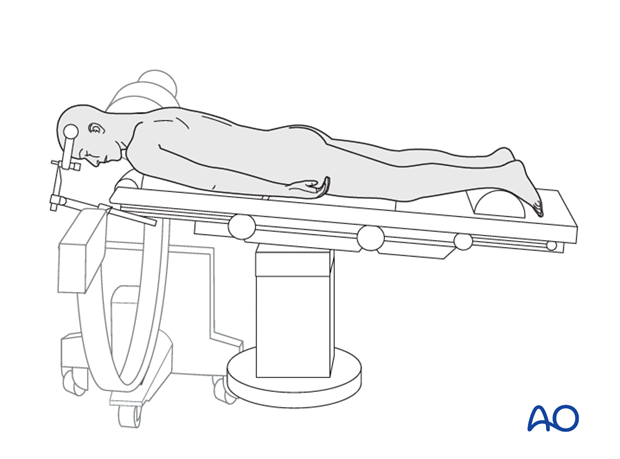
Prone for C0-C7
1. Positioning
The patient is anaesthetized and intubated while taking care to keep the unstable cervical spine immobilized.
The head may be attached to a Mayfield clamp, or a halo-vest or other immobilizing device may be used.
When using a Mayfield clamp select the pin entry points such that the clamp can be rotated freely over the nose once the patient is put into the prone position.
Make sure that there are adequate personnel to safely receive and turn the patient from supine to prone position on a preferably radiolucent operating table.
In patients with unstable tumors, who are at risk for neurological deterioration during positioning, base line electrodiagnostic signals can be obtained to allow for comparison after positioning. Other options in high risk patients include awake positioning or a wakeup test after positioning.
Using a ‘spinal cord at risk’ protocol is recommended in cases where intraoperative neurological deterioration is expected.
The patient is placed on two horizontal padded bolsters (one at the level of sternum and one at the level of anterior iliac spine) or a frame. Designated radiolucent spine surgery frames with similar supports are ideal.
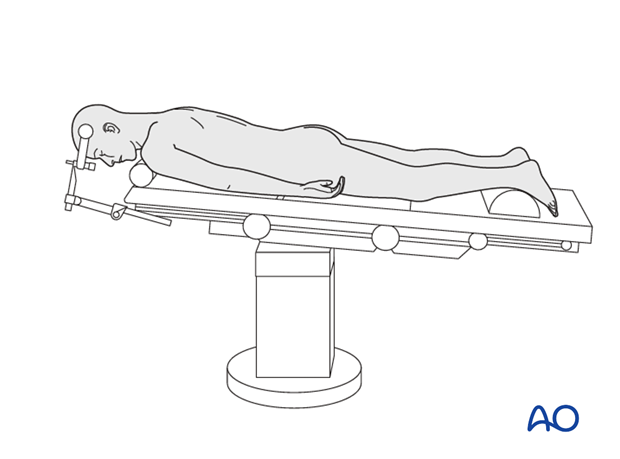
2. Anesthesia
With highly unstable cervical tumors, either an awake or fiberoptic intubation should be considered. In patients with severe spinal cord compression, it is essential to avoid hypotensive anesthesia and the mean arterial blood pressure should be maintained above 80 mmHg.
3. Preoperative antibiotics
Antibiotics should be administered 30-60 min prior to the incision.
A cephalosporin antibiotic with good gram positive coverage is generally recommended.
4. Spinal cord monitoring
Spinal cord monitoring is optional.
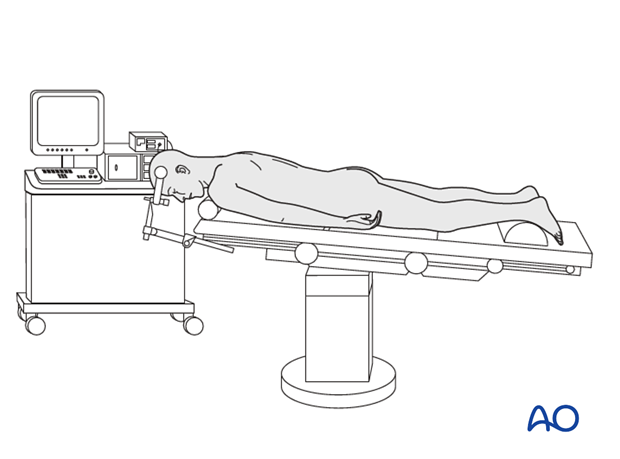
5. Fluoroscopy/x-ray control
The incision can be planned based on the lateral fluoroscopic view.