MIO - Antegrade nailing
1. Patient preparation and approach
Patient positioning
This procedure may be performed with the patient placed supine.
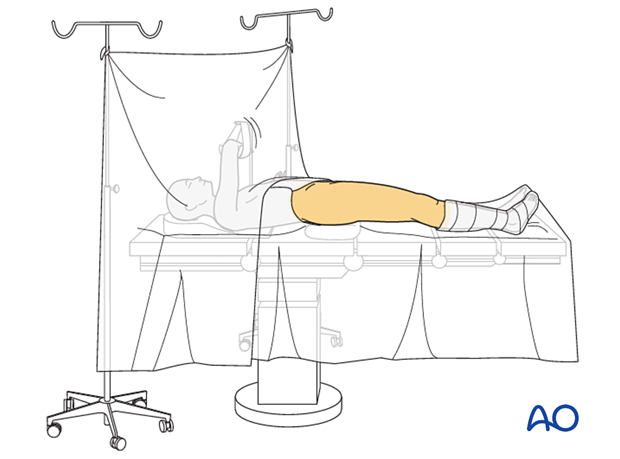
Surgical approach
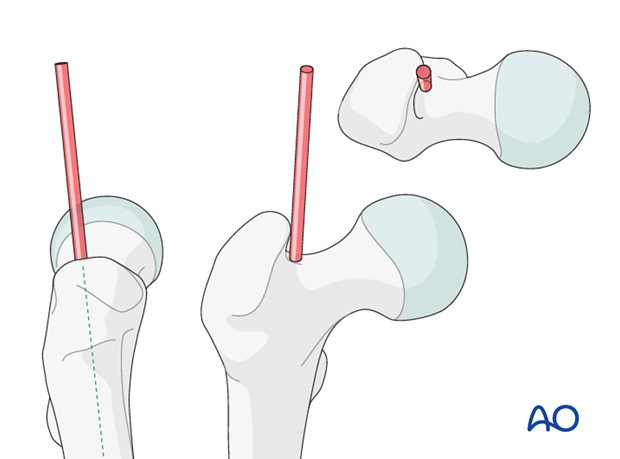
The piriformis entry point is used for straight nails.
The trochanteric entry point is used for proximally curved nails.
2. Reduction
General considerations
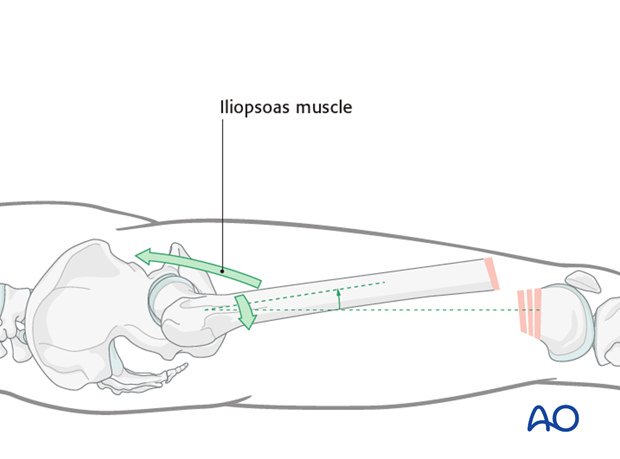
In more proximal fractures, due to the pull of the iliopsoas muscle, the upper main fragment may be flexed and externally rotated, and the distal segment lies posteriorly due to gravity.
Reduction is performed under image intensification.
Several options for fracture reduction can be considered:
- Elevation of the distal fragment by use of a crutch.
- Lowering of the proximal fragment by external pressure from a mallet.
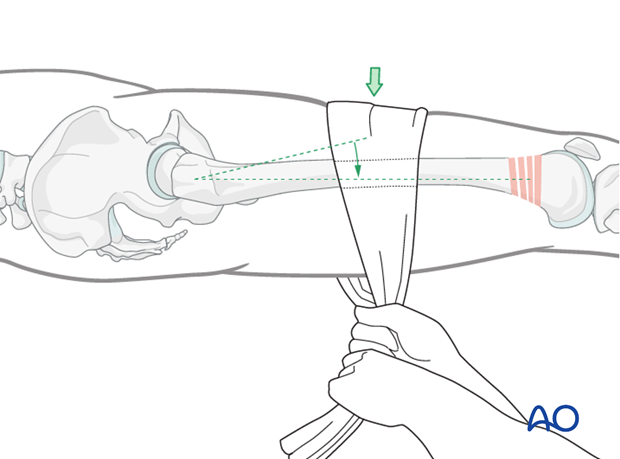
- A wrap around the femur. A sustained pull will help in reduction.
- A Schanz screw inserted into one of the fragments.
- Use of a bone hook.
- (Manual reduction)
- Poller screws
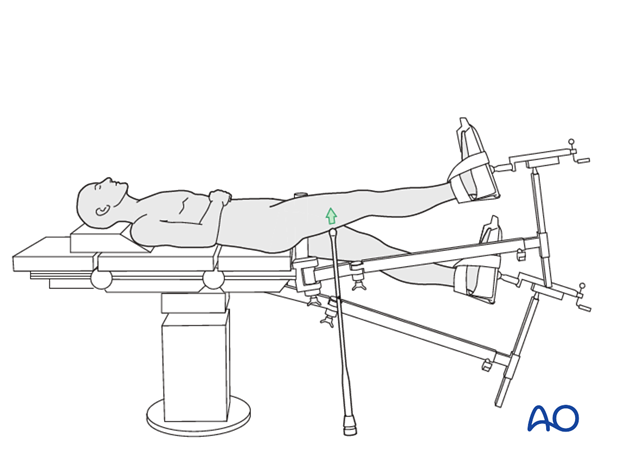
This option may only be used if the patient is on traction in a scissor position. A crutch is slid beneath the distal main fragment to elevate it to the level of the proximal fragment.
Firm manual pressure is usually required to achieve fracture reduction.
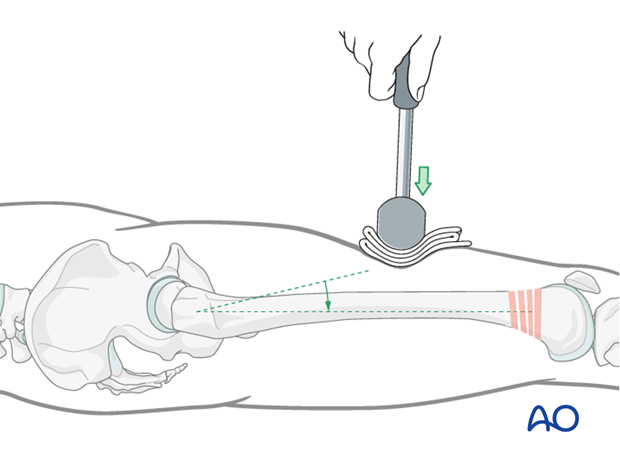
Based on the nature of the fracture, the wrap is usually placed around the larger fragment.
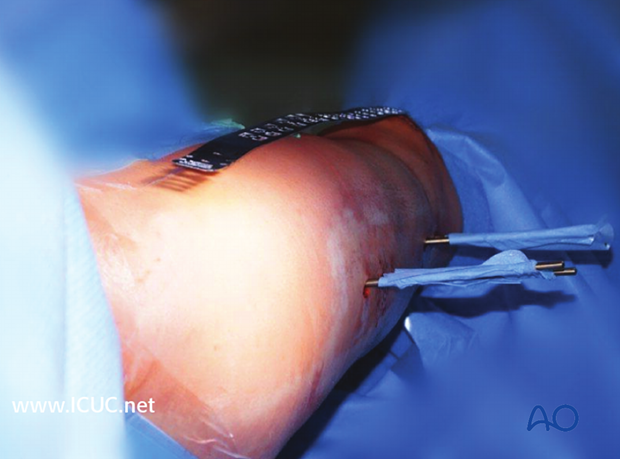
A monocortical Schanz screw (preferably 5 mm) can be helpful for providing direct control of the displaced fragments. It is superior to reduction maneuvers through the skin.
Collinear clamp
Depending on the fracture morphology, reduction of the distal femur can also be achieved using a collinear clamp.

Reduction using a bone hook with minimal incision is advised.
