ORIF through extended iliofemoral approach
1. General considerations
Sequence of the treatment
Pre-operative traction will be advantageous if the hip is subluxed medially.
For ORIF of transverse/posterior wall fractures with extended iliofemoral approach, the following surgical sequence is common:
- Joint distraction and removal of incarcerated fragments
- Reduction of femoral head dislocation if not achieved closed on admission
- Reduction of the transverse element of the fracture
- Assessment of reduction (the anterior column reduction can be direct with this approach unlike with a Kocher-Langenbeck)
- Fixation of the anterior and posterior column
- Reduction and fixation of the posterior wall fragments
Planning/templating
Preoperative templating is essential for understanding the complexity of an acetabular fracture.
When using implants on the innominate bone, it is important to know the best starting points for obtaining optimal screw anchorage (see General stabilization principles and screw directions).
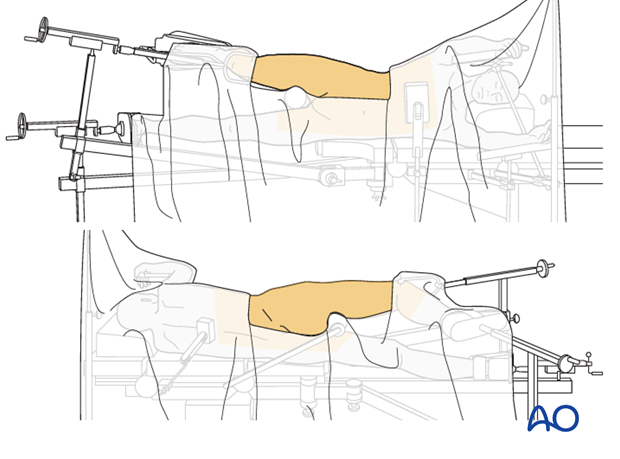
Patient positioning
The patient is positioned lateral on a flat top radiolucent table or a fracture table. Typically, a distal femoral traction pin is applied to allow the application of traction and also to stabilize the extremity. The knee is flexed 45°.
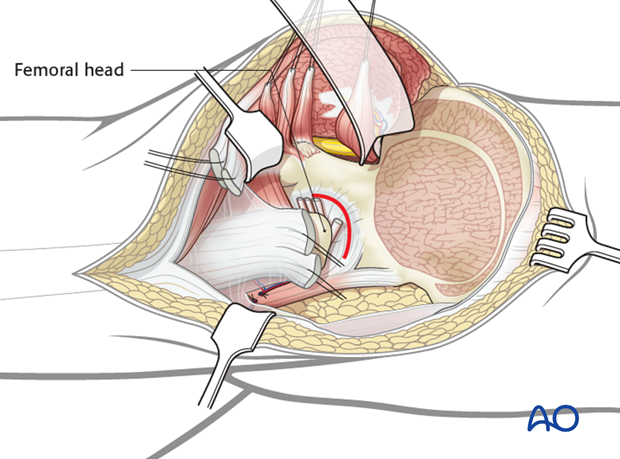
Capsulotomy
The extended iliofemoral approach allows the hip joint to be opened with a capsulotomy, just distal to the labrum. Lateral and/or distal retraction of the femoral head makes it easier to see into the joint.
It also allows the fracture to be seen well on the external surfaces of both the anterior and the posterior columns.
The internal surface of the pelvis can be palpated with a finger in the greater sciatic notch, for further assessment of the reduction.
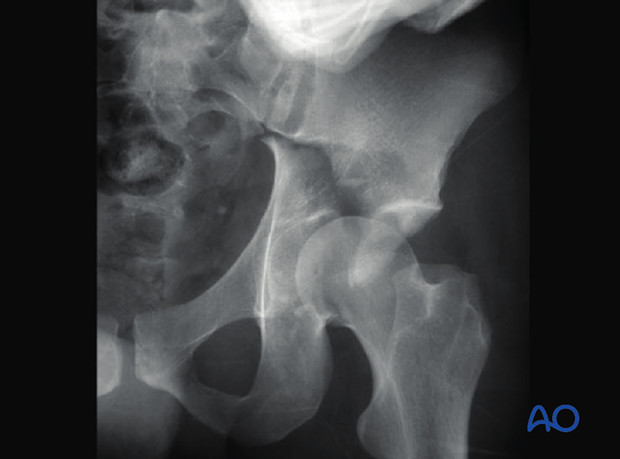
Sciatic nerve injury
Posterior wall fractures, elemental and associated, usually result from posterior hip dislocation. The sciatic nerve may be injured. Post reduction CT will be used to evaluate the fracture characteristics. Watch for bone and cartilage impaction.
