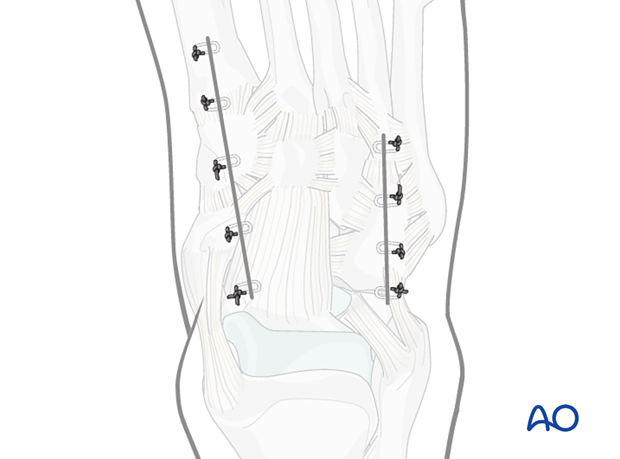
Dorsomedial approach to the midfoot
1. Introduction
The following structures can be accessed through this approach:
- 1st and 2nd proximal metatarsals
- 1st and 2nd tarsometatarsal joints
- Medial and middle cuneiform
- Navicular
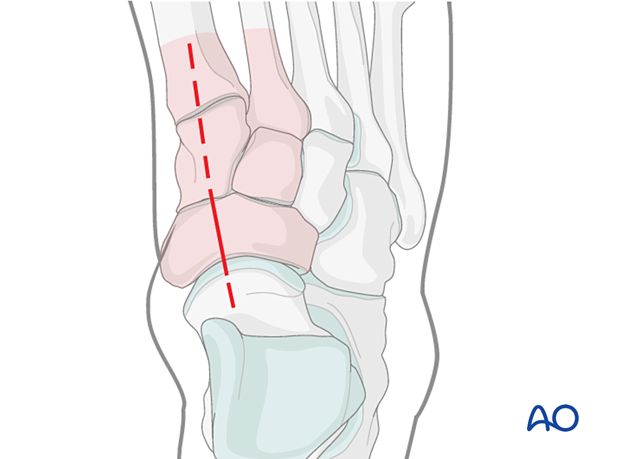
Combination with a dorsolateral approach
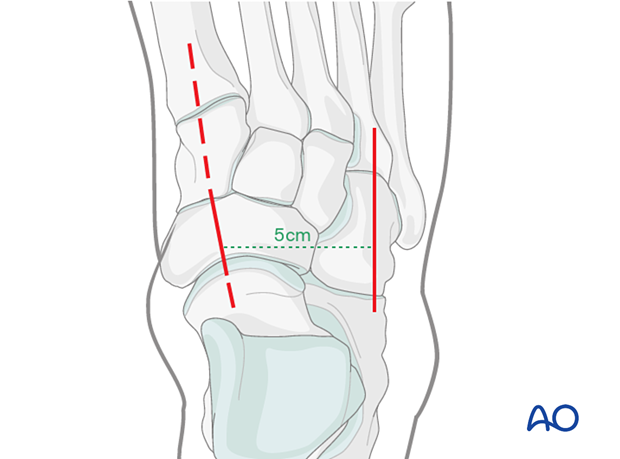
This approach may be combined with the dorsolateral approach to the cuboid. In this case, it is crucial to keep a minimum of 5 cm distance between the two incisions to ensure the survival of the skin bridge.
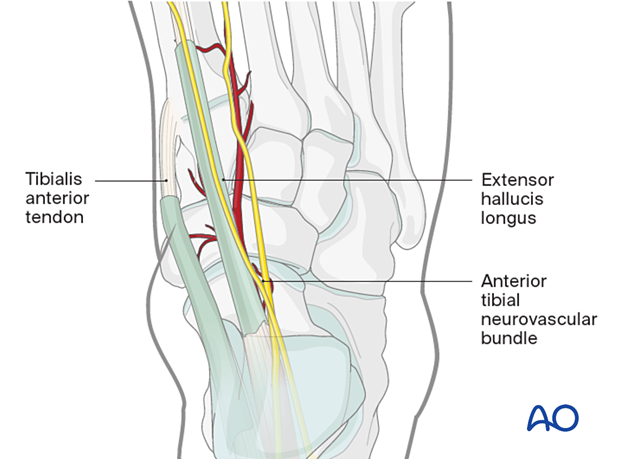
2. Anatomy
The critical anatomical structures encountered in this approach are the following:
- Extensor hallucis longus
- Tibialis anterior tendon
- The anterior tibial neurovascular bundle
3. Skin incision
The incision is centered over the fracture in the interval between the tibialis anterior and the extensor hallucis longus.
