Posterior decompression and stabilization C3-C7
1. Introduction
Preoperative planning
Based on CT and MRI imaging, a plan should be prepared to determine:
- The size and optimal location of implants used
- Whether spinal cord decompression is necessary and if so, the amount of tissue to remove in order to achieve sufficient spinal cord decompression
Every case will be unique, and we will here illustrate just one example.
Use of dexamethasone
Administration of dexamethasone (10 mg bolus, 4 mg every 6 hours) is recommended as soon as ESCC causing neurologic deficit is diagnosed. Dexamethasone should be stopped or tapered as soon as spinal cord decompression is completed.
Embolization
Embolization procedures are recommended to reduce operative blood loss in hyper vascular tumors. , especially for larger resections.
Neurological evaluation
The preoperative neurological assessment must be carried out as described in the Neurological Evaluation.
2. Patient positioning and surgical approach
Preoperative planning
For this procedure the patient is placed in the prone position and the posterior approach to the cervical spine is used.
3. Instrumentation
Posterior instrumentation should normally include two levels above and two to three below the affected vertebra.
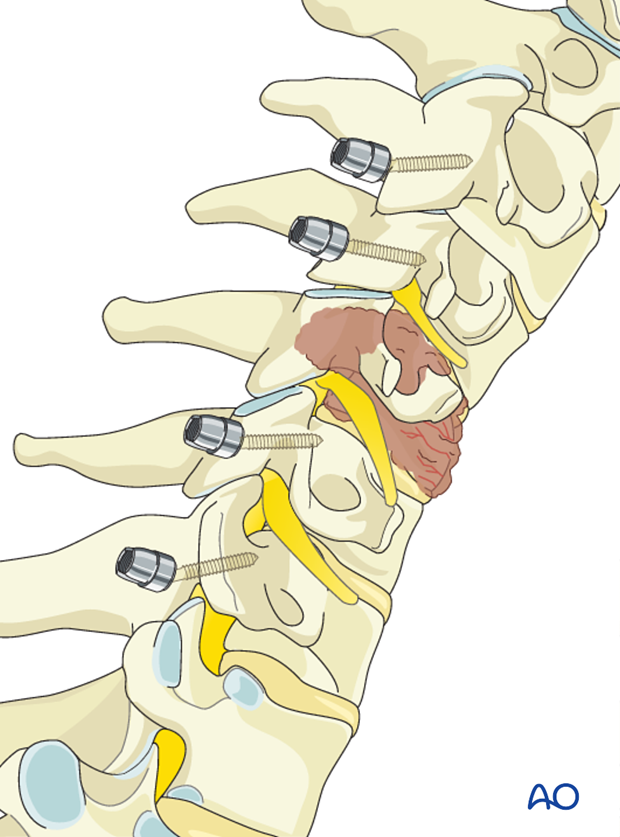
C1 fixation
If C1 instrumentation is indicated lateral mass screws are used.
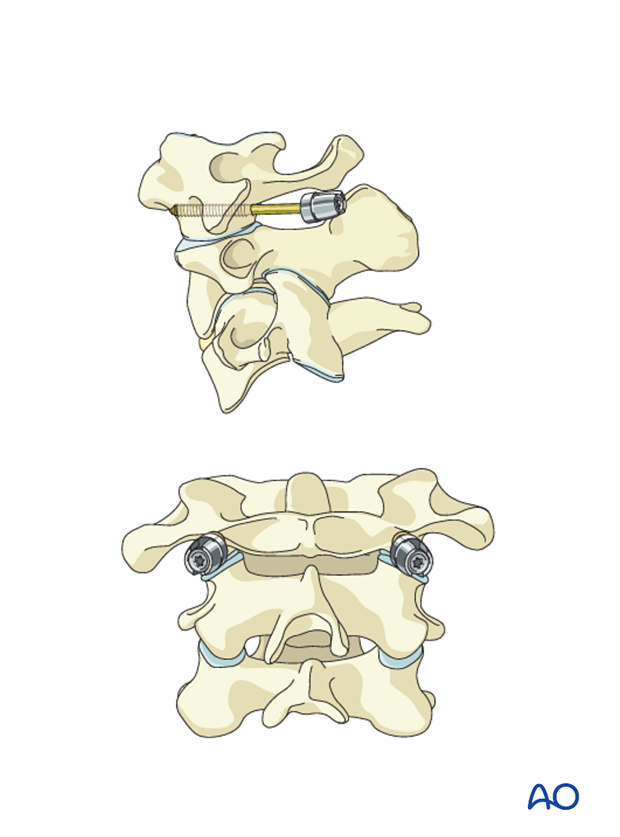
C2 fixation
For C2 fixation the following options are available (in order of preference):
A consideration is given to use pedicle or laminar screws when doing an occiput to C2 fusion as oftentimes the starting point for the pars screws may compromise the facet joint.
