Bridge plating
1. General considerations
Multifragmentary fractures are best treated with bridge plating.
ORIF provides sufficient stability for immediate mobilization, reducing the risk of joint stiffness and tendon adhesions.
Even in the hand, which is well vascularized, small fragment comminution means poor soft-tissue attachment to the fragments and, thereby, compromised vascularity.
Some wedge fracture patterns, eg, with a small wedge fragment, cannot be stabilized with lag-screw and plate fixation and therefore need bridge plating.
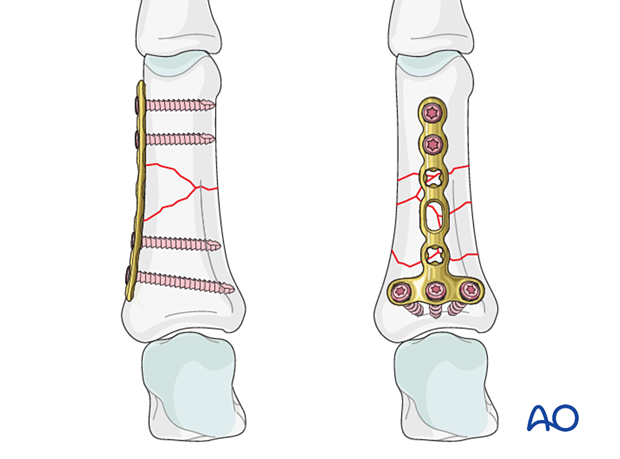
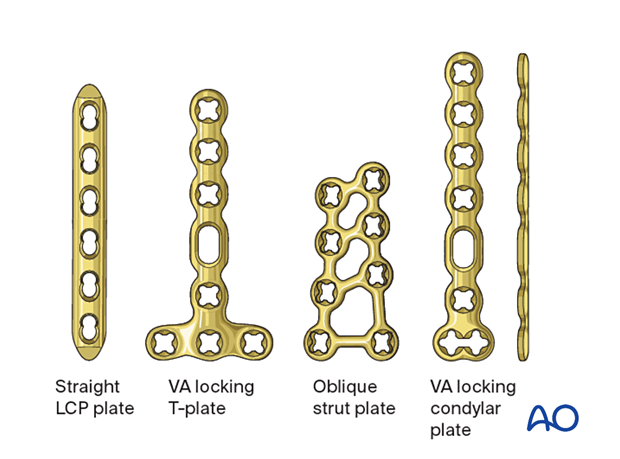
For bridge plating, several plate types may be used:
- Conventional straight locking compression plate (LCP); dorsal and lateral
- T-plate; dorsal
- Strut plate; dorsal
- Condylar plate; lateral or dorsal
The plates may come with or without variable-angle (VA) locking head screws. If an anatomical plate is not available, a conventional minicondylar plate may be used.
The plate selection depends on the fracture pattern and should allow at least two screws in the proximal and distal main fragments.
In this procedure, bridge plating with a VA T-plate is shown with the transverse part applied to the phalangeal base.
2. Patient preparation
Place the patient supine with the arm on a radiolucent hand table.

3. Approaches
For this procedure, the following approach is normally used for application of a lateral plate:
Application of a dorsal plate may require a dorsal approach:
4. Reduction
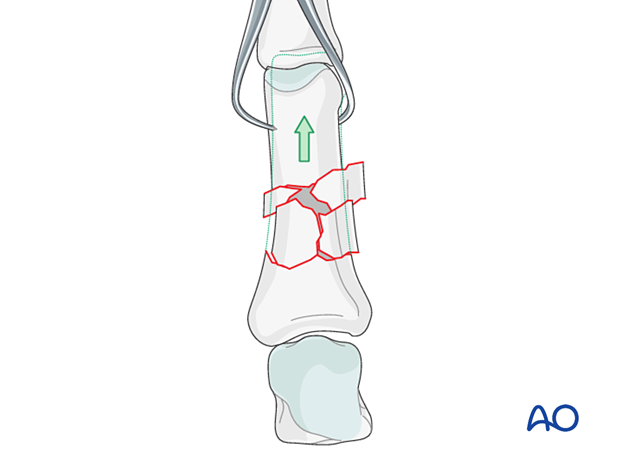
Gaining length
Length can be gained by traction applied manually, by a finger trap, or with pointed reduction forceps.
