ORIF - Lag screw fixation
1. Principles/Introduction
In a multifragmentary fracture of the glenoid fossa, the small fragments are often too small to fix with the standard 3.5 conventional/cannulated screws. Typically, the following mini-fragment screws are then used:
- Conventional 2.0 or 2.7 lag screws
- Headless 2.4 screws (cannulated)
Headless screws are preferable where fixation involves putting them through capsule or labrum.
In addition, they are the smallest cannulated screw system.

2. Patient preparation
Depending on the approach, the patient may be placed in the following positions:
3. Approach
The approach will depend on the fracture pattern.
If the trans-glenoid fracture line run from posterior superior to low anterior or if the fracture line is horizontal, then both the deltopectoral or dorsal approach can be used.
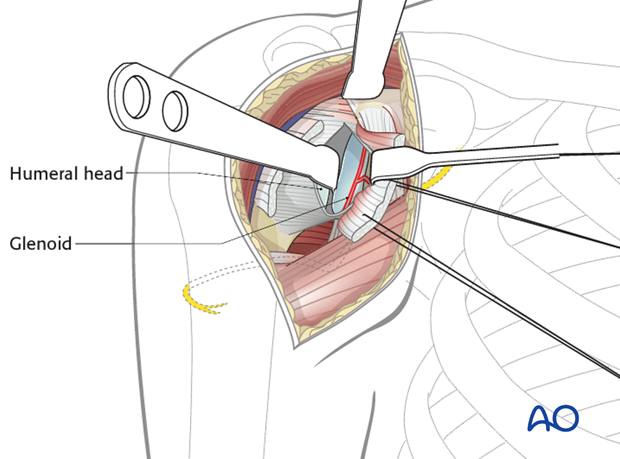
If the fragments are small and lag screw fixation from anterior is not possible, then a posterior approach and fixation is carried out.
4. Reduction
One K-wire is partially inserted in the main fragment and is used as a joystick for reduction. If conventional screws are to be used for fixation, make sure that the fragment is big enough to take the head. Otherwise use the headless screw.
K-wires and screws must be extra articular.
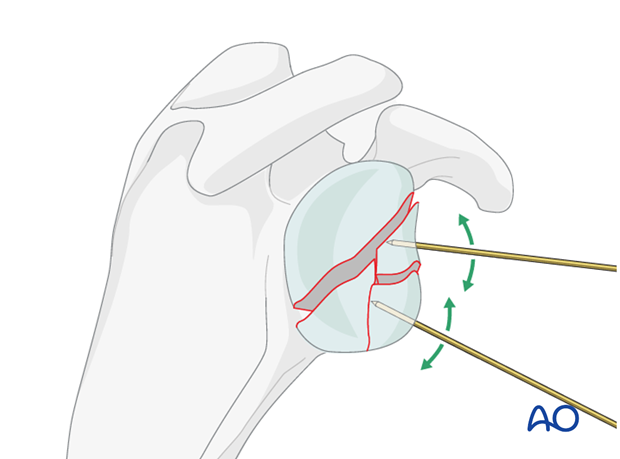
When reduction is completed, insert the K-wires further to secure temporary fixation of the fracture.
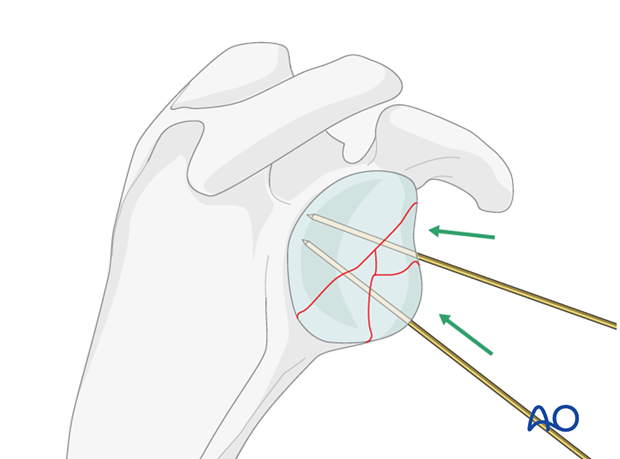
The size of the fragments determines their fixation. At times, if the fragment is very small, a K-wire will serve as its definitive fixation. Otherwise, use either the headless screw or the small fragment cannulated screws.
