MIO - Bridge plating (DSC)
1. Principles
Note on illustrations
Throughout this treatment option illustrations of generic fracture patterns are shown, as four different types:
A) Unreduced fracture
B) Reduced fracture
C) Fracture reduced and fixed provisionally
D) Fracture fixed definitively
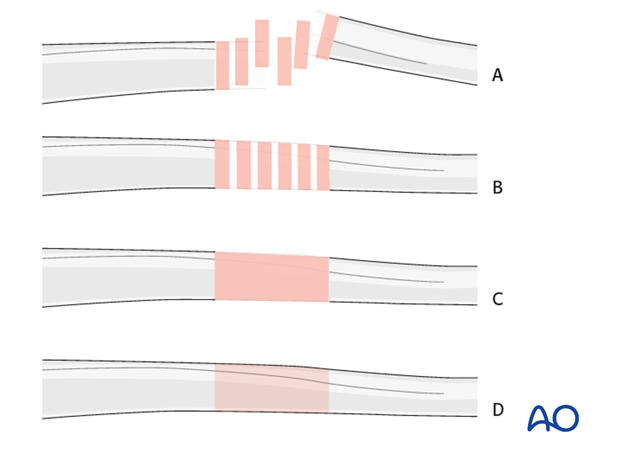
Bridge plating
Bridge plating uses the plate as an extramedullary splint, fixed to the two main fragments, leaving the intermediate fracture zone untouched. Anatomical reduction of intermediate fragments is not necessary. Furthermore, their direct manipulation would risk disturbing their blood supply. If the soft tissue attachments to the fragments are preserved, and the fragments are relatively well aligned, healing is enhanced.
Alignment of the main shaft fragments can be achieved indirectly with the use of traction and the support of indirect reduction tools, or indirectly via the implant.
Mechanical stability, provided by the bridging plate, is adequate for gentle functional rehabilitation and results in satisfactory indirect healing (callus formation). Occasionally, a larger wedge fragment might be approximated to the main fragments with a lag screw.
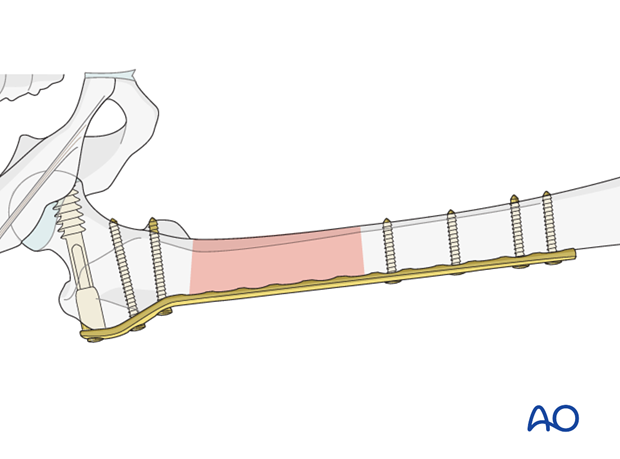
Bridge plate
Bridge plates inserted through a minimally invasive (MIO) approach leave the soft tissues intact over the fracture site. The incisions are made proximally and distally, and the plate is inserted through a submuscular tunnel. This normally requires fluoroscopic intensifier monitoring.
The DCS implants can be placed with locking or non-locking screws, but locking screws should only be used where osteoporotic bone is present.

Reduction
It is important to restore axial alignment, length, and rotation.
Reduction can be performed with a single reduction tool (eg, large distractor), or by combining several steps (for example fracture table +/- external fixator, +/- reduction via the implant, +/- cerclage wiring, etc.) to achieve the final reduction.
The preferred method depends on the fracture and soft-tissue injury pattern, the chosen stabilization device, and the experience and skills of the surgeon.
If a large fragment has separated from the fracture zone and impaled the adjacent muscle, direct reduction may be required.
2. Patient preparation
The patient may be placed in one of the following positions:
3. Approach
For this procedure a MIO approach is used.
