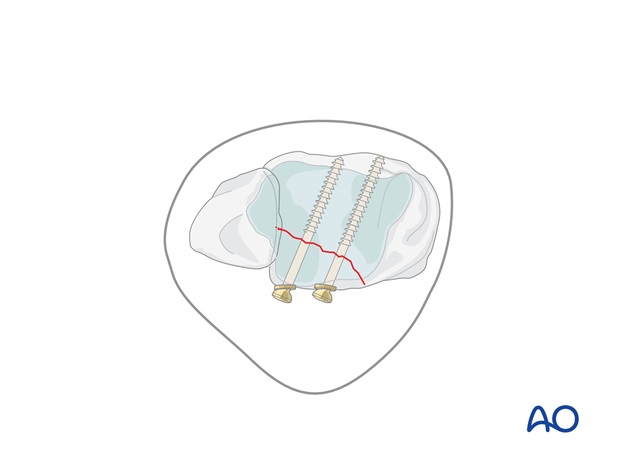
Volkmann fracture: posterior lag screw
1. Preliminary consideration
This procedure is easier to perform with cannulated screws if they are available.
Medium sized fragments (> 25% of the articular surface) are fixed with lag screws. If the fragment is large and has a proximal extension, add more screws or a buttress plate.
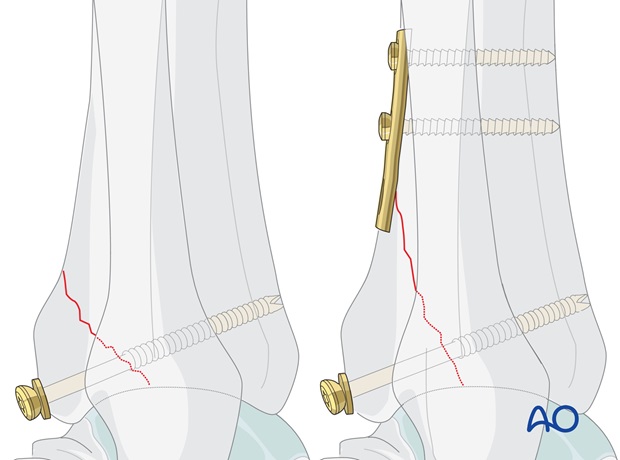
If the fragment is large and has a proximal extension, add more screws or a buttress plate.
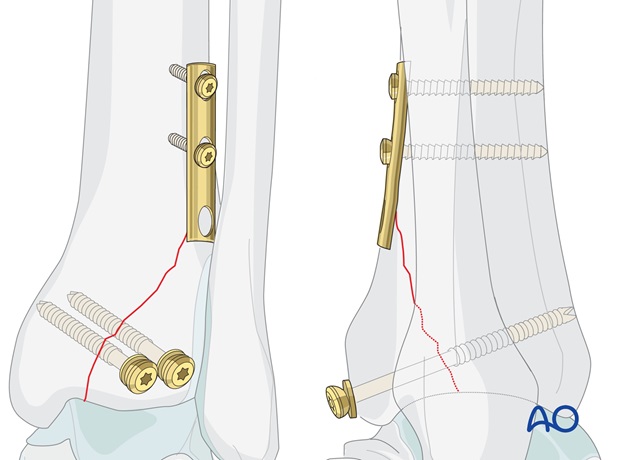
A small fragment (< 25% of the articular surface) with joint stability after malleolar reconstruction = fixation is not necessary.
A medium sized fragment (> 25% of the articular surface), without long proximal extension = fixation with lag screw(s).
A large fragment (> 25% of the articular surface) with long proximal extension = fixation with lag screws (+/- buttress plate).