Confirm length and rotation with the neighboring fingers with the metacarpophalangeal (MCP) joint in 90° flexion.
Provisional K-wire fixation
Provisional fixation can be provided by a K-wire, inserted through the head of the metacarpal, with the MCP joint in 90° of flexion, through the base, medullary canal, and into the head of the proximal phalanx.
To avoid conflicts with the plate screws, the K-wire should be inserted slightly oblique to the phalangeal axis.
Take great care to control rotational alignment.
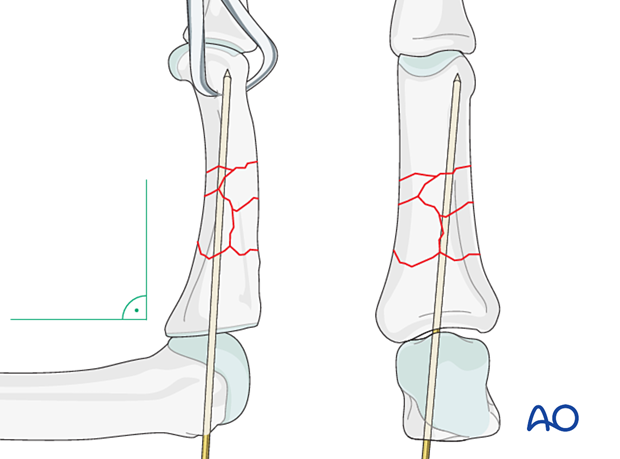
The K-wire provides angular alignment in both planes but does not control rotation.
Rotational alignment can only be judged with the fingers in a degree of flexion and never in full extension. Malrotation may manifest itself by overlap of the flexed finger over its neighbor. Subtle rotational malalignments can often be judged by a tilt of the leading edge of the fingernail when the fingers are viewed end-on.
Any malrotation needs to be corrected by direct manipulation and later fixed with the plate.
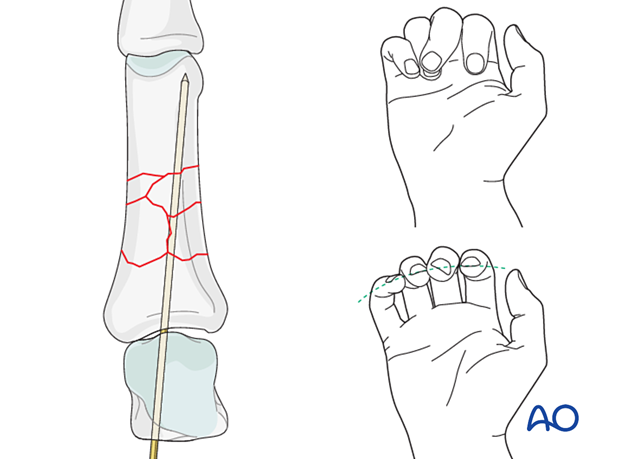
5. Checking alignment
Identifying malrotation
At this stage, it is advisable to check the alignment and rotational correction by moving the finger through a range of motion.
Rotational alignment can only be judged with flexed metacarpophalangeal (MCP) joints. The fingertips should all point to the scaphoid.
Malrotation may manifest by an overlap of the flexed finger over its neighbor. Subtle rotational malalignments can often be judged by a tilt of the leading edge of the fingernail when the fingers are viewed end-on.
If the patient is conscious and the regional anesthesia still allows active movement, the patient can be asked to extend and flex the finger.
Any malrotation is corrected by direct manipulation and later fixed.