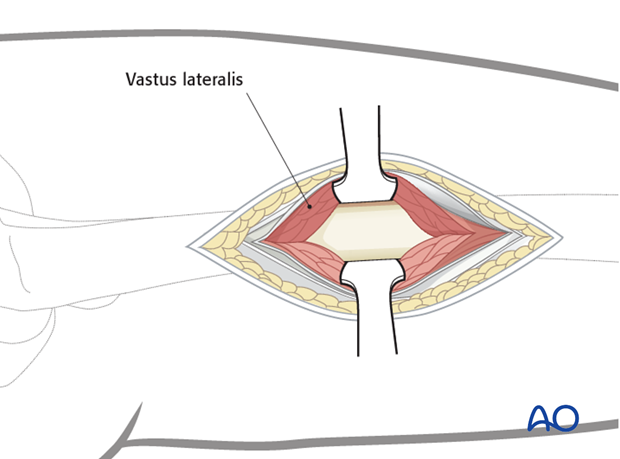
4. Preliminary reduction
General considerations
Subtrochanteric fractures present a particular problem in terms of fracture reduction and alignment. Due to the strong pull of the iliopsoas muscle, the proximal fragment is flexed and externally rotated and therefore difficult to control. This may even require open reduction maneuvers to ensure a proper alignment.
If a closed plating technique is used, a preliminary reduction should be undertaken before plate insertion. Once the plate is attached to the proximal fragment, the definitive reduction with respect to length, rotation and axis can be achieved.
For the preliminary reduction several options are available:
- Lowering the proximal fragment by using external pressure with a mallet.
- A Schanz screw inserted into one of the main fragments.
- Use of a distractor / external fixator.
- Use of cerclage wiring
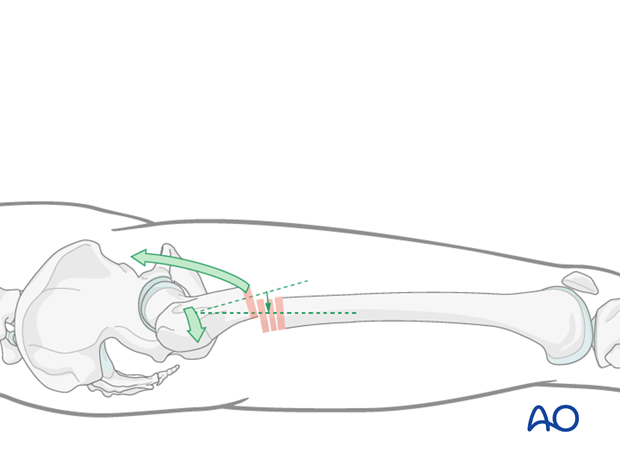
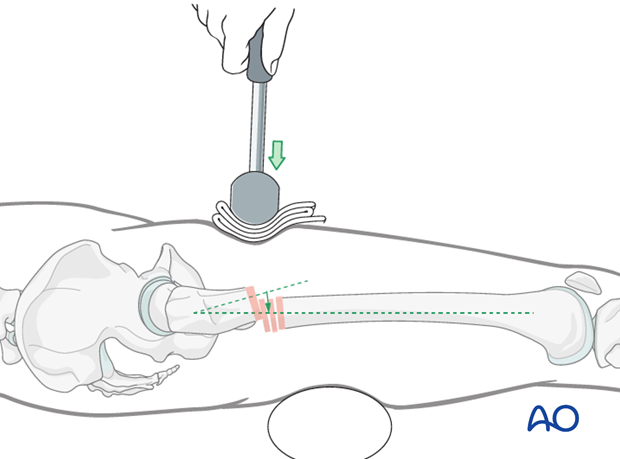
Extension of the flexed proximal fragment by use of a mallet
A mallet may be used, but this will be difficult if the proximal fragment is short.
A crutch can be used under the proximal end of the distal fragment.
