Open reduction; K-wire fixation
1. Introduction
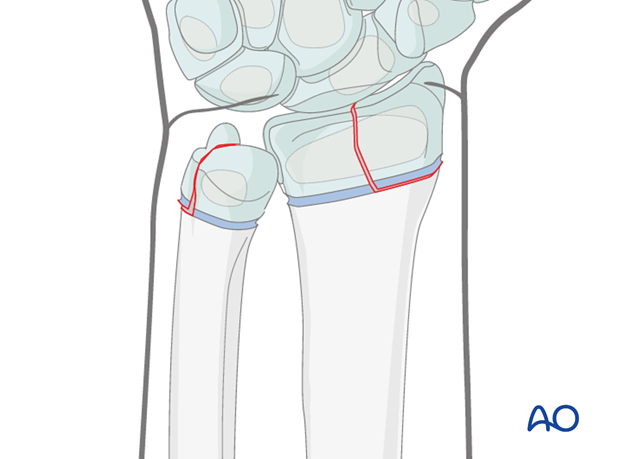
These are intraarticular fractures and the adult principles of anatomical reduction and stable fixation are also relevant in children.
If closed reduction, with or without the assistance of a percutaneous K-wire, is unsuccessful, open reduction is required.
Impediments to closed reduction include pronator quadratus and/or periosteum in radial injuries and the ulnar nerve and adjacent tendons in ulnar injuries.
In younger children, fixation can be achieved using a K-wire. A lag screw, totally within the radial epiphysis, can be used as an alternative near skeletal maturity when the epiphysis is largely ossified.
Preoperative CT imaging is desirable to determine the exact anatomy of the fracture and, therefore, the correct orientation of any intraepiphyseal implant.
2. Patient preparation
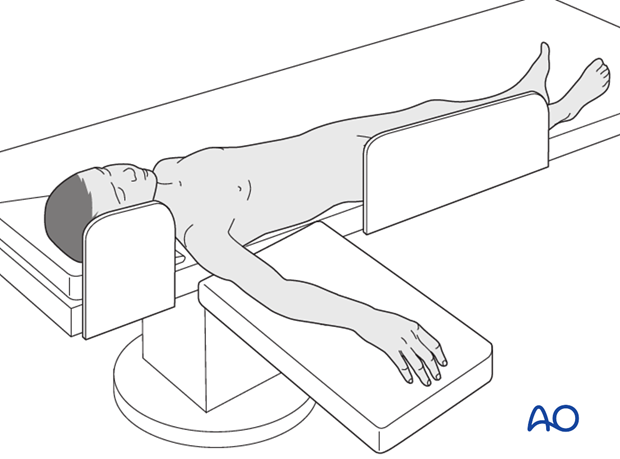
This procedure is normally performed with the patient in a supine position.
3. Approach
Volar (anterior) approach
For this procedure a volar (anterior) approach is normally used.
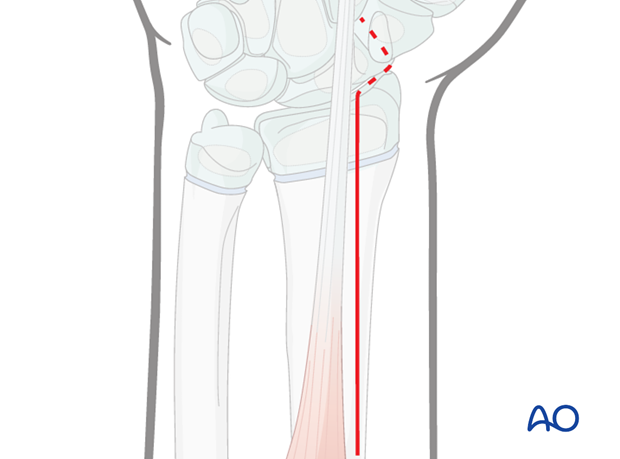
Anatomy to the distal forearm
A thorough knowledge of the anatomy of the wrist is essential.
The additional material gives a short introduction.