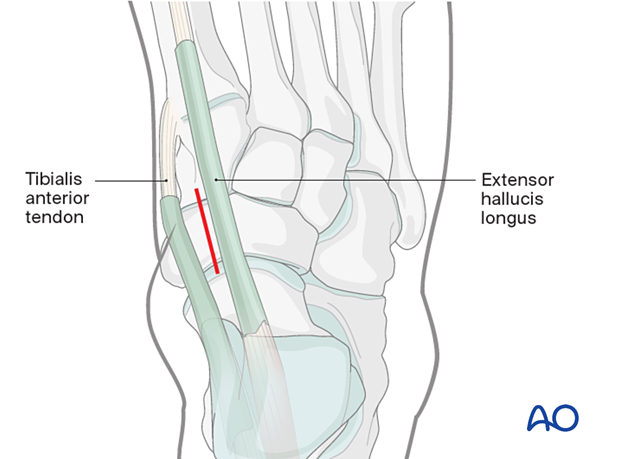
The incision can be extended distally along the first metatarsal axis to expose the cuneiform and the proximal 1st metatarsal.
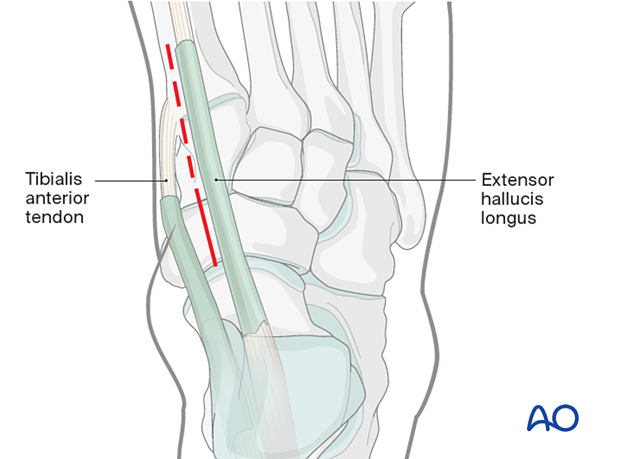
The incision can be extended proximally to include the talonavicular joint.
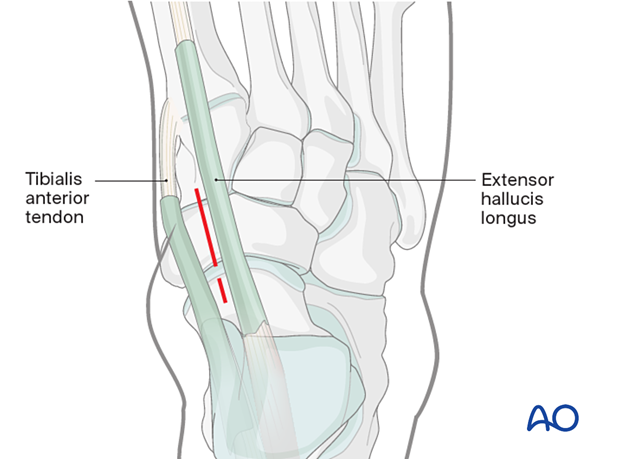
Further dissection can proceed in either of two planes. However, the flap should be full thickness with no undermining of tissues.
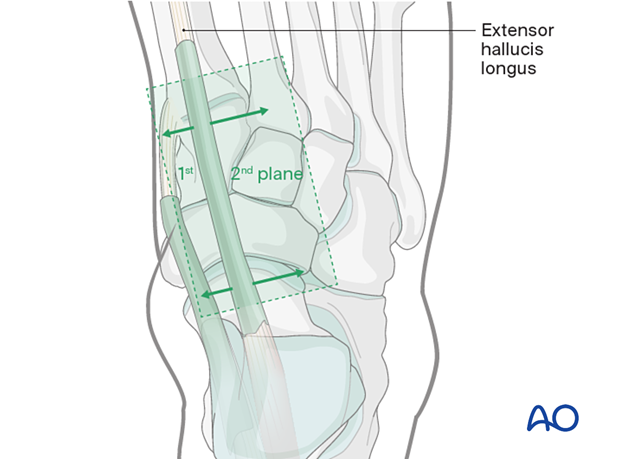
Medial plane: Exposure of navicular and medial cuneiform
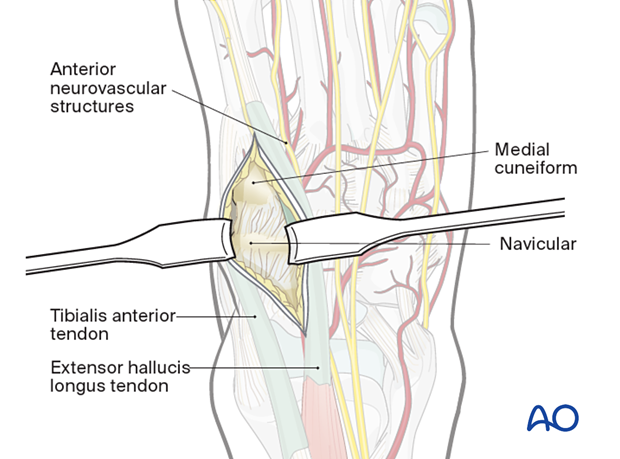
The plane between the EHL and the tibialis anterior is developed to access the navicular and the medial cuneiform.
