Supine position with knee flexed 90°
1. Introduction
This position is helpful for all procedures involving the toes, metatarsals, and the midfoot.
Careful pre-cleaning of the soft tissues should be performed, especially if gross contamination occurs.
2. Preoperative preparation
Operating personnel need to know and confirm:
- Verify site and side of fracture with the patient along with the type of operation planned
- Ensure that the surgeon has marked the operative site
- Implant to be used
- Patient positioning
- Details of the patient (including a signed consent form and appropriate antibiotic and thromboprophylaxis)
- Comorbidities, including allergies
3. Anesthesia
This procedure is performed with the patient under general or regional anesthesia.
If a spinal anesthetic is used, the surgeon and anesthetist need to be confident that the procedure will last the duration of the anesthetic.
Long-acting pain blocks for the injured leg should be avoided if there is a risk of compartment syndrome, as this could hide symptoms of a subsequent compartment syndrome.
4. Prophylactic antibiotics
Perioperative antibiotics are required for all open procedures. The standard first-generation cephalosporin is given before surgery and may be readministered for up to 24h. Antibiotics are administered according to local antibiotic policy and specific patient requirements.
Many surgeons use a Gram-positive prophylactic antibiotic cover for closed fractures, adding Gram-negative prophylactic coverage for open fractures.
5. Tourniquet
Thigh or calf tourniquets can help minimize blood loss and improve the view of the articular surface. In the trauma patient, the surgeon must consider the effects of ischemia/reperfusion and the potential effects of tourniquet use in the presence of a compromised soft-tissue envelope and compromised vascular supply.
Consideration of tourniquet use should be part of the preoperative planning process.
The tourniquet should not be left on longer than 120 minutes and shorter in older patients or those with known vascular disease.
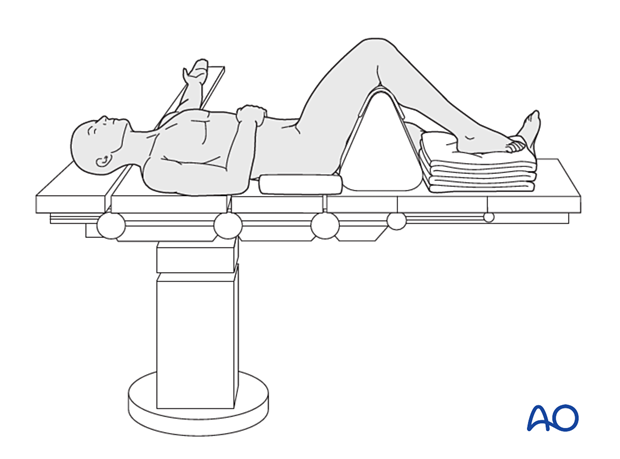
6. Patient and x-ray positioning
- Place the patient supine on a radiolucent operating table
- Depending on the surgeons' preference, the knee may be flat on the bed or flexed 90° over a well-padded triangle
- The injured foot should be positioned at the end of the table
- A bump is placed under the ipsilateral hip to orient the foot vertically
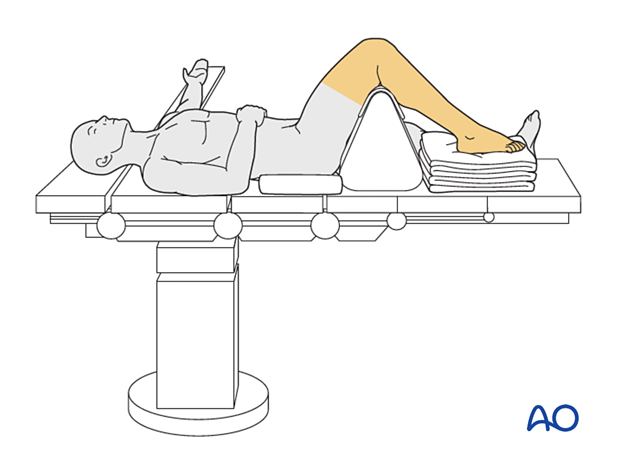
- The injured foot may be elevated by placing it on top of a support to facilitate imaging
- If used, a tourniquet is placed
- Ensure that soft tissues, skin pressure points, and the subcutaneous nerves (peroneal nerve of the opposite knee) are well protected
- Adjust the operating table to the appropriate height and place the image intensifier on either side of the injury. If only operating on the hallux, it may be easier to bring in the C-arm from the same side as the operative leg

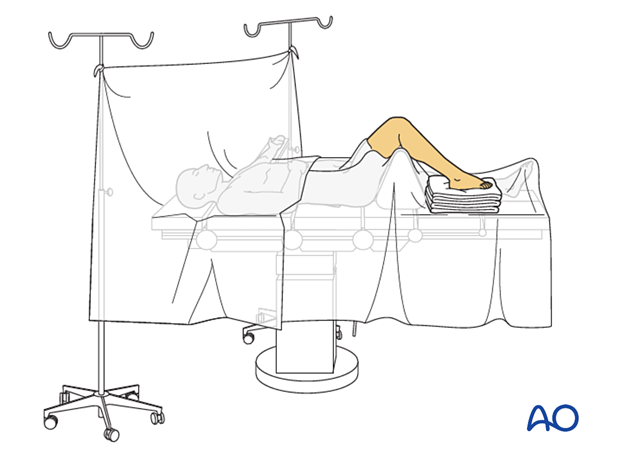
7. Skin disinfecting and draping
Disinfect the expected operating field, including the entire foot, with the appropriate antiseptic.
- Use either a U-drape or an extremity drape
- Drape the image intensifier
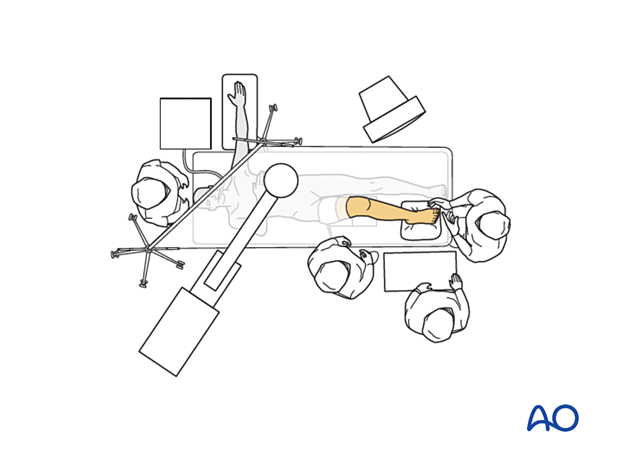
8. Operating room set-up
The surgeon and the ORP stand at the end of the bed. The assistant stands next to the surgeon.
Place the display screen in full view of the surgical team and the radiographer.