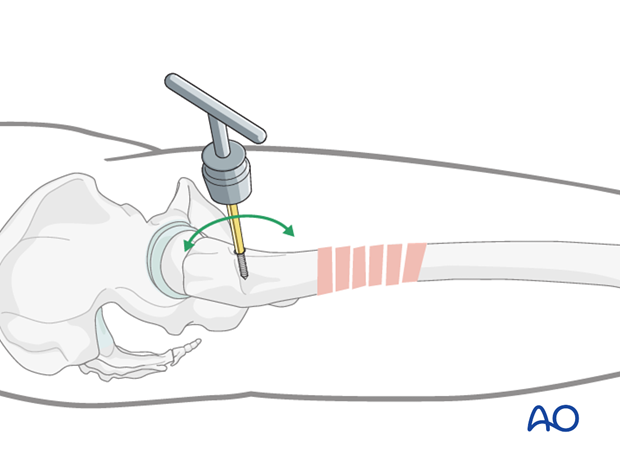
A Schanz screw inserted into one of the main fragments
A monocortical Schanz screw can be helpful in providing direct control of the displaced main fragments. It is advantageous when compared with reduction maneuvers through the skin.
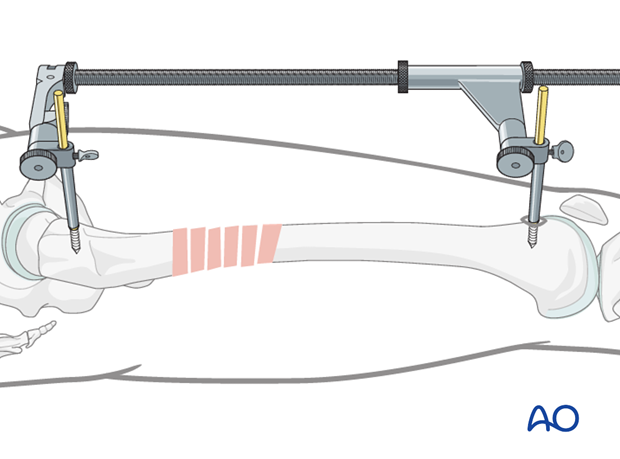
Use of a large distractor
After placement of two pins - one in the greater trochanter and the other in the shaft - the large distractor is attached. Attention must be paid so that the pins do not conflict with the later plate position.
In case of a closed procedure, every step of the reduction should be verified by image intensifier control.
The preliminary reduction is held by tightening the clamps of the large distractor.
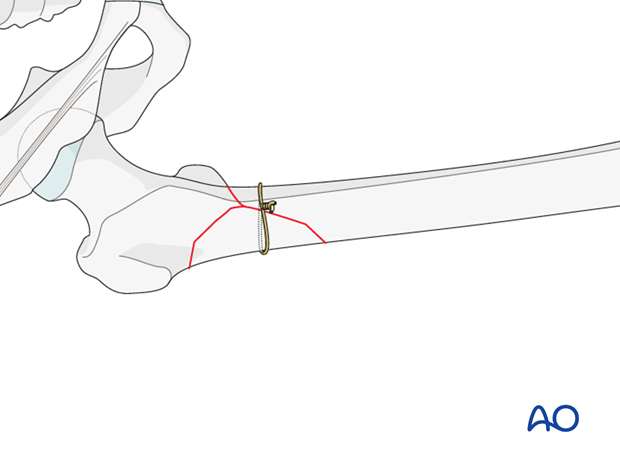
Cerclage wire
To supplement a reduction of an intact wedge fracture, a cerclage wire may be very complimentary through a minimal incision.
Teaching video
AO teaching video: Application of the large distractor
5. Preoperative planning
Plate length and number of screws
Depending on the extent of the zone of fracture comminution and the underlying bone stock (osteoporosis), the appropriate plate length is chosen. Sufficient bicortical screws (a minimum of three up to six) should be inserted in each fracture fragment. Relative stability results from leaving plate holes empty over the fracture zone.

6. Plate fixation to proximal fragment
Guide wire insertion
As a first step, a guide wire for the condylar screw is inserted proximally.
The aiming device is lined up parallel to the femoral neck in both the axial, and the AP views, the guide wire is aimed at the lower portion to the femoral head. The wire is advanced to just short of the subchondral bone of the femoral head. Its position is checked fluoroscopically, and adjusted, if necessary.
