Plate fixation
1. Principles
Toe fractures versus long bone fractures
Toe fractures are different from long bone fractures.
- The bones are very small
- Fracture gaps are small
- Fixation devices don't need to counter large forces
Thus, following the AO principles is less critical than for long bones, and often isolated screws or K-wires alone will work satisfactorily.
Restoration of length, rotation, and angulation are important for cosmesis.
The hallux is particularly critical due to its importance for walking.
Simple fractures
The goal of fixation should be absolute stability.
Anti glide or buttress mode may be used for oblique fracture patterns (as illustrated).
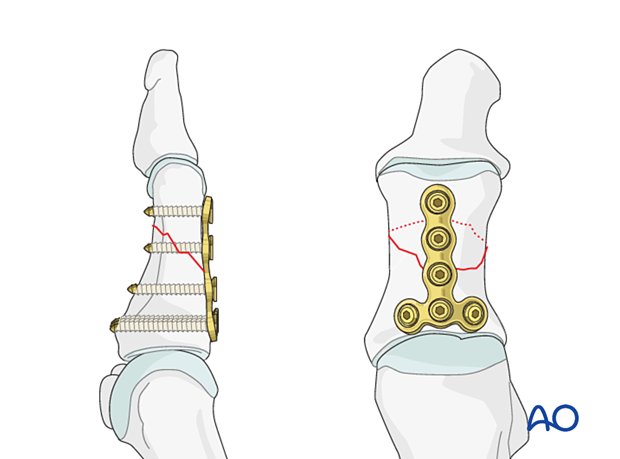
Wedge and comminuted fractures
Absolute stability can be performed for some complex patterns.
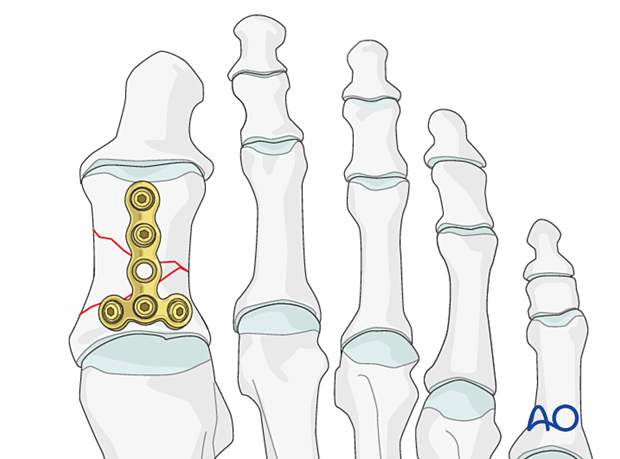
If extensive comminution is present, the plate should be used in bridging mode (relative stability).
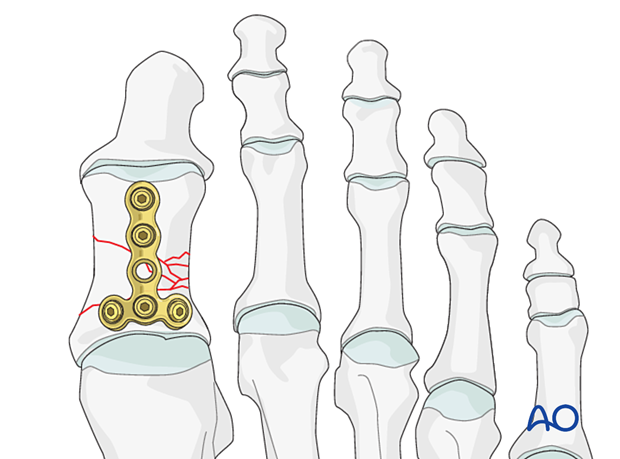
Hardware selection
A 2.0 or 2.4 T-plate (or straight plate) is typically used. The length of the plate should allow for the insertion of two screws in the distal segment.
Hardware placement
As a dorsal plate will cause less soft tissue irritation than a medial plate, some surgeons prefer dorsal plate application independently of the fracture patterns direction.
Timing of surgery
The timing of surgery is influenced by the soft tissue injury and the patient's physiologic status.
Dislocation or injuries associated with the skin at risk requires immediate intervention regardless of the amount of soft tissue swelling.
If possible, swelling should be significantly decreased before surgery, which can take up to two weeks in some instances.
Open fractures should be promptly irrigated and debrided, and treated with antibiotics. Definitive fracture fixation may not be possible during this setting.