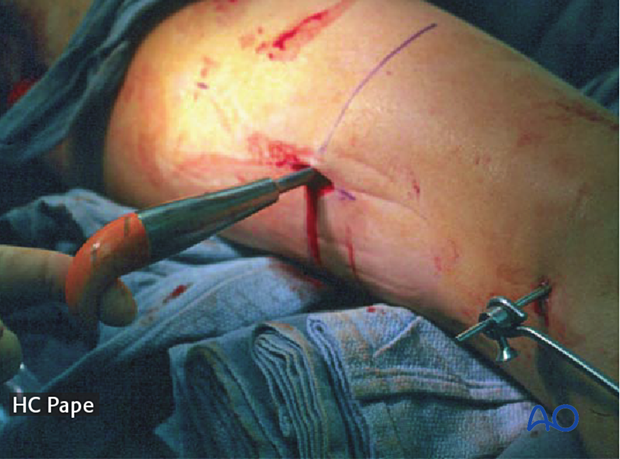
Manual reduction is not recommended as radiation of the surgeon‘s hands may be unavoidable and reduction cannot be maintained during nailing.
Guide wire insertion
A guide wire is advanced into the distal main fragment until it is about 5 mm proximal to the intercondylar notch. It is important that the guide wire be centered to prevent eccentric reaming and subsequent malposition of the nail, which can result in varus/valgus/antecurvatum/retrocurvatum malalignment.
Unreamed nailing does not require a guide wire. When unreamed nailing is performed, the nail is used as a reduction tool.
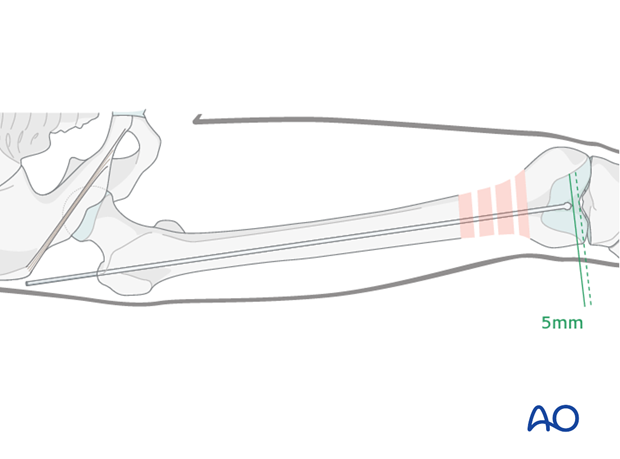
Guide wire inserted down the femur before reduction of femur shaft and nailing.
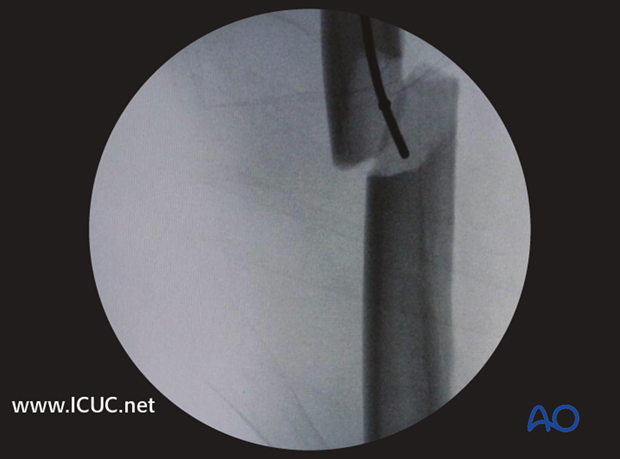
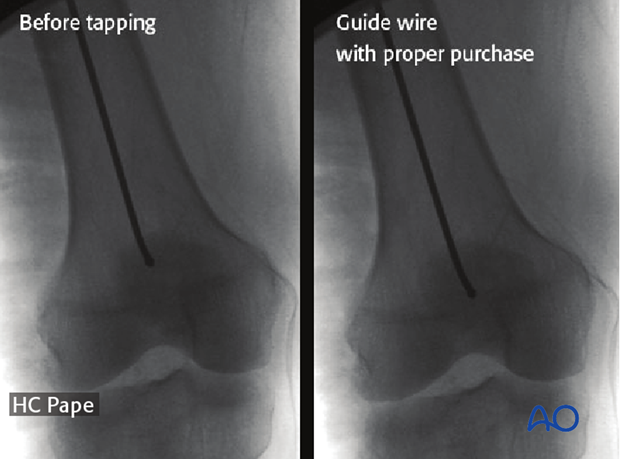
To ensure maintenance of alignment of the K-wire throughout the reaming process, it may be gently tapped to provide purchase in the cancellous subchondral bone. If this is not achieved, the guide wire may displace on removal and exchange of the reamers.
Teaching videos
AO teaching video: Femur - Shaft fractures - Intramedullary Nailing with the Antegrade Femoral Nail (AFN)
AO teaching video: Femur—Shaft fracture 32-B2 Intramedullary nailing with the Expert Lateral Femoral Nail (LFN)
3. Poller screw (blocking screw)
General considerations
The concept of a Poller screw is based on the principle that the malalignment induced by oblique, proximal and distal fractures can be counteracted by the nail-directing effect of the screw. Therefore, its position should aim to counteract the displacement of the fracture. Most often it is therefore placed in the short side in the distal fragment. If there is a wide canal, two screws can be placed on either side of the path of the nail.
It is advisable to insert the poller screw prior to reaming, and in case of unreamed nailing, prior to nail insertion, to provide adequate contact between the nail and the screw. If the poller screw is inserted after reaming, the path of the nail is already set and the poller screw will not work. A small fracture screw or a locking screw can be used as a poller screw, depending on the local anatomy.
The reaming process in the presence of the poller screw must be performed very carefully in order not to harm the reamer tip.
The most frequent indication for poller screws is a proximal or distal oblique fracture which tends to shift when the axial knee blow technique is used to close any fracture gap, or when the patient is mobilized.
In these cases, prophylactic poller screws are very helpful.
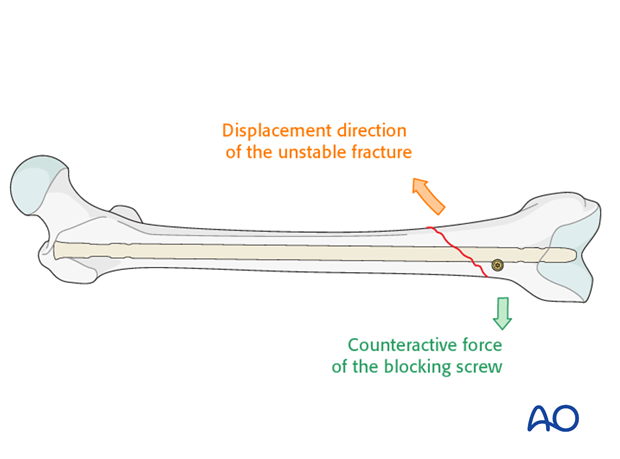
Distal oblique fractures
The muscular forces in oblique fractures try to displace the fracture. The blocking screw counteracts these forces when properly positioned on the short side of the distal fragment.
4. Determine nail length and diameter
Determine nail length via guide wire (only with reamed nailing)
The correct length of the nail is determined by comparing a second guide wire to the one that has been inserted. The correct placement of the guide wire in the distal canal should be assessed via image intensifier. Additionally, the second guide wire must be positioned in contact with the greater trochanter. This must be verified by image intensifier as well.
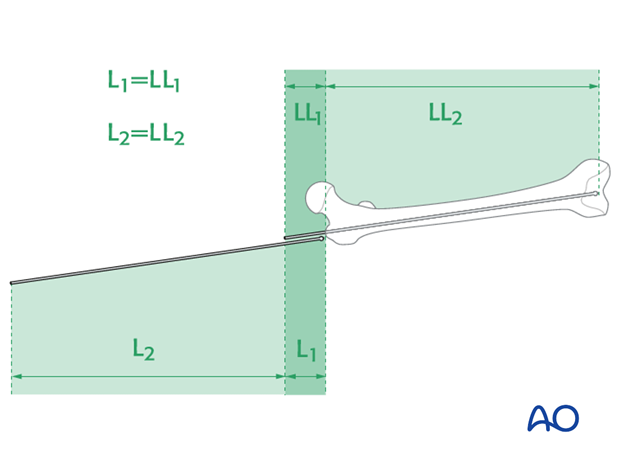
Radiographic ruler
Alternatively, a radiographic ruler may be used.
The tip of the ruler should be positioned in the center of the distal end of the femur. Nail length is determined by the position of piriformis fossa, not by the tip of the greater trochanter.