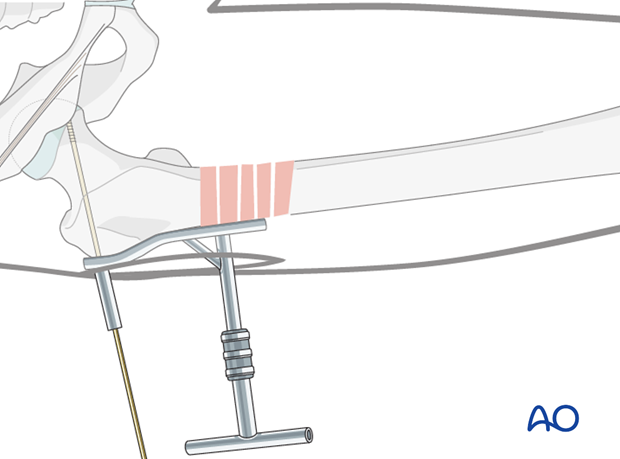
Reaming
After indirect measurement of the guide wire insertion depth using the measuring device, drilling is performed over the guide wire with a triple reamer, adjusted to the correct length.
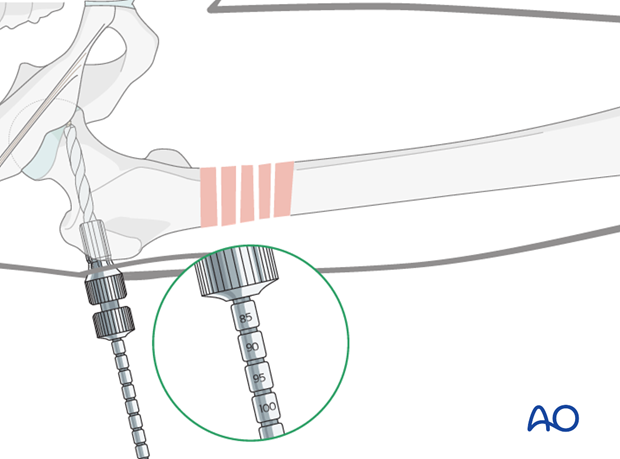
Preliminary screw insertion
The following steps are recommended for the minimally invasive technique.
First, the condylar screw is inserted so that its outer end is still visible outside the lateral cortex.
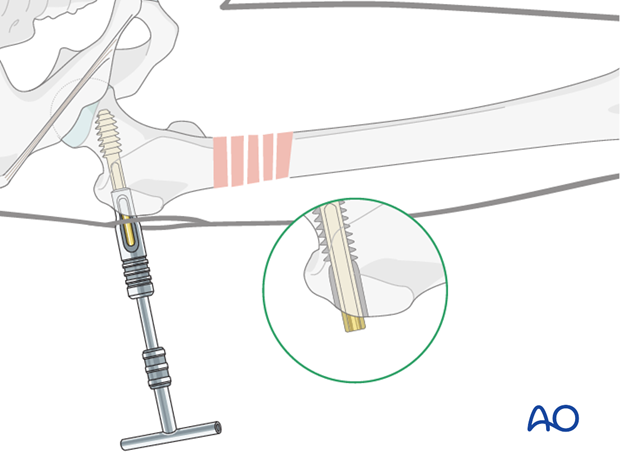
Plate placement
Next, the T-handle is detached, and the plate is inserted sub-muscularly from proximal to distal.
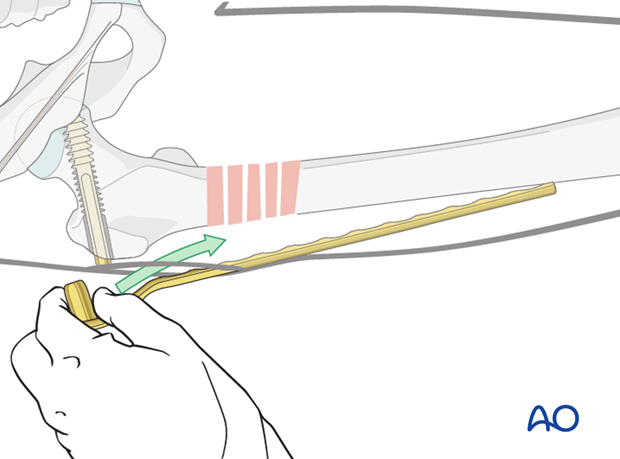
Pearl: preparation of the plate tunnel
Three options are in use for preparation of the plate path in the distal main fragment.