4. Open reduction
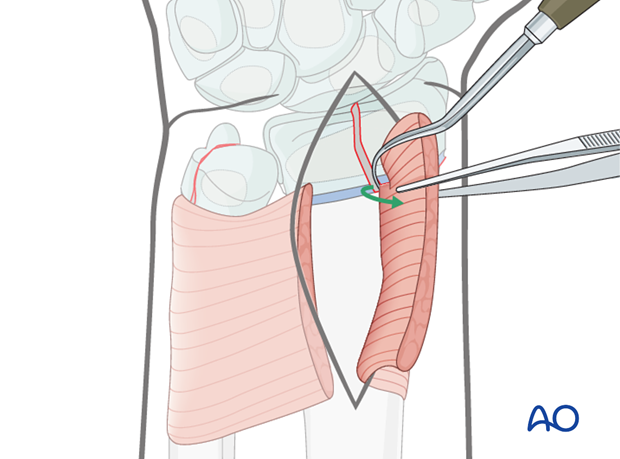
Removal of impediments
Soft tissue impediments to reduction are removed.
Reduction
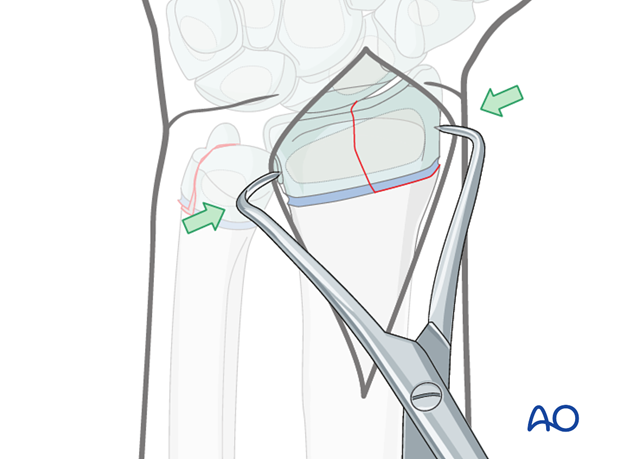
After soft tissue impediments have been removed, the fracture will generally reduce directly using a small pointed reduction clamp.
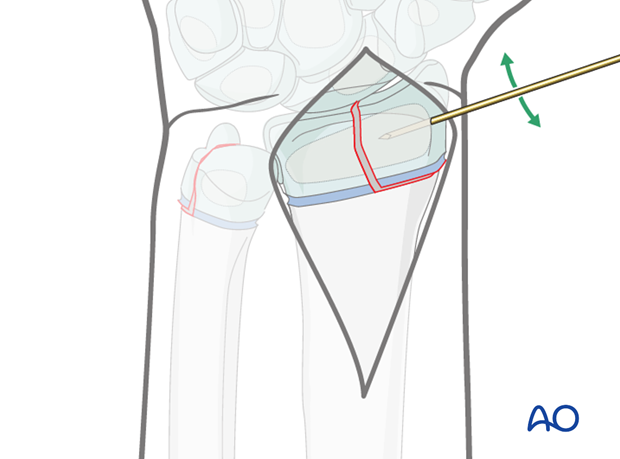
Reduction with the help of a K-wire
A single K-wire can be inserted into the epiphyseal fragment and used as a joystick to facilitate reduction.
If this wire is inserted in the direction of the proposed definitive fixation, it can then be advanced across the fracture after reduction has been secured.
5. K-wire fixation
Skin incision
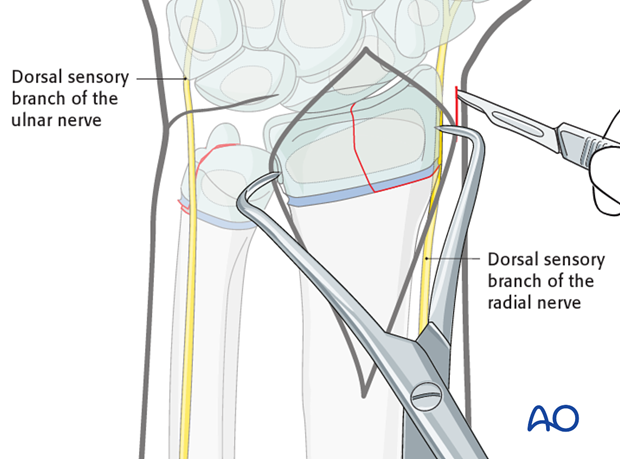
A small skin incision is made for the K-wire insertion.