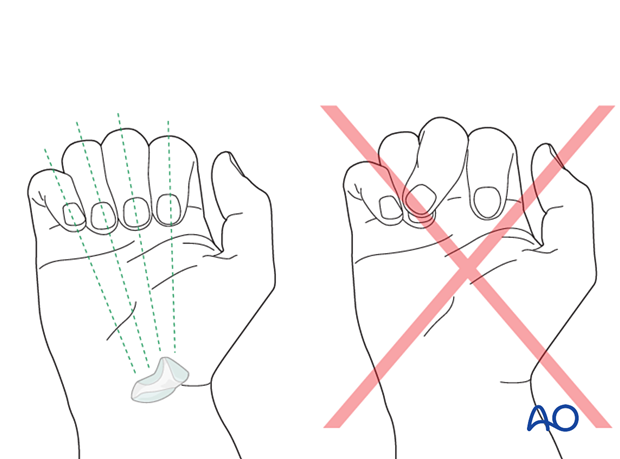
Using the tenodesis effect when under anesthesia
Under general anesthesia, the tenodesis effect is used, with the surgeon fully flexing the wrist to produce extension of the fingers and fully extending the wrist to cause flexion of the fingers.
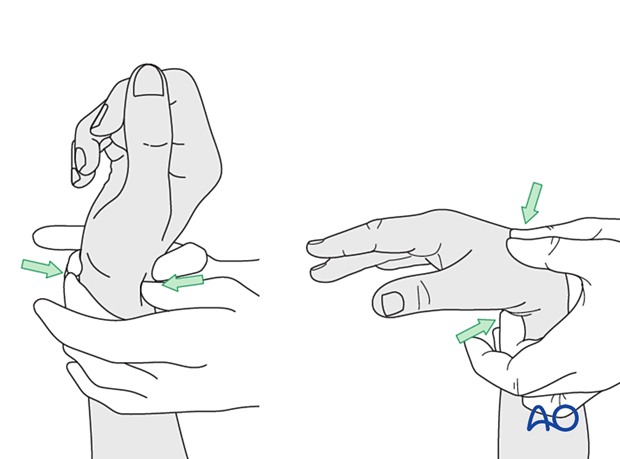
Alternatively, the surgeon can exert pressure against the muscle bellies of the proximal forearm to cause passive flexion of the fingers.
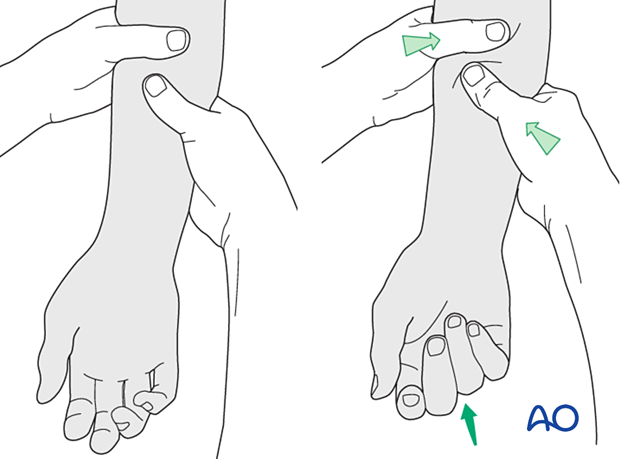
Confirm fracture fixation and stability with an image intensifier.
6. Plate preparation
Plate trimming
Adapt the plate length to fit the length of the proximal phalanx. Avoid sharp edges, which may be injurious to the tendons. There should be at least 3 plate holes distal to the fracture available for fixation in the diaphysis. At least two screws need to be inserted into the diaphysis.