- Insert a long pair of scissors, spread them, and then pull backwards.
- Insert a periosteal elevator and slide it extraperiosteally along the distal main fragment. (The tip of the plate can be used in a same manner).
- A soft-tissue retractor is available which serves the same purpose (as illustrated).

Plate and screw combination
The T-handle is then inserted through the barrel of the plate and reconnected to the condylar screw. This can be challenging and often requires abandoning the preliminary reduction.

Final screw placement
When the screw is in the final position (when the T-handle is parallel to the long axis of the proximal shaft fragment in the lateral view), the barrel is placed fully over the screw, and the T-handle then removed.

Plate fixation with cortical screw
After verification of the correct plate position, a cortical screw is inserted to secure the plate to the proximal fragment.
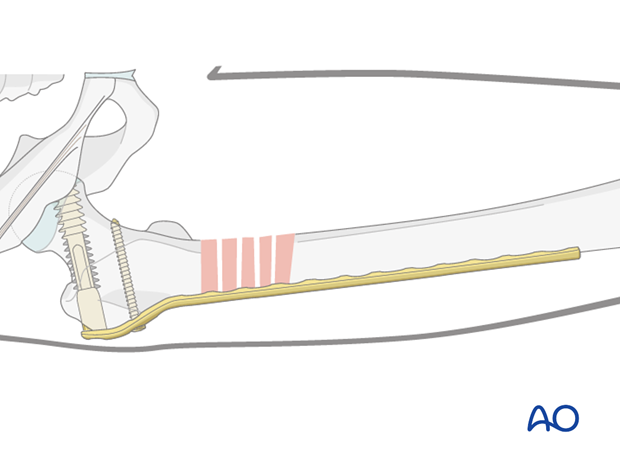
7. Plate fixation to distal fragment
Verification of reduction
Under image intensifier control, the preliminary reduction is again checked with respect to axial alignment, and length and, to a degree, the rotation (in more complex fractures, judging the clinical accuracy of the rotation becomes more important, while at the same time the associated radiological findings can be challenging to interpret).
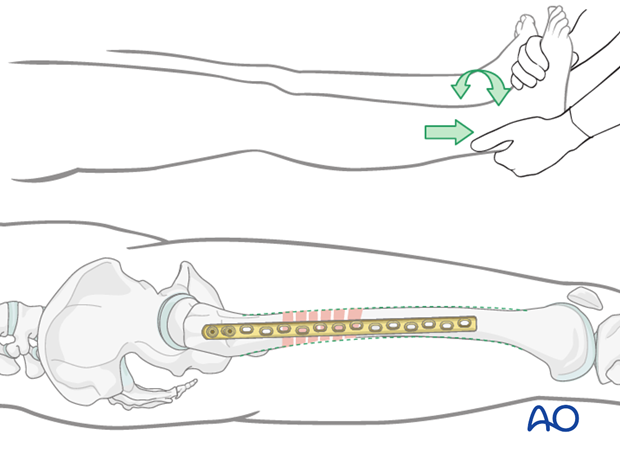
The illustration shows the distal main fragment incompletely aligned.
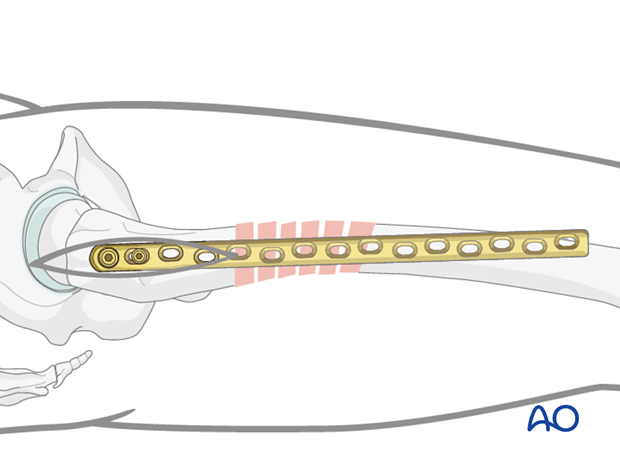
Insertion of first screw into distal fragment
The approaches / stab incisions over the distal fragment are made according to the planned final screw placement.
