Antiglide plate
1. Principles
The one-third tubular plate, which is placed posterolaterally on the fibula in an anti-glide position, indirectly reduces the fracture and acts as a buttress to resist the posterior and proximal displacement of the distal fragment.
Additionally, when the fracture configuration allows, the fracture can be compressed with a lag screw, inserted through the plate.

Teaching videos
AO teaching video: Type B Malleolar Fracture 44-B (2004)
AO teaching video: Malleolar-Fracture Type B (1988)
2. Patient preparation and approach
The patient may be placed in the following positions:
For this procedure a lateral approach is normally used.
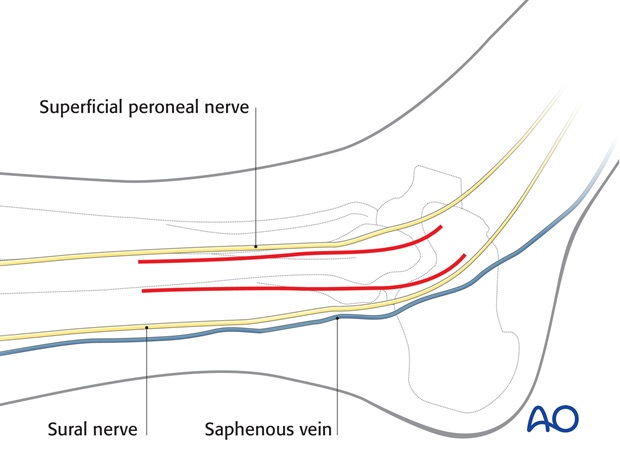
3. Preliminary reduction
Preparation of the fracture site
Remove any minor bone fragments which are blocking reduction. Do not strip the periosteum more than necessary.
Preliminary reduction before plate application
Reduce the fracture by applying light longitudinal traction and rotating the foot internally.
Optionally, small pointed reduction forceps can be used.

4. Plate preparation
Bending the plate
Prepare a four-hole one-third tubular plate. To improve the anti-glide buttressing effect, the plate is slightly bent at its distal end.
The central section of the plate is left straight so that when the central screw is tightened, it will pull the plate against the bone. This applies posterior compression on the distal fragment, which augments compression across the fracture plane.

Planning the plate position
Accurate positioning of the plate is essential in obtaining the buttress effect and allowing the insertion of a lag screw. The proximal hole closest to the fracture site should be located 3-5 mm proximal to the fracture line.
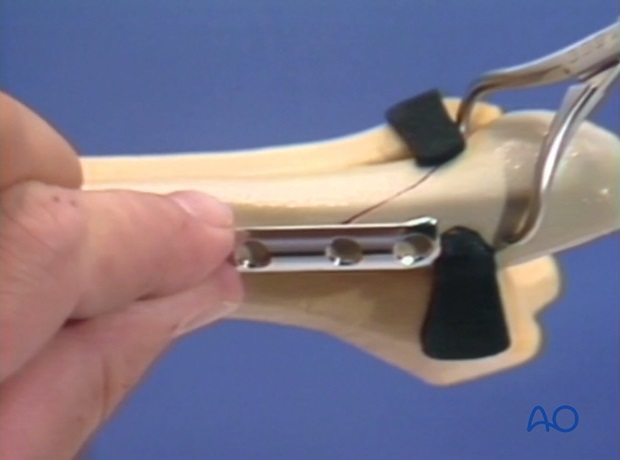
5. Fixation
Drilling
Reduce the main fragments and hold with a pointed reduction forceps.
Either make sure the position of the forceps allows the plate to lie in the correct position, or alternatively, place the forceps through the hole in the plate before tightening the forceps.
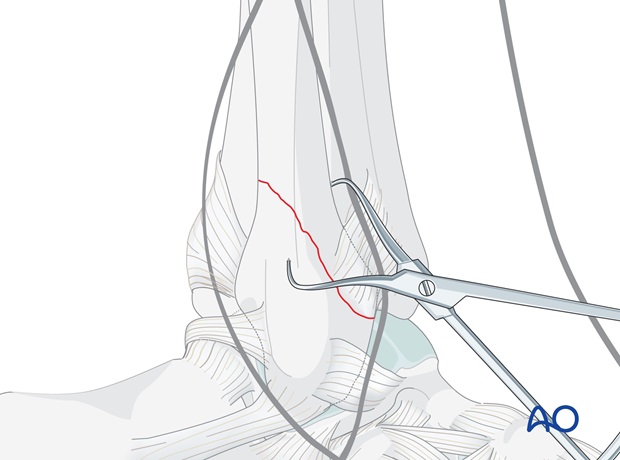
In the proximal fibular fragment, drill a 2.5 mm hole through both cortices, from posterior to anterior, 3-5 mm proximal to the apex of the fracture.
