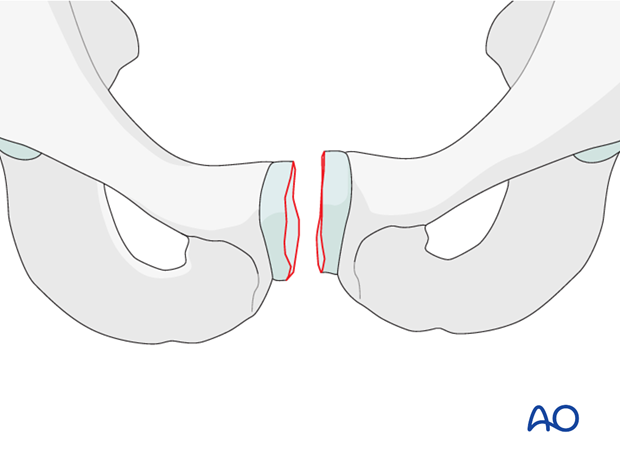
The anterior disruption, which can be quite wide, is almost always through the pubic symphysis.
The width of the disrupted symphysis, as shown by an initial AP x-ray may understate the degree of instability. Stress radiographs may be necessary for accurate assessment of instability.
While some open book injuries with slight symphyseal diastasis do not need surgery, there is no specific width that separates stable from unstable injuries.
Principle of treatment
Theoretically, due to the intact posterior "hinge", open book injuries can be stabilized by reducing and fixing the anterior arch disruption.
However, incomplete sacroiliac ligament disruptions present with a range of instability. This might be recognized by sagittal rotation or displacement on appropriate stress x-rays.
Posterior ring fixation is not necessary for all open book injuries. However, posterior fixation should be considered for more severe posterior arch injuries to prevent:
- persistent posterior pain
- post-traumatic arthritis,
- failure of anterior fixation
Specific indications for posterior fixation of open book injuries remain unclear.
2. Sequence of reduction and fixation
Reduction of the symphysis is performed first. Because of the intact posterior hinge, this restores alignment of the mobile hemipelvis.
If any posterior stabilization is considered, it should follow the anterior arch repair.
3. Patient preparation
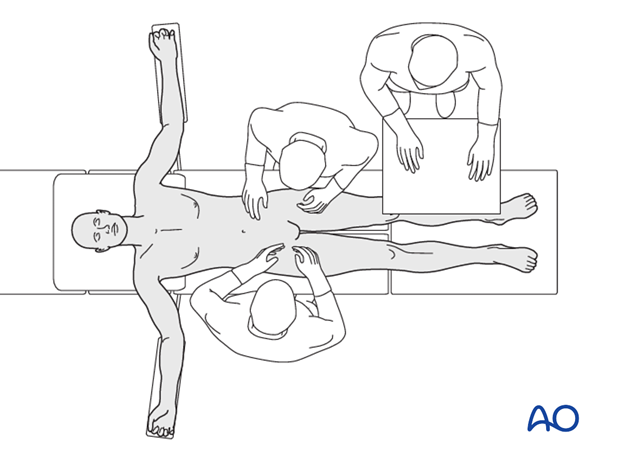
This procedure is performed with the patient in a supine position.
4. Reduction and fixation
Anterior fixation
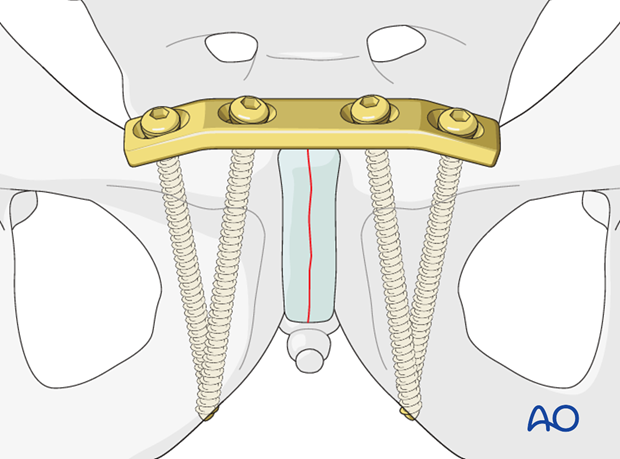
Plating of the pubic symphysis is indicated for symphysis disruptions associated with pelvic ring instability. Evidence of mechanical instability is confirmed with physical exam and/or stress x-rays.
The required technique for symphyseal repair is:
For this procedure an approach to the pubic symphysis with the patient in supine position is used.
Posterior fixation
Partially unstable SI joints or incomplete sacral alar fractures are widened anteriorly on CT scans. If displacement extends all the way through the posterior part of the SI joint or the sacral fracture, complete posterior arch disruption is likely and internal fixation must be considered.
