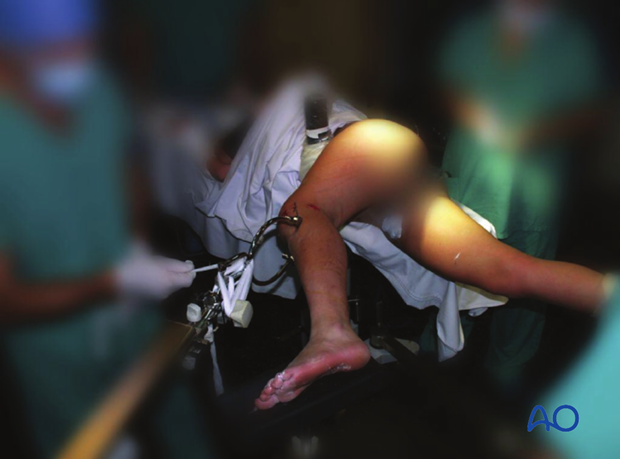
Lateral decubitus position
1. Lateral decubitus position with traction of the affected leg
This position is recommended for very proximal fractures because finding the nail entry-point is easier. However, it is more time consuming and iatrogenic injuries to the pudendal nerve have been documented, due to prolonged or excessive traction. This position is also recommended for obese patients.
Careful pre-cleaning of the soft tissues should be performed especially if gross contamination occurs.
2. Preoperative preparation
Operating room personnel (ORP) need to know and confirm:
- Site and side of the fracture
- Type of operation planned
- Ensure that the operative site has been marked by the surgeon
- Condition of the soft tissues (fracture: open or closed)
- Implant to be used
- Patient positioning
- Details of the patient (including a signed consent form and appropriate antibiotic and thromboprophylaxis)
- Comorbidities, including allergies
3. Anesthesia
This procedure is performed with the patient under general or regional anesthesia
Long-lasting postoperative complete pain blocks for the patient with injured leg should be avoided as this could hide symptoms of a subsequent compartment syndrome.
4. Positioning
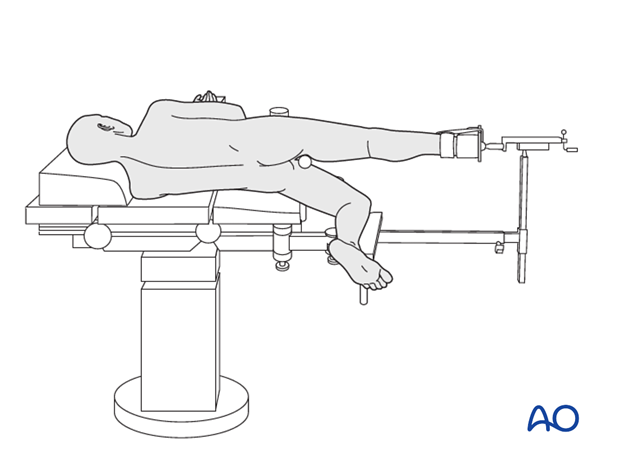
- Reconfigure the fracture table to establish the lateral decubitus position and transfer the patient to a fracture table.
- Position the fractured leg with traction in a 20° hip flex position with traction.
- The unaffected leg goes underneath the traction post and is in a 20° hip extension position with the knee flexed or in a traction boot.
- Reduce the fracture with traction and manipulation before preparing and draping the patient.
- Pad all pressure points carefully (down elbow and in the groin). Place the ipsilateral arm across the chest to be out of way.
- Position the image intensifier on the opposite side of the injury and the operating surgeon.
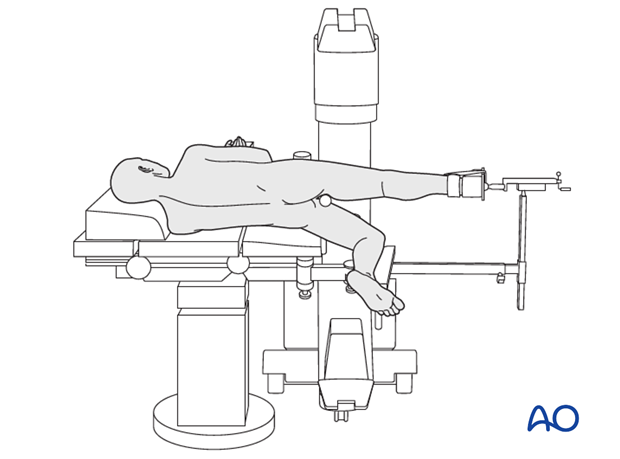
- Ensure that you can get good-quality AP (illustrated) and lateral x-ray views of the entry point (piriform fossa), fracture site, and distal femur before draping.