Teaching video
AO teaching video: Use of the distractor on the pelvis
2. Principles of reduction
Fracture reduction
Fracture reduction can be difficult and it is possible to reduce for example the posterior fracture apparently perfectly, but with significant anterior displacement still.
Indirect visualization
Unusually for a significant joint, articular reduction of acetabular fractures is indirect. The articular surface of the hip joint is not seen directly. Reduction must be assessed by the appearance of the extraarticular fracture lines and intraoperative fluoroscopic assessment. Some fracture lines are palpated manually but not seen directly such as transverse fracture lines on the quadrilateral plate.
Marginal impaction in the posterior wall fracture can be seen directly prior to final closure of the cortical fragment.
Quality of reduction
Posttraumatic arthrosis is directly related to the quality of reduction - the better the reduction, the greater the chance of a good or excellent result.
3. Transverse fracture: reduction
Reduction of the fracture can be achieved for both anterior and posterior columns simultaneously under direct vision.
Begin the reduction by cleaning all clot and bone fragments from the fracture plane.
Femoral head subluxation
If the femoral head has been reduced in a closed fashion, subluxation of the joint to clear bony fragments would be required.
If the head is still dislocated then the joint can be cleaned before reduction.
Reduction of femoral head
To begin the reduction, the femoral head must be replaced congruently under the superolateral articular surface. Traction accomplishes this, and may be aided with a Schanz screw in the femur, or possibly a femoral distractor. Inspect the femoral head for articular surface injury.
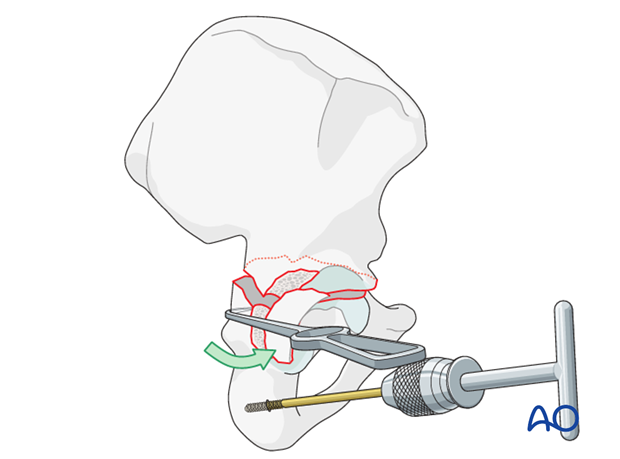
Use of a bone hook and a T-handle
A hook inserted through the lesser or greater sciatic notch helps to pull the posterior end of the distal fragment laterally.
A Schanz screw can be inserted into the ischium to use as a joystick for manipulation of the distal fragment posteriorly (see below).
Use of reduction forceps
Posteriorly, the reduction can be held in place with a Farabeuf or a Jungbluth clamp, or alternatively with pointed reduction forceps.
Anteriorly, pointed reduction forceps are used.
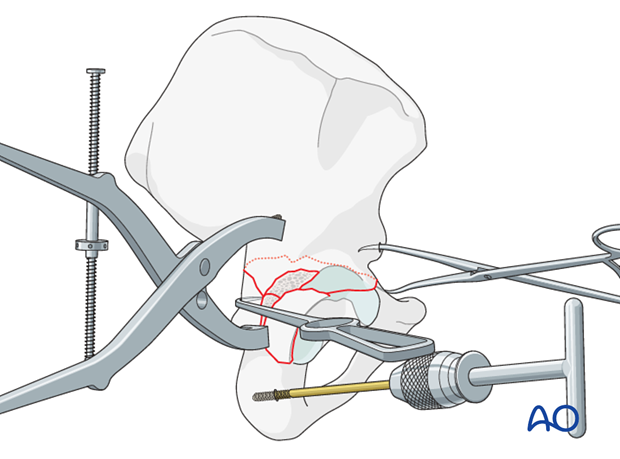
Alternative anterior technique
Another anterior reduction technique involves use of forceps applied to a 3.5 mm screw placed into the distal fragment.
