ORIF
1. Principles
General considerations
These are unstable injuries and the integrity of the syndesmosis must be restored. This necessitates bringing the fibula out to length and then securing the syndesmosis with two positioning screws. The fibular fracture is not normally fixed.
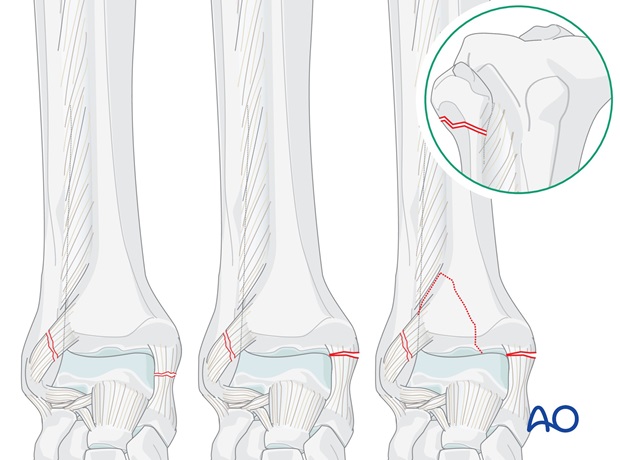
2. Order of fixation
The crux of treatment is the correct reduction of the lateral malleolus and fibula. Length alignment and rotation must be restored otherwise it will not be possible to reduce the talus, the syndesmosis or the Volkmann’s triangle (if present).
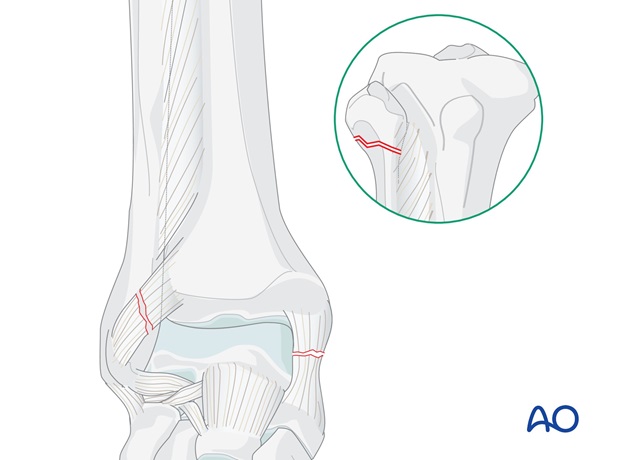
Proximal fibular fracture without shortening
- The medial malleolus is fixed (if fractured)
- The integrity of the syndesmosis is restored
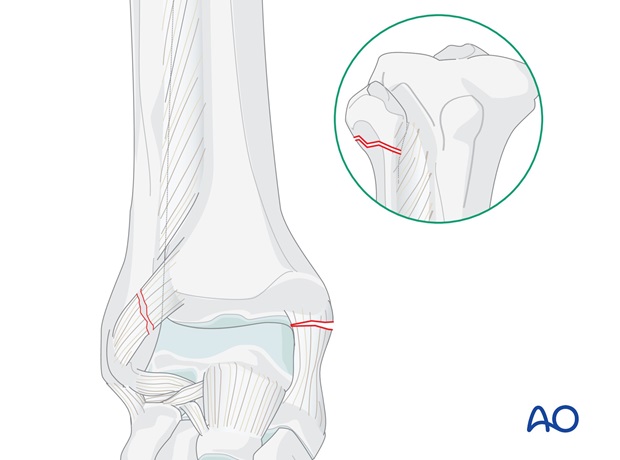
Proximal fibular fracture with shortening
- The medial malleolus is fixed (if fractured)
- The fibula is brought down to length and the integrity of the syndesmosis is restored
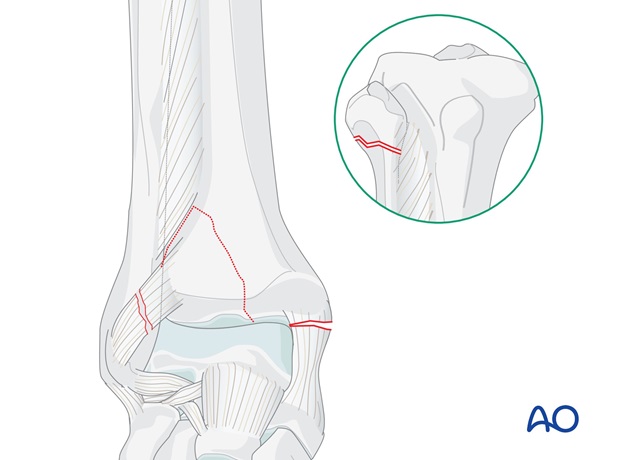
Proximal fibular fracture with medial and posterior fracture
- The medial malleolus is fixed (if fractured)
- The fibula is brought down to length if necessary and the integrity of the syndesmosis is restored
- The Volkmann's fragment is reduced and fixed
3. Patient preparation
Depending on the approach, the patient may be placed in the following positions:
- Supine position
- Lateral position
- Supine position, figure-of-four
- Prone position (preferred for posterior fractures)
4. Approaches
Approach to the medial fracture
A medial fracture is addressed through the medial approach.