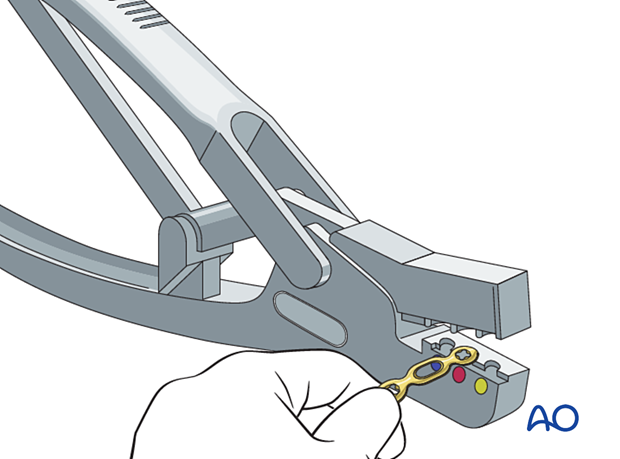
Contouring
Contour the plate exactly to replicate the normal dorsal shape of the phalanx.
The T-end of the plate must be bent to follow the convexity of the dorsal surface of the phalangeal base.
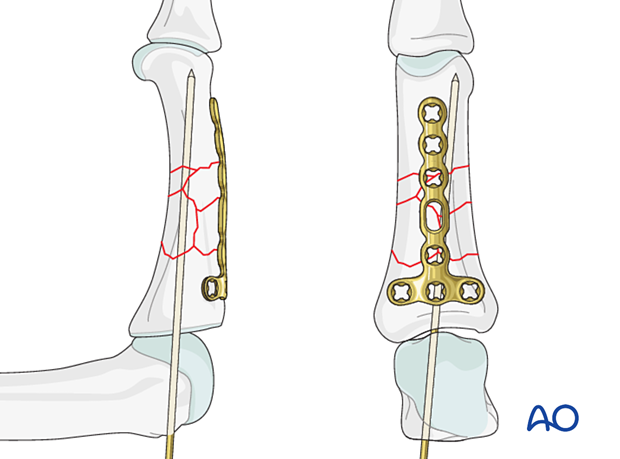
Check for perfect adaptation of the plate to the base of the phalanx before screw fixation.
If it is not perfectly adapted, fracture displacement or malrotation may occur.
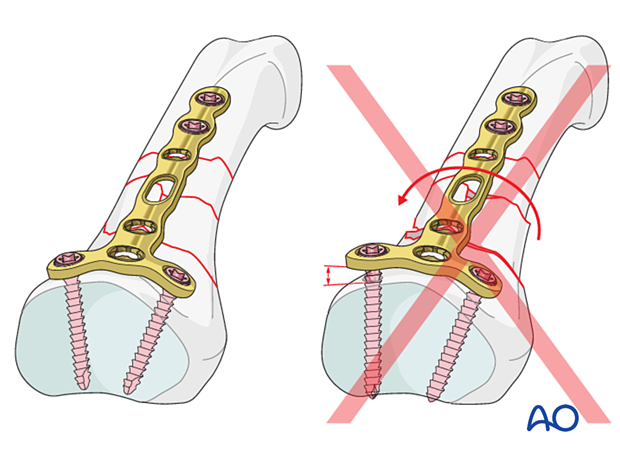
7. Plate fixation
Plate positioning
Place the plate dorsally on the phalanx, proximally enough from the comminuted area, to allow at least three screws to be inserted into the metaphysis.
Ensure that the plate is centered on the diaphysis in the coronal plane.
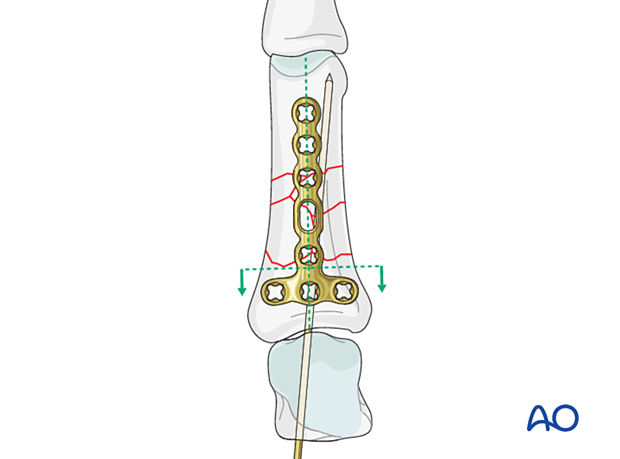
Keep the plate in place with the atraumatic forceps.
