ORIF through trochanter osteotomy extension
1. General considerations
Choice of approach
The morphology, size and location of fracture fragments are highly variable.
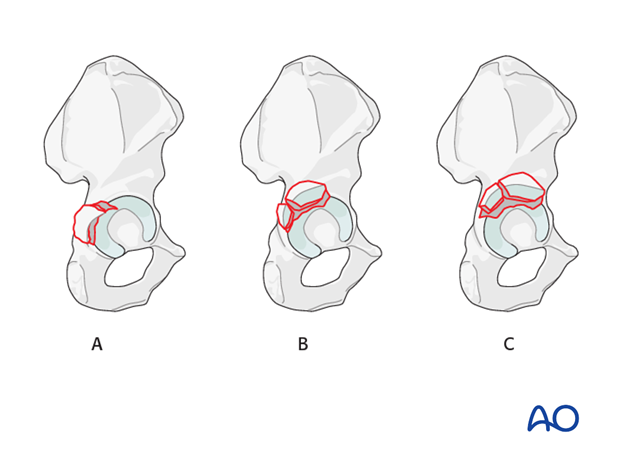
Most commonly, elementary fractures are confined to the retroacetabular surface involving only a small amount of the acetabular roof (A). This area of the innominate bone is appropriately accessed with the traditional approach. This can be performed in either the prone or lateral position.
If the fragment is more superior in location and involves an extensive portion of the acetabular roof (B), additional cranial exposure may be required. This can be accomplished with the addition of the trochanteric osteotomy to the approach. This technique allows better visualization and better reduction of the fragments.
In cases where the fragment extends anterior to the gluteus medius pillar (C), the interval and prone positioning may limit the anterior exposure required for adequate reduction. In these cases, the more anterior interval of the modified Gibson approach with the trochanteric osteotomy significantly enhances cranial and anterior exposure.
Sequence of the treatment
With posterior wall fractures, the following surgical sequence is common:
- Joint distraction and removal of incarcerated fragments
- Reduction of femoral head dislocation if not achieved closed on admission
- Reduction and stabilization of marginal impaction
- Reduction and fixation of the posterior wall fragments
Planning/templating
Preoperative templating is essential for understanding the complexity of an acetabular fracture.
When using implants on the innominate bone, it is important to know the best starting points for obtaining optimal screw anchorage (see General stabilization principles and screw directions).
Patient positioning
The Kocher-Langenbeck with trochanteric osteotomy in the prone position may give exposure to the posterior half of this large superior fragment. However, in order to completely expose this fracture for optimal reduction and fixation, the Gibson interval with trochanteric osteotomy in the lateral position is used.
The more anterior interval and the additional hip motion allow exposure to the anterior inferior iliac spine, not possible with the patient prone.
If a hip dislocation is expected, the patient should be positioned in the lateral position.
The maintenance of knee flexion (at 90°) and hip extension throughout the procedure reduces tension on the sciatic nerve.
Sciatic nerve injury
Posterior wall fractures, elemental and associated, usually result from posterior hip dislocation. The sciatic nerve may be injured. Post reduction CT will be used to evaluate the fracture characteristics.
Teaching video
AO teaching video: Posterior wall fracture through Kocher-Langenbeck approach
2. Principles of reduction
Indirect visualization
Unusually for a significant joint, articular reduction of acetabular fractures is indirect. The articular surface of the hip joint is not seen directly. Reduction must be assessed by the appearance of the extraarticular fracture lines and intraoperative fluoroscopic assessment. Some fracture lines are palpated manually but not seen directly such as transverse fracture lines on the quadrilateral plate.
Marginal impaction in the posterior wall fracture can be seen directly prior to final closure of the cortical fragment.
Quality of reduction
Posttraumatic arthrosis is directly related to the quality of reduction - the better the reduction, the greater the chance of a good or excellent result.
