Plate fixation
1. General considerations
Goal of surgery
The main goals of the surgery are to restore the length and stability of the medial column without compromising the blood supply of the cuneiform.
Principles
ORIF of the cuneiform can generally be divided into five steps.
- Reconstruction of the articular surface using lag screws, K-wires, or both.
- Reconstruction of length by distraction
- Grafting to fill any defects (if needed)
- Application of a plate to maintain the reconstruction (if possible)
- Temporary bridging to support reconstruction until healing (if badly comminuted)
In the ideal case:
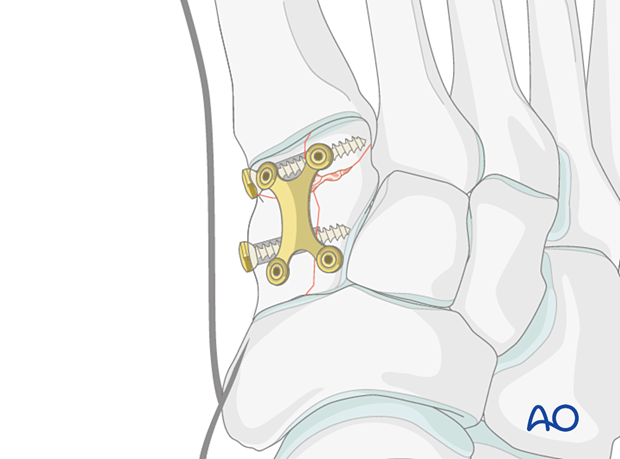
- The articular surface can be reconstructed using lag screws
- The length of the cuneiform is maintained using a plate without fusion or bridging of any joint.
In cases of severe comminution or when the articular fixation is only secured with K-wires or pins, the reconstruction can be protected using a bridging device until the fracture is healed.
Timing of surgery
The timing of surgery is influenced by the soft tissue injury and the patient's physiologic status.

Maintenance of column length and relationship
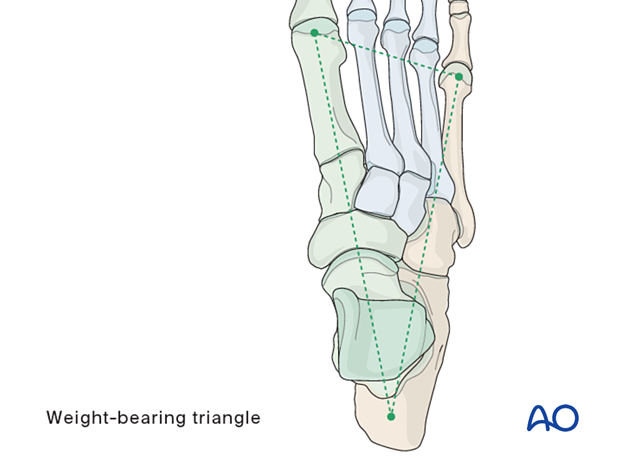
The foot’s form and function depend on the normal relationship between the medial and lateral columns.
If the cuneiform injury has resulted in comminution with loss of length, reconstruction must restore length and normal geometry.
Relative shortening of the medial column leads to cavus, whereas relative shortening of the lateral column leads to flat foot.
Essential versus nonessential joints
The essential joints of the hind and midfoot are the talonavicular, calcaneocuboid, and subtalar joints. Loss of motion in any of these joints will limit the movement of the other two and result in loss of complex hindfoot circumduction.
The tarsometatarsal joints and the naviculocuneiform joint are nonessential for hindfoot motion and can be fused if they cannot be reconstructed.

2. Temporizing measures
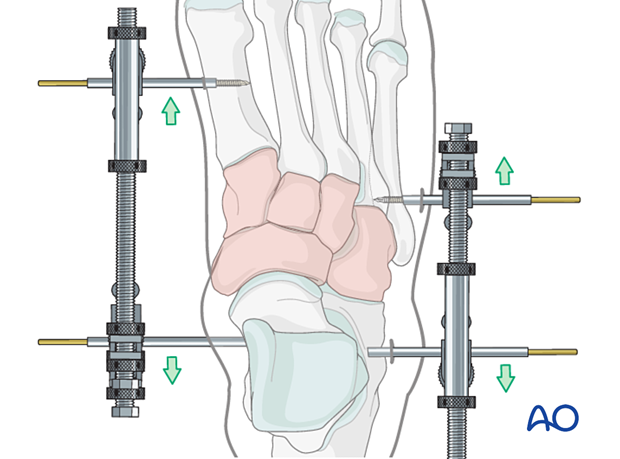
Medial and lateral external fixation (with a distractor device to restore columnar length) should be applied as soon as possible to stabilize the foot and decrease further injury to the soft tissues.