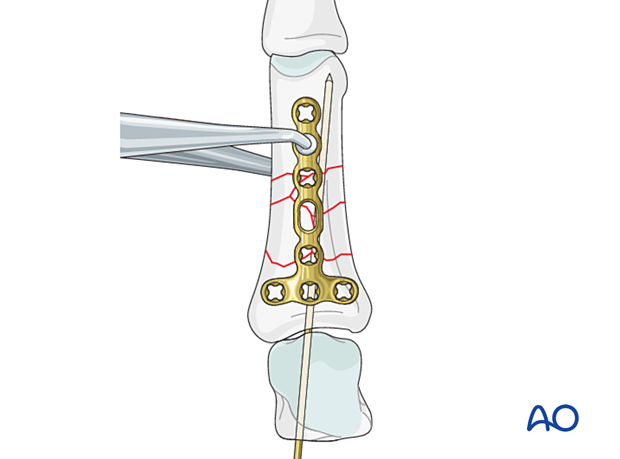
Screw insertion (proximal)
Start with screw insertion in the peripheral holes in the transverse part of the plate. This will fix the plate securely while avoiding conflict with the provisional K-wire.
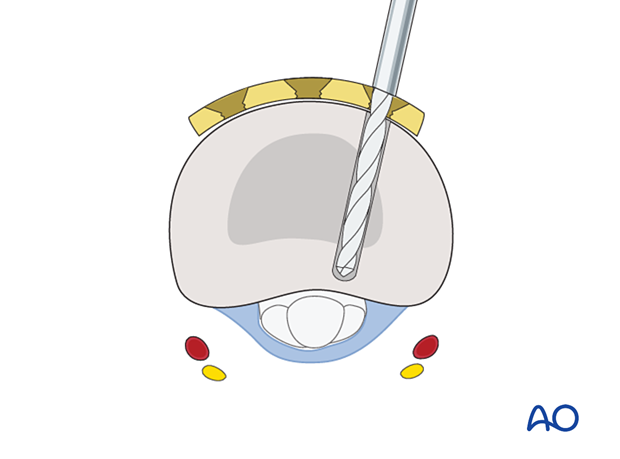
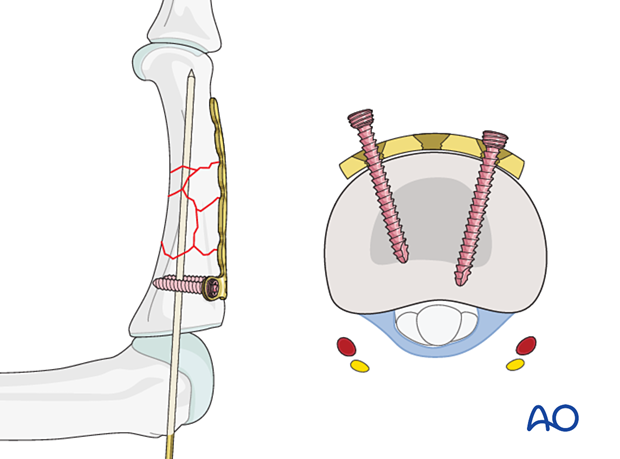
Insert the first screw but do not fully tighten it. Ensure it engages the far cortex but does not protrude into the fibroosseous flexor digital channel, where the flexor tendons run. The digital nerve and artery are also at risk of injury.
Insert the second screw, alternately tightening both screws.