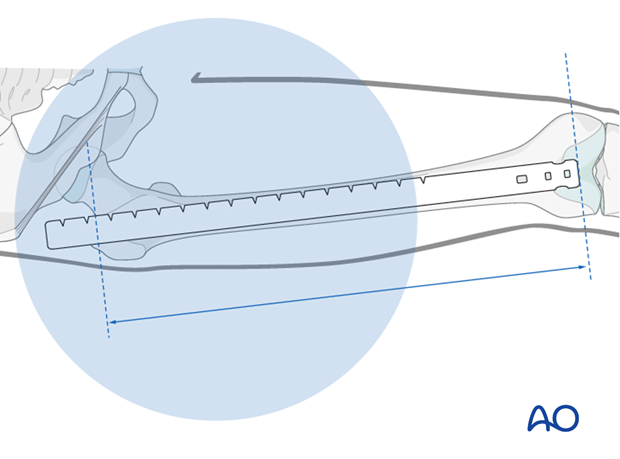
It is important to visualize the fracture zone by image intensifier to ensure that adequate restoration of femoral length has been achieved.
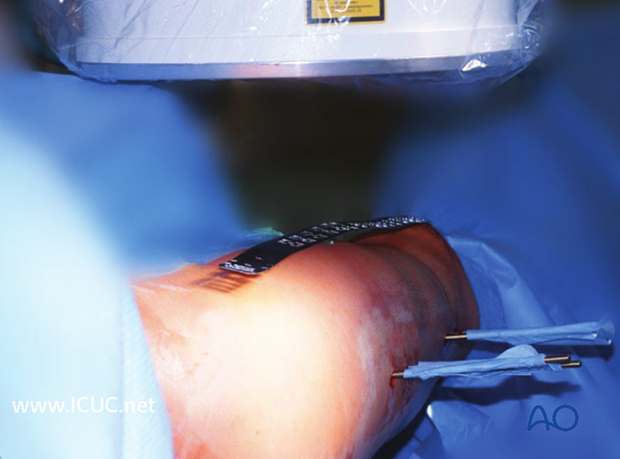
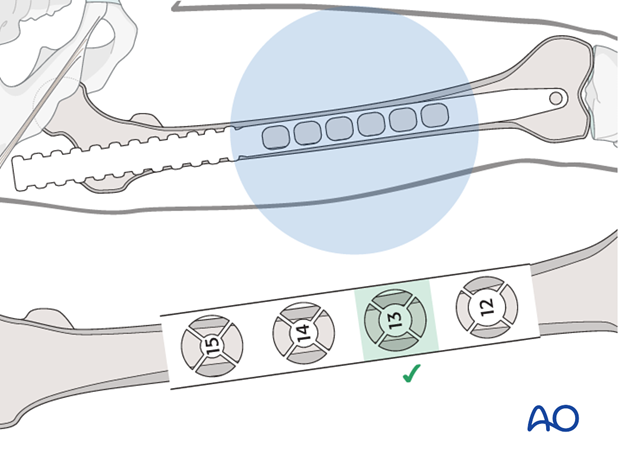
Nail diameter
It is important to measure the medullary diameter at the mid portion of the femur, which represents the narrowest segment of the medullary canal.
The inner cortical edge should touch with the inner numbered disk of the ruler aperture. In the illustration an inner cortical diameter of 14 mm is shown.
Consideration for special situations
In multifragmentary fractures, or in open fractures with bone loss, it is safer to perform preoperative planning on the uninjured leg. In bilateral femoral fractures, the less comminuted side should be used to determine the length and diameter of the nail.
5. Reaming
Insertion of reaming rod
After the tissue protector has been introduced, the reaming shaft, fitted with the first reamer head, is inserted over the guide wire. Reaming begins with a 9 mm end cutting medullary reamer.
Sequential reamer size increase
Reaming is performed in sequential steps by increments of 0.5 mm each.
As soon as chatter from cancellous bone can be felt and heard, the inner cortex has been reached. This may not be the case in segmental fractures or when severe comminution is present.
Adequate reaming must be performed to allow for smooth nail insertion. For example, for a nail width of 10 mm, reamers of up to 10.5 or 11 mm diameter are used. If a very tight fit of the reamer can be detected before the desired reaming size is reached, one should consider using a smaller nail than previously planned.
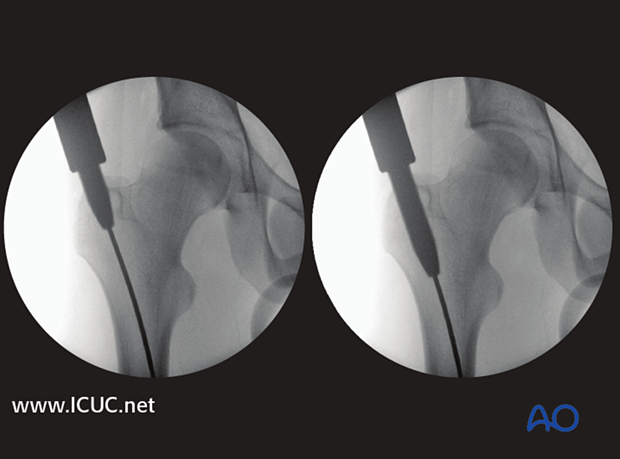
Eccentric reaming
Eccentric reaming can cause weakening of the adjacent cortex which may interfere with healing or even cause a fatigue fracture.
Trapping of reamer by slow spinning
If the reamer becomes trapped while reaming, it must be gently removed by the most senior surgeon, because breakage of the reamer tip in this situation can be a devastating complication.
Heat necrosis by overaggressive reaming
Overaggressive reaming should be avoided because it may cause heat necrosis of the femoral canal. This applies especially for narrow midshaft canals (9 mm or less in diameter).
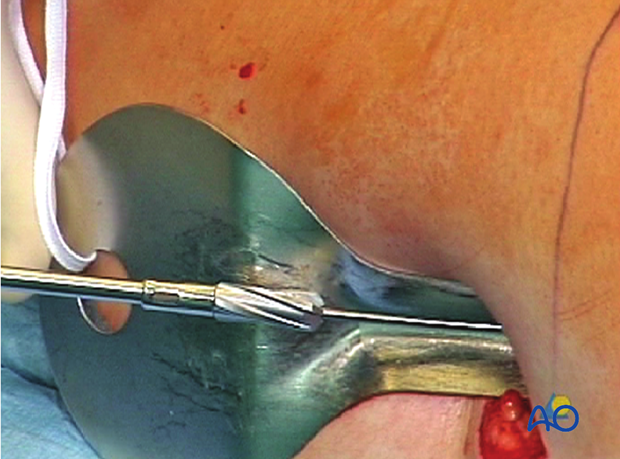
Rapid thrusting/systemic fat embolization
Care should be taken to use sharp reamers, to advance the reamers slowly, and to allow sufficient time between reaming steps for the intramedullary pressure to normalize. Rapid thrusting of the reamer may worsen the intramedullary pressure increase that is observed during nailing. This image demonstrates fat extrusion in a human cadaver specimen with a window in the proximal section.
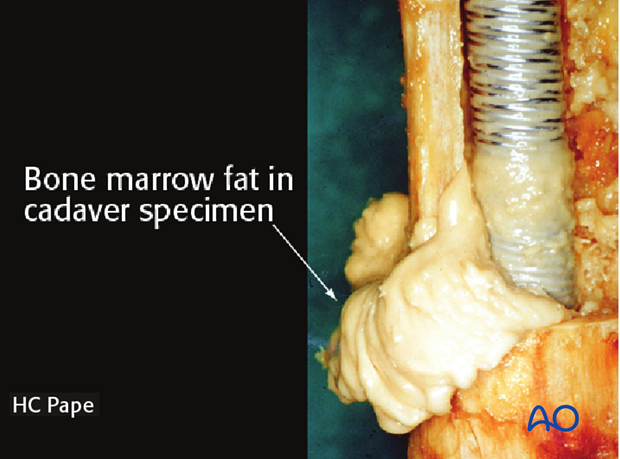
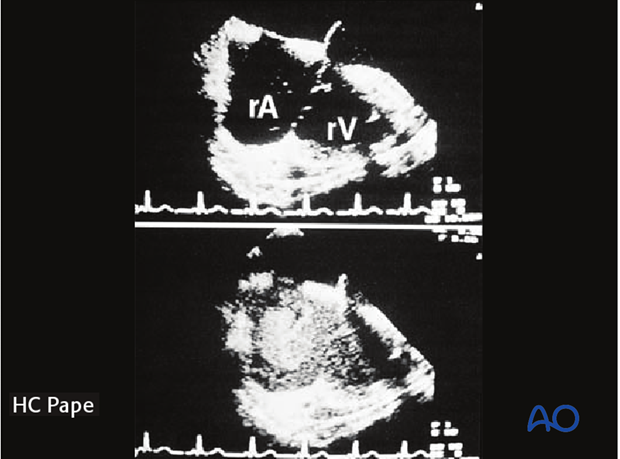
This may cause pulmonary embolization of medullary fat, which in turn may lead to pulmonary dysfunction (lower image in the enlarged view shows an example of fat embolization through the right atrium).