Place the screw before beginning the reduction maneuver. It should be inserted medial to the acetabulum, into the best obtainable bone of the distal fragment. Stay close to the quadrilateral surface, outside the hip joint.
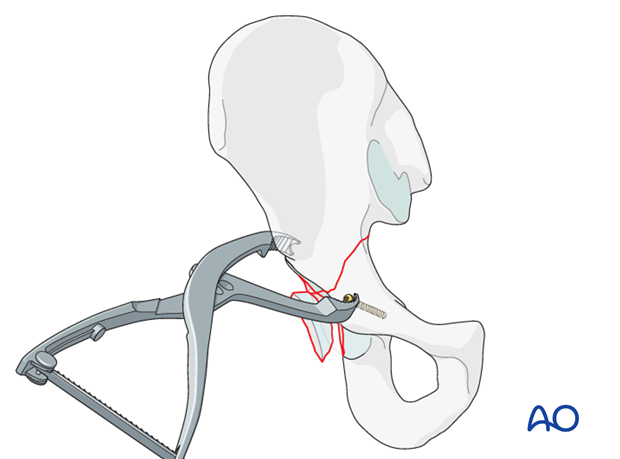
Free bone fragment
If possible, include any loose bone fragments in the final reconstruction, particularly if they form part of the articular surface. They may be stabilized with 2 mm screws or intraosseous wires.
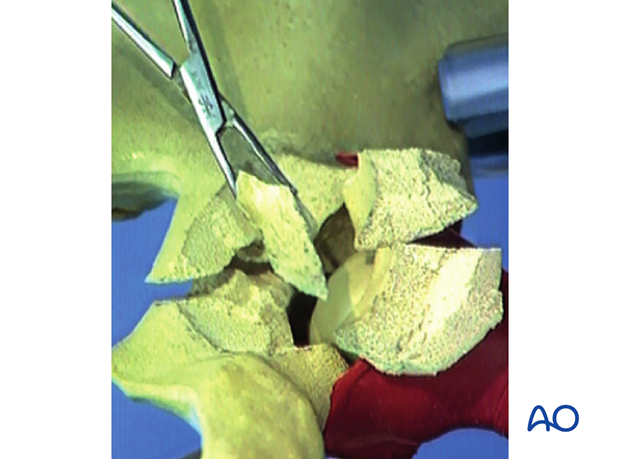
Confirm reduction
After manipulation of the posterior and anterior aspects of the fracture, confirm that the reduction is truly anatomical. Check the articular surface visually and by palpation within the joint. Also confirm reduction on the internal pelvic surface by palpation through the greater sciatic notch.
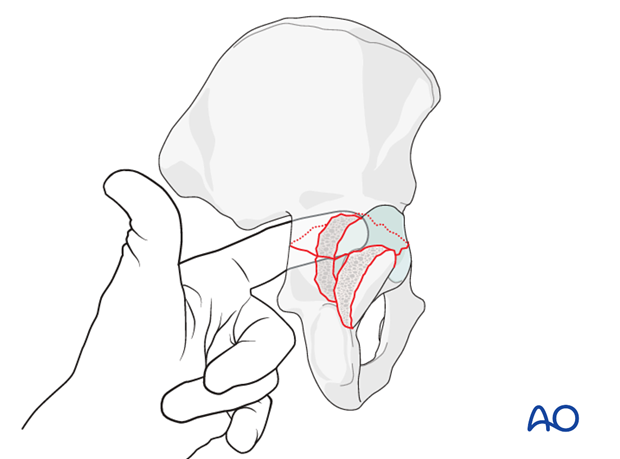
4. Transverse fracture: fixation
Anterior column fixation
The anterior part of the fracture is compressed with an appropriately placed lag screw.