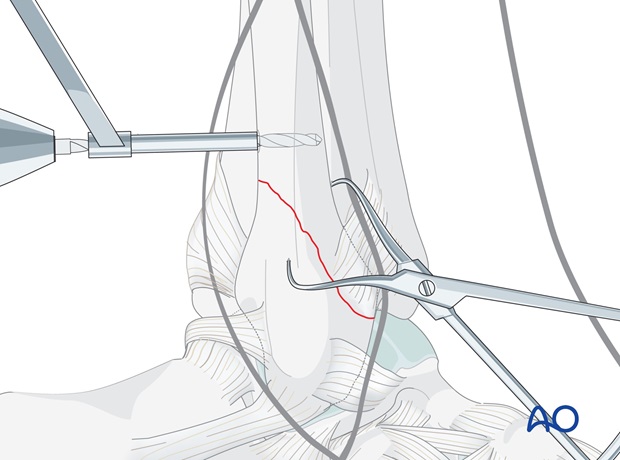
Plate application
Carefully position the plate so that two holes overlie each fragment, and hold it in place with a finger.
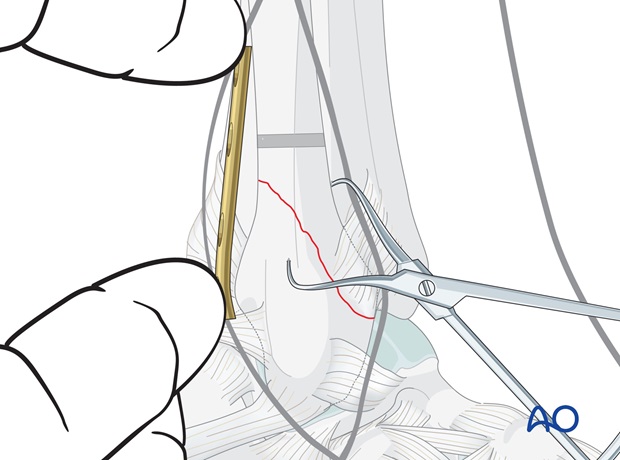
Insertion of the first proximal screw
Measure the length of the drilled hole through the plate.
Tap with the 3.5 mm cortical tap and insert the first 3.5 mm cortex screw.
Check reduction visually and under image intensification.
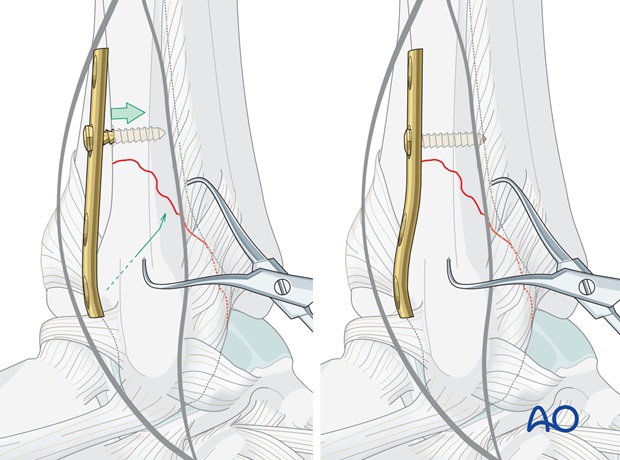
Insertion of the second proximal screw
Insert the second screw through the most proximal plate hole, drilling, measuring and tapping through the plate hole.
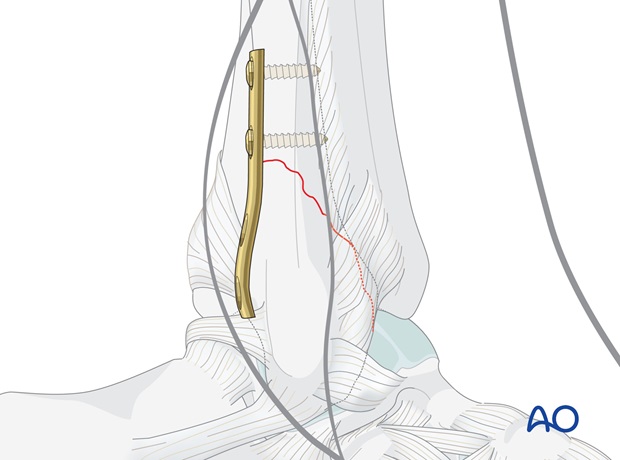
Prepare insertion of a lag screw
Drill a gliding hole in the near cortex, through the plate hole closest and just distal to the fracture, using a 3.5 mm drill bit. The hole should be drilled as perpendicularly to the fracture line as possible.