This incision is deepened to the bone using a blunt artery forceps and a protective sleeve is inserted.
Care should be taken to avoid the dorsal sensory branch of the radial nerve and the dorsal sensory branch of the ulnar nerve.
Insertion of the intraepiphyseal K-wire
A smooth 1.25-1.6 mm K-wire is inserted through the radial epiphysis in a direction determined by the fracture pattern. The K-wire should ideally cross the fracture plane as near to 90° as the fracture anatomy permits.
The wire should be inserted with an oscillating drill and cooled with saline solution to prevent thermal injury.
The wire may also be inserted by hand using a T-handle.
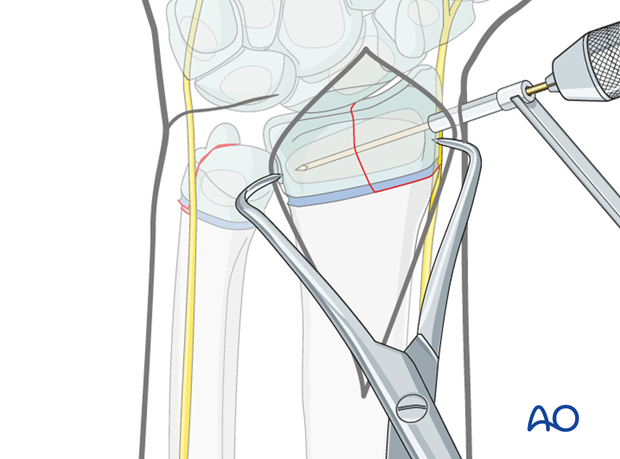
Ideally, the K-wire is inserted using image intensifier control, in order to check the trajectory of the wire.
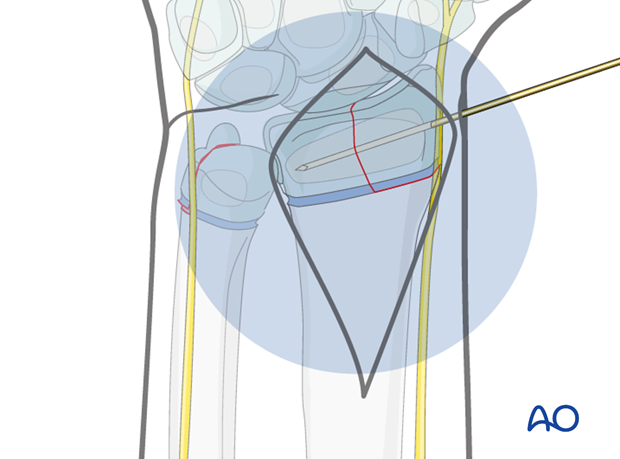
Alternative: Cannulated screw
In the child nearing skeletal maturity an intra epiphyseal lag screw can be inserted. Using the intraepiphyseal wire as a guide, a cannulated screw is inserted over the wire with the appropriate soft-tissue protection, provided the full instrumentation is available.
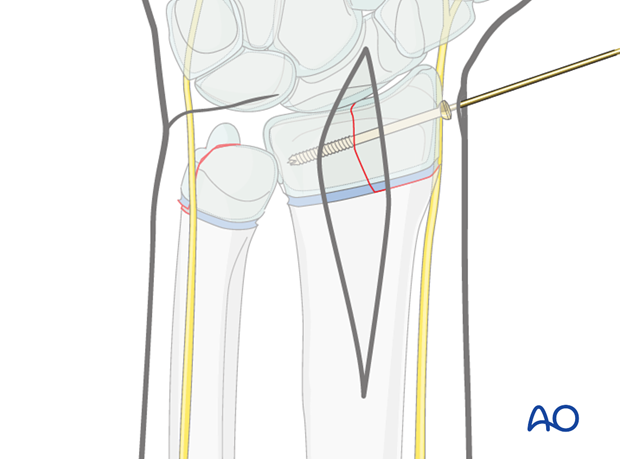
Insertion of a second K-wire
Occasionally a second wire is required to maintain the reduction.