Reduction of femoral head
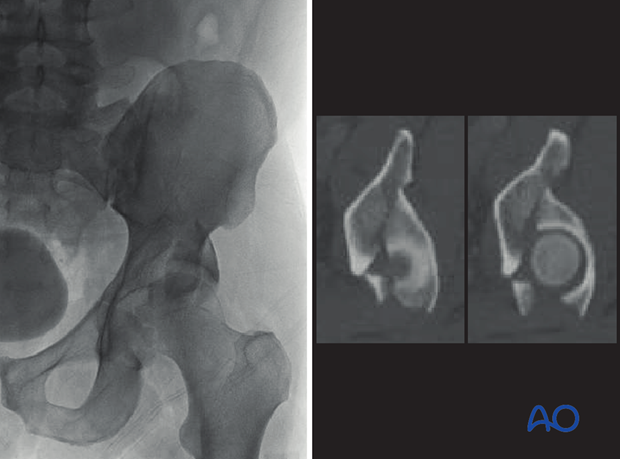
In the superior, extended posterior wall fractures, the posterior dislocation of the femoral head may be subtle, as the entire radiological roof is involved in the displaced fragment. Therefore, unlike ‘typical’ posterior wall fractures, the femoral head may not overlap the radiological roof – a telltale sign of dislocation. Inspection of the obturator oblique and the CT scan will demonstrate that the femoral head is not concentric in the acetabulum.
Ideally, this dislocation should have been reduced upon the patient's arrival in hospital, to restore blood flow to the femoral head and minimize additional joint trauma. However, because the entire roof is involved, maintaining a reduction is commonly not possible in the superior, extended posterior wall fractures. The reduction may need to be accomplished intraoperatively, and is generally quite a challenge.
3. Joint distraction
Traction can be applied either manually or with a femoral distractor. These cases are challenging as there is no intact region under which to reduce the femoral head. Therefore, sufficient traction needs to be maintained while the wall fragment (and structural roof) are reduced and stabilized.
Because the patient is in the lateral position, and the extremity’s position manipulated frequently throughout the procedure, use of a fracture table to maintain traction is difficult. Therefore, femoral distractor is a very useful adjunct in these fractures patterns.
To apply the distractor, insert a 5 mm Schanz screw into the sciatic buttress proximally. Place a second Schanz screw into the femur at the level of the lesser trochanter.
Tension on the distractor can be adjusted as needed for visualization or reduction.
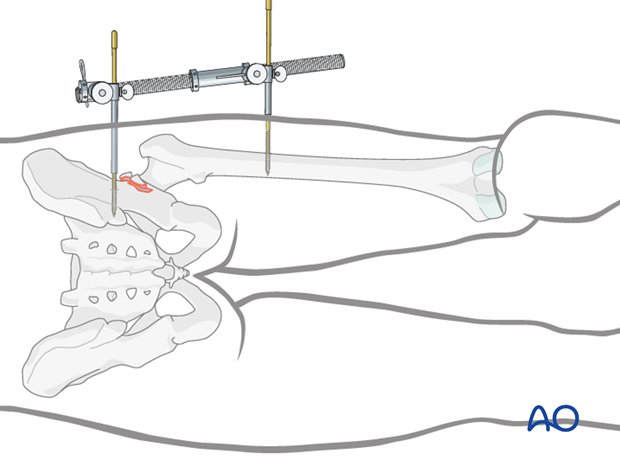
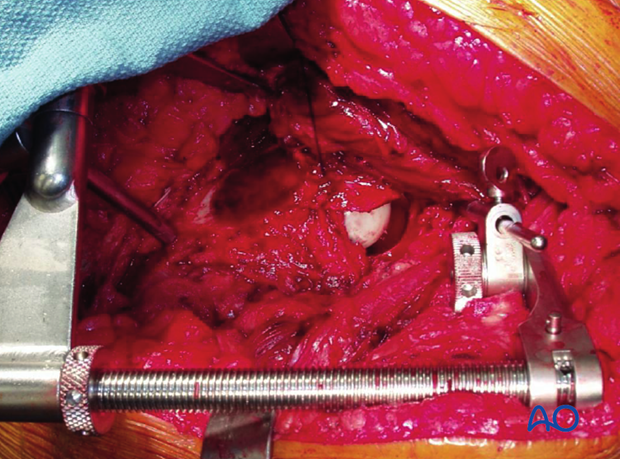
Once sufficient traction has been applied, the femoral head can be medialized into the remaining, intact acetabulum. This often requires readjustment of the distractor.