Insert a 2.5 mm drill sleeve inside the gliding hole and drill the threaded hole in the far cortex with a 2.5 mm drill bit.
Measure the depth of the hole with the hook of the depth gauge pointing proximally.
Tap the far cortex with the 3.5 mm cortical tap.
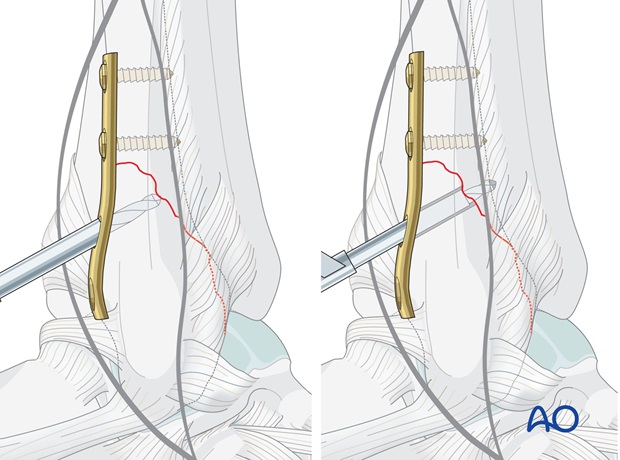
Insertion of the lag screw(s)
Insert a 3.5 mm cortical screw, functioning as a lag screw, and tighten carefully.
If the bone is osteoporotic, or if the fragment is large, a second cortical lag screw may be inserted through the remaining distal plate hole.
Final x-rays should be taken now.
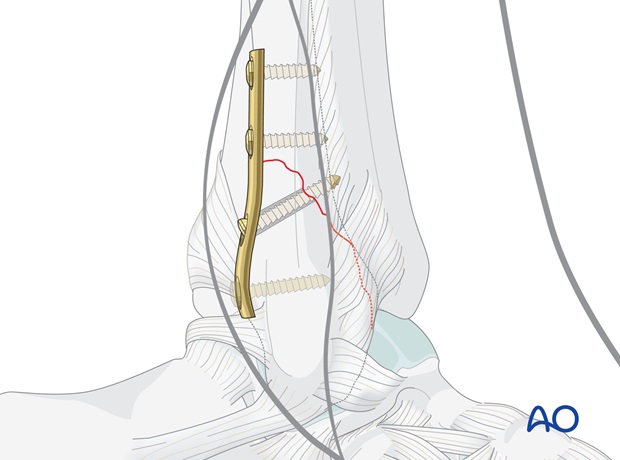
Note
In less oblique fractures, or comminution of the anterior cortex (Le Fort lesion), it may not be possible to insert a lag screw, but the distal fragment may still be held with cortex screws through the plate.
6. Fixation of anterior syndesmotic injury
Avulsion from the tibia (Tillaux-Chaput)
Anatomically reduce the fragment with a small dental hook and preliminarily fix it with a 1.0 mm K-wire.
Drill a hole with a 2.5 mm drill bit and protection sleeve as perpendicular as possible to the fracture line without drilling the far cortex.
Measure the depth. Tap the fragment with the 4.0 mm tap and protection sleeve. Insert the 4.0 mm cancellous screw with a washer.
Note
If the fragment is too small for 4.0 mm screw fixation, use a 2.7 mm or a 2.0 mm cortex screw, or suture the fragment to the periosteum of the anterior tibia.
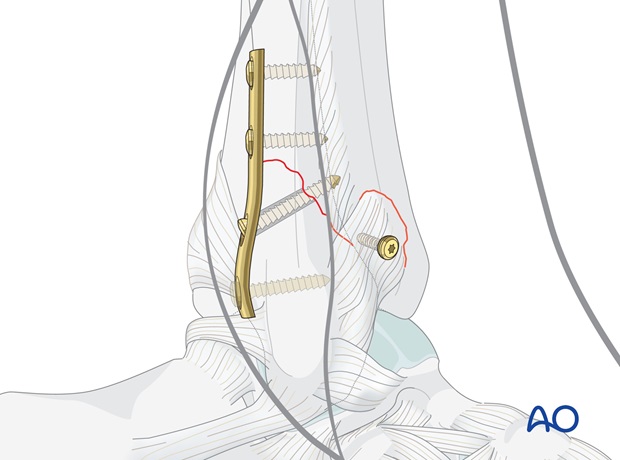
Avulsion from the fibula (Le Fort lesion or Wagstaff fragment)
Usually, the fragment is very small. In this case suture it to the fibular periosteum. If the fragment is large enough, small lag screw fixation can be used.