The anterior screw is placed obliquely from above the greater sciatic notch across the fracture. It is aimed anteriorly towards the root of the superior pubic ramus. The entry point is along the anterior (gluteus medius) pillar of the iliac wing, 3 to 4 cm above the acetabular margin.
A 7.3 mm partially threaded screw is usually used to offer compression of the anterior portion of the transverse fracture.
A 2.8 mm guidewire is inserted along the anterior column before the appropriate length screw is passed over the wire.
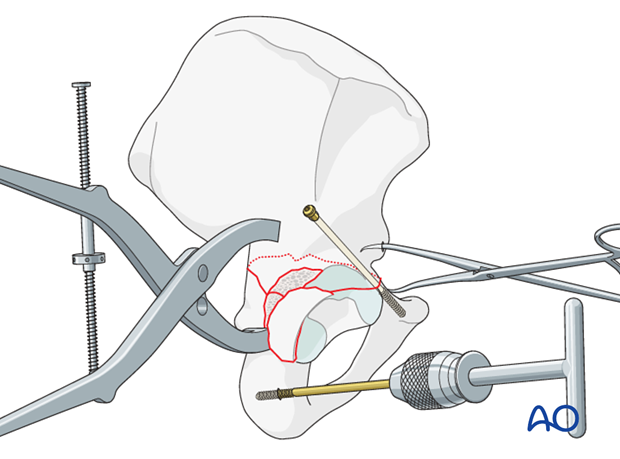
Posterior column fixation
An axial posterior column screw provides interfragmentary compression across the posterior part of the fracture. This is inserted from distal to proximal.
A 7.3 mm partially threaded cannulated screw is inserted through a separate stab incision in the buttock crease over a guide wire.
The starting point is at the ischial tuberosity, and a finger in the greater sciatic notch is used to guide the wire and screw up the posterior column, exiting at the pelvic brim.
Care is taken to protect the sciatic nerve at the level of the ischial tuberosity.
The use of a screw aids the placement of the posterior wall plate as it increases the freedom of placement of the wall plate.
This is commonly referred to as the “butt screw”.
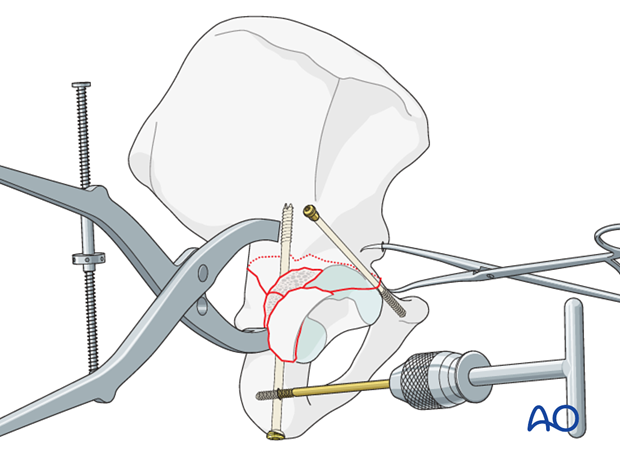
Alternative: medial posterior column plate
An alternative to the posterior column screw is a contoured pelvic reconstruction plate applied over the fracture, along the posterior column medially.
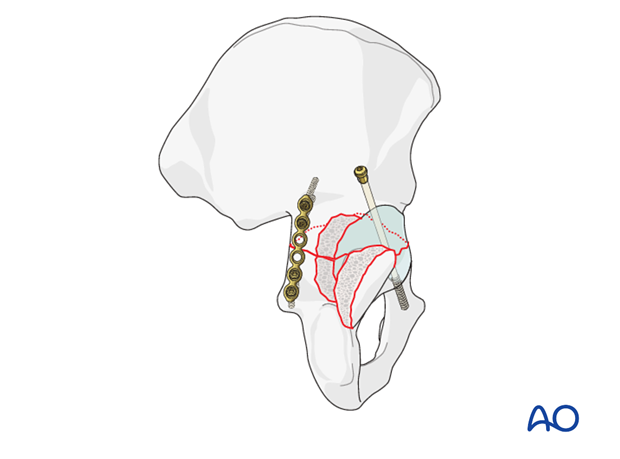
5. Posterior wall: reduction
Reduction of a free fragment
After release of the traction, the femoral head is reduced into the joint. Reconstruction of the posterior wall begins with replacement of any free osseocartilaginous fragment, so that its articular surface is congruent with the femoral head. The wall fragments must be reduced anatomically, and fixed in place. Any free fragment will be held reduced by the overlying posterior wall fragments.