Teaching video
AO teaching video: Use of the distractor on the pelvis
4. Cleaning of the fracture site
Removal of incarcerated fragments
Commonly, there are incarcerated bone fragments that require removal.
In cases in which the reduction of the dislocated hip occurs intraoperatively, incarcerated fragments are removed prior to femoral head reduction. If the hip was successfully reduced preoperatively, joint distraction is required to remove the incarcerated fragments.
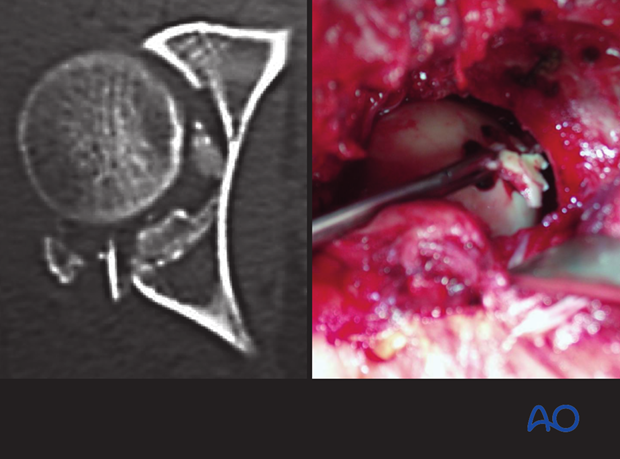
5. Reduction and stabilization of marginal impaction
Excessive joint distraction is maintained to reduce any regions of marginal impaction.
The surgeon inspects the articular surface for regions of marginal impaction, and will then use the femoral head and intact regions of the acetabular articular surface as a template for their reduction. Impaction is often difficult to detect, but mandatory to treat.
Marginal impaction is an area of articular surface, with its associated subchondral bone, that has been impacted into the metaphyseal bone at the leading edge of the fracture. The articular surface is displaced by the femoral head as it dislocates. Typically, the femoral head pushes the articular fragment into the intact, unfractured region of the stable segment.
- Marginal impaction that has been displaced by the femoral head dislocation
- Intact acetabular articular surface
Fracture impaction is often associated with posterior wall fractures. It causes joint incongruity, and deforms the fracture surfaces so that anatomical reduction is not possible until the impaction is corrected.
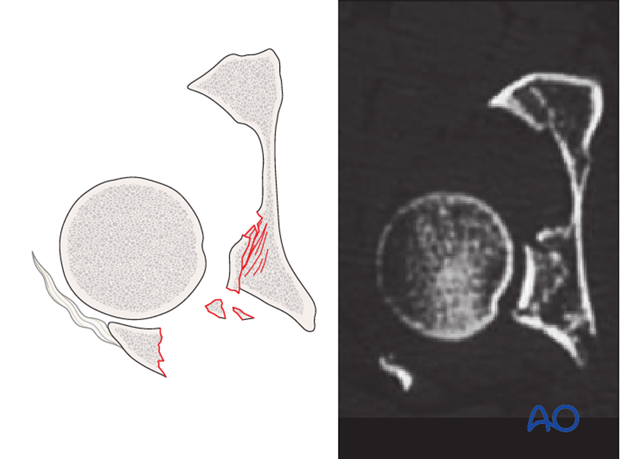
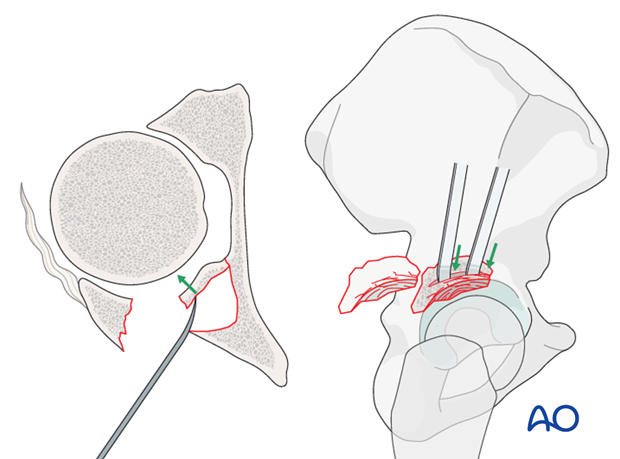
With the femoral head distracted to allow access to the impacted fragments, one can carefully elevate and mold the area, utilizing the femoral head as a template.