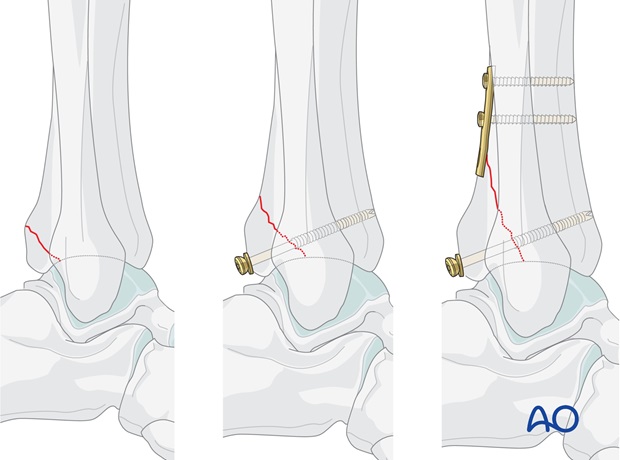
2. Reduction
The fragment is visualized directly.
The fragment is triangular. It may be held with a K-wire as a joystick and brought down into its anatomic position. Simple finger pressure may be adequate to maintain reduction while the K-wire is driven into the tibia.
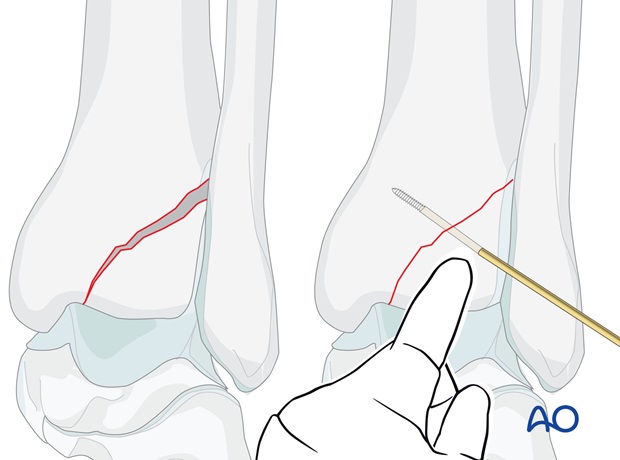
Alternatively, it may be possible to hold the reduction with a large pointed bone forceps.
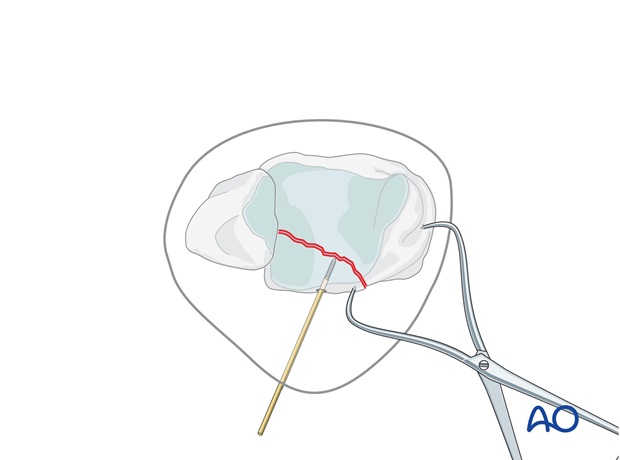
As it is reduced the apex of the triangle can be seen to fit into the cortical defect. This confirms anatomic reduction even though the joint surface cannot be directly visualized.
Reduction may also be confirmed with image intensifier.
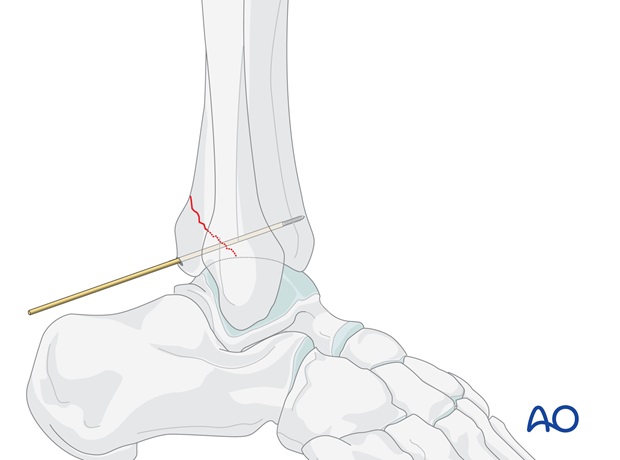
Provisional fixation of the Volkmann’s triangle is achieved with two K-wires, or 1.25 mm guide wires for the cannulated screws. The guide wires should be perpendicular to the fracture plane, at the desired positions of the planned screws, and should not penetrate the anterior cortex.