Conversion from an external fixator to an intramedullary nail
If an external fixator is in place, the Schanz screws must be partially withdrawn to allow the guide wire, the reamers, and later the nail, to pass through. The external fixator is held in place by monocortical purchase to assure that the fracture remains stable. The external fixator also acts as a joystick for the reduction.
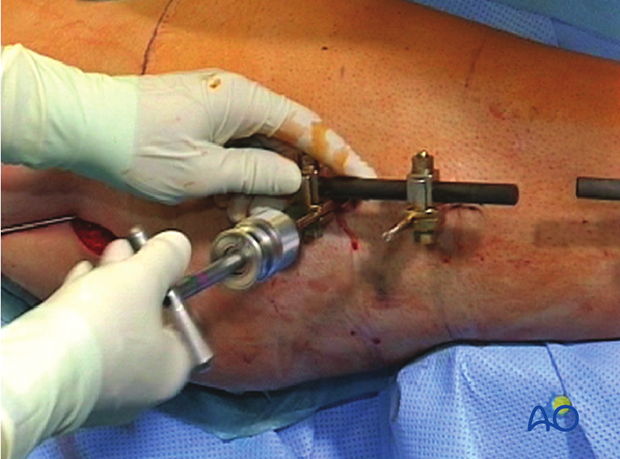
6. Nail insertion
Connecting handle to nail
The insertion handle is connected to the nail by the corresponding connecting screw. It is attached using the hexagonal screwdriver through the hole in the insertion handle. It is recommended that the nail be inserted manually and rotated about 90 degrees from its point of entry to its final orientation.
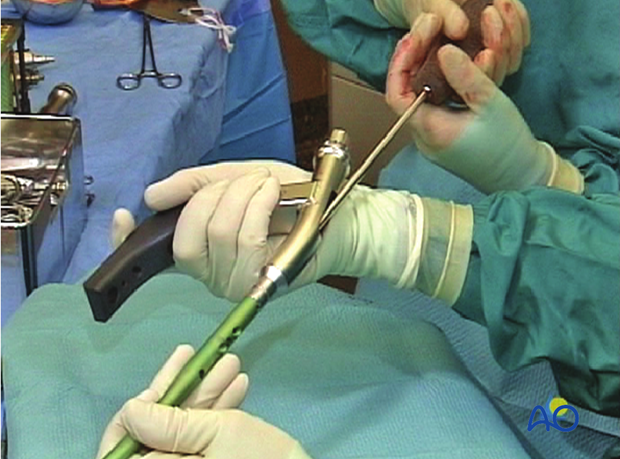
Introduction of nail
Under control with the image intensifier, the nail is pushed down as far as the fracture zone. After the driving cap has been fixed to the insertion handle, the nail is further advanced into the medullary cavity by gentle hammer blows, whilst verifying the position of the tip of the nail under the image intensifier.
In this intraoperative view, the nail is about to pass the fracture site in the intensifier image.
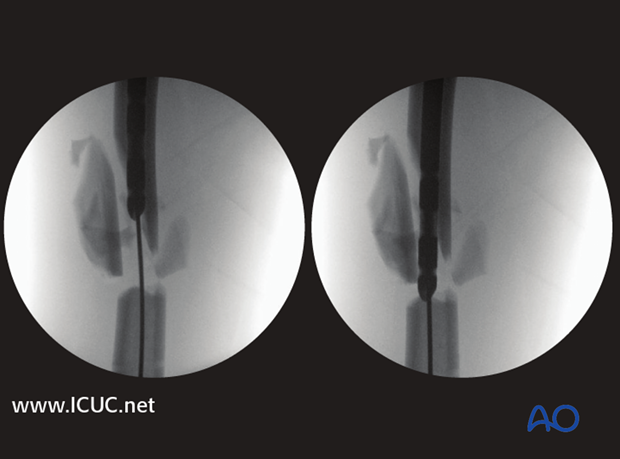
In this intraoperative view an unreamed nail is inserted and the external fixator is used as a joystick to help to reduce the fracture anatomically.
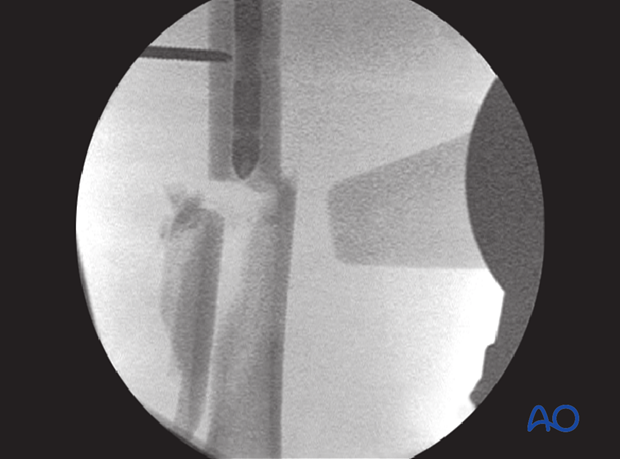
Once past the fracture, the nail is advanced by hand or by gentle hammer blows.
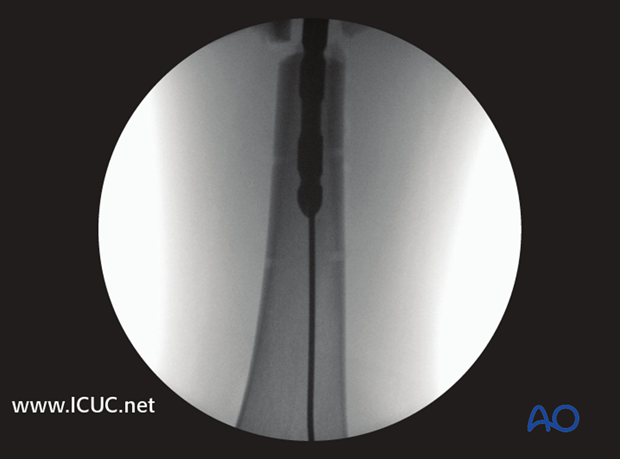
Passing the fracture zone
It is important that the tip of the nail does not become trapped in the distal main fragment because blow out fractures can occur. Each gentle hammer blow should advance the nail. Do not force the nail through a tight canal – if necessary, re-ream to another 0.5 mm diameter.
In many cases, the nail will help to align the fracture.
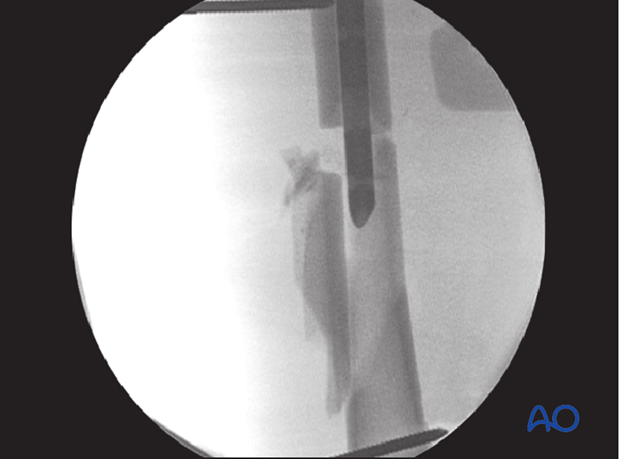
A solid nail (unreamed technique) passes the fracture site into the distal medullary canal.