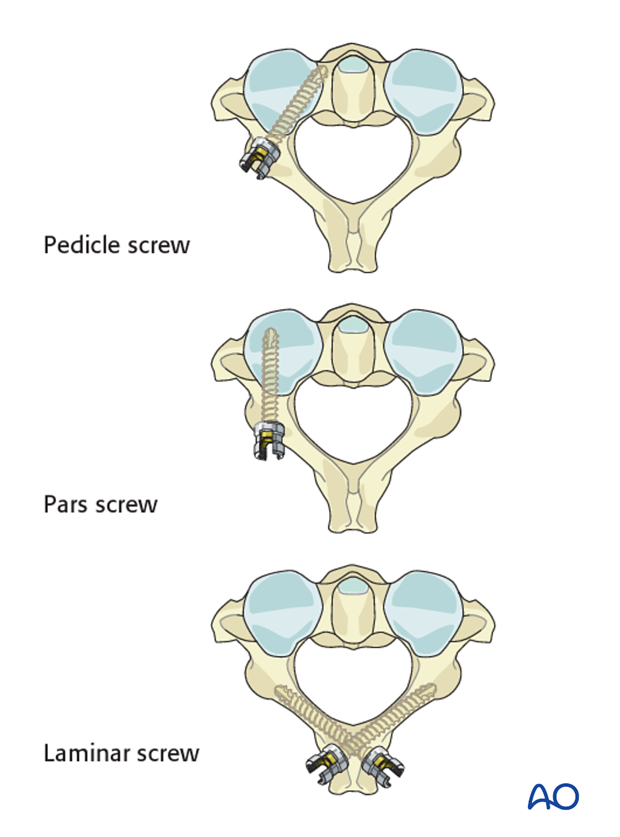
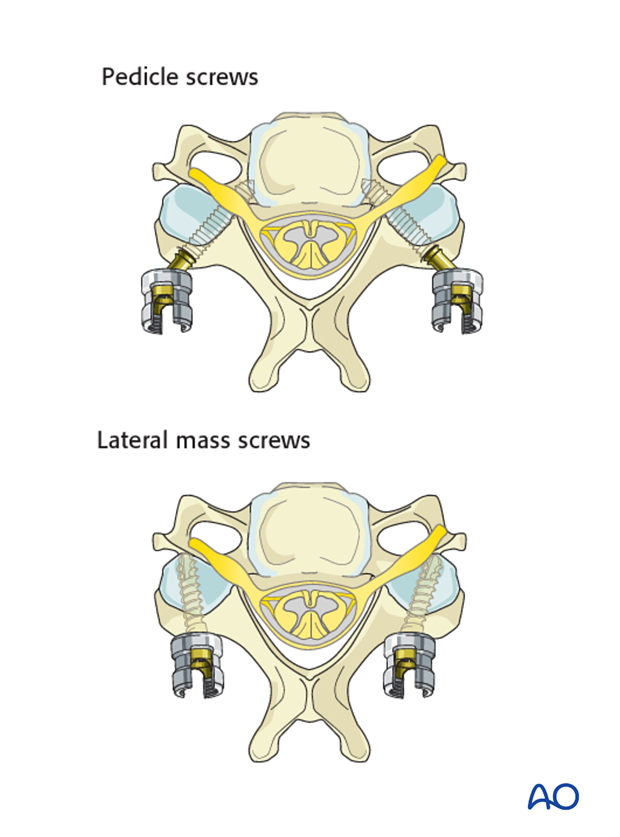
Lateral mass screws vs. pedicle screws C3-C7
Fixation can be achieved with either lateral mass screws, pedicle screws or combination of the two.