This wire is inserted obliquely through the radial epiphysis, across the physis and engaging the medial cortex of the radial metaphysis.
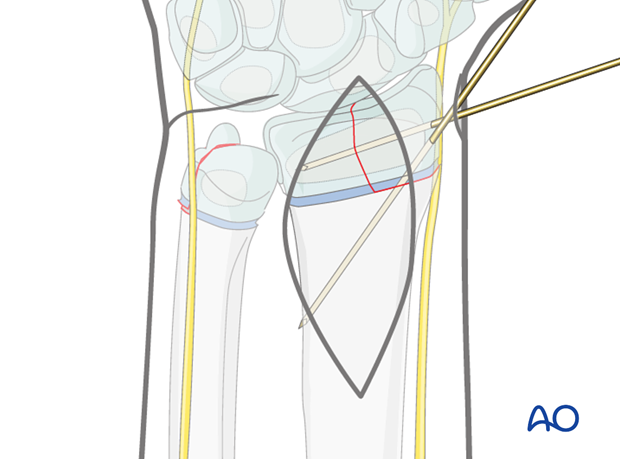
Stabilization of the ulna
An oblique wire is used to stabilize the ulna using similar principles.
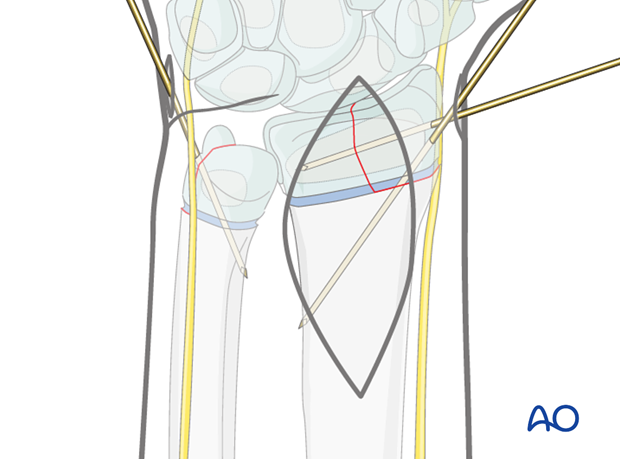
Confirmation of reduction
Ideally, reduction should be confirmed using image intensification, or arthrography.
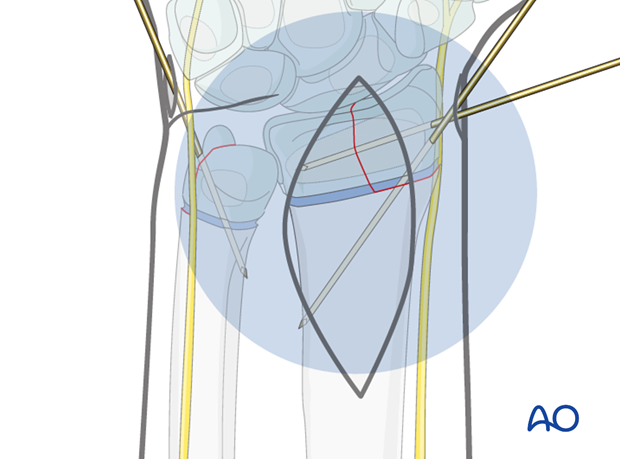
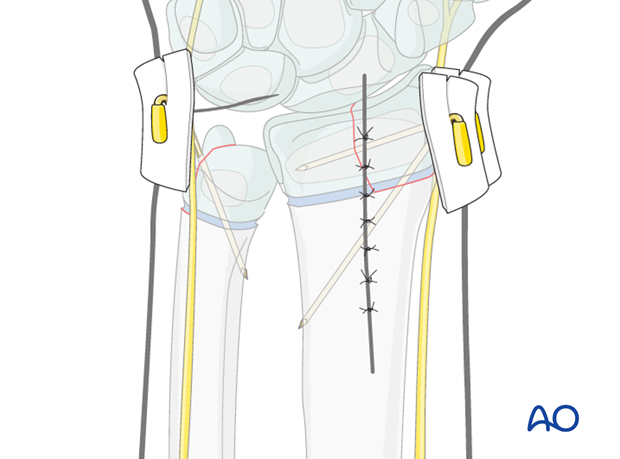
The K-wires are left protruding through the skin, bent and cut. The skin is protected with sterile padding prior to application of a cast.