Two blunt Hohmann retractors placed ventrally and dorsally around the femoral shaft can help to control the lateral position of the plate.
If the overall reduction is found to be sufficient, the first cortical screw in the distal fragment is placed without being fully tightened. This allows additional fine tuning of the plate position.
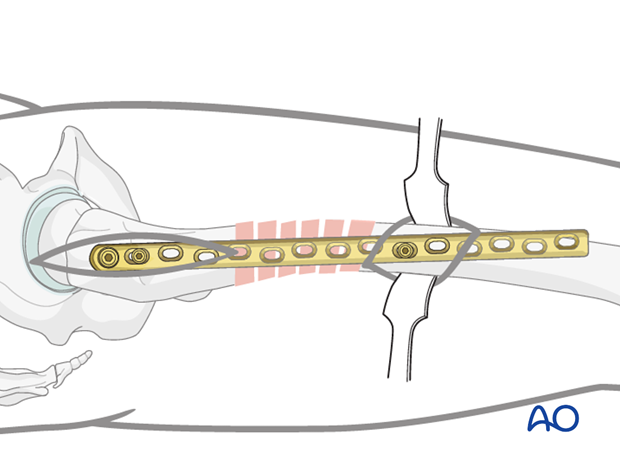
Pearl: final reduction
If the fracture fragments are incompletely reduced laterally, the use of sterile bolsters is recommended.
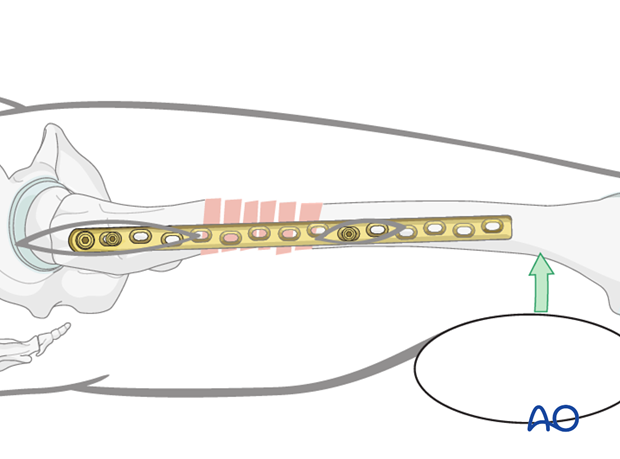
Insertion of second screw into distal fragment
Once the most distal screw has been inserted, the first screw in the distal main fragment is fully tightened.

Additional screw placement
According to preoperative planning, additional screws are inserted into the proximal and distal main fragments.

8. Aftercare
Compartment syndrome and nerve injury
Close monitoring of the femoral muscle compartments should be carried out especially during the first 48 hours, in order to rule out compartment syndrome.
Postoperative assessment
In all cases in which radiological control has not been used during the procedure, a check x-ray to determine the correct placement of the implant and fracture reduction should be taken within 24 hours.
Functional treatment
Unless there are other injuries or complications, mobilization may be started on postoperative day 1. Static quadriceps exercises with passive range of motion of the knee should be encouraged. If a continuous passive motion device is used, this must be discontinued at regular intervals for the essential static muscle exercises. Afterwards special emphasis should be placed on active knee and hip movement.
Weight bearing
Full weight bearing may be performed with crutches or a walker.
Follow-up
Wound healing should be assessed regularly within the first two weeks. Subsequently a 6 and 12 week clinical and radiological follow-up is usually made. A longer period may be required if the fracture healing is delayed.
Implant removal
Implant removal is not mandatory and should be discussed with the patient, if there are implant-related symptoms after consolidated fracture healing.