Depending on the size of the main fragments, one or two appropriate length screws are then inserted…
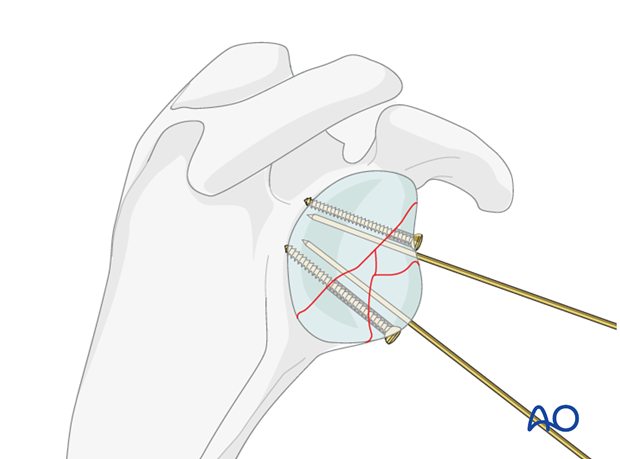
... and the K-wires are removed. Smaller fragments may be keyed into place and held by the larger fragments.
Sometimes one must resort to an anchor if the fragment is very small as well as a small spring plate.
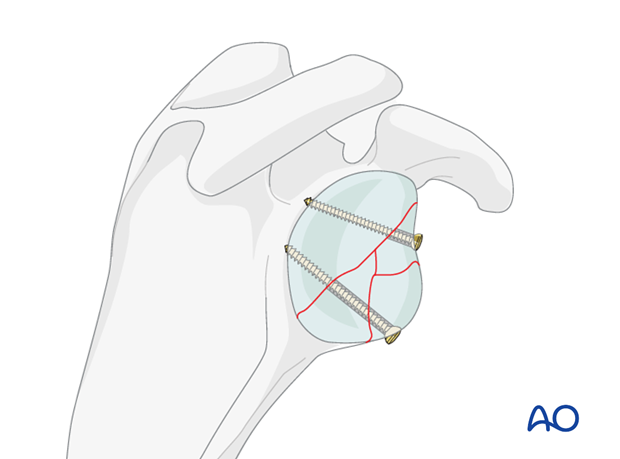
Use the image intensifier to check your reduction prior to any definitive fixation. At the end, check once again with the image intensifier to make sure that there is no intra articular metal.
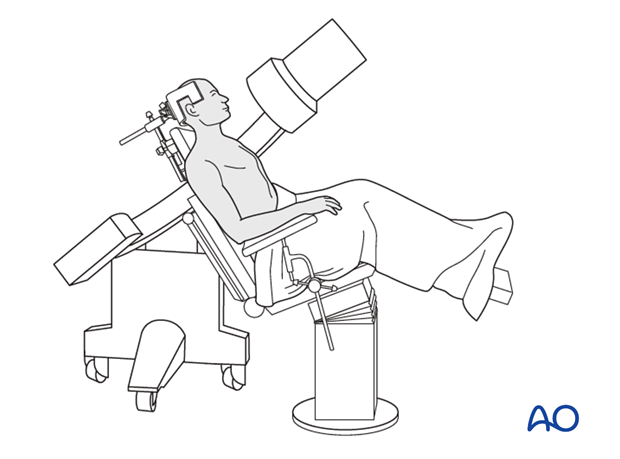
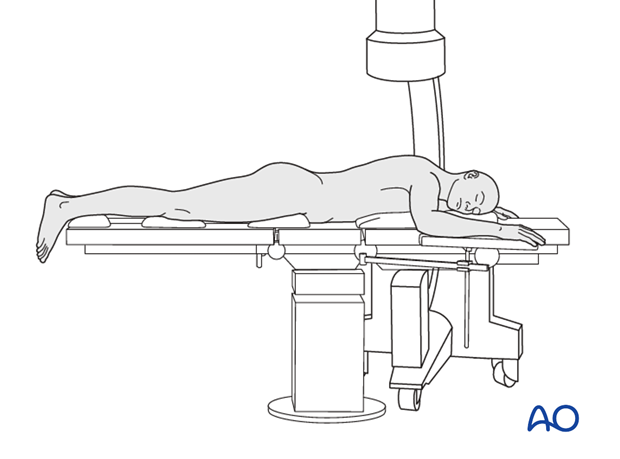
5. Aftercare
The aftercare can be divided into 4 phases:
- Inflammatory phase (week 1–3)
- Early repair phase (week 4–6)
- Late repair and early tissue remodeling phase (week 7–12)
- Remodeling and reintegration phase (week 13 onwards)
Full details on each phase can be found here.