Check reduction and position of guide wires under image intensification.
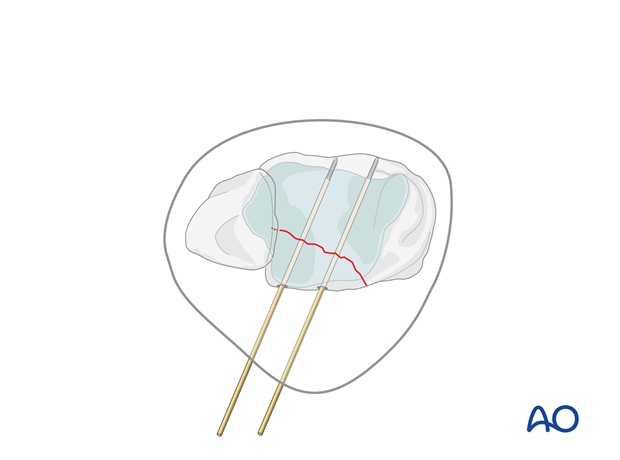
3. Fixation with cannulated screw
Screw selection
Determine the length of the screw with the appropriate depth measuring device.
The chosen 3.5 mm partially threaded cannulated screw must lie with its threads completely beyond the fracture to achieve interfragmentary compression, but should not penetrate the anterior cortex. If the bone is osteoporotic and there is a risk that the head of the screw will sink into the bone, use a washer.
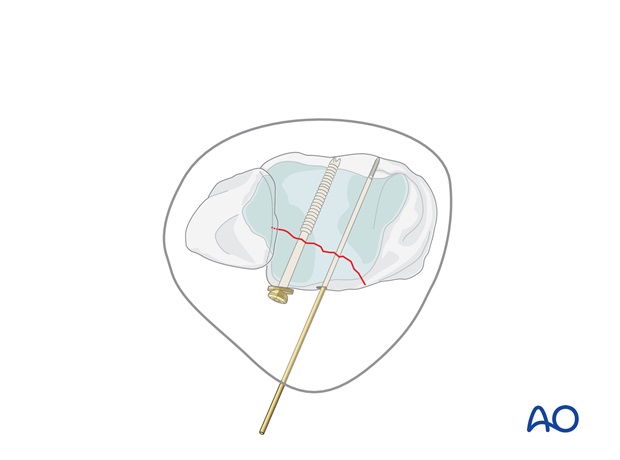
Alternatively, a fully threaded screw may be used with lag effect by overdrilling the hole in the Volkmann's fragment.
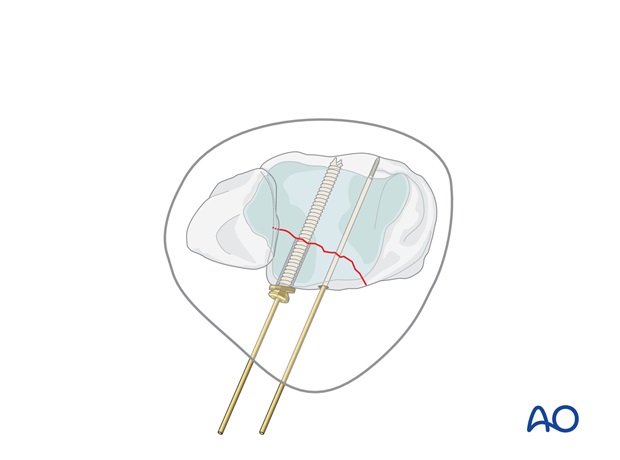
Insert first screw
Drill a hole over the more lateral guide wire, through both fragments, with a 2.7 mm cannulated drill bit. Tap the posterior tibial cortex with the 3.5 mm cannulated tap and protection sleeve.