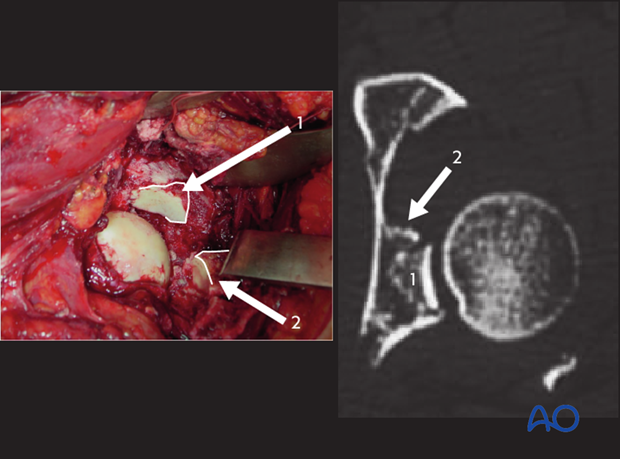
Clinical example 1
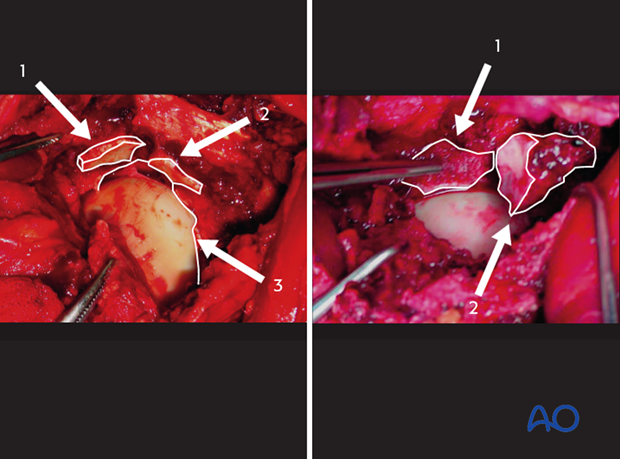
In the left clinical image, there are at least 3 specific fragments of the acetabular articular surface to identify.
- Displaced marginal impaction
- Displaced marginal impaction
- Intact region of acetabular articular cartilage
The femoral head will be used as a template, upon which to reduce the marginal impaction fragments. They will ultimately align with the intact region of acetabular articular cartilage as well.
Traction is adjusted until the femoral head is in a normal relationship with the unaffected region of the articular surface.
In the image on the right, the impacted fragment 1 has been mobilized and positioned to restore the normal relationship of this fragment with the femoral head. Of note, the surgeon has further displaced and mobilized fragment 2, which will be reduced next.
Filling the defect
Fill the metaphyseal defect left after reduction to the impaction with cancellous autograft or a structurally supportive bone substitute.
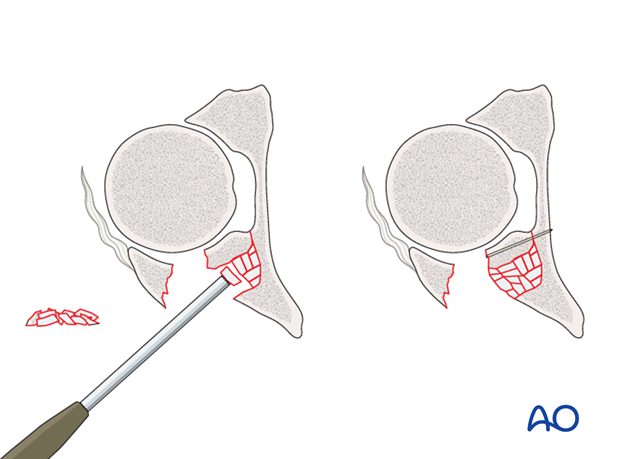
Fixation of marginal impaction
In osteochondral fragments large enough to support independent fixation, K-wire or mini fragment screws can be placed to maintain the reduced position.
