ORIF - Lag screw fixation
1. Principles/Introduction
Main goal
In this procedure the main goal is to reconstruct the joint surface.
Screw selection
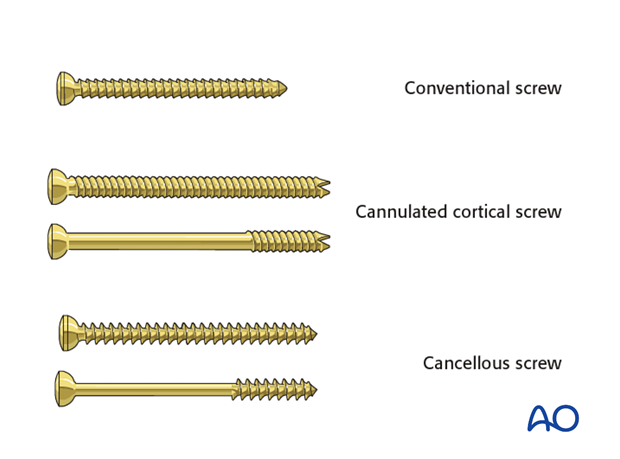
For this procedure the following screws are typically used:
- Conventional 3.5 lag screws
- Cannulated 3.5 lag screws
- Headless 3.0 screws
Headless screws are preferable where fixation involves inserting them through capsule or labrum.
If a headless screw is used, bicortical purchase is preferred but not required for compression.
2. Patient preparation
Depending on the approach, the patient may be placed in the following positions:
3. Approach
An anterior approach to the shoulder joint is easier to perform. It may therefore be easier to fix large posterior fragments through an anterior approach.
In a posterior fracture dislocation, the anterior deltopectoral approach is chosen because it offers better dual opportunities, not only to restore posterior lesions but also allows restoration of humeral head impaction lesions.
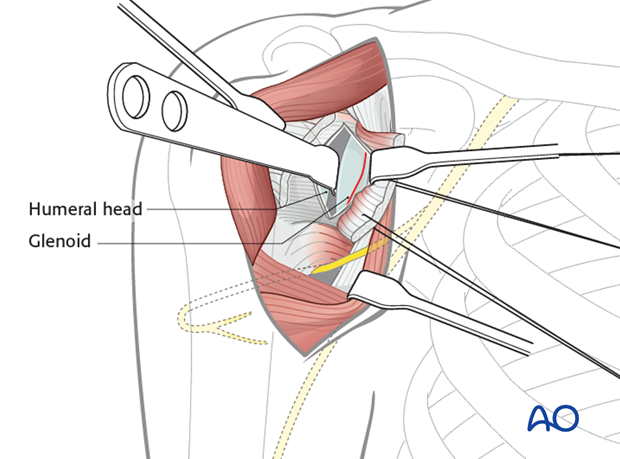
If the fragments are small and lag screw fixation from anterior is not possible, a posterior approach and fixation is carried out.
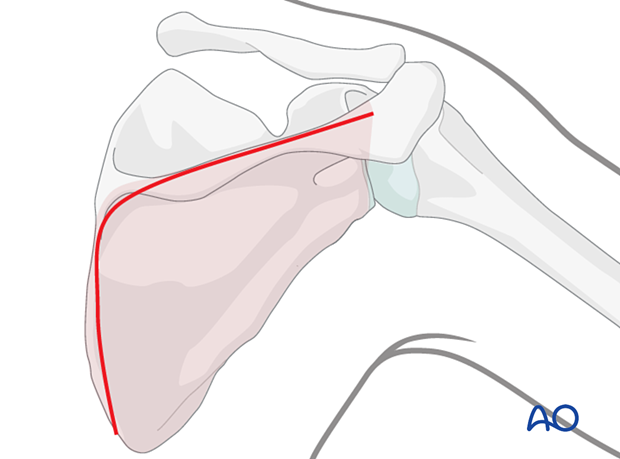
4. Reduction
Reduction of the articular surface may be facilitated by the insertion of a K-wire to be used as joystick. For this reason, we prefer to use the cannulated system and insert the K-wire in such a way that it will subsequently serve as a guide for the lag screw trajectory.
The liquid used for distension should not be under high pressure. If it is under high pressure it will drive the fragments apart and make the reduction difficult.
If a satisfactory reduction cannot be achieved by closed manipulation one must resort to an open reduction and fixation.
Whenever K-wires are used as joysticks, whether as subsequent guide wires or not, they should not be inserted trans articular.
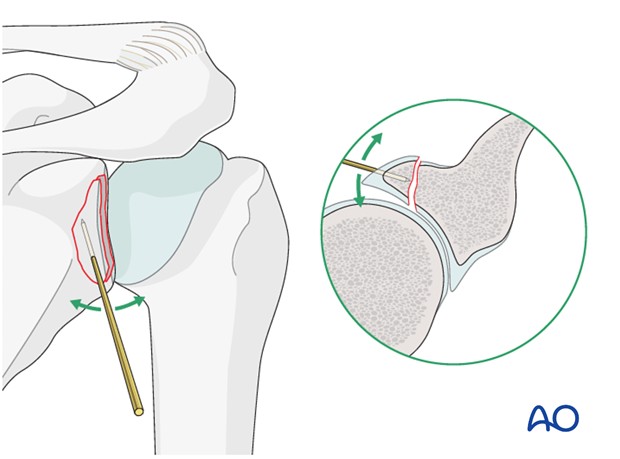
When conventional screws are used for the fixation, care must be taken that the K-wire does not interfere with the planned screw placement.