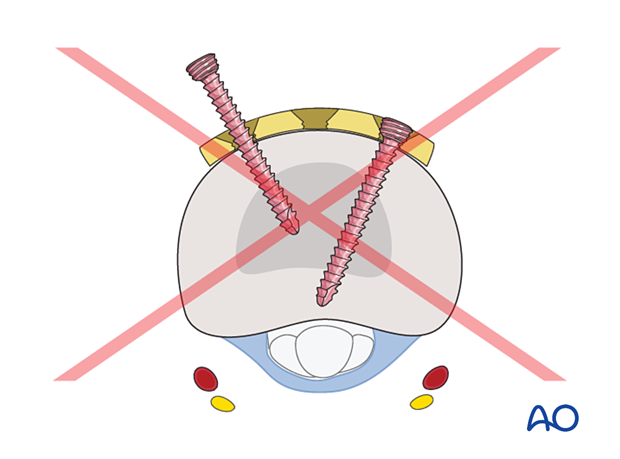
Pitfall: interfering screws
Correcting malrotation
Manipulate the distal part of the phalanx to correct any malrotation.
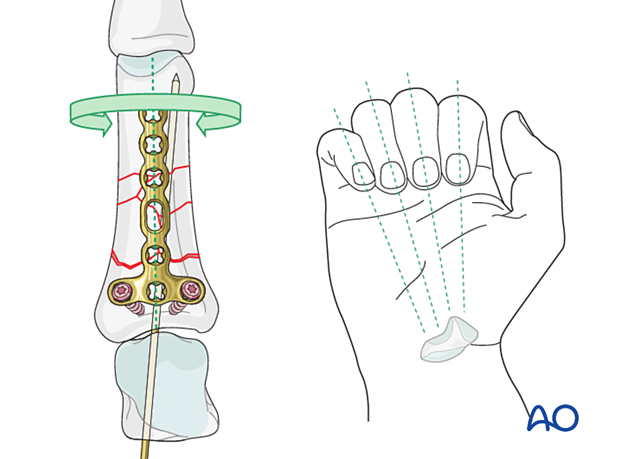
Screw insertion (distal)
Partially retract the provisional K-wire sufficiently to prevent interference with drilling the most distal hole.
Insert the screws into the most distal plate holes.
Remove the K-wire and confirm length, alignment, and rotation.
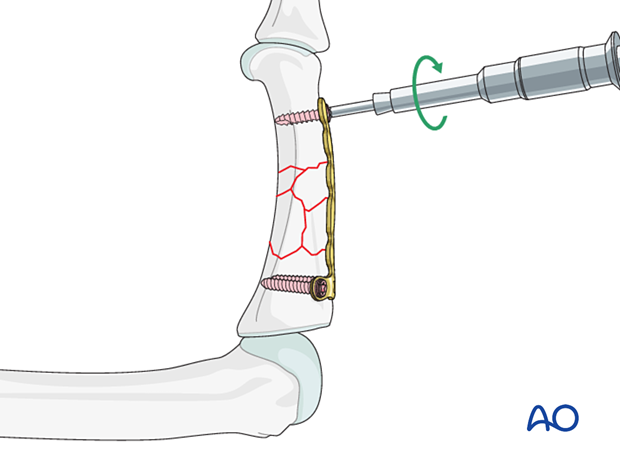
Insertion of additional screws
If the fracture configuration allows, insert a further screw in the next plate hole, but be sure not to enter the comminuted zone.
Insert the middle screw in the transverse part of the plate in the same fashion.
Cover the plate with periosteum to avoid adhesion between the tendon and the implant leading to limited finger movement.
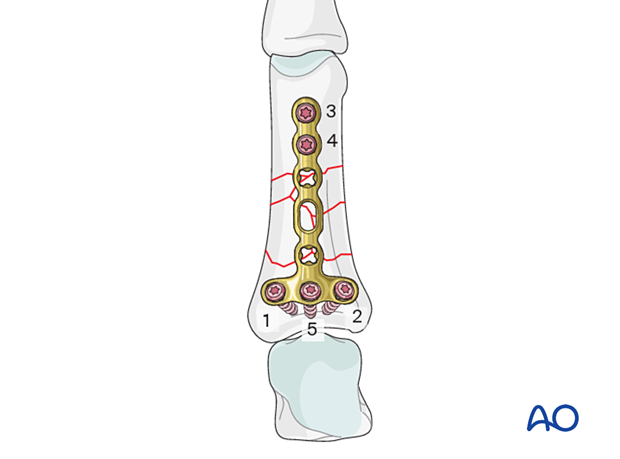
Screw fixation of a wedge fragment
In some wedge fractures, it may be desirable to approximate the wedge fragment to the plate to strengthen the construct. Insert a short neutral monocortical screw and carefully tighten it.