Temporary percutaneous K-wires can be used to reduce displaced fragments and are left as temporary fixation.
3. Patient preparation and surgical approach
The procedure is performed with the patient placed supine with the knee flexed 90°.
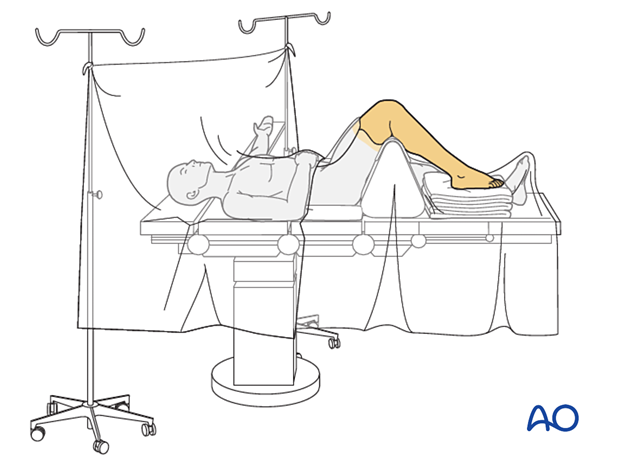
For this procedure, either a dorsomedial approach and/or medial utility incision can be used.
Due to the high-energy injury of these fractures, the soft tissues, including capsule and periosteum, are disrupted. Care should be taken to minimize soft-tissue stripping during the approach. This will help maintain blood supply to the fragments.
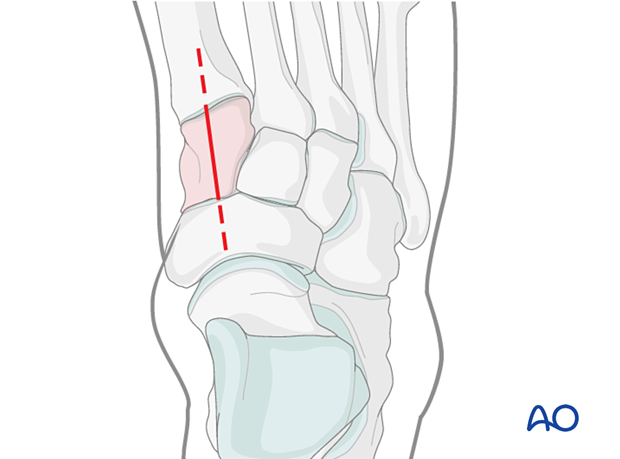
4. Visualization
Use a medial-column distractor to achieve the articular surface visualization needed for accurate reduction and fixation.
Distraction is essential when dealing with comminution or a delay between the injury and the definitive reduction.
The proximal pin is inserted into the neck of the talus through a stab incision. Image intensification can be used to ensure correct pin placement outside the articular surfaces. The correct insertion point is often located 1–2 cm posterior to the navicular tubercle.
The distal pin is inserted in the midshaft of the first metatarsal.
The distraction vector needs to be in line with the talus and the first metatarsal in the medial plane.
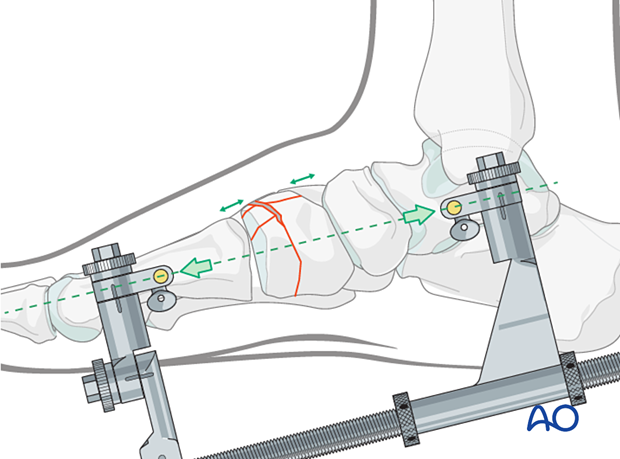
Debridement
Irrigate the fracture site using, eg, a syringe.