Lateral plane: Exposure of 1st and 2nd tarsometatarsal joints and the middle cuneiform
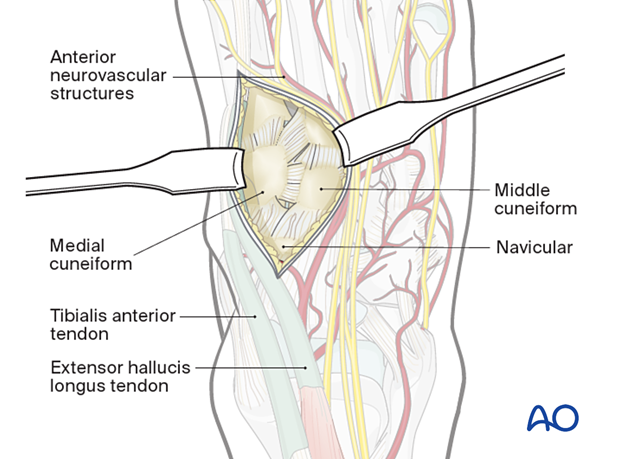
The plane lateral to the EHL is used to access the 1st and 2nd tarsometatarsal joints and the middle cuneiform.
The plane between the EHL and the anterior tibial neurovascular bundle is developed. The anterior tibial neurovascular bundle is mobilized laterally (most often) to allow better visualization.
Further development of this plane exposes 1st and 2nd tarsometatarsal joints and the middle cuneiform.
4. Visualization of the joint
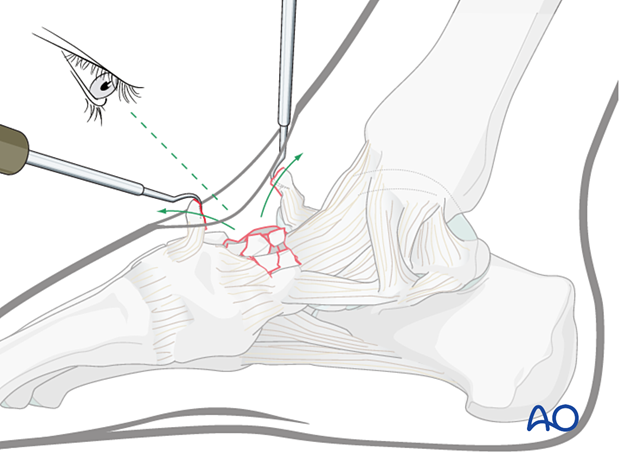
In a high-energy injury, the comminution may be severe. Take care not to strip the periosteum or joint capsule from any small pieces. If a piece is attached to a proximal piece of the joint capsule, then the best course of action may be to flip it proximally so as not to disrupt its soft-tissue attachments. Once the joint is reconstructed, this “trap-door” piece can be reduced and fixed.
5. Additional medial percutaneous incision
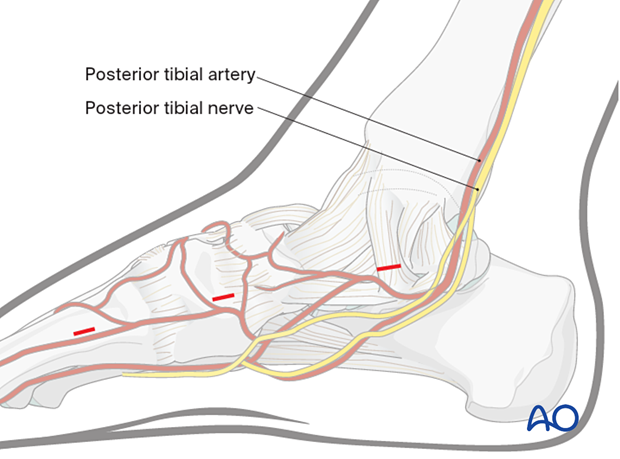
In some cases, additional medial stab incisions may be required (eg, insertion of lag screw or distractor pins).
6. Wound closure
The wound is closed in layers taking care to prevent skin tension.