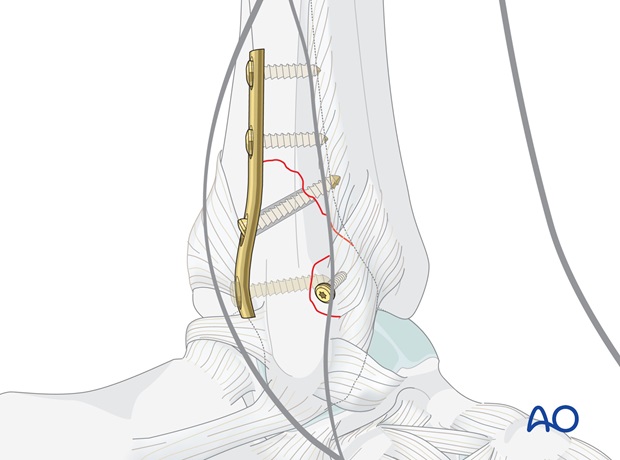
7. Case
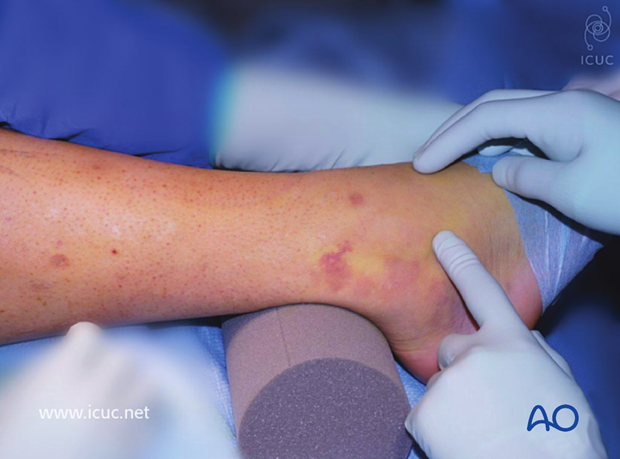
Preoperative images of closed, transsyndesmotic, lateral isolated simple fracture of the malleolus in a 55-year-old patient.
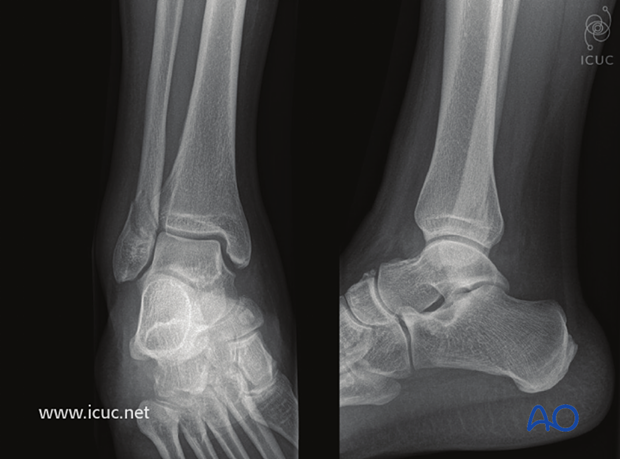
The clinical picture show bruising and the limb placed over a bolster to aid in reduction.
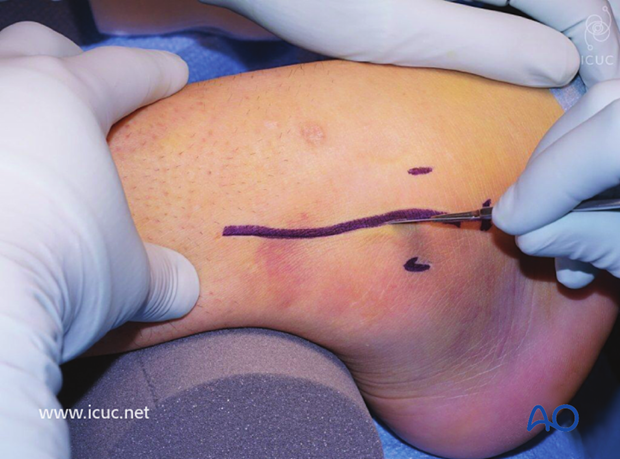
A lateral approach to the fibula was used.