Because lateral mass fixation is generally sufficient, and carries less risk, pedicle screw fixation is limited to rare cases where lateral mass fixation would be insufficient or not possible. A pedicle screw is most often used in C7 if instrumented.
4. Rod insertion
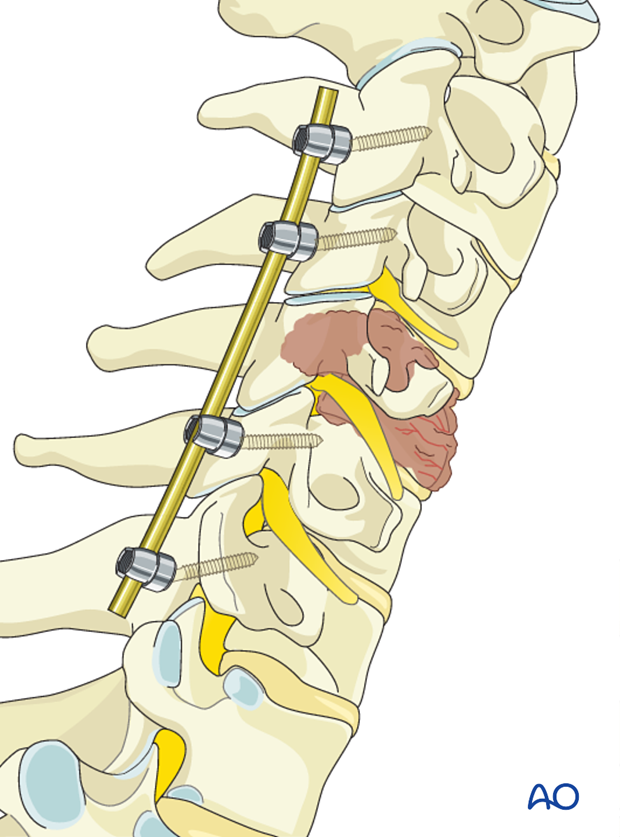
The rod should be bent to align with the lordosis achieved during positioning.
The rod is inserted into the screw heads and the screw heads are tightened with the inner nuts.
If posterior decompression is performed, only one rod is inserted to facilitate access to the spinal canal.
For non-fusion surgeries, consideration should be given to using large diameter rods (4.0 mm) to prevent rod fracture.
5. Decompression
Timing of decompression
A patient who is experiencing neurologic deficit from solid tumor ESCC resulting in loss in ability to ambulate, in the absence of medical and oncological contraindications, requires urgent surgical decompression.
Expeditious diagnosis and prompt surgery are recommended to improve the probability of neurological recovery.
Technique
A laminectomy is performed in the area between the pedicles of the vertebra.
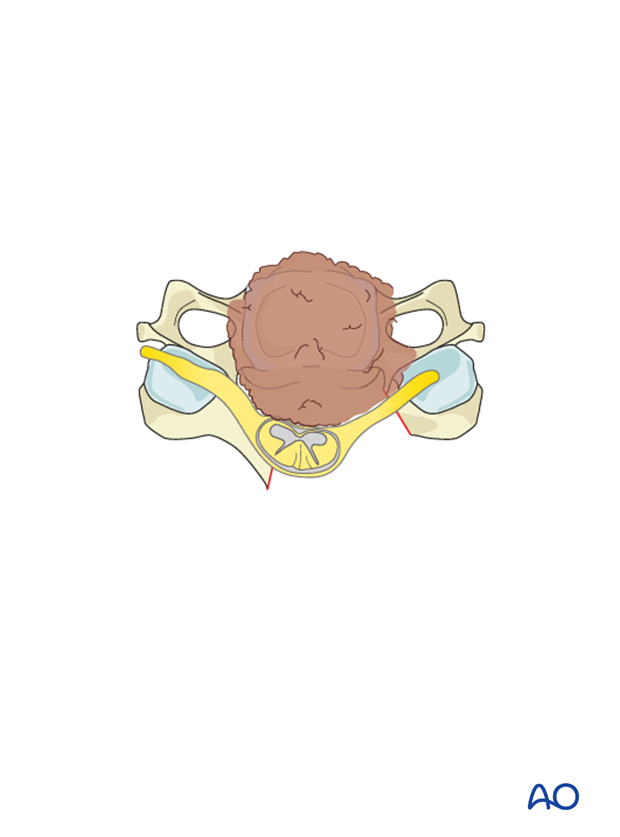
Excise the adjacent spinous processes and the intervening ligamentum flavum.