5. Restoration of the articular surface
Use a curved elevator to restore the joint surface. The opposing articular surface of the base of the first metatarsal or the navicular serves as a template.
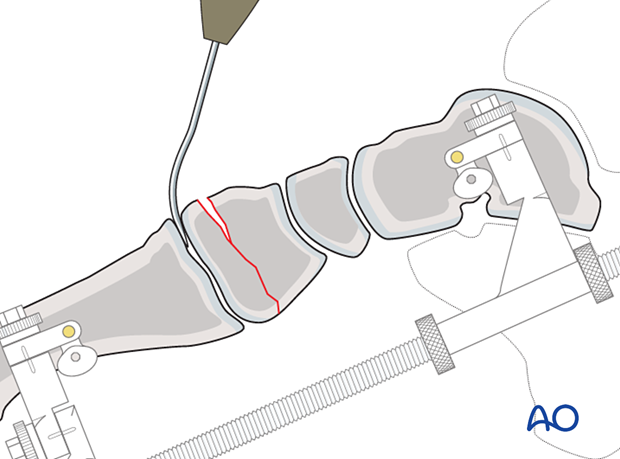
It may be helpful to have a variety of elevators available to aid reduction.
Free fragments with articular surface should be salvaged and secured with K-wires or small screws. If possible, one should try to use lag screws to reconstruct the articular surface. In contrast to lag screws inserted in the diaphysis, these lag screws will typically not penetrate the far cortex, as this would damage the opposite articular surface.
Ideally, the reconstruction should be made by inserting hardware only into the cuneiform. However, if needed, hardware may also be inserted into the navicular or base of the first metatarsal for added support.
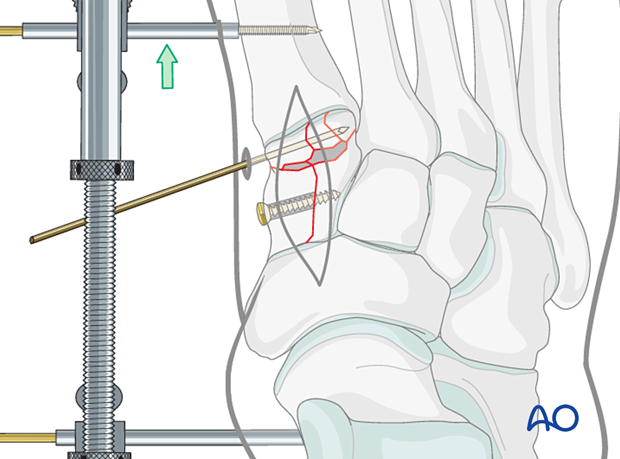
6. Restoration of medial-column length
Once the fracture(s) has/have been reconstructed, use the medial-column distractor to restore the length of the medial column.
It is helpful to have an x-ray from the uninjured side to compare the reduction with the non-injured side. It will help in judging length and overall morphology.
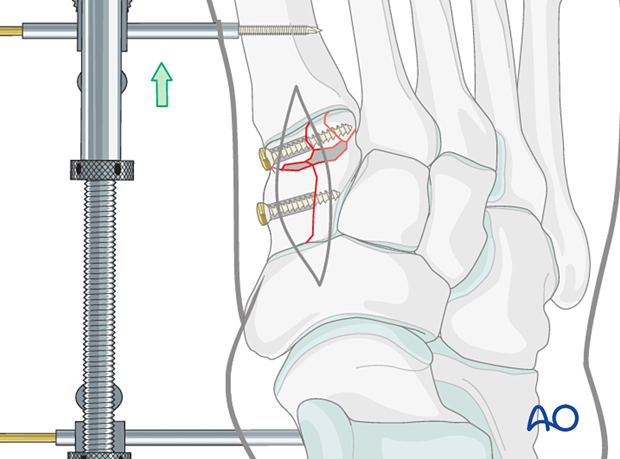
7. Grafting of the bony defect
If the length restoration has resulted in bony defects, these should be filled with bone graft.