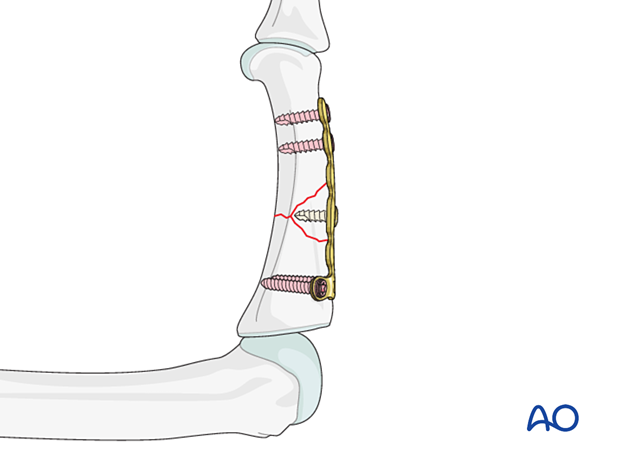
Alternative constructs
Bridge plate fixation with a strut plate
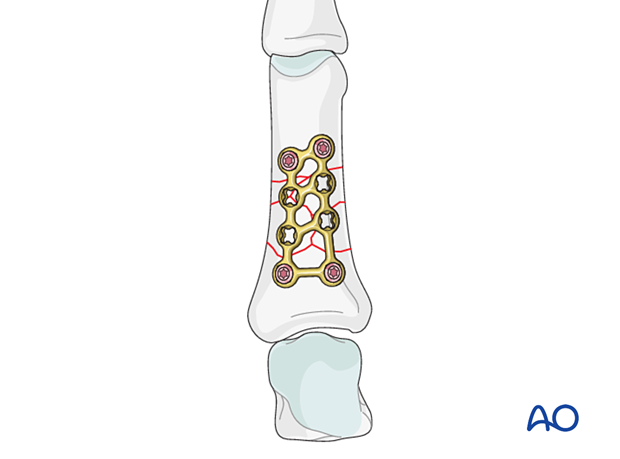
8. Final assessment
Confirm fracture reduction and stability and implant position with an image intensifier.
9. Aftercare
Postoperative phases
The aftercare can be divided into four phases of healing:
- Inflammatory phase (week 1–3)
- Early repair phase (week 4–6)
- Late repair and early tissue remodeling phase (week 7–12)
- Remodeling and reintegration phase (week 13 onwards)
Full details on each phase can be found here.
Postoperative treatment
If there is swelling, the hand is supported with a dorsal splint for a week. This would allow for finger movement and help with pain and edema control. The arm should be actively elevated to help reduce the swelling.