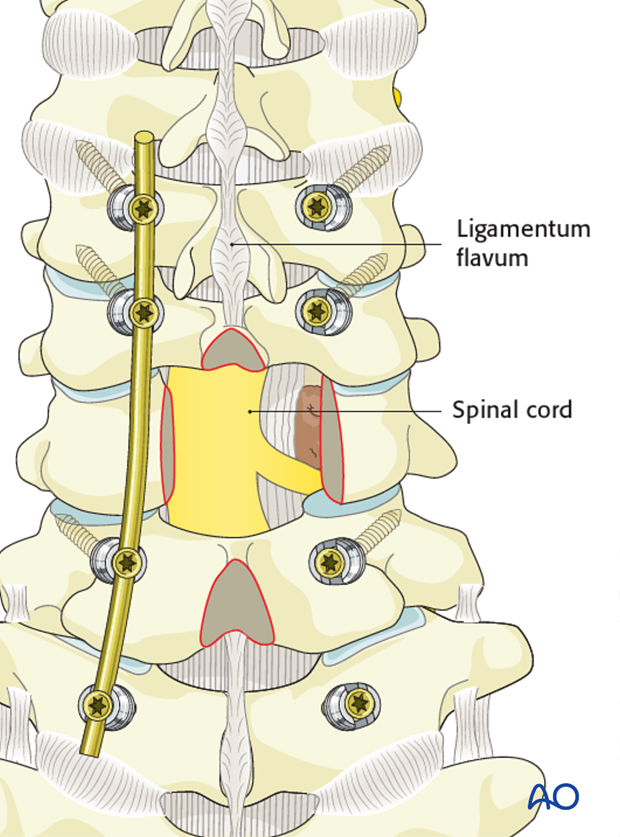
Remove the superior and inferior lamina, and the medial portion of the facet joint.
Based on preoperative planning, the amount of lamina to be removed to achieve enough decompression can be determined beforehand.
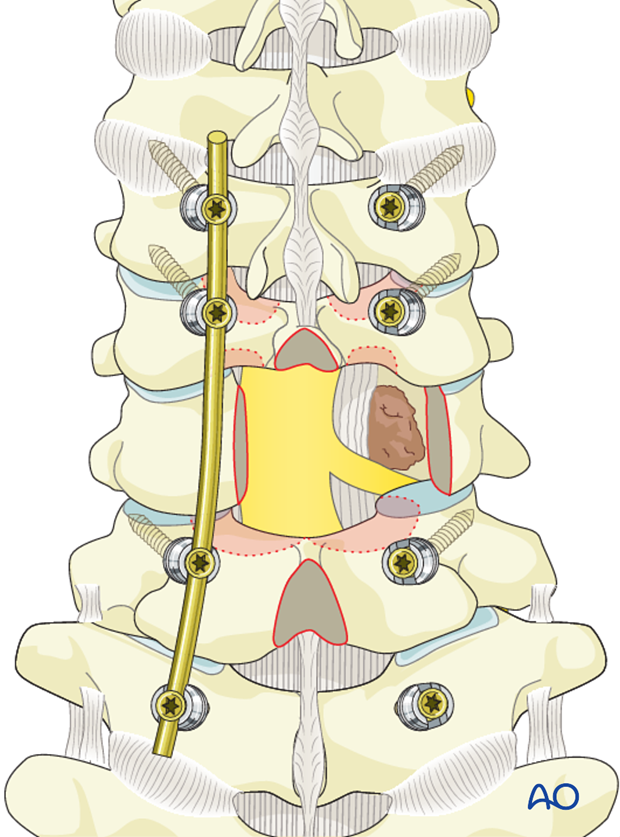
The posterior longitudinal ligament (PLL) should be identified and separated from the dura using a dura dissector.