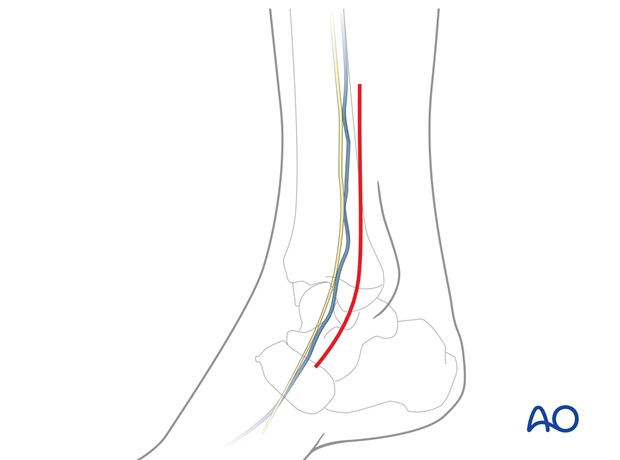
Approach to the syndesmosis
A direct lateral approach is used for insertion of positioning screws.
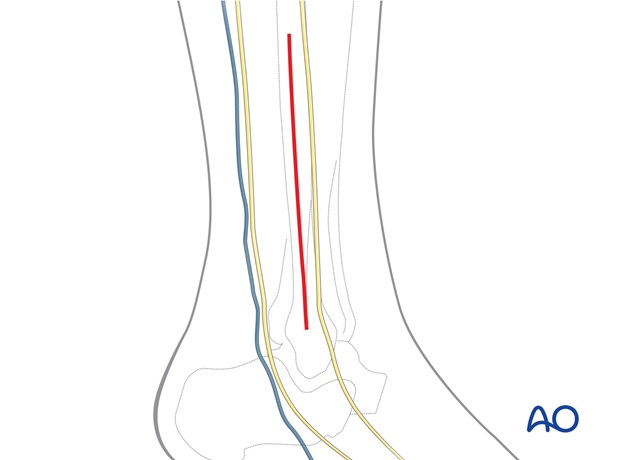
Approaches to the Volkmann's fragment
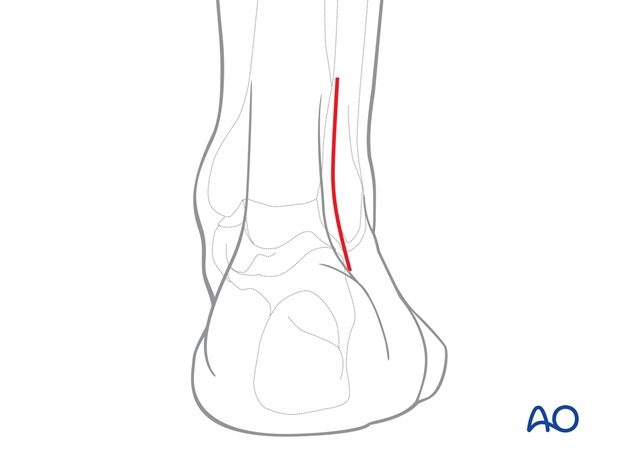
If direct reduction and fixation of the Volkmann's fragment is chosen, a posterior lateral approach is used.