Forefoot fractures do not contribute to physiologic instability. If there is no soft tissue at risk, urgent intervention is not required.
2. Patient preparation and approach
Patient preparation
This procedure is typically performed with the patient placed supine and the knee flexed 90°.
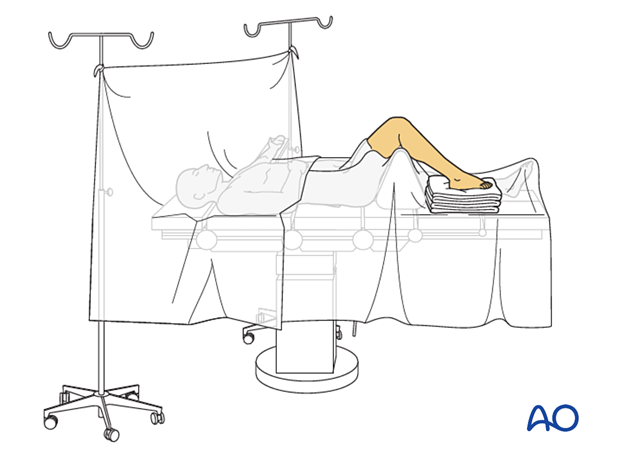
Approach
These fractures may be approached through either the:
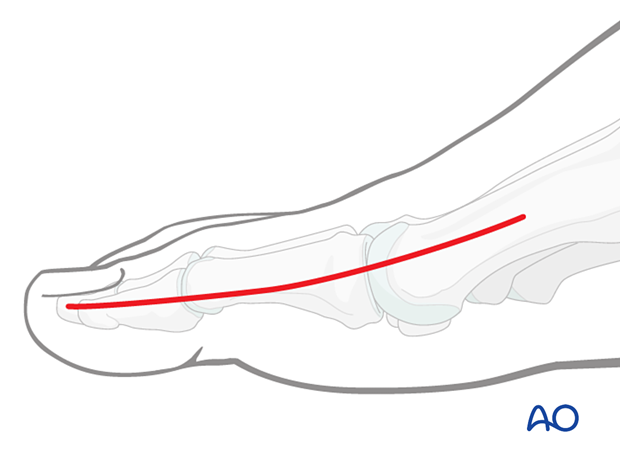
3. Reduction of multifragmentary fractures
The fracture will shorten through the comminuted region.
If there is a significant amount of comminution, length may be restored using indirect reduction techniques such as manual distraction or the use of a distractor.
After correct length, rotation, and angulation have been restored, a distractor will maintain the reduction, whereas a manual distraction will not.
The distraction pins should not interfere with the planned plate position and can be inserted medially.

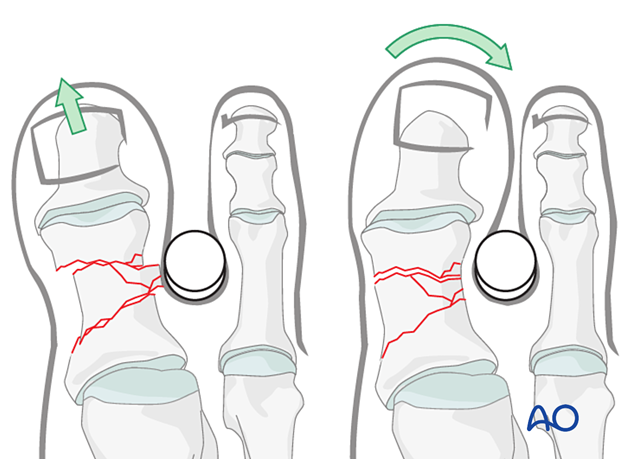
A sturdy cylindrical object at the fracture's apex can be used as a fulcrum to facilitate reduction.
If closed reduction is not successful, open reduction may be required.
Irrigation
Clean the fracture using a dental pick. Direct suction or irrigation is helpful.
The fracture edges are exposed, and the fragment mobility is assessed. It is essential to maintain the vascularity of small fragments.