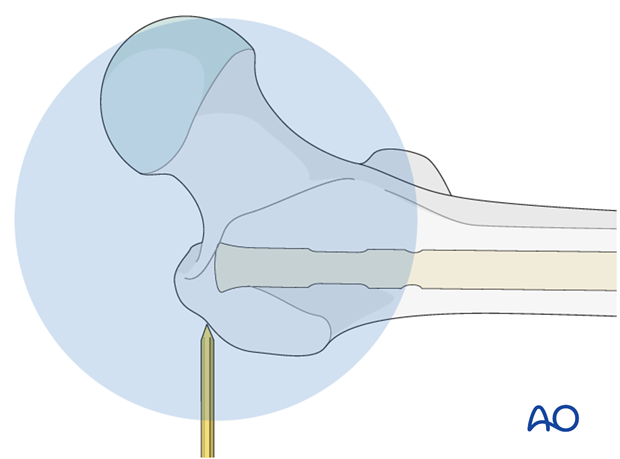
Assessing proper nail insertion
The nail is then completely inserted. This is assessed by using an additional K-wire that marks the proixmal end of the nail.
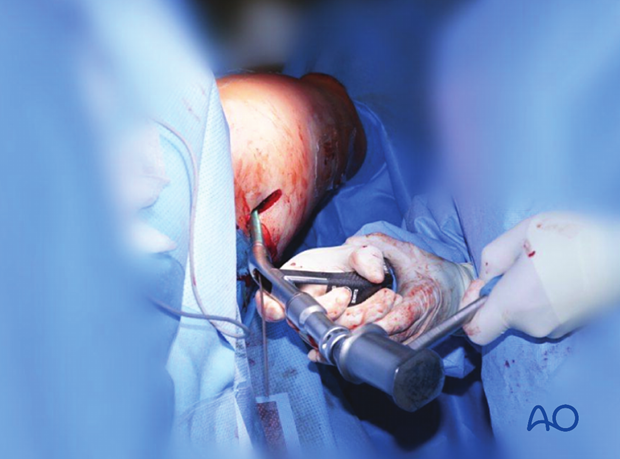
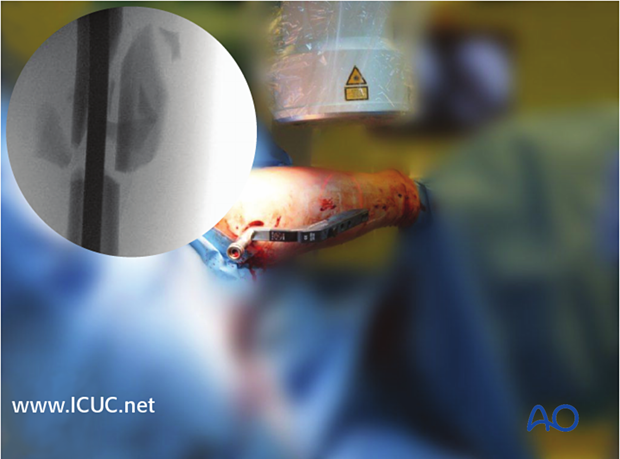
Intraoperative photo of nail inserted with fracture reduced and mild distraction.
AP image of nail inserted in the proximal femur.
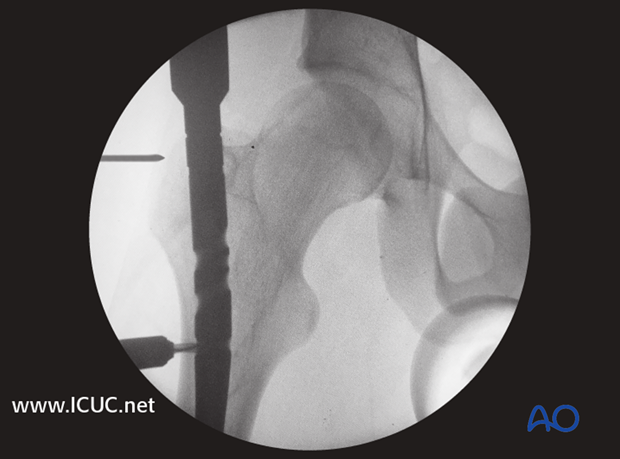
7. Nail locking
Purpose of locking
Locking was developed to provide and maintain rotational stability and length. It can also be used to finalize fracture reduction.
"Backslap" technique
The nail can distract the fracture site with impaction and this complication must be avoided. The backslap technique is necessary if the fracture gap is too large. This technique is only used for transverse fractures.
If the fracture is distracted, judging the distraction gap helps to determine how much deeper than usual the nail must be inserted. Distal locking is performed first with 2–3 screws, and the nail is pulled back with gentle hammer blows until fracture contact is achieved. Recheck the proximal end of the nail, which should not protrude proximally.
Static locking
Simple spiral and simple oblique fractures are usually stabilized with static locking screws.
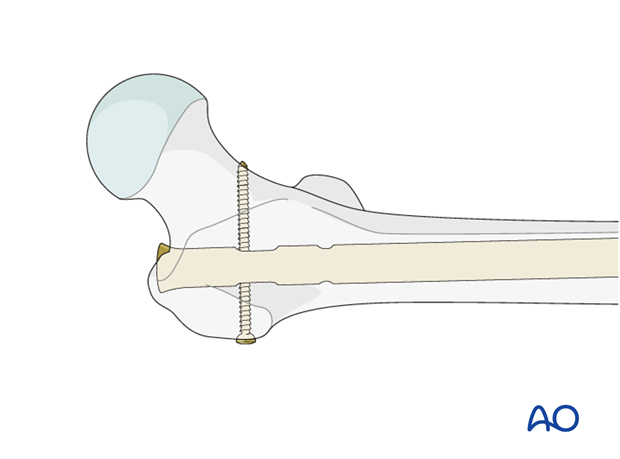
8. Nail locking
Purpose of locking
Locking was developed to provide and maintain rotational stability and length. It can also be used to finalize fracture reduction.
Static locking
Multifragmentary fractures are the least axially stable fractures. Special care must be taken to avoid limb shortening and static locking should be performed in all cases. The length may be assessed by comparison to the contralateral femur.
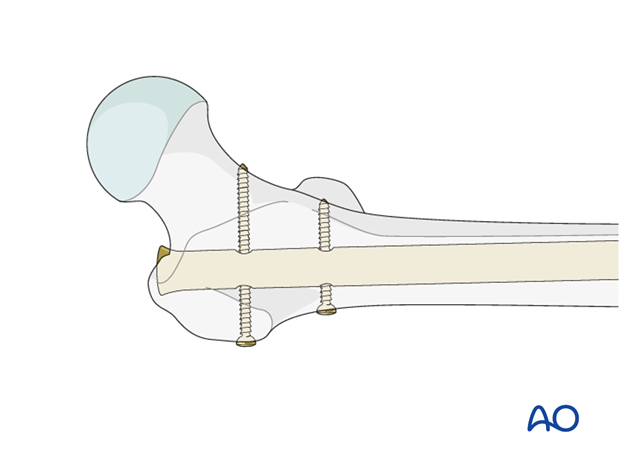
9. Distal locking
Verification of successful reduction
It is very important to restore the biomechanical axis of the lower limb. The normal biomechanical axis follows a line from the center of the femoral head, through the center of the proximal tibia and then through the center of the ankle joint. This axis can be checked intraoperatively by using a piece of cable, such as the diathermy cord. The cord is stretched from the iliac spine across the patella to the cleft between the first and second toes.
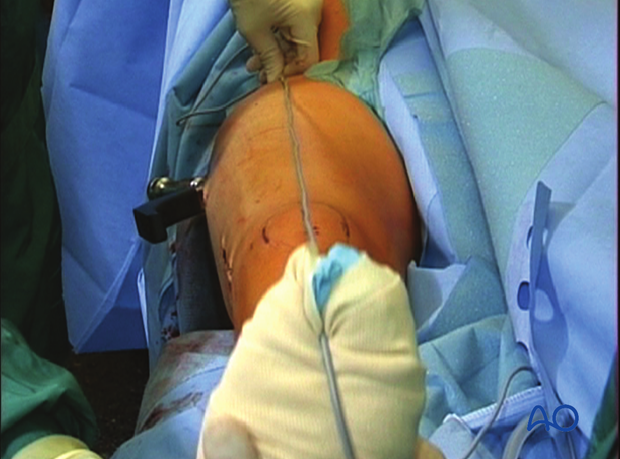
If rotation is correct, this cord will pass over the midline of the patella, and slightly medial to the tibial eminence. The radiological landmarks of the center of the femoral head, the center of the knee and the center of the ankle joint should all be in line if the mechanical axis of the femur is correct.
Another method of assessing rotational reduction is to compare the cortical thickness above and below the fracture. If a shaft fracture is multifragmentary, the image intensifier cannot be used to compare cortical diameters on each side of the fracture.