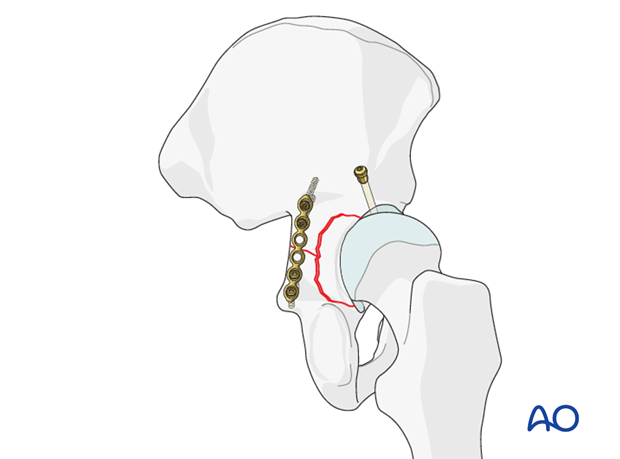
Reduction with ball spike pushers, dental picks, or elevators
Reduce the posterior wall fragments, with attached hip capsule. Use ball spike pushers, dental picks, or elevators.
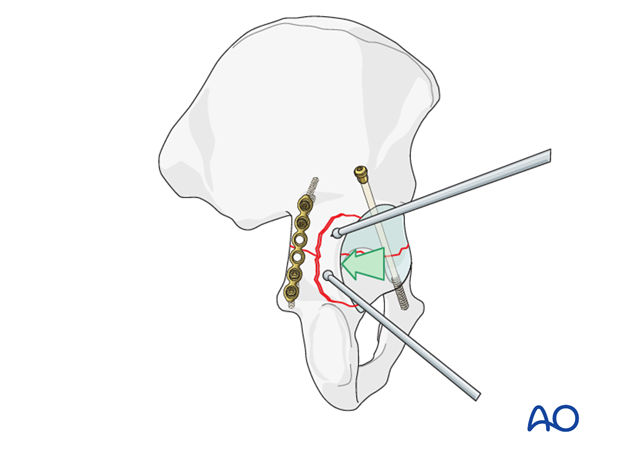
6. Posterior wall: initial fixation
This figure shows the wall fragment reduced and fixed with two lag screws after initial posterior column fixation with a plate. Another plate must be added across the wall fracture to obtain secure fixation.
Commonly, two 2.7 mm cortical screws are used. If the fragment is large enough, a 3.5 mm screw can be used, but it should be a lag screw, with a 3.5 mm gliding hole drilled in the wall fragment, and 2.5 mm thread hole in the underlying bone. It is important to avoid the joint when placing these screws.
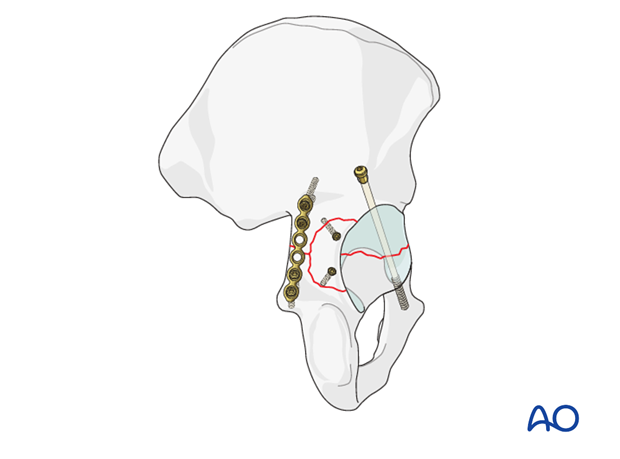
7. Posterior wall: completing the fixation
Choice and contouring of plate
There are both straight and curved pelvic reconstruction plates. A curved plate usually works well on the posterior wall. Any plate must be contoured and positioned for optimal support of the wall fragments.