The illustration demonstrates the use of a small section of plastic tubing over the cut ends of the protruding wire. This adds further protection for the skin.
Note: Excessive pressure between dressing and skin should be avoided to prevent skin necrosis.
6. Short arm cast
General considerations
The purpose of the cast is protective and for pain relief, as stability is provided by the K-wire(s).
The short arm cast is applied according to standard procedure:
Note: In young, small, or noncompliant patients, it is safer to apply a long arm cast.
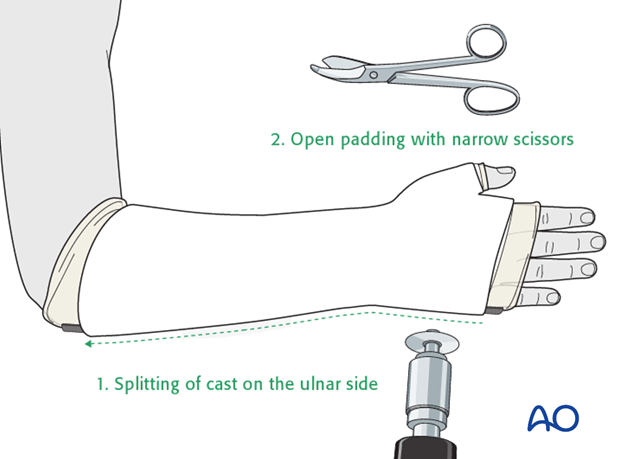
Splitting of cast
If a complete cast is applied in the acute phase after injury, it is safer to split the cast down to skin over its full length.
7. Long arm cast
In the event that a long arm cast is necessary (see above) it is applied and split according to standard procedure.
8. Aftercare
Tight cast
Further swelling in a restricting cast can cause pain, venous congestion in the fingers and occasionally a compartment syndrome.
For this reason any complete cast applied in acute phase should be split down to skin.
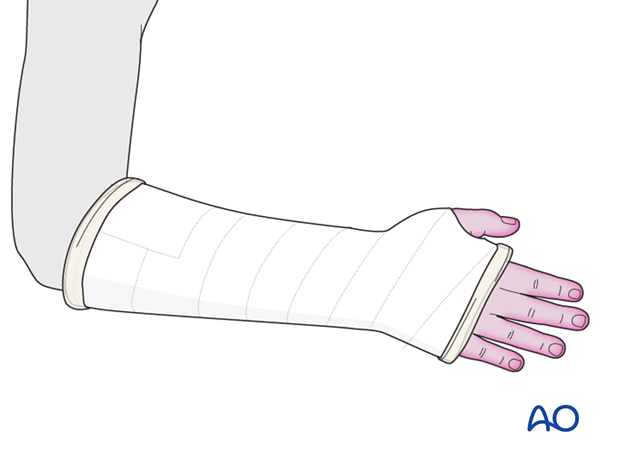
Parents/carers should be instructed how to detect circulatory problems by pressing and releasing the fingertips and watching if the blood flow/color returns to normal (capillary refill), compared to the opposite hand.