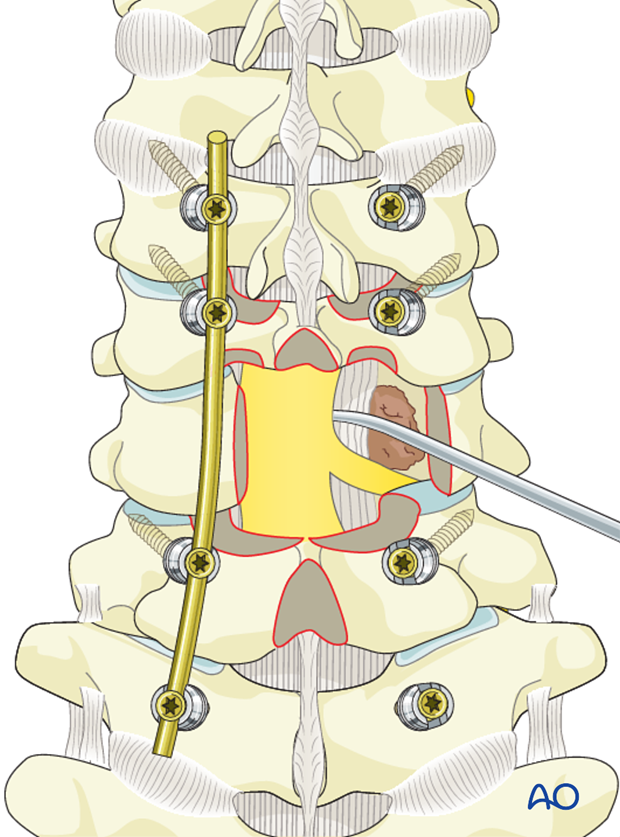
The PLL should be cut to expose the vertebral body and the epidural tumor.
This circumferential spinal cord decompression technique coupled with postoperative SBRT is known as separation surgery.
The spinal cord, dura, and tumor should be manipulated as little as possible.
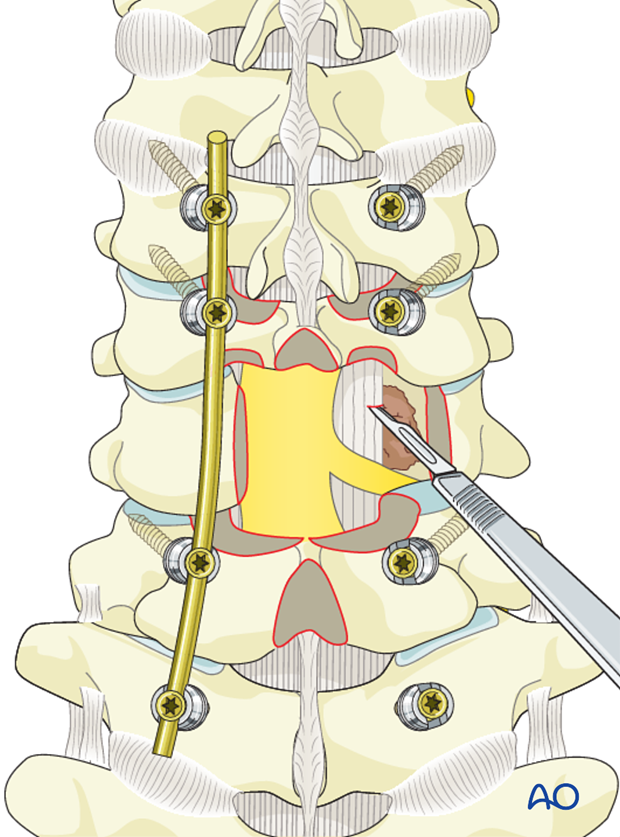
Reverse-angle curettes and pituitary rongeurs can be inserted through this opening, and any tumor and bone fragments compressing the anterior neural elements can be removed or impacted into the vertebral body.