To aid contouring, a malleable template is first fit to the bone. This provides a model for contouring the 3.5 mm reconstruction plate.
The plate is slightly undercontoured, over the convexity of the posterior column, compared with the template. This is so that it compresses the fragments slightly as its screws are tightened.
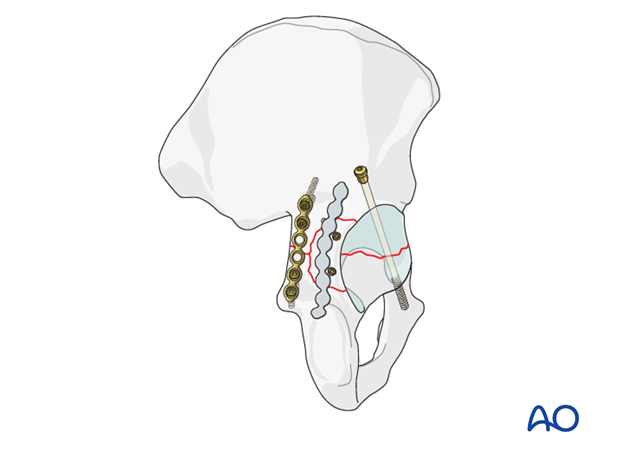
Application of the plate
First fix the distal end of the plate with a screw into its concave bend, just above the superior pole of the ischial tuberosity.
Drill a 2.5 mm hole before insertion of a 3.5 mm cortical screw but do not completely tighten it yet.
Position the plate optimally, and hold it with a ball spike pusher during the next step.
Next, insert the most proximal screw. Drill eccentrically, closer to the proximal end of the hole, so that tightening this screw tensions the plate, analogous to a dynamic compression plate.
Addition of remaining distal and proximal screws should improve final contouring, to provide uniform compression of the posterior wall fragments. The screws in the mid-portion of the plate should be omitted because of the underlying hip joint. Each major posterior wall fragment should have a screw, either through the plate and into good underlying bone, or inserted outside the plate.
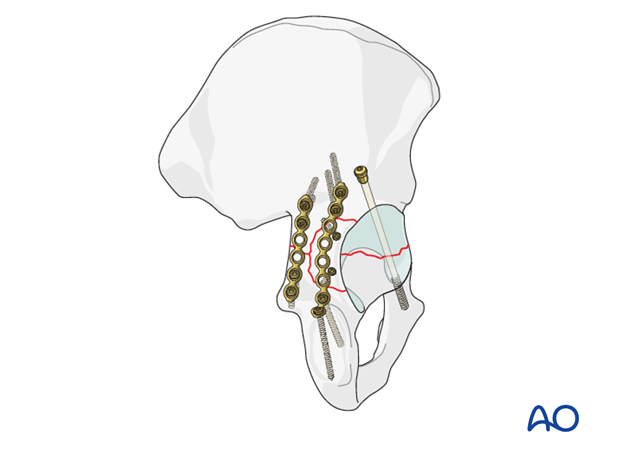
Examples for completed fixation
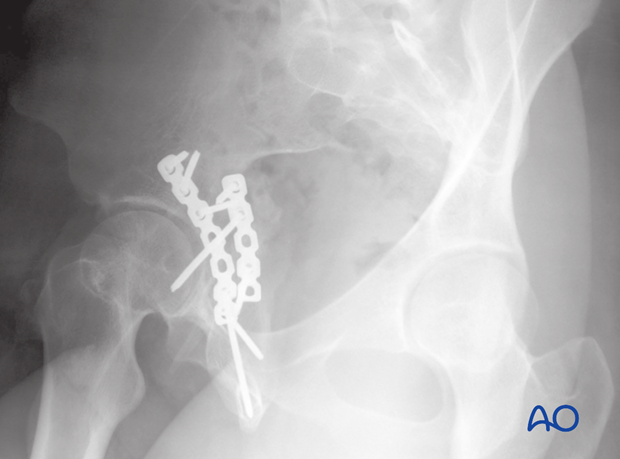
This example shows the use of an initial lag screw with posterior plates.