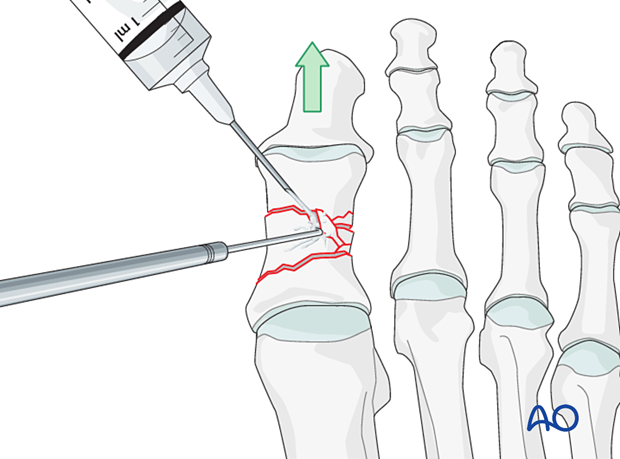
4. Reduction of simple and wedge fractures
Restore anatomical axial rotation, length, and angulation using one or more techniques below.
It is important to assess rotation to avoid interference with the adjacent toe during flexion.
Reduce the temporarily fix the fracture using reduction forceps.
Be careful not to apply excessive force as this can lead to fragmentation. If possible, apply the reduction clamp so that the forces created by the clamp are at right angles to the fracture line.

Insert a K-wire into one of the fragments and use it as a joystick for reduction. Once reduction is accomplished, the reduction is secured either using reduction forceps or by advancing the wire to secure the reduction (if possible).
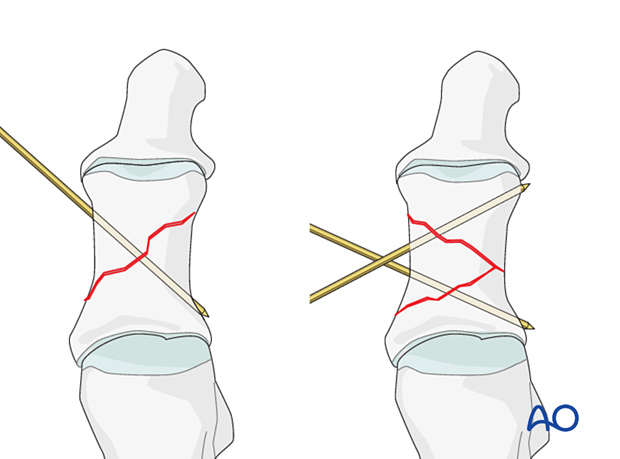
A periosteal elevator can be inserted at the fracture site and aid in reduction. The reduction can be secured either using reduction forceps or a K-wire.

5. Fixation
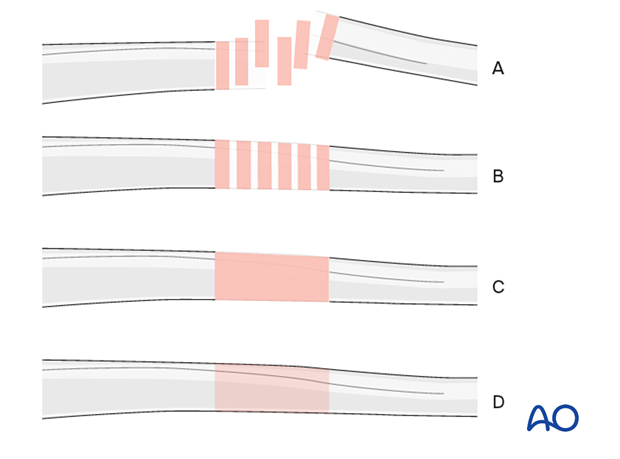
Throughout this treatment option, illustrations of a generic fracture pattern are shown in four different ways:
- Unreduced fracture
- Reduced fracture
- Fracture reduced and fixed provisionally
- Fracture fixed definitively
Bending and contouring the plate
The plate is contoured to approximate the shape of the normal dorsal surface of the proximal hallux.
The plate may be slightly over-bent for simple fractures to prevent a gap at the opposite cortex when tightening the screws.
The plate's T-end must be bent to follow the convexity of the dorsal surface of the base of the hallux.
A dorsal plate will generally cause less soft tissue irritation than a medial plate. Here, we will only demonstrate the application of a dorsal plate.

Plate application
The plate is placed distally enough from the fractured area to allow at least two screws to be inserted into the proximal segment.
Ensure that the plate is centered on the long axis of the diaphysis.