Insert the selected 3.5 mm partially threaded cannulated screw, with a washer if desired.
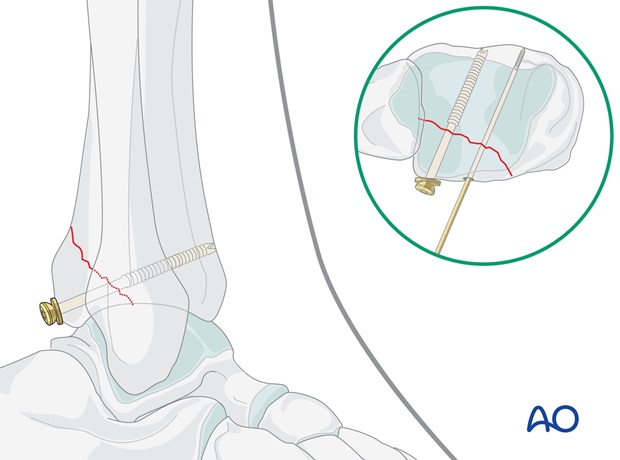
Insert the second screw
Remove the first guide wire and repeat the process for the second screw.
If the fragment has a large enough proximal extension, a third screw may be used here, or a buttress plate may be applied.
Confirm satisfactory reduction and screw placement with X-ray control.
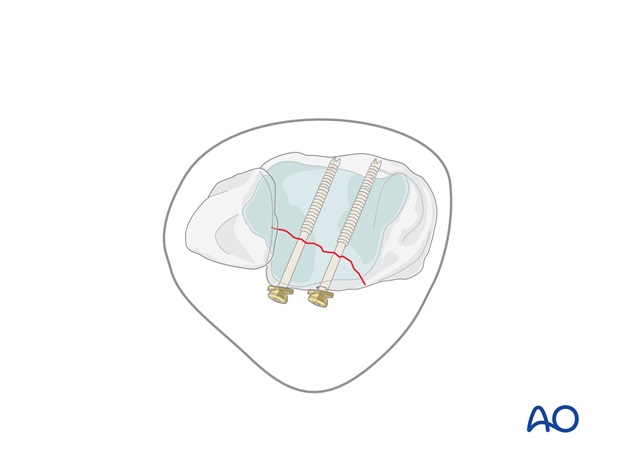
4. Fixation with non-cannulated screws
First screw
Remove one K-wire and drill a hole through the fragment parallel to the other K-wire, using a 2.5 mm drill bit and protection sleeve.
Measure the depth of the hole and tap the near tibial cortex with the 4.0 mm cancellous tap and protection sleeve. Insert a 4.0 mm partially threaded cancellous screw, with a washer if needed.
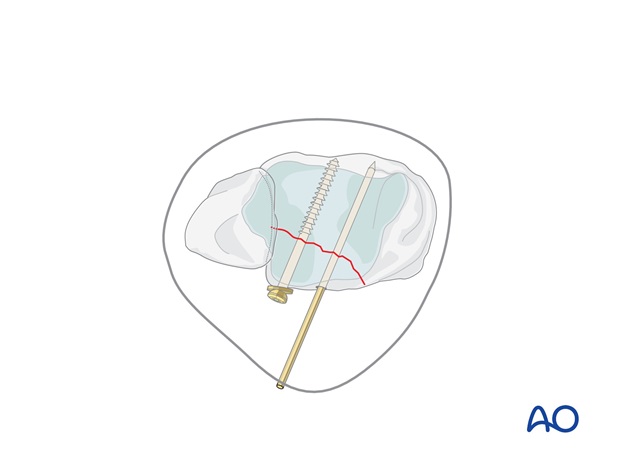
Second screw
Replace the second K-wire with the second lag screw.
Confirm satisfactory reduction and screw placement with X-ray control.