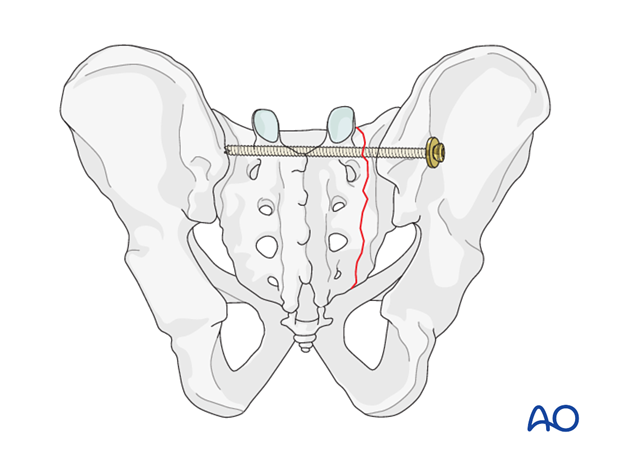
Percutaneous iliosacral screw fixation is usually the preferred technique.
In the rare case of of an open book sacral fracture, this should be repaired with an IS screw, unless it is displaced or associated with neurological deficit.
If available, the use of intraoperative navigation may be beneficial for iliosacral screw fixation.
5. Check of osteosynthesis
Check the completed osteosynthesis with Imaging, and physical exam if there is any question about pelvic stability.
Using inlet and outlet views, with the C-arm, confirm that pelvic deformity has been corrected and that involved sacroiliac joints and pubic symphysis are anatomically reduced.
Unless a C-arm with a large field of view is available, it may be wise to obtain similarly oriented portable x-rays of the entire pelvis, to be certain about overall alignment.
Confirm that reduction of each fracture or joint injury is satisfactory, Make sure that all fixation devices are properly placed, and that each screw is of appropriate length. Multiple views are typically needed, including both axial and perpendicular views for questionable screws. If screws protrude from bone, consider risks to nerves, vessels, and adjacent viscera, especially urethra and bladder after pubic symphysis repair.

6. Aftercare following open reduction and fixation
Postoperative blood test
After pelvic surgery, routine hemoglobin and electrolyte check out should be performed the first day after surgery and corrected if necessary.
Bowel function and food
After extensile approaches in the anterior pelvis, the bowel function may be temporarily compromised. This temporary paralytic ileus generally does not need specific treatment beyond withholding food and drink until bowel function recovers.
Analgesics
Adequate analgesia is important. Non pharmacologic pain management should be considered as well (eg. local cooling and psychological support).
Anticoagulation
Prophylaxis for deep vein thrombosis (DVT) and pulmonary embolus is routine unless contraindicated. The optimal duration of DVT prophylaxis in this setting remains unproven, but in general it should be continued until the patient can actively walk (typically 4-6 weeks).
Drains
Dressings should be removed and wounds checked after 48h, with wound care according to surgeon's preference.
Wound dressing
Dressings should be removed and wounds checked after 48h, with wound care according to surgeon's preference.
Physiotherapy
The following guidelines regarding physiotherapy must be adapted to the individual patient and injury.
It is important that the surgeon decide how much mechanical loading is appropriate for each patient's pelvic ring fixation. This must be communicated to physical therapy and nursing staff.
For all patients, proper respiratory physiotherapy can help to prevent pulmonary complications and is highly recommended.
Upper extremity and bed mobility exercises should begin as soon as possible, with protection against pelvic loading as necessary.
Mobilization can usually begin the day after surgery unless significant instability is present.
Generally, the patient can start to sit the first day after surgery and begin passive and active assisted exercises.
For unilateral injuries, gait training with a walking frame or crutches can begin as soon as the patient is able to stand with limited weight bearing on the unstable side.
In unstable unilateral pelvic injuries, weight bearing on the injured side should be limited to "touch down" (weight of leg). Assistance with leg lifting in transfers may be necessary.
Progressive weight bearing can begin according to anticipated healing. Significant weight bearing is usually possible by 6 week but use of crutches may need to be continued for three months. It should remembered that pelvic fractures usually heal within 6-8 weeks, but that primarily ligamentous injuries may need longer protection (3-4 months).
Fracture healing and pelvic alignment are monitored by regular X-rays every 4-6 weeks until healing is complete.
Bilateral unstable pelvic fractures
Extra precautions are necessary for patients with bilaterally unstable pelvic fractures. Physiotherapy of the torso and upper extremity should begin as soon as possible. This enables these patients to become independent in transfer from bed to chair. For the first few weeks, wheelchair ambulation may be necessary. After 3-4 weeks walking exercises in a swimming pool are started.
After 6 weeks, if pain allows, the patient can start walking with a three point gait, with less weight bearing on the more unstable side.
Full weight bearing is possible after complete healing of the bony or ligamentous legions, typically not before 12 weeks.