The hand should be splinted in an intrinsic plus (Edinburgh) position:
- Neutral wrist position or up to 15° extension
- MCP joint in 90° flexion
- PIP joint in extension
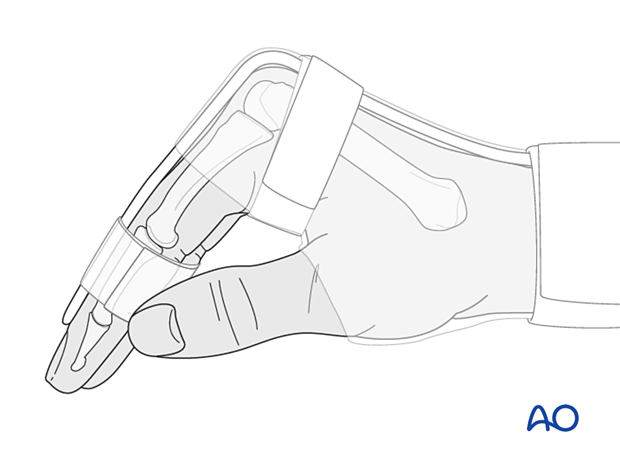
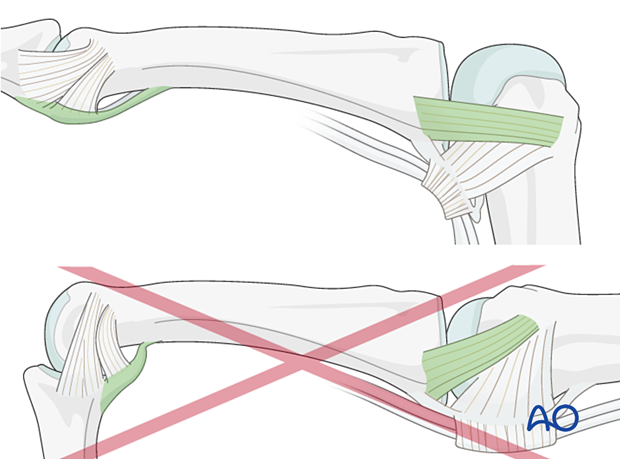
The reason for splinting the MCP joint in flexion is to maintain its collateral ligament at maximal length, avoiding scar contraction.
PIP joint extension in this position also maintains the length of the volar plate.
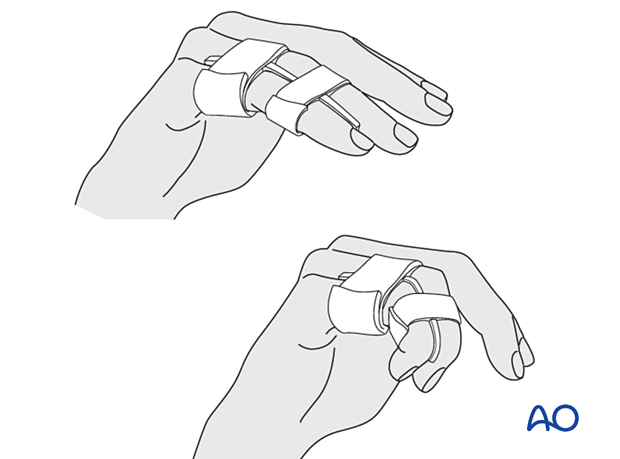
After subsided swelling, protect the digit with buddy strapping to a neighboring finger to neutralize lateral forces on the finger.
Functional exercises
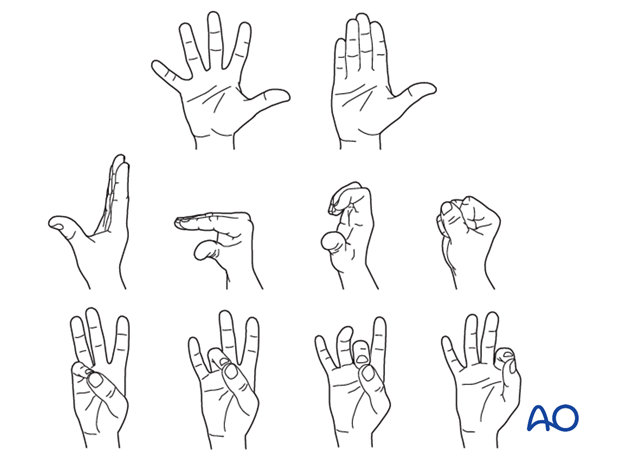
To prevent joint stiffness, the patient should be instructed to begin active motion (flexion and extension) immediately after surgery.
Follow-up
See the patient after 5 and 10 days of surgery.
Implant removal
The implants may need to be removed in cases of soft-tissue irritation.
In case of joint stiffness or tendon adhesion restricting finger movement, arthrolysis or tenolysis may become necessary. In these circumstances, the implants can be removed at the same time.