Most commonly however, the impacted fragments have insufficient subchondral bone to support independent fixation. In these cases, supportive rafting occurs after the primary wall fragment has been reduced (see below).
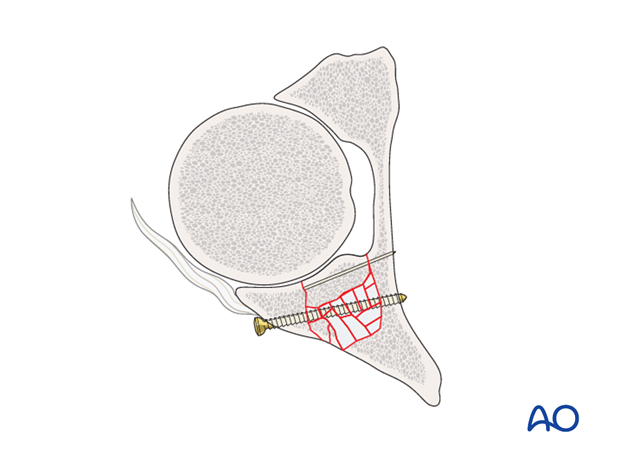
Clinical example 2
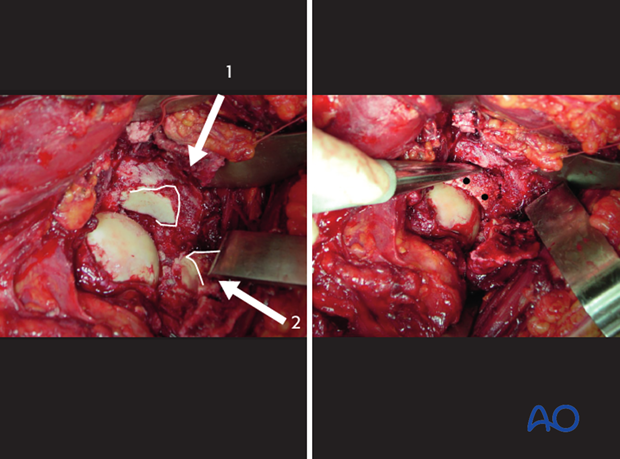
In this clinical example, a large fragment of marginal impaction (1) is seen to be impacted into the distal acetabular metaphysis.
On the right, this fragment has been reduced to its normal position, restoring the articular surface. The femoral head has been used as a template. This osteochondral fragment is large enough to support bio-absorbable pins as illustrated. These pins are drilled directly into the fragment itself to stabilize it.
6. Reduction and preliminary fixation of posterior wall fragment(s)
Reduction
After reduction of the marginal impaction, reduction and initial fixation of the posterior wall fragment are the next steps. In cases where the impacted fragments are too small to support independent fixation, the posterior wall fixation should provide a supportive “raft” as illustrated.
Supportive rafting occurs after the primary wall fragment has been reduced.
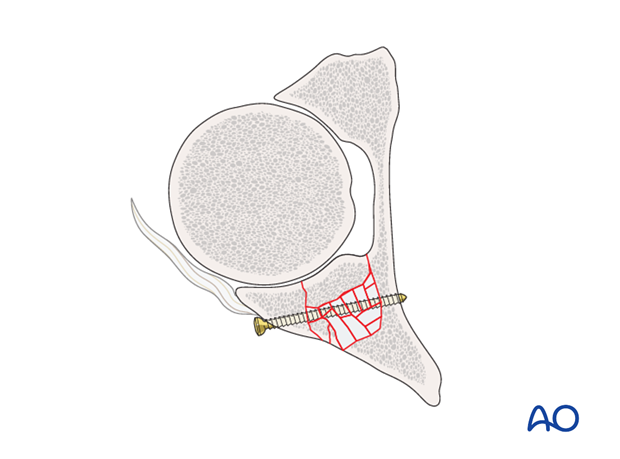
Use of pelvic reduction forceps or ball spike pusher
Reduction of superior posterior wall fragments generally requires multiple forces and adjuncts. If there is insufficient traction, or if the femoral head is not properly located within the acetabulum, it will be impossible to reduce this large cranial fragment into its native location. Readjustment of the femoral distractor is often required for additional traction at this point.