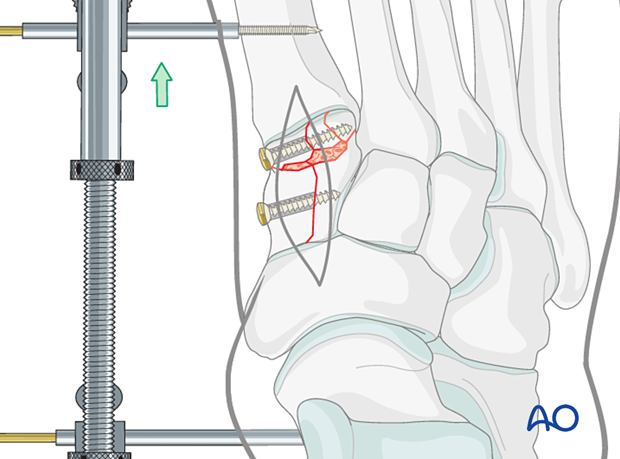
8. Application of plate
A plate should ideally be applied to maintain the length of the medial column.
If this is not possible, the reconstruction should be bridged temporarily using an external fixator or a bridge plate until the bone is healed.
If the reconstructed cuneiform is stable, plates with non-locking screws can be used.
For multifragmentary or osteoporotic bone, locking head screws should be used.
Contour the plate to fit the individual anatomy.
Care must be taken to prevent screw penetration of the joint surfaces. If fixed angle locking head screws are used, additional contouring of the plate may be necessary to prevent joint penetration.
When contouring locking plates, care must be taken not to deform the screw holes.
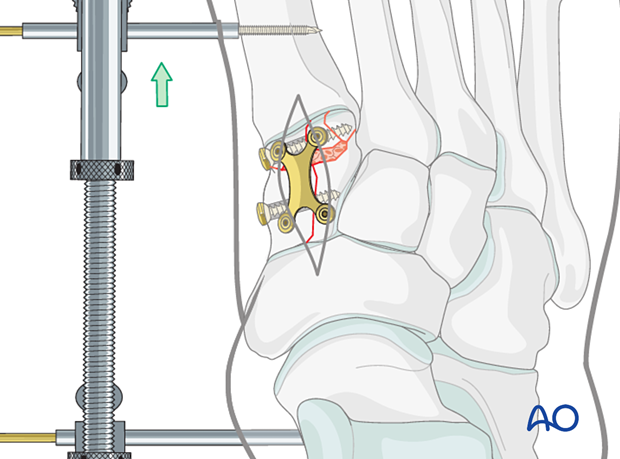
Quality control
Using intraoperative imaging, verify
- Restoration of the appropriate length of the medial column
- Restoration of cuneiform shape
- Appropriate screw placement and length
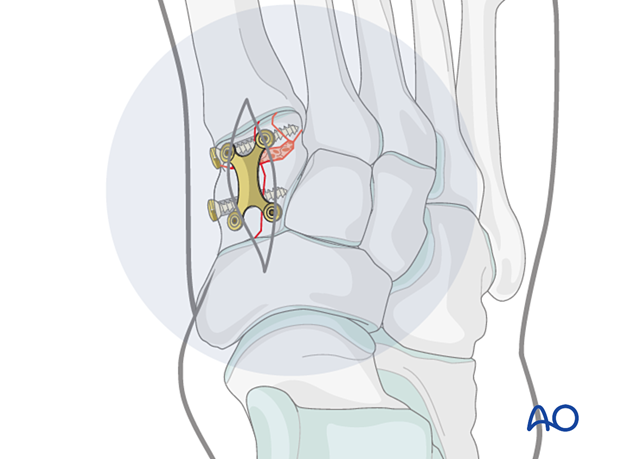
9. Temporary bridging (if needed)
A reconstructed cuneiform that is not strong enough to withstand compressive forces may be bridged temporarily to protect the fixation.
One can use the distractor, an external fixator, or a plate as a bridging device.
The bridging device should be removed when there is radiographic evidence of bone healing.
Typically locking plates will give better strength and purchase for the fixation.
The plate selection will depend on whether the fracture is within the cuneiform or juxta-articular.