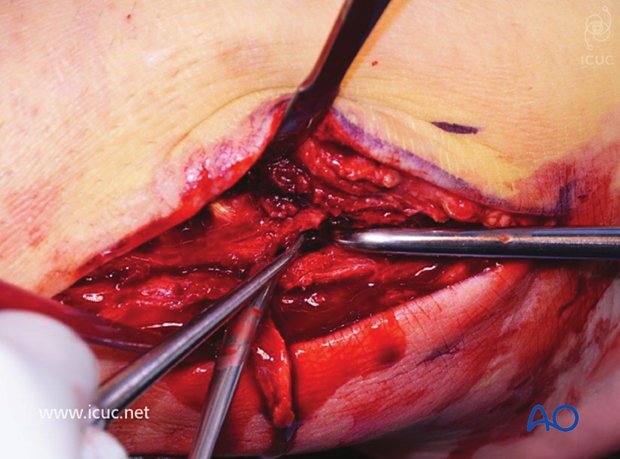
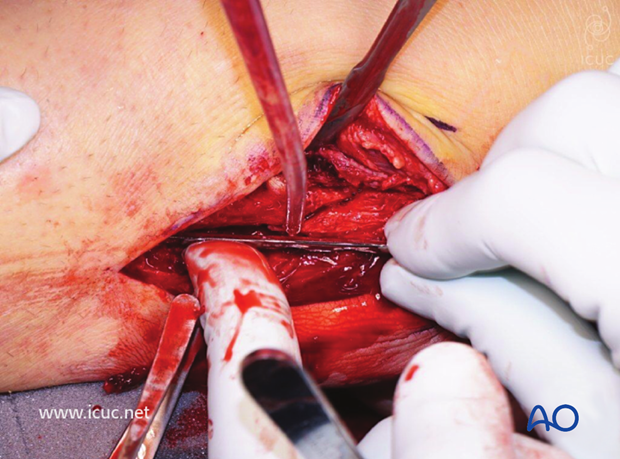
The oblique fracture site is cleaned.
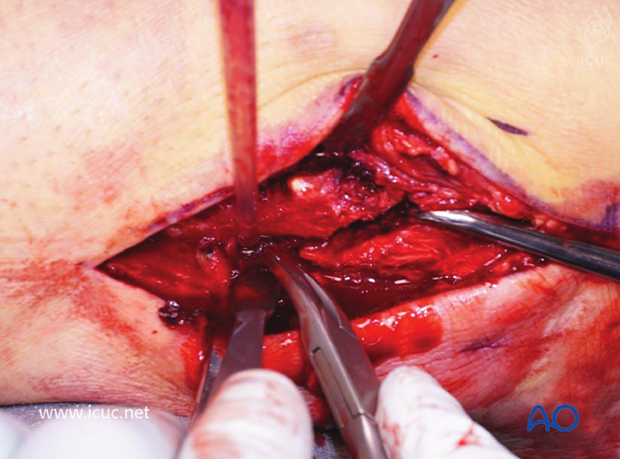
The fracture site is here cleaned and ready for reduction and fixation.
The posterior antiglide fibular plate is inserted.
This plate may be placed posteriorly as an anti-glide plate or lateral after lag screw insertion.
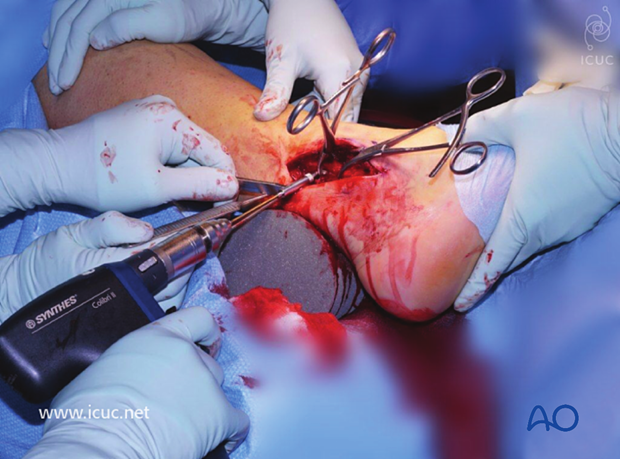
Initial screw insertion in the proximal anti glide plate.