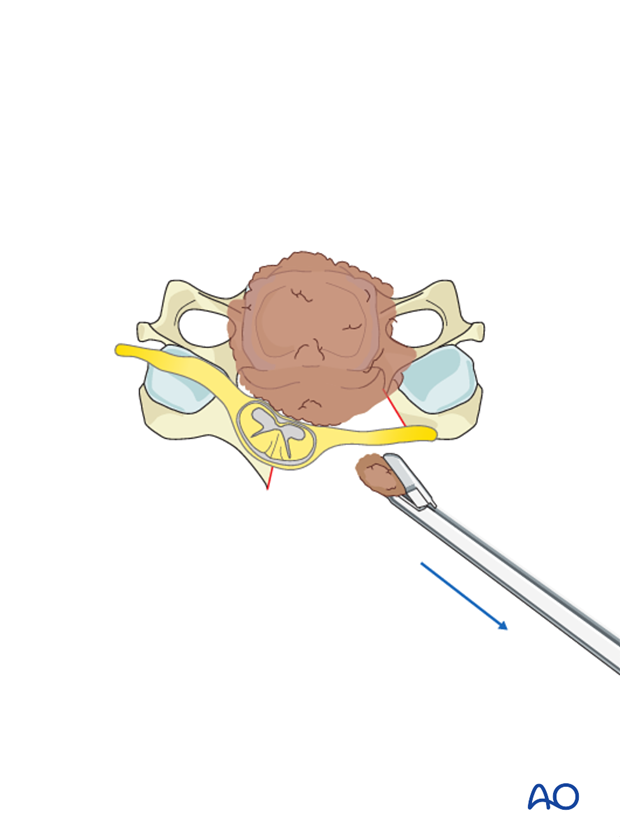
If further decompression is needed, the same technique may be applied on the other side.
If the decompression is adequate on both sides of the canal, the second rod may be inserted and tightened.
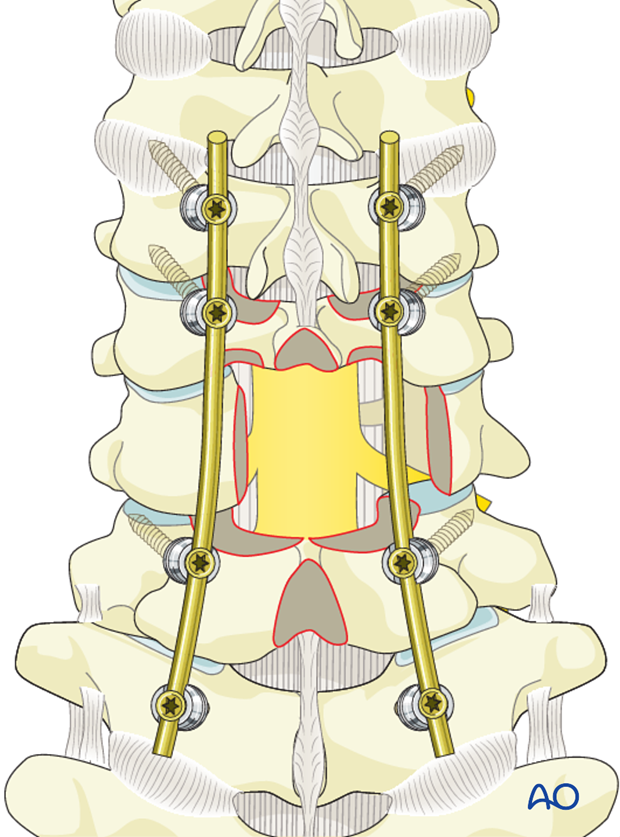
6. Fusion
Life expectancy and performance status should be used to determine whether bone grafting is indicated.
For patients with good prognosis and a long life-expectancy, posterior fusion may optionally be performed using allograft and/or local autograft.
The facet capsule is excised, and the joint cartilage surfaces are denuded/curetted.
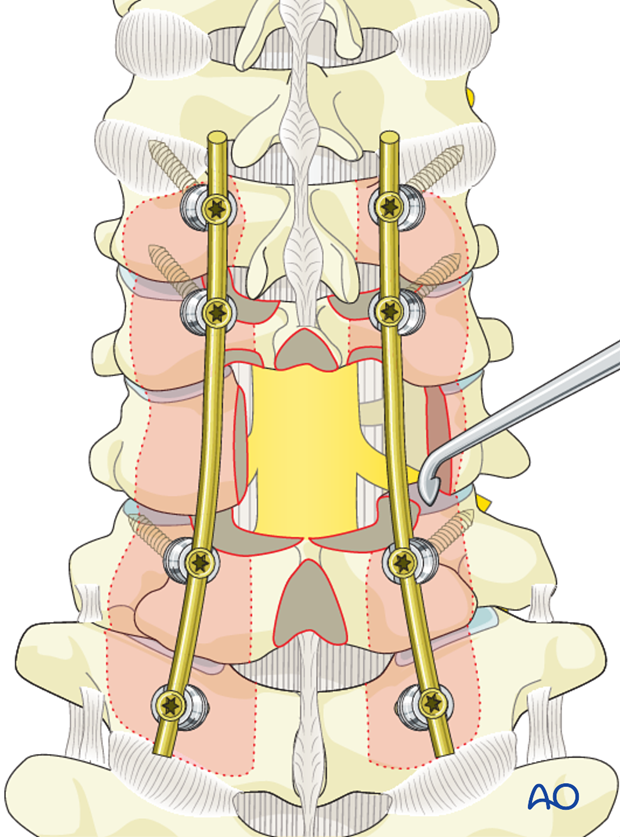
Pieces of bone graft (autograft, allograft) are inserted into the decorticated facet joint for fusion.