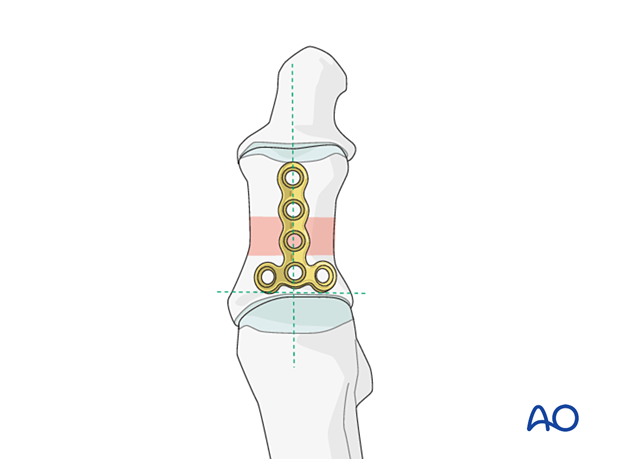
Proximal screw insertion
Insert the first screw but do not tighten it fully. Ensure that it engages the far cortex but does not protrude into the neurovascular bundle.
Check the transverse part of the plate in relation to the metaphysis and the long axis of the bone. Insert the second screw in the opposite hole of the transverse part of the plate. Sequentially tighten the screws in an alternating manner.

Convergent screws inserted in the transverse portion of the plate may block each other. The plate's T end may be given a slight twist to prevent this.
Joint penetration must be avoided.
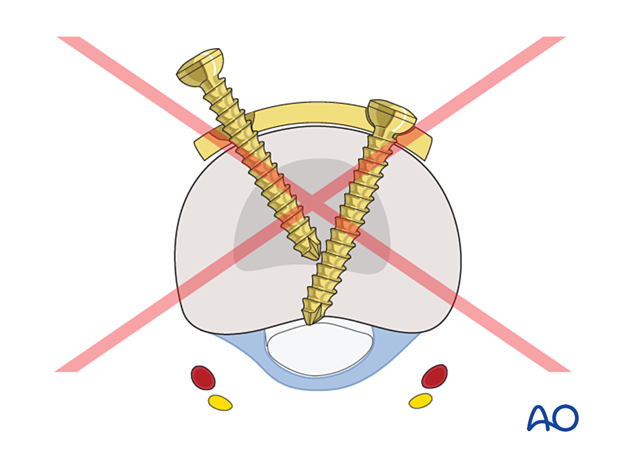
Distal screw insertion
Insert two screws in the shaft segment and verify length, alignment, and rotation. Remove any temporary fixation devices.
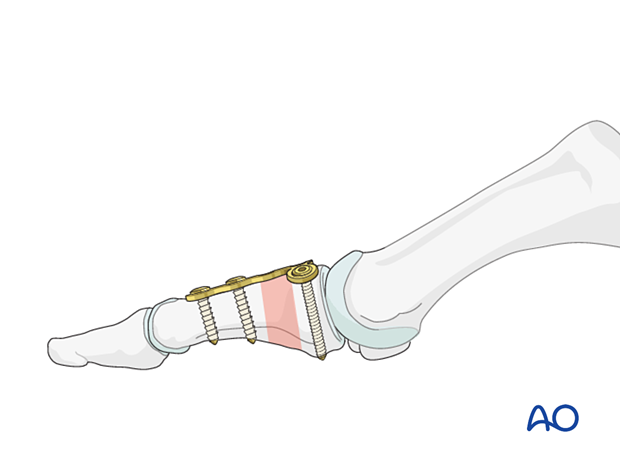
6. Aftercare
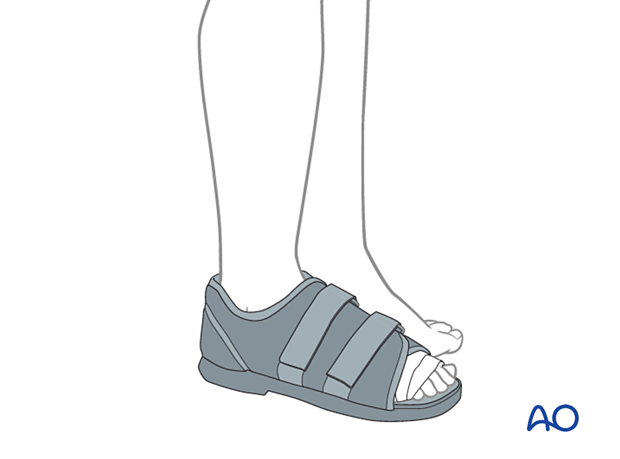
Weight-bearing may be allowed as long as the patient is provided with a flat, rigid sole shoe, which is continued for 6 weeks until x-rays or clinical examination is consistent with healing.
Provided that the fracture construct is stable, range of motion exercises (both actively and passively) may be initiated once soft tissues permit.