Note, in this image, the posterior to anterior direction to buttress this particular fracture.
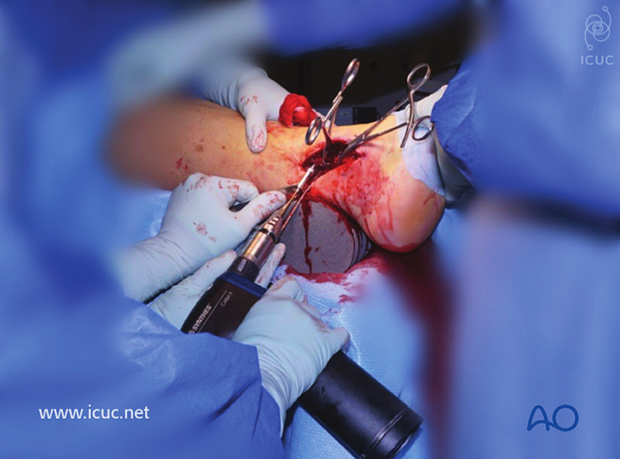
Screw insertion.
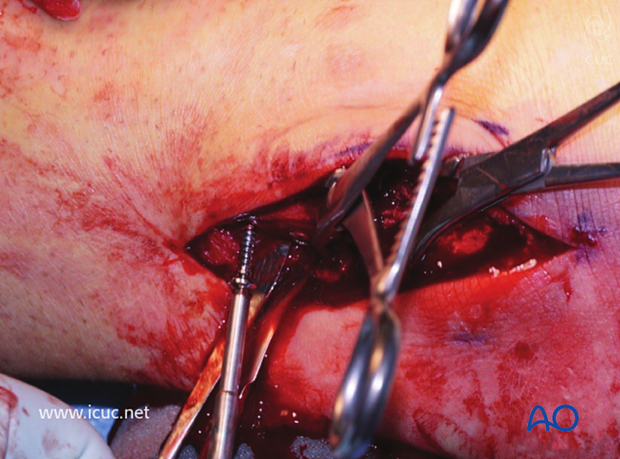
Intraoperative AP image shows the fracture buttressed but not yet with an interfragmentary lag screw inserted.
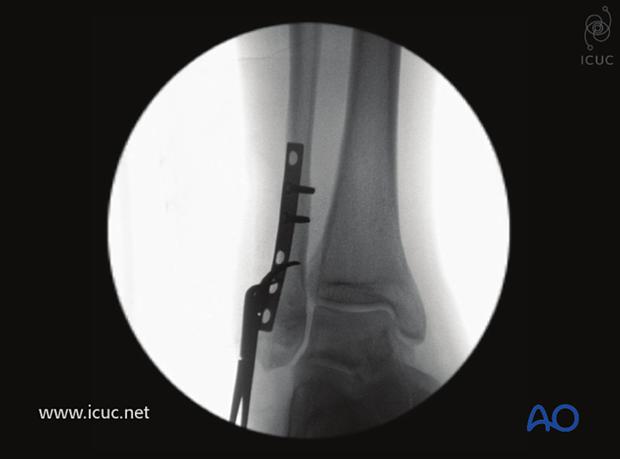
Same as above in the lateral view.

Drilling prior to lag screw insertion through the plate across the fracture site.
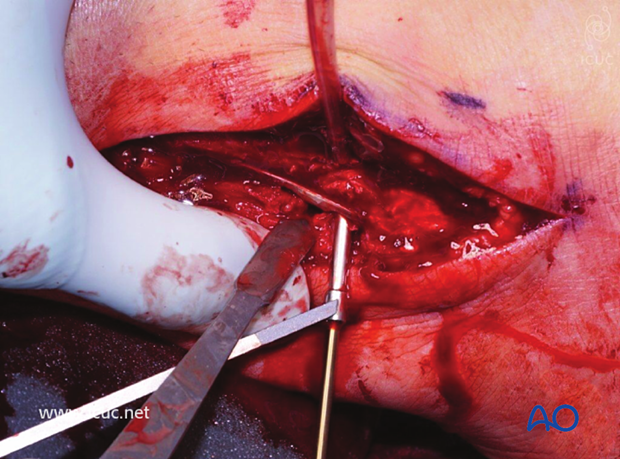
Lag screw insertion.