The medial one, near the sciatic notch, was placed first to fix the posterior end of the transverse fracture. The second plate fixes the posterior wall component, and adds additional posterior column support with separate small lag screws in the posterior wall fragment.
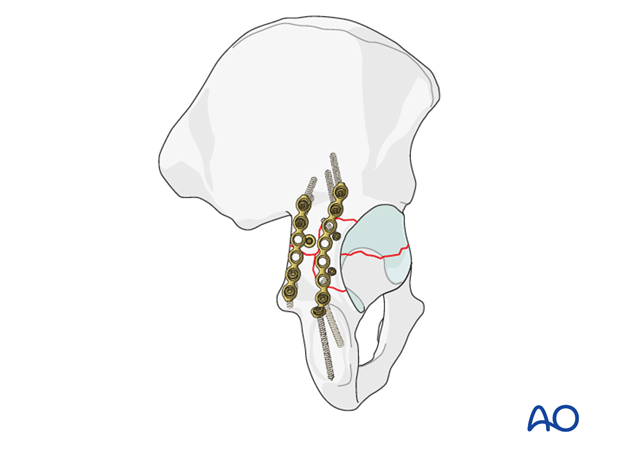
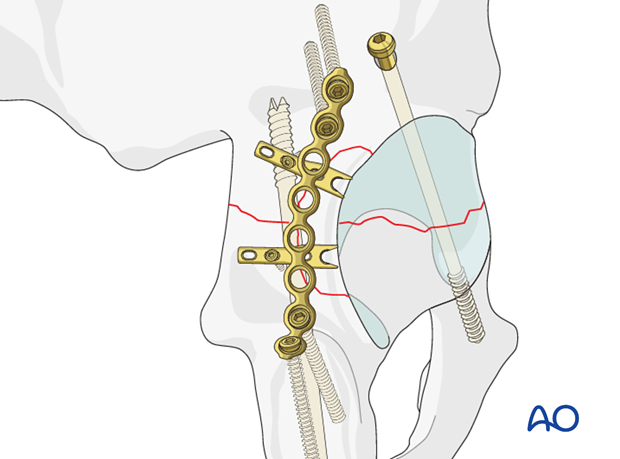
The second example has used a posterior column screw to stabilize instead of a medial plate.

Spring hook plates
Stabilization of the posterior wall fragments sometimes requires spring hook plates to resist shearing forces on the fragment which are inserted either instead of lag screws, or before them to resist the shear created by the compression.
The spring hook plates should extend medially beyond the posterior wall buttress plate. These supplementary plates provide additional buttress support for the comminuted fragments.
The hooks must press on the bone fragments and not into the labrum.
Spring hook plates are available pre-contoured or made from small fragment one third tubular plates. For details see the corresponding basic technique.
8. Radiographic assessment
Intraoperative confirmation of hardware position
During reduction and fixation, take fluoroscopic images in AP, iliac, and obturator oblique views to confirm reduction and/or screw placement.
In particular to confirm that posterior wall lag screws are extraarticular an image exposed with the fluoroscope’s central ray superimposed on the long axis of the screw is taken.
Final radiographic assessment
Once all fixation is in place, confirm the appropriate appearance of AP, obturator oblique and iliac oblique views and check the location of any screw that is placed near the hip joint.
The AP view should be inspected to assure that congruence has been obtained. The femoral head should have the same relationship to the radiological roof, the anterior rim and the posterior rim as on the contralateral side.
If the low anterior column was affected, the obturator foramen profile and symphysis should be inspected to assess the quality of the distal reduction.
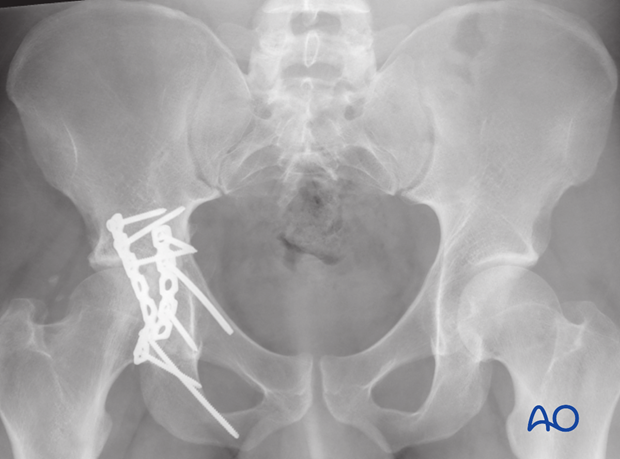
The lag screw should be seen to be crossing the level of the transverse fracture, and the lower plate screws should be directed down the ischium and not in the direction of the posterior wall.