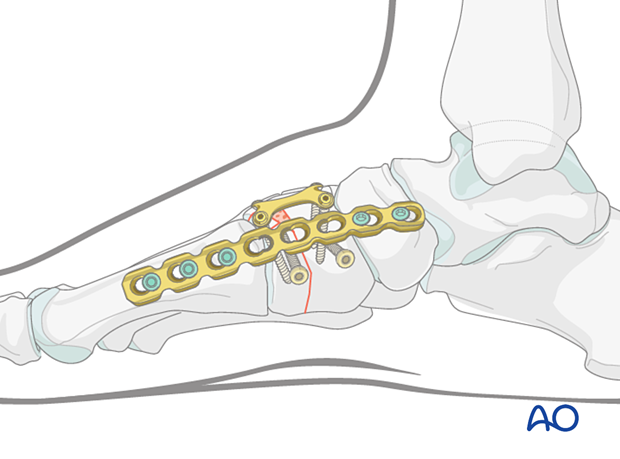
Temporary bridging with a plate
Plating can be performed through the dorsal or medial incision; however, soft-tissue stripping should be avoided.
Extensive dissection can be avoided by sliding the contoured plate subcutaneously along the medial aspect of the foot.
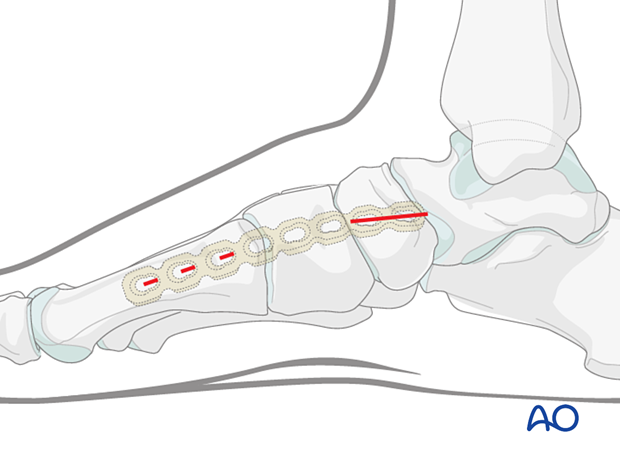
The plate length should allow for fixation using a minimum of two screws both proximally and distally.

The plate needs to be contoured to achieve a good fit and prevent tenting of the skin.
- In-plane bending to adapt to the arch of the medial foot
- Out of plane bending to adapt to the medial contour of the medial column
- Torquing to fit both the neck of the talus proximally and the medial aspect of the first metatarsal distally
The step-by-step bending procedure is analog to the bending of reconstruction plates.
The plate may be pre-contoured using a saw-bone foot model and fine-tuned in situ as an alternative to using a template.

Fix the bridge plate, using a minimum of two screws proximally (navicular) and two or three screws distally (first metatarsal).
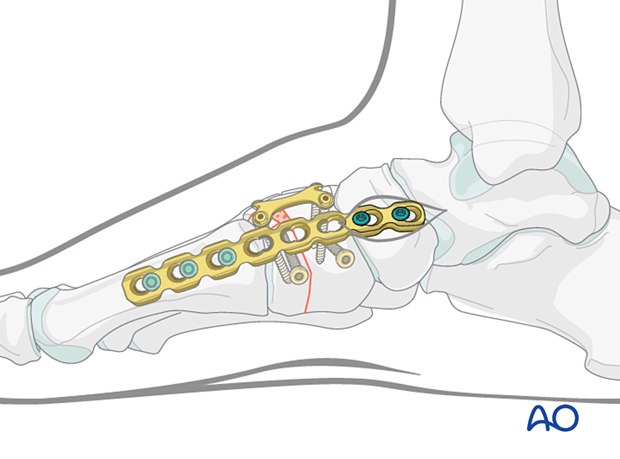
Temporary bridging using an external fixator
Instead of bridge plating, the medial column distractor can be replaced with an external fixation construct, which can be left in place while the bone heals.
Two bicortical pins are inserted in both the calcaneus and the 1st metatarsal.