This incision may be extended proximally to allow access and fixation of the fibular fracture if it is relatively low. Alternatively, and more commonly, the fibular fracture is relatively high, and is approached through a separate lateral incision placed more proximally.
Alternatively, the integrity of the syndesmosis may be restored through a standard lateral approach, and the Volkmann's fragment may be addressed with indirect reduction and anterior screw fixation through additional anterior stab incisions.
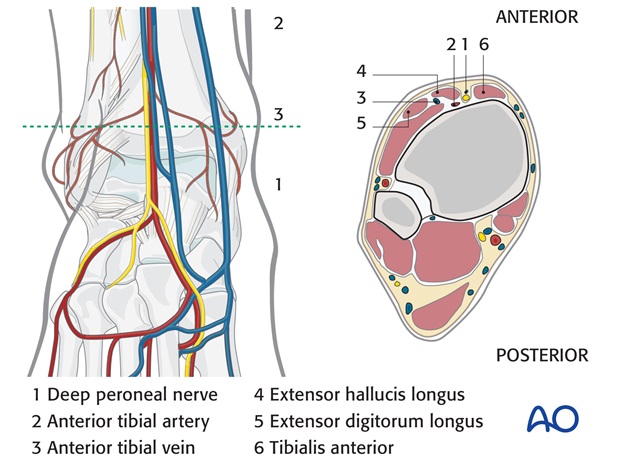
5. Fixation
Medial malleolar fracture (if present)
The ankle joint in these fractures is often very unstable. The stability is dramatically improved once the medial fracture is fixed (if present).
Most medial fractures are fixed with lag screws, which should be inserted perpendicular to the plane of the fracture.
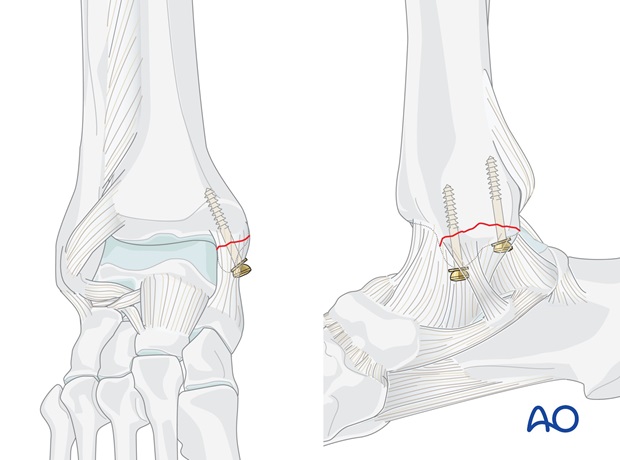
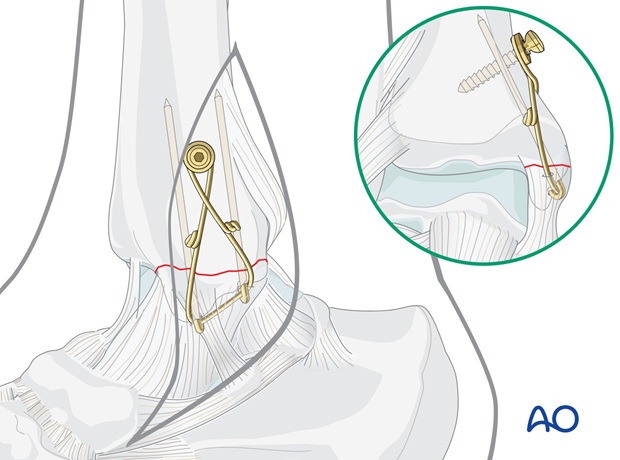
If the fragment is too small or in poor quality bone, K-wires and cerclage compression wiring may be better.