Not only must the biomechanical axis be restored, but care should be taken to ensure that there is no malrotation of the distal femur on the proximal femur.
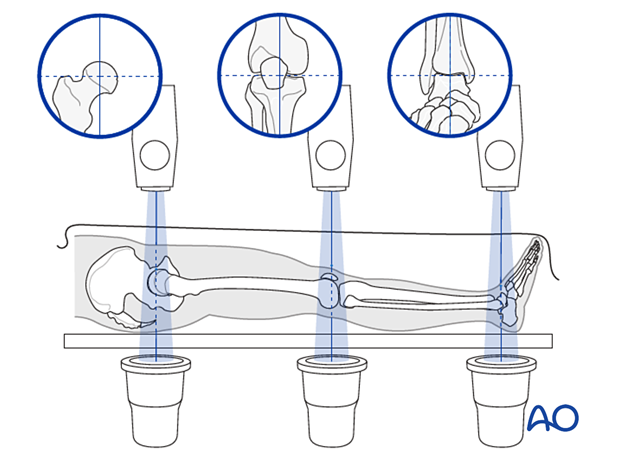
This illustration shows the longitudinal axes of the lower limb.
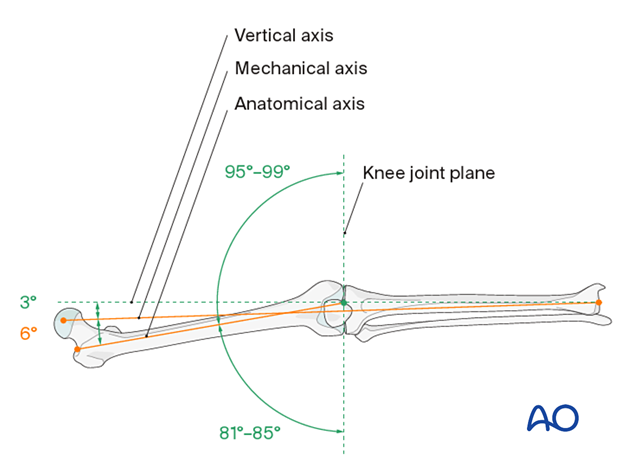
Distal aiming
For distal locking, the image intensifier is brought into a strict lateral position. The distal hole must be seen as a perfect circle and the tip of a scalpel is projected into the center of the hole.
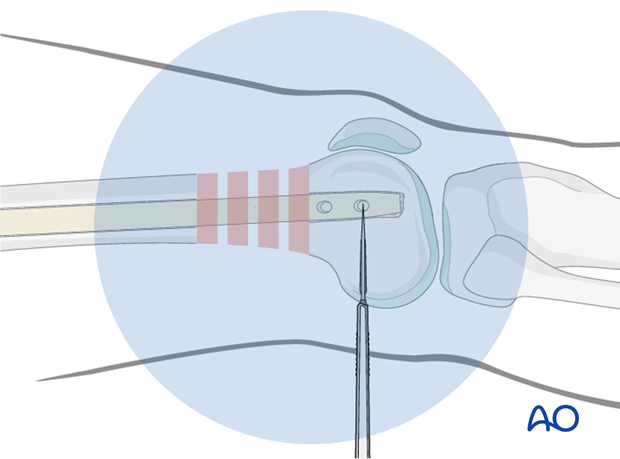
Screw insertion technique
The radiolucent drive helps to position the drill bit so that the locking screw can be properly inserted. While the locking hole is drilled, the assisting surgeon must prevent the lower extremity from moving in order not to miss the target hole. The length of the locking screw is determined, using the appropriate depth gauge. Then the locking screw is inserted.
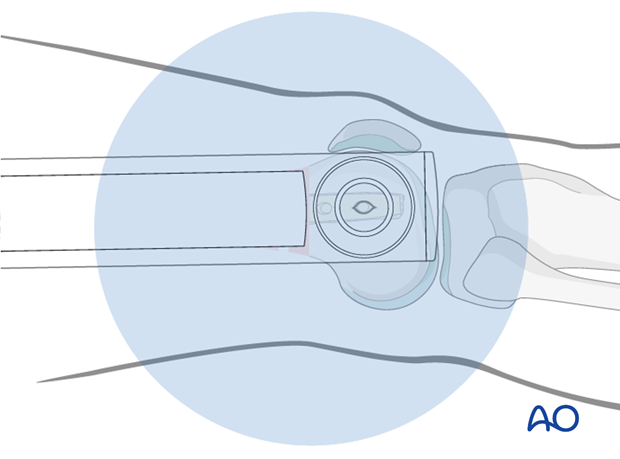
If a radiolucent drive is not available, the projection of the tip of the drill bit should be placed as centrally as possible (see image). Start drilling but assess the position of the tip of the drill bit repeatedly, with the drill temporarily uncoupled.
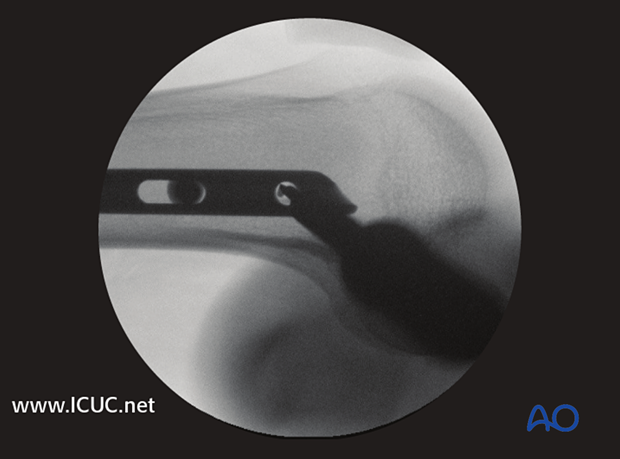
Pearl: If the contact between the screw driver and the locking screw is lost, the screw may move within the soft tissue and become extremely hard to capture. To prevent this time-consuming complication, the locking screw should be lassoed with a strong absorbable suture.
Pitfall: If the screw holes are not perpendicular to the nail, the locking screw may become trapped and may not be advanced properly.
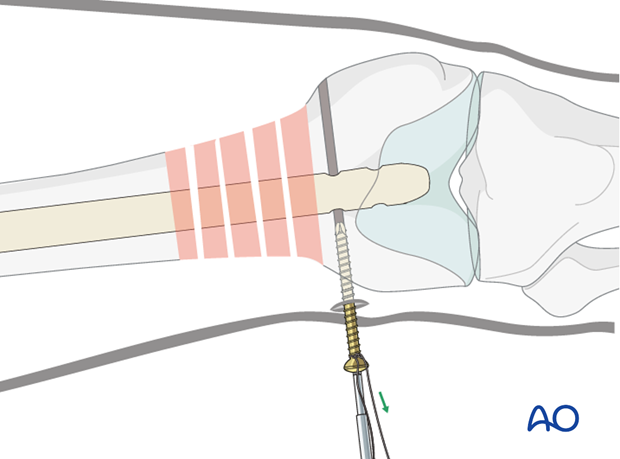
Completed distal locking
The image shows the distal locking completed.
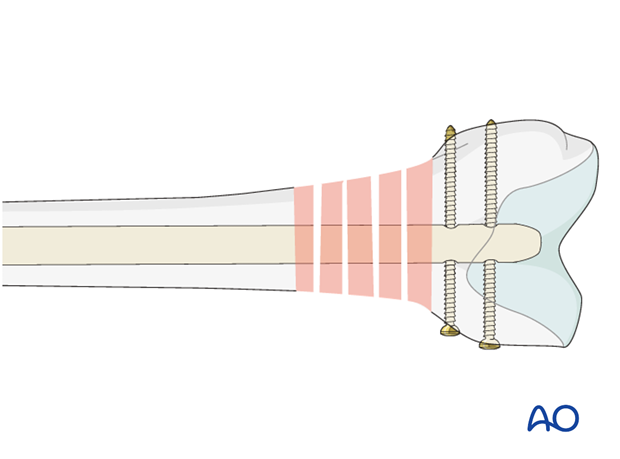
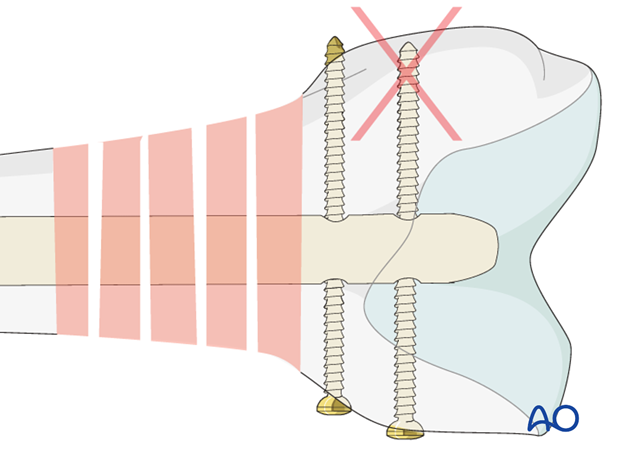
Pitfall: screw loosening
Care should be taken to capture the far cortex to prevent toggling when the patient is mobilized. This would lead to early loosening of the locking screw. In the image shown, the proximal locking screw is of correct length, but the distal one is marginally too short.