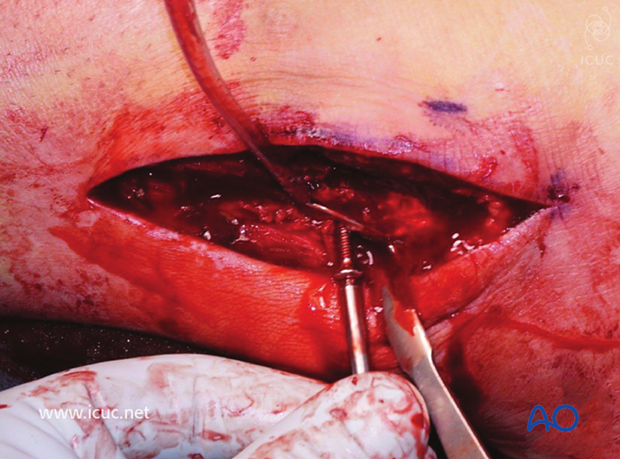
Distal fixation into the malleolus.
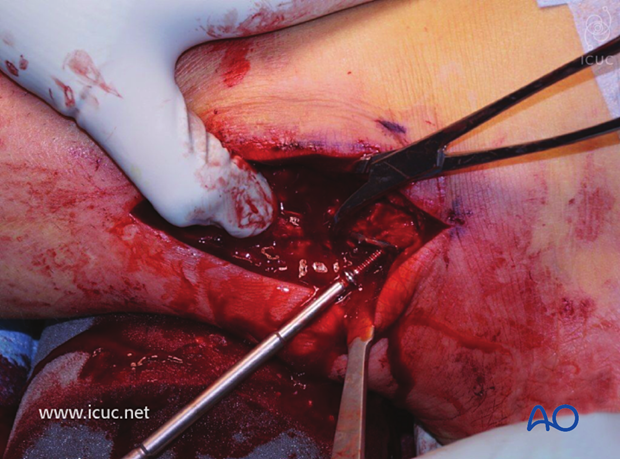
Intraoperative AP image of final fracture reduction and fixation.
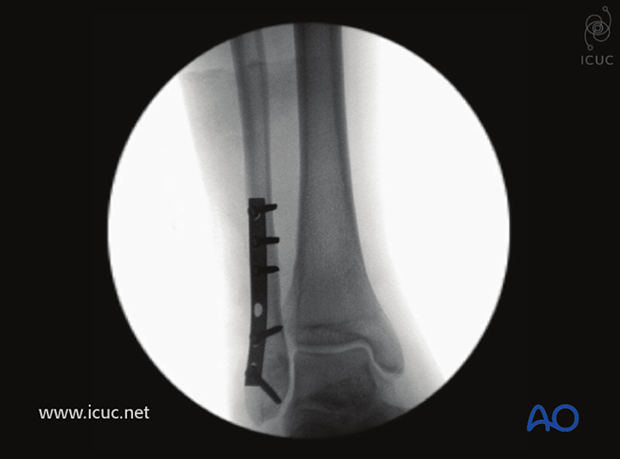
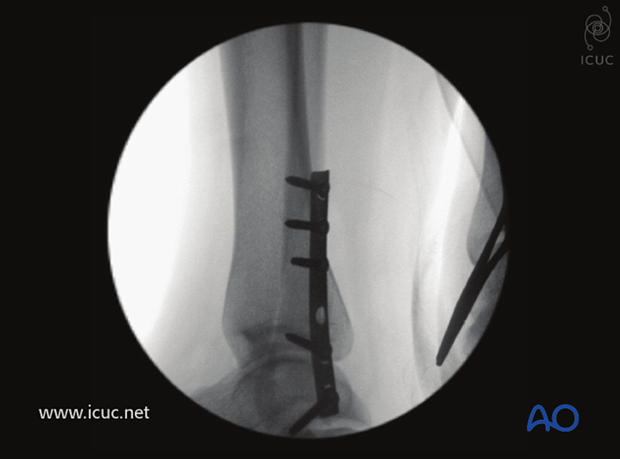
Same as above in lateral view. Note the screw second from the bottom is a lag screw through the plate.
