Nonoperative treatment
1. General considerations
Introduction
For conservative fracture treatment, a circumferential cast is recommended for up to 6 weeks according to interval radiological and clinical evaluation. The cast material selected does not affect the outcome.
Splinting is usually only used for additional stabilization after ORIF.
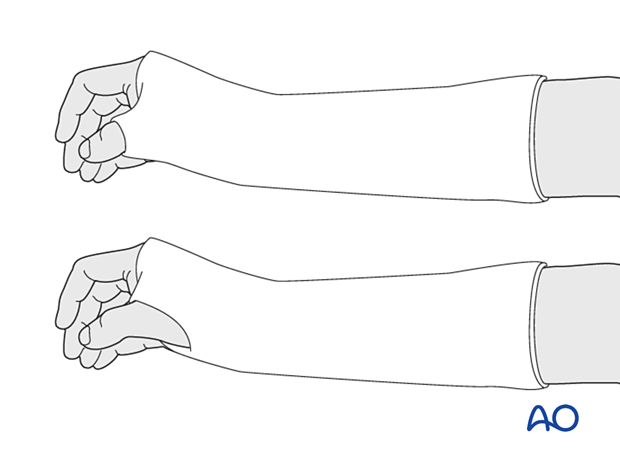
The wrist is immobilized in a below-elbow cast, with the wrist slightly extended and the proximal phalanx of the thumb included in a position of slight opposition (“scaphoid cast”).
The alternative is a below-elbow cast, with the wrist in neutral or slight extension but the thumb is free.
The selection is surgeon’s preference as there is not enough evidence available to distinguish the advantage of one over the other.
Isolated vs complex carpal injuries
In case of an isolated scaphoid fracture diagnosis, be aware of a missed complex carpal injury, eg, greater arc injuries. CT imaging may be helpful.
More complex injuries of the wrist usually need ORIF.
Closed reduction for low-demand and high-risk patients
Displacement is usually an indication for operative treatment. However, under certain circumstances (eg, low-demand or high-risk patient), nonoperative treatment may be preferable.
The amount of displacement can sometimes be reduced by molding the cast before it hardens.
2. Cast application
Padding
Pad the arm and hand to avoid pressure sores, especially on the distal ulna and styloid process of the radius.

Plaster application
Apply the circumferential plaster in a standard manner, starting at the fracture level.
The wrist should be in slight dorsiflexion.

Make sure that the plaster does not extend too far distally, both at the levels of the metacarpophalangeal (MCP) joints of the fingers and the interphalangeal (IP) joint of the thumb. The cast must allow complete movement of these joints.

Closed reduction with cast molding
Press the scaphoid tuberosity upwards from the palmar aspect. Carefully mold dorsally over the capitate to depress the distal carpal row in relation to the proximal carpal row.

3. Aftercare
The aftercare can be divided into four phases of healing:
- Inflammatory phase (week 1–3)
- Early repair phase (week 4–6)
- Late repair and early tissue remodeling phase (week 7–12)
- Remodeling and reintegration phase (week 13 onwards)
Full details on each phase can be found here.
Pain control
To facilitate rehabilitation, it is important to control the postoperative pain adequately.
- Management of swelling
- Appropriate splintage
- Appropriate oral analgesia
- Careful consideration of peripheral nerve blockade