10. Intraoperative radiological assessment
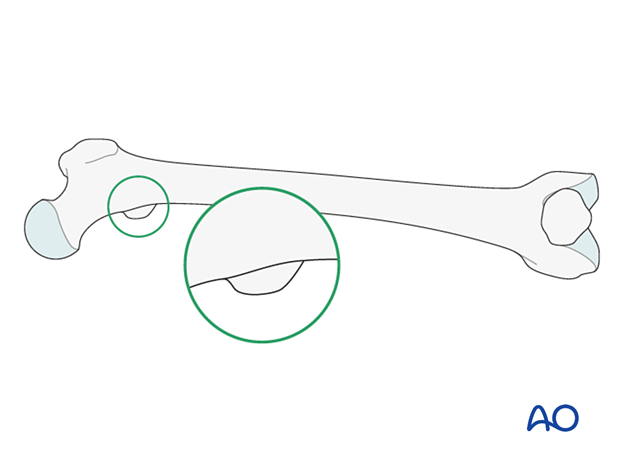
Assessment of rotation
Compare the profile of the lesser trochanter with that of the contralateral leg (lesser trochanter shape sign), holding the leg so that the patella faces anteriorly on both sides.
Before positioning the patient, store the profile of the lesser trochanter of the intact opposite leg (patella facing anteriorly) in the image intensifier.
The illustration shows the lesser trochanteric profile of the intact opposite side.
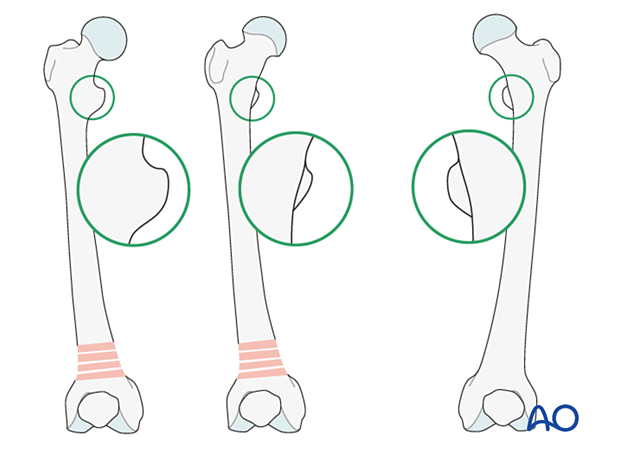
Malrotation
In cases of malrotation, the lesser trochanter is of a different profile when compared to that of the contralateral leg.
Take care to assess rotation with the patella facing directly anteriorly.
Matching of the lesser trochanter shape
After securing the plate to the distal femur, correct any malrotation by rotating the distal femur. Ensure that the profiles of the lesser trochanters are matched.
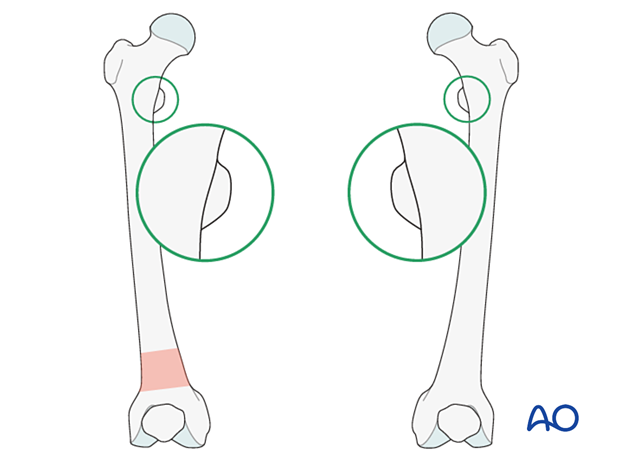
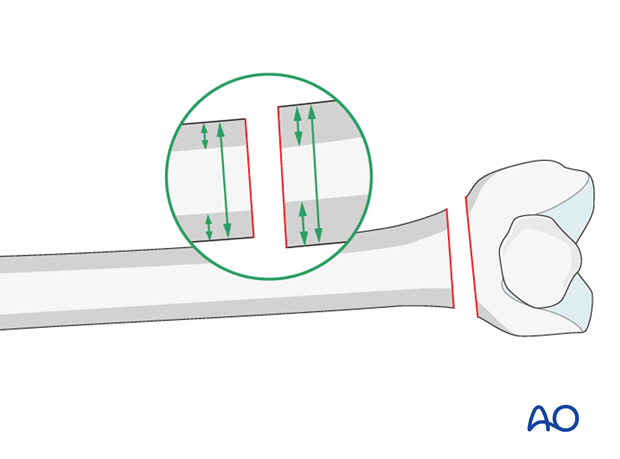
Cortical step sign and diameter difference sign
The presence of considerable rotational deformity may be diagnosed by the difference in thickness of the cortices above and below the fracture zone.
The diameter difference sign is of use at levels where the bone cross section is oval rather than round. In cases of malrotation, the proximal and distal main fragments will appear to be of different diameters.
11. Proximal locking
Proximal aiming device
If proximal locking is performed before distal locking, it is important to verify the correct position of the distal end of the nail under the image intensifier, before the proximal aiming device is attached to the insertion handle.
When dynamic locking is performed, only the dynamic locking hole is used.
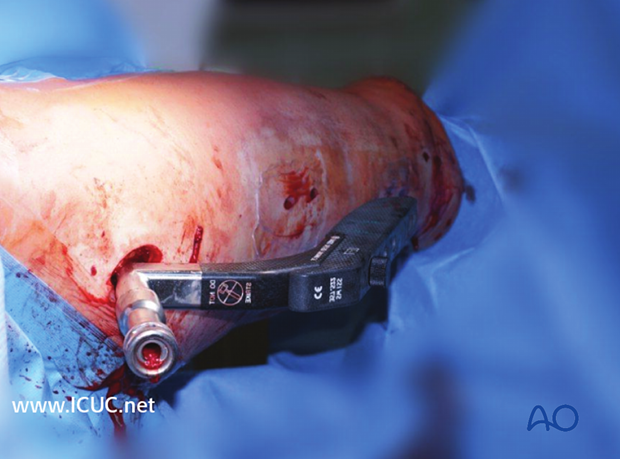
Preparation for screw insertion
The sites of the skin and fascial incisions for the drill bit and locking screws may be determined after the drill sleeve assembly has been in the holes of the aiming device.
The length of the locking screws is read from the calibrated drill bit. The correct length is confirmed antero-posteriorly using the image intensifier. The insertion handle should not be removed until the correct placement of all the locking screws has been verified.
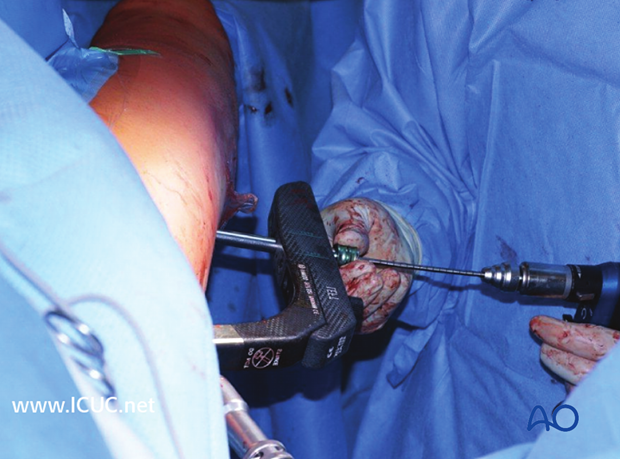
Drill sleeve to bone contact
The drill sleeve must be in close contact with the bone at all times since it is important for the measurement of the locking screws. Close contact is maintained by pressing down on the sleeve with the contralateral thumb.