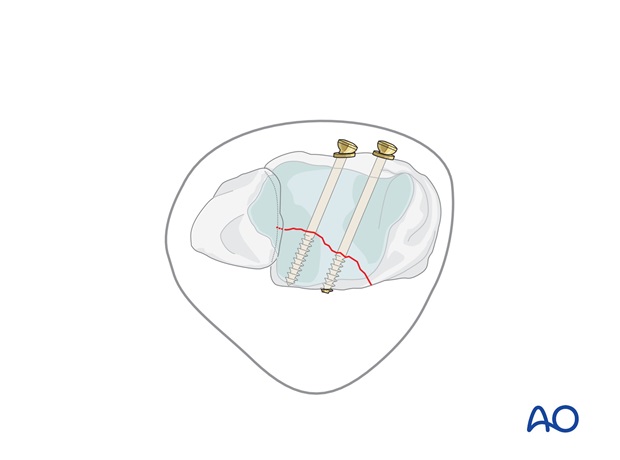
Syndesmosis
The integrity of the syndesmosis is restored and stabilized with one or two positioning screws.
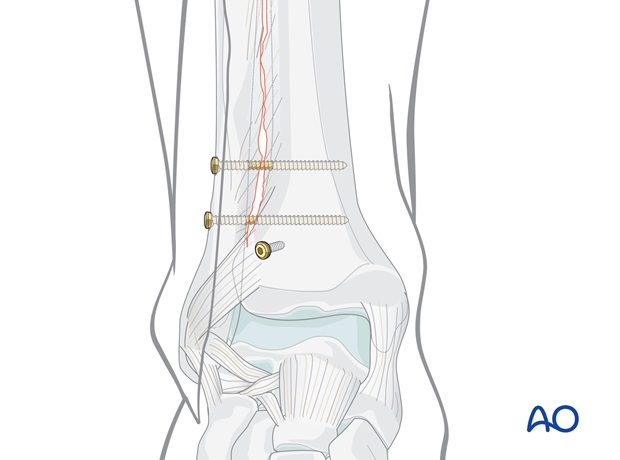
Volkmann's fragment (if fractured)
The Volkmann's fragment may be addressed under direct vision through a posterolateral approach.
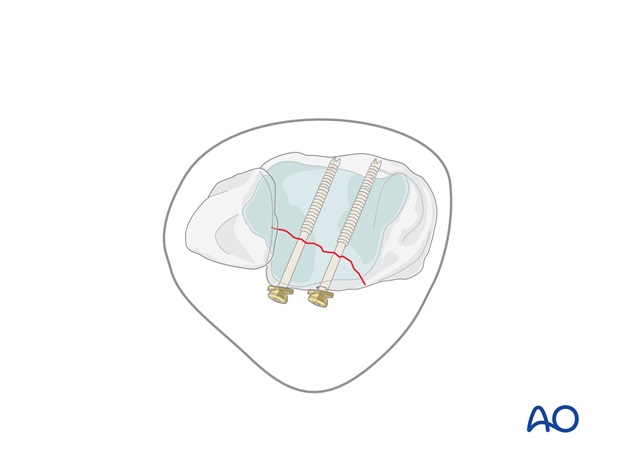
If indirect reduction of the Volkmann's fragment is chosen, sagittal lag screws are inserted through separate stab incisions.
6. Check of osteosynthesis
Check the completed osteosynthesis by image intensification.
Make sure the intra articular components of the fracture have been anatomically reduced.
Make sure none of the screws are entering the joint. This needs to be confirmed in multiple planes.
7. Postoperative treatment of suprasyndesmotic malleolar fractures
Postoperatively, the joint is held in neutral position by a splint.
If drains are used, they are removed after 24-48 hours. The patient is mobilized with crutches depending on the swelling of the soft tissues.
Postoperative CT control of both ankles is recommended if any syndesmotic incongruence is suspected or if a positioning screw was inserted; special notice is taken of the rotation of the fibula in the syndesmosis, compared with the uninjured side.
Joint motion is allowed and encouraged during physiotherapy. Weight bearing of 20-30 kg when the foot is unsupported. Full weight bearing may be possible using a cast, or an ankle brace, but should not be allowed when a positioning screw is used because of the risk of implant failure.
The positioning screw may be removed after 8-10 weeks.