If a posterior wall fragment was involved, it should be seen as reduced and stabilized on this image.
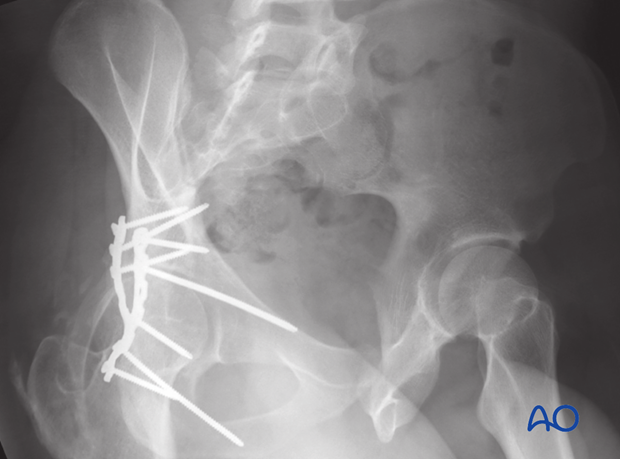
Iliac oblique view should be inspected to ensure that the posterior column reduction is anatomic. The screws directed down the posterior column should be inspected and verified as extraarticular.
Postoperatively, obtain formal high-quality radiographs of AP and both oblique views.
9. Postoperative care
During the first 24-48 hours, antibiotics are administered intravenously, according to hospital prophylaxis protocol. In order to avoid heterotopic ossification in high-risk patients, the use of indomethacin or single low dose radiation should be considered. Every patient needs DVT treatment. There is no universal protocol, but 6 weeks of anticoagulation is a common strategy.
Wound drains are rarely used. Local protocols should be followed if used, aiming to remove the drain as soon as possible and balancing output with infection risk.
Specialized therapy input is essential.
Following the extended iliofemoral approach, the patient’s leg may be positioned in abduction in order to reduce tension on the muscles of the reconstructed area.
Follow up
X-rays are taken for immediate postoperative control, and at 8 weeks prior to full weight bearing.
Postoperative CT scans are used routinely in some units, and only obtained if there are concerns regarding the quality of reduction or intraarticular hardware in others.
With satisfactory healing, sutures are removed around 10-14 days after surgery.
Mobilization
Early mobilization should be stressed and patients encouraged to sit up within the first 24-48 hours following surgery.
Mobilization touch weight bearing for 8 weeks is advised.
Weight bearing
The patient should remain on crutches touch weight bearing (up to 20 kg) for 8 weeks. This is preferable to complete non-weight bearing because forces across the hip joint are higher when the leg is held off the floor. Weight bearing can be progressively increased to full weight after 8 weeks.
With osteoporotic bone or comminuted fractures, delay until 12 weeks may be considered.
Implant removal
Generally, implants are left in situ indefinitely. For acute infections with stable fixation, implants should usually be retained until the fracture is healed. Typically, by then a treated acute infection has become quiescent. Should it recur, hardware removal may help prevent further recurrences. Remember that a recurrent infection may involve the hip joint, which must be assessed in such patients with arthrocentesis. For patients with a history of wound infection who become candidates for total hip replacement, a two-stage reconstruction may be appropriate.
Sciatic nerve palsy
Posterior hip dislocation associated with posterior wall, posterior column, transverse, and T-shaped fractures can be associated with sciatic nerve palsy. At the time of surgical exploration, it is very rare to find a completely disrupted nerve and there are no treatment options beyond fracture reduction, hip stabilization and hemostasis. Neurologic recovery may take up to 2 years. Peroneal division involvement is more common than tibial. Sensory recovery precedes motor recovery and it is not unusual to see clinical improvement in the setting of grossly abnormal electrodiagnostic findings.