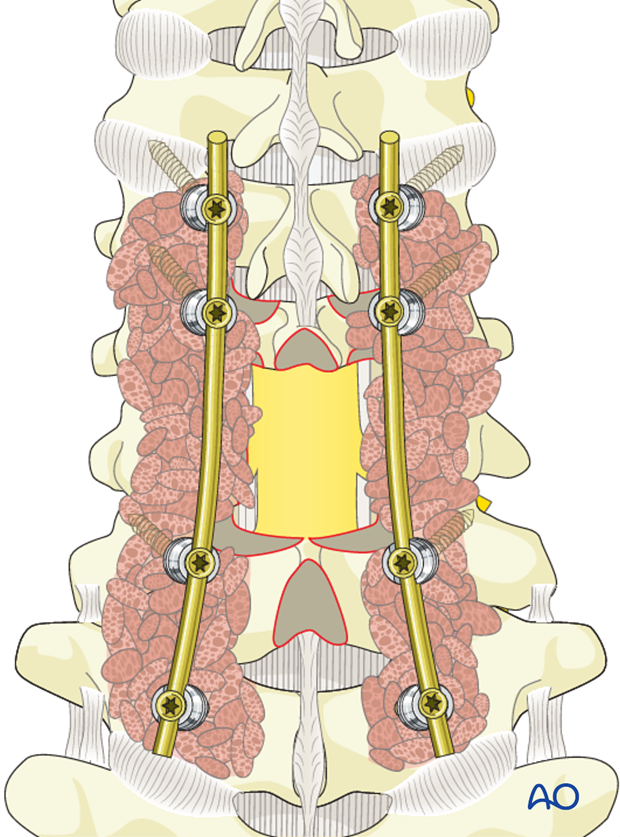
7. Aftercare
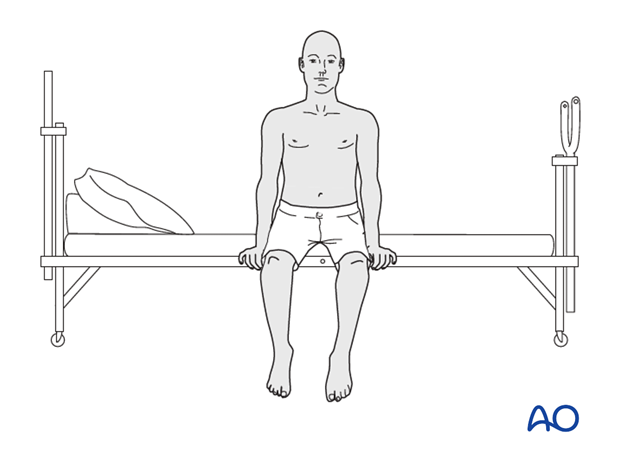
Patients are made to sit up in the bed on the first day after surgery. Bracing is optional but preferably omitted for patient comfort. Patients with intact neurological status are made to stand and walk on the first day after surgery.
Patients can be discharged when medically stable or sent to a rehabilitation center if further care is necessary.
During admission adequate caloric intake of a high-quality diet should be monitored.
Patients are generally followed with periodical x-rays and (optionally) MR imaging at 6 weeks, 3 months, 6 months, and 1 year to monitor for tumor recurrence and hardware failure.
Postoperative radiation is required to avoid tumor recurrence. SBRT is usually initiated within two weeks following surgery. Conventional radiotherapy is usually initiated 2-4 weeks after surgery to reduce the risk of wound healing disturbances.
The radiation modality is selected based on tumor histology and history of prior radiation.