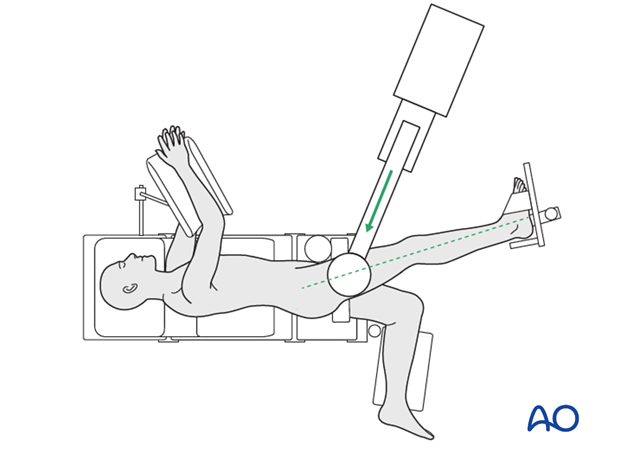
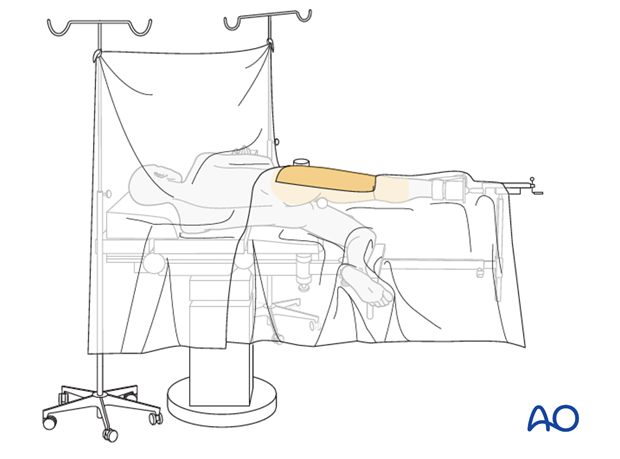
5. Skin disinfecting and draping
- Maintain traction on the limb during preparation to avoid excessive deformity at the fracture site.
- Disinfect the exposed area from above the iliac crest to the mid-tibia with the appropriate antiseptic.
- Ensure the adhesive portion of the drape is large enough to reach from the iliac crest to the knee joint to allow distal locking.
- Place the image intensifier on the nonsterile side of the exclusion drape.
- Traditional drapes may be used. Ensure a waterproof environment for the operative site.
- Drape the image intensifier.
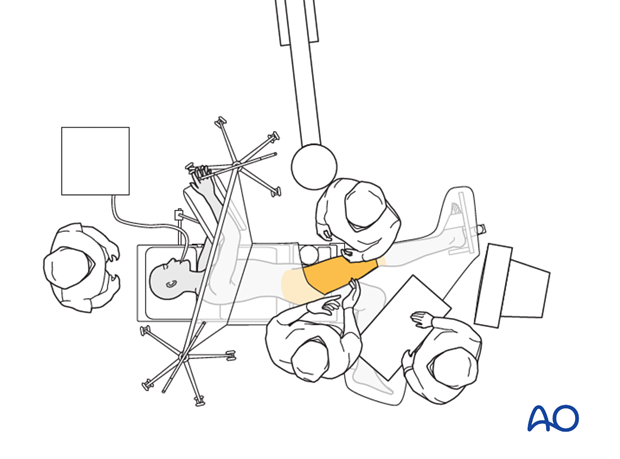
6. Operating room set-up
- Position the operating table (if feasible) within the operating room to allow maximum space on the operating side for the surgeon, staff, and trolleys.
- The surgeon and the ORP stand on the side of the injury. The Assistant may be on either side.
- Place the image intensifier on the opposite side of the patient, perpendicular to the patient.
- Place the image intensifier display screen in full view of the surgical team and the radiographer
7. Additional traction at knee joint
Alternatively, additional traction at the knee joint may be applied to take account of any flexion of the proximal fracture fragment.