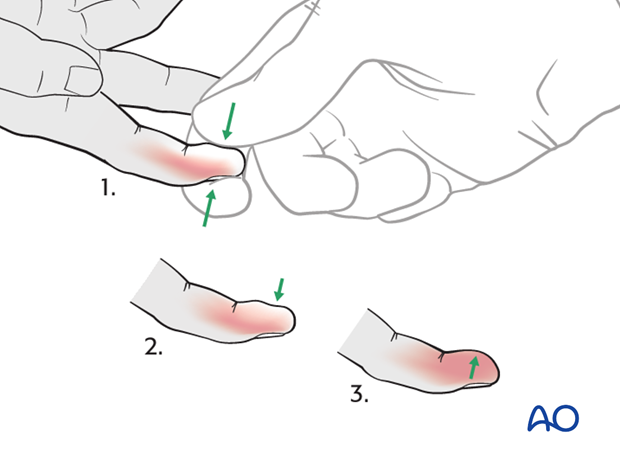
Compartment syndrome
Compartment syndrome is an unusual but serious complication after the application of a complete cast and can be difficult to diagnose, especially in younger children. Neurological signs appear late and the main sign is excessive pain on passive extension of the fingers.
It is important to make sure that the parents/carers are aware of the risk of compartment syndrome.
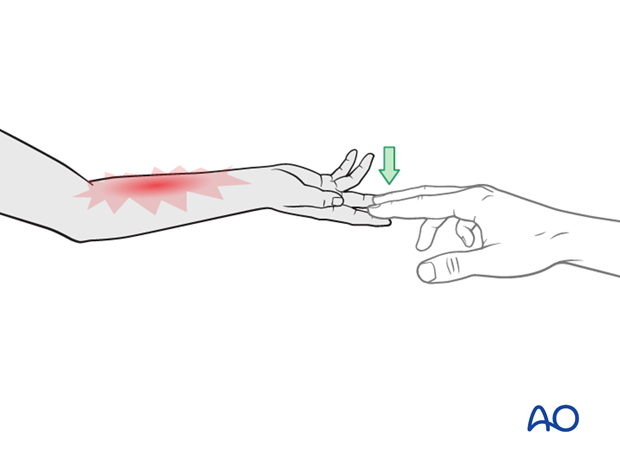
The parents/carers and patient should be informed to take note of increased pain and/or unresponsiveness to normal painkillers.
They should know that this may indicate serious complications. It is important for them to detect these signs as early as possible and report them urgently to the surgeon/nurse by telephone, or to attend the Emergency Room (ER) without delay.
Nerve compression is an occasional complication and the signs include:
- Sensory deficits (numbness)
- Weakness of active finger movement
- Paresthesia
Infections
See also the additional material on postoperative infections.
Cast care
If a normal plaster of Paris cast is used, it is important to keep the cast clean and dry in order to maintain the reduction.
When the swelling has reduced, the cast can become loose. The loss of support can result in loss of reduction.
In this circumstance, the parents/carers are advised to return to the healthcare provider.
Follow-up x-rays
Depending on the fracture pattern, the age of the child and the method of treatment, the patient has to return for follow-up x-rays to monitor the fracture position.
X-rays taken for fracture position can be taken with cast in place. Any x-rays to assess the state of bone healing must be taken without the cast and correlated with clinical examination.
In most cases, it is conventional to obtain follow-up x-rays after reduction to ensure that the position is maintained.
In general, in the child below 5 years of age, the follow-up is usually about 4-5 days after reduction. In the older child with a potentially unstable fracture, an x-ray would normally be taken at 7-10 days.
Further follow-up x-ray is a matter of clinical judgement, the responsibility of the treating surgeon, and tends to be longer in older children (see also Healing times).
For complete fractures of the metaphysis, redisplacement after reduction is not uncommon. It is therefore, important to take early follow-up x-rays in order to detect a possible redisplacement.
See also the additional material on posttraumatic growth disturbances.
K-wire removal
The K-wires can be removed without sedation in the clinic after approximately 3 weeks (depending on the age of the child).