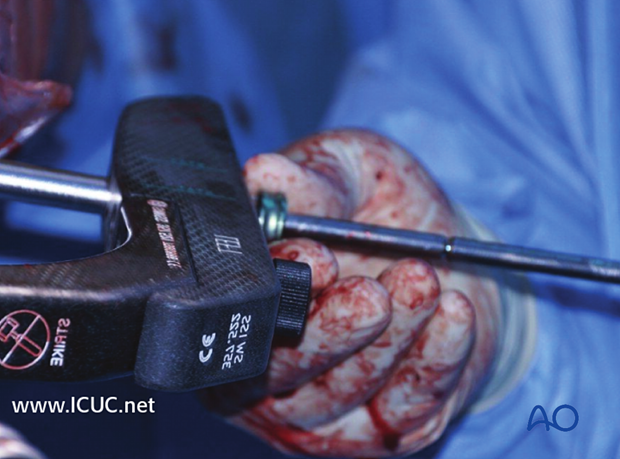
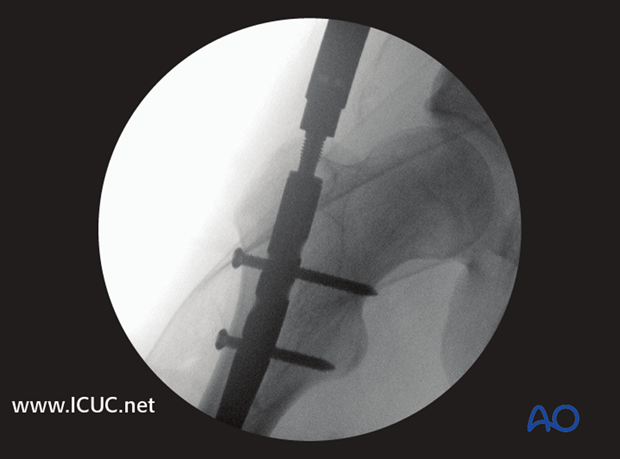
Fluoroscopy of proximal locking of femoral nail.

Verification of locking screw placement
A final x-ray in two planes should be obtained in all cases in order to verify the exact locking screw placement.
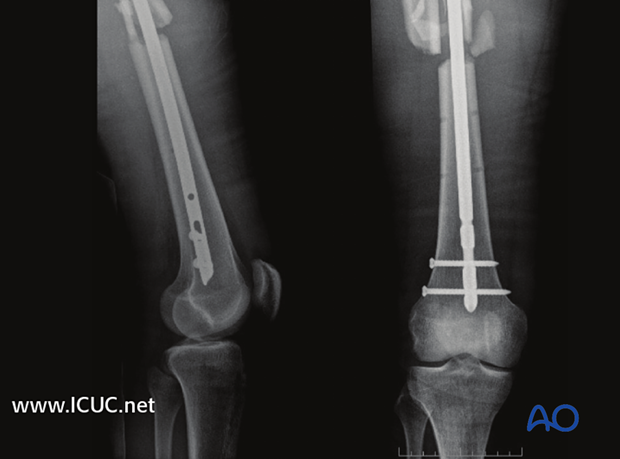
Here showing the final x-rays of a fragmentary segmental fracture.
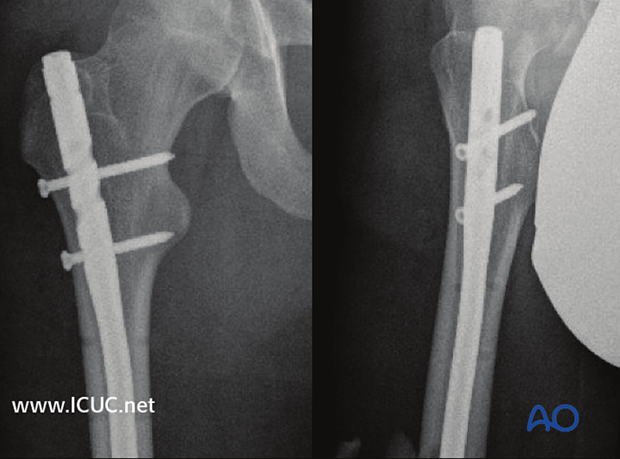
MainText
12. Insertion of end cap
An end cap may be used, depending on the final assessment of the nail length in relation to the tip of the greater trochanter.
The distance between the proximal end of the nail and the tip of the trochanter determines the appropriate length of the end cap, which is between zero and 20 mm, in 5 mm increments. The end cap is introduced using a hexagonal screwdriver.
The end cap is optional for the standard femoral nail.
Pitfall: The removal of the end cap may be very difficult if an exchange nailing is required. Bony overgrowth may require an extensive dissection of the greater trochanteric region. On the other hand, the end cap will have prevented tissue ingrowth and so, after its removal, the insertion of the extractor device is easier.
13. Wound closure and assessment of alignment
Wound closure
The procedure ends with the closure of the fascia and the skin as separate layers.
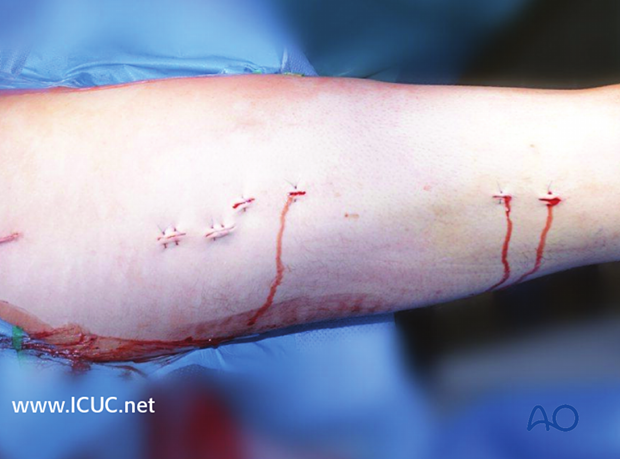
Assessment of alignment
Before the patient is moved from the fracture table, rotation of the leg is observed clinically and compared to the contralateral leg.
With the femur now stable, it is possible to perform a thorough examination of the knee joint to rule out additional ligamentous injuries.
14. Aftercare
Impediments to the restoration of full knee function after distal femoral fracture are fibrosis and adhesion of injured soft tissues around the metaphyseal fracture zone, joint capsular scarring, intra-articular adhesions, and muscle weakness.
Early range of motion helps restore movement in the early postoperative phase. With stable fracture fixation, the surgeon and the physical therapy staff will design an individual program of progressive rehabilitation for each patient.
The regimens suggested here are for guidance only and not to be regarded as prescriptive.
Functional treatment
Unless there are other injuries or complications, knee mobilization may be started immediately postoperatively. Both active and passive motion of the knee and hip can be initiated immediately postoperatively. Emphasis should be placed on progressive quadriceps strengthening and straight leg raises. Static cycling without load, as well as firm passive range of motion exercises of the knee, allow the patient to regain optimal range of motion.
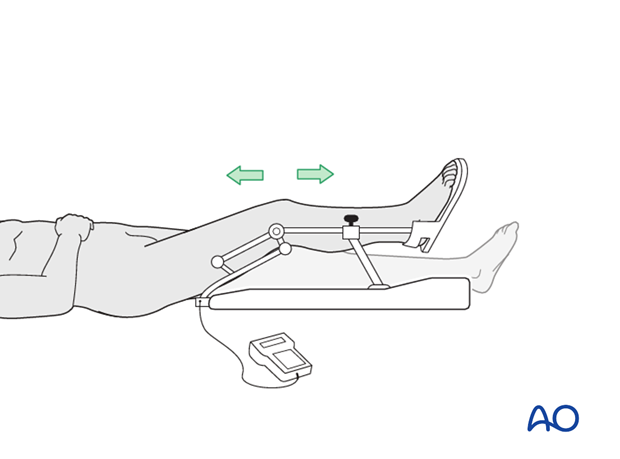
Weight bearing
Full weight bearing can be started immediately with range of motion.
Follow-up
Wound healing should be assessed at two to three weeks postoperatively. Subsequently 6-week, 12-week, 6-month, and 12-month follow-ups are usually made. Serial x-rays allow the surgeon to assess the healing of the fracture.
Implant removal
Implant removal is not essential but should be discussed with the patient if there are implant-related symptoms after consolidated fracture healing.
Thrombo-embolic prophylaxis
Thrombo-prophylaxis should be given according to local treatment guidelines.