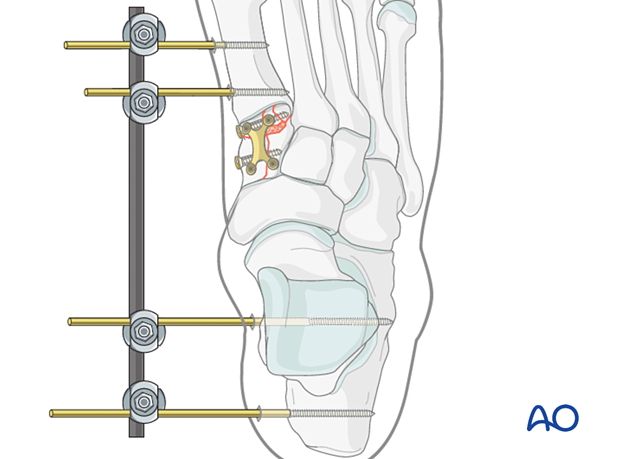
Removal of bridging device
The bridging device should be removed when there is radiographic evidence of cuneiform healing, typically a minimum of three months.

10. Aftercare
Dressing
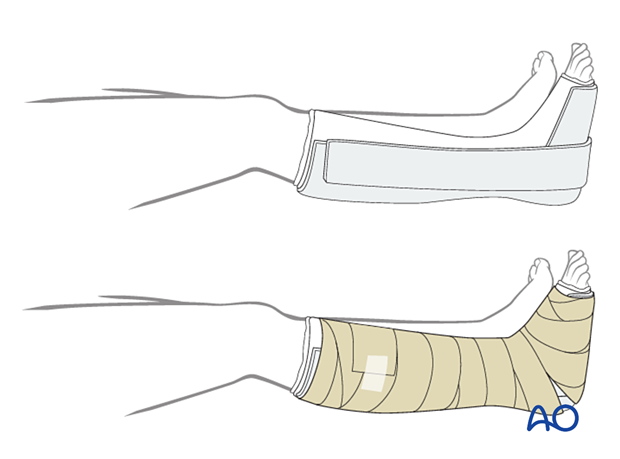
The non-adherent antibacterial dressing is applied as a first layer. Sterile undercast padding is placed from toes to knee. Extra side and posterior cushion padding are added.
Immobilization
The foot should be immobilized for the first two weeks, which can be achieved using a three-sided plaster splint. The anterior area is left free of plaster to allow for swelling. Ensure that the splint’s medial and lateral vertical portions do not overlap anteriorly and that the splint does not compress the popliteal space or the calf.
Follow-up
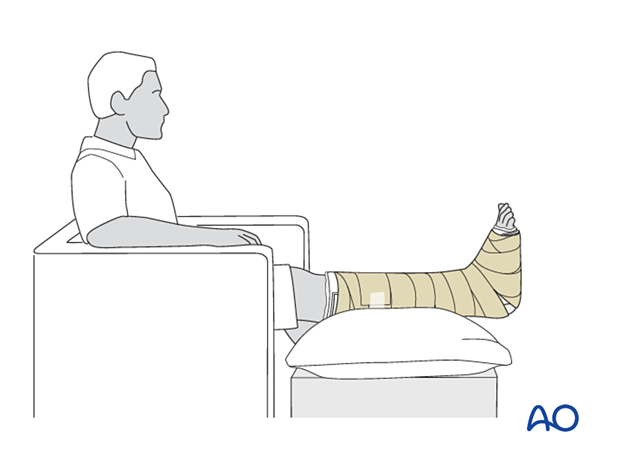
The patient should be counseled to keep the leg on a cushion and elevated. Remember not to elevate the leg too much as it may impede the inflow. The foot’s ideal position is halfway between the waist and the heart when the patient is sitting. While seated, the foot should be on a cushion and elevated, but if badly swollen, the patient must be supine since elevating the foot while seated decreases swelling less effectively.
Avoid direct pressure against the heel during recumbency to prevent decubiti.
The OR dressing is usually left in place and not changed until the first postoperative visit at two weeks when x-rays are obtained once the dressing is removed. If any complication is suspected (eg, infection or compartment syndrome), the dressing must be split and, if necessary, removed to allow full inspection.
The strict non-weight bearing should be maintained until there is evidence of healing and any transfixion K-wires (6–12 weeks) or bridging devices (min 12 weeks) are removed.
Daily toe movement is encouraged.
Formal physical therapy should not begin in the early postoperative period.
A gastrocnemius release may need to be performed in cases with postoperative gastrocnemius contracture. This occurs more typically in the mid and hind-foot.