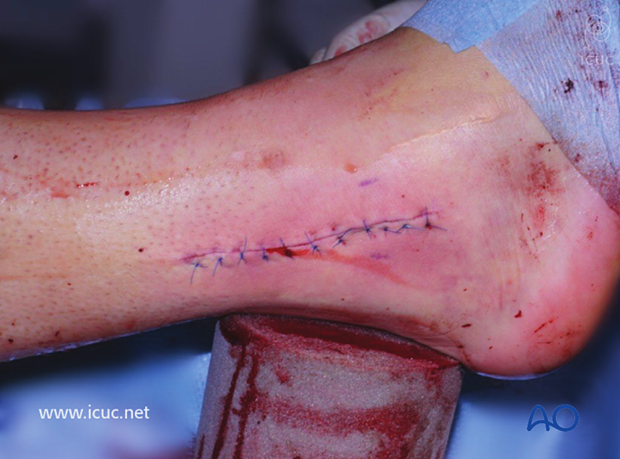
Final closure.
Here a non-weight bearing cast is applied. However, with stable fixation such as this, full weight bearing would be advised.
Postoperative image in AP and lateral view.
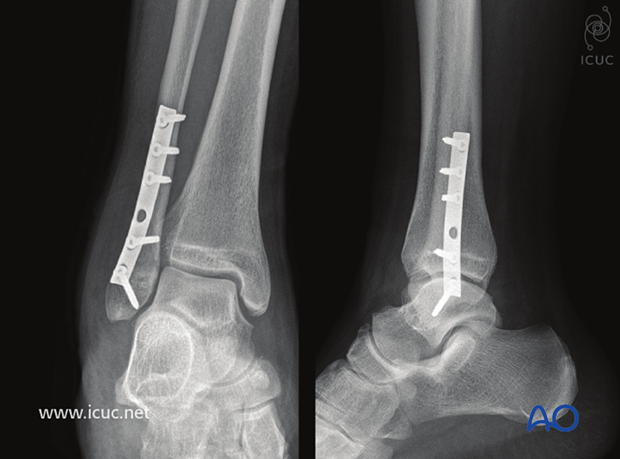
5 Week postoperative images show maintenance of reduction and no callus formation. Callus formation is not expected as there is a compression in a metaphyseal fracture.
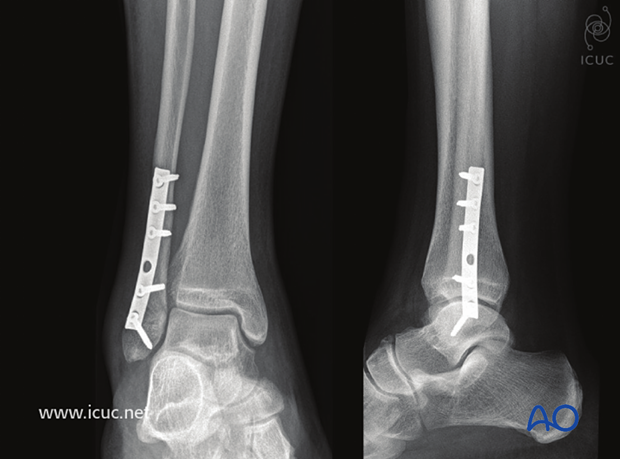
15 Weeks postoperative images.
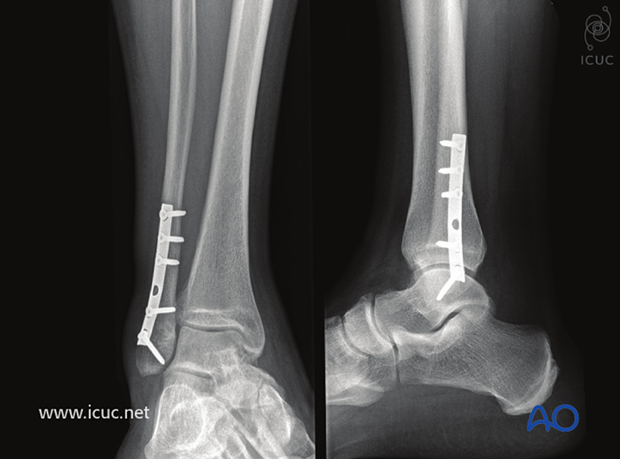
8. Postoperative treatment of infra- and trans-syndesmotic malleolar fractures
A bulky compression dressing and a lower leg backslab, or a splint, are applied, and the limb is kept elevated for the first 24 hours or so, in order to avoid swelling and to decrease pain.
In anatomically reconstructed, stable malleolar fractures, early active exercises and light partial weight bearing are encouraged after day one. In osteoporotic bone, weight bearing should be postponed.
X-ray evaluation is made after 1 week and then monthly until full healing has occurred. Progressive weight bearing is recommended as tolerated.