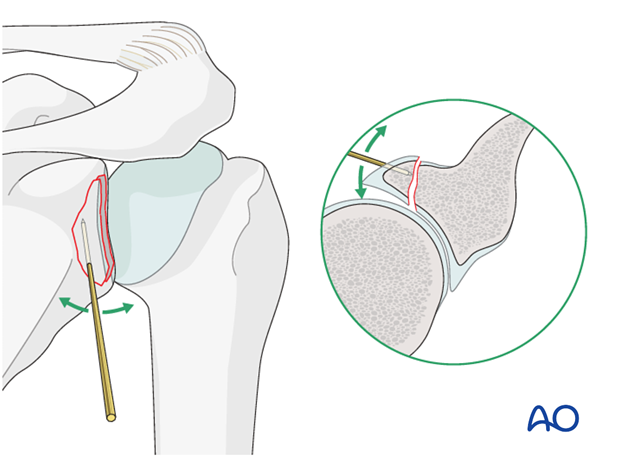
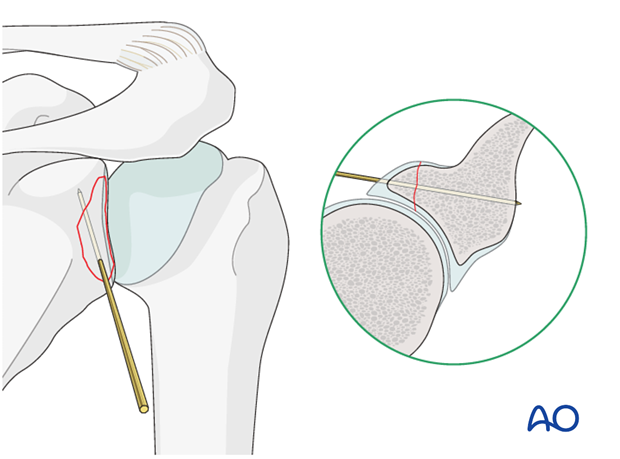
When reduction is completed, the K-wire is further inserted to temporarily fix the fracture.
Make sure that K-wires are not directed into the suprascapular notch where they can compromise the neurovascular bundle.
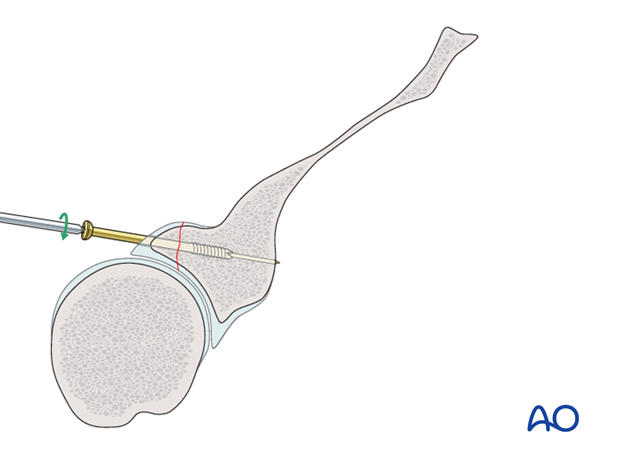
Depending on the size of the fragment, two lag screws are preferred since one does not offer rotational stability.
The K-wires are removed.
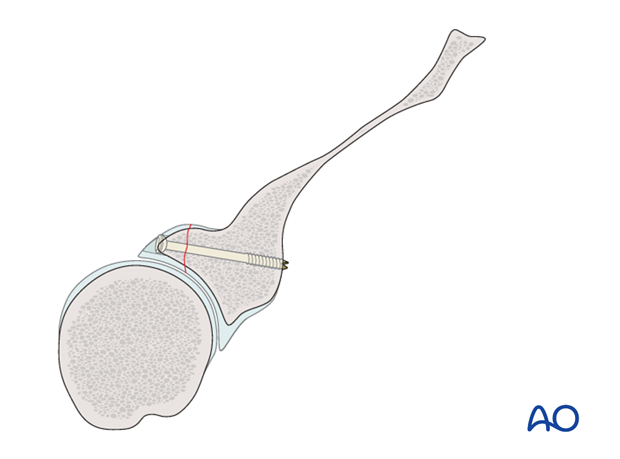
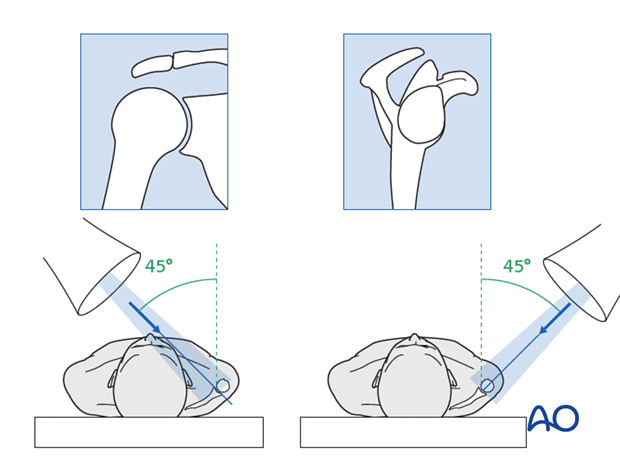
Check the position of the screws and the reduction by image intensification in the standard projections (trans-glenoid and trans scapular view). A 3D-CT scan, if available, is very useful to verify the position of the fixation devices.
5. Aftercare
The aftercare can be divided into 4 phases:
- Inflammatory phase (week 1–3)
- Early repair phase (week 4–6)
- Late repair and early tissue remodeling phase (week 7–12)
- Remodeling and reintegration phase (week 13 onwards)
Full details on each phase can be found here.