Ball spike pushers, dental picks, and modified hooks can be used to manipulate the fragment into its bed and compress the fractured edges. The reduction must be maintained manually until definitive fixation.
Occasionally, pelvic reduction forceps can be used for provisional stabilization and assist with reduction. A posterior clamp can often be applied through the sciatic notch. Additionally, an anterior clamp can be applied with the internal point placed submuscularly around the anterior border of the bone.
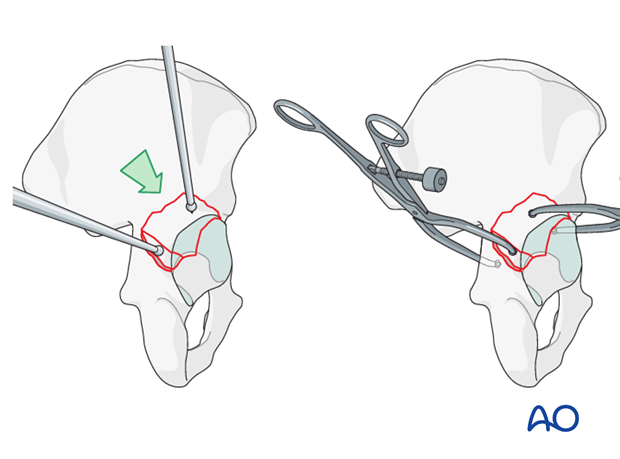
Preliminary K-wire fixation
Once the reduction has been obtained, provisional stabilization with K-wires may be possible. Alternatively, the reduction may be maintained manually with ball spike pushers, while lag screw fixation is obtained.

7. Definitive fixation
Lag screw fixation (large fragments)
The optimal, final construct involves fragment specific fixation as well as plate stabilization of the posterior wall.
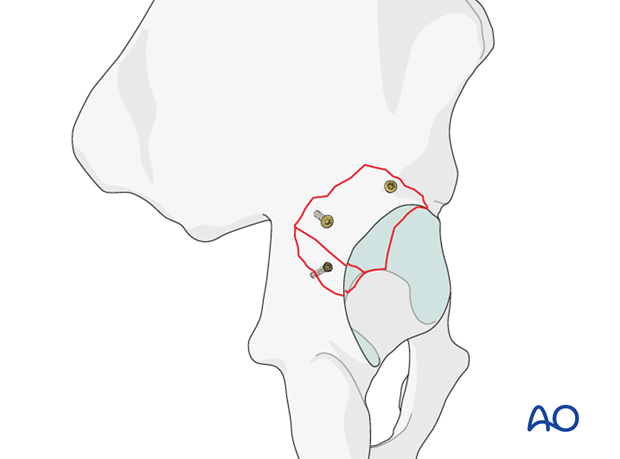
Fragment specific fixation will depend on the size and location of the fragments. Ideally, lag screw fixation of each fragment should occur as demonstrated in this illustration.
Screw size is determined by the fragment size, and can be 1.5 mm, 2.0 mm, 2.7 mm or 3.5 mm.
The superior posterior wall fracture fragments are commonly quite large and allow screw fixation into the sciatic buttress for excellent purchase. It is, however, common to encounter multifragmentary posterior wall fractures requiring smaller fragment fixation.
The final construct may require more than one plate (see below). Therefore, lag screw placement should be strategic so as not to block plate placement.
At times, 2.0 mm screws may be utilized to secure small peripheral posterior wall fragments. The definitive plate(s) may lie directly over these low-profile screws.
Of note, screws placed more peripherally, risk intraarticular penetration. The closer the screws are to the acetabular rim, the more dangerous due to the concavity of the acetabulum.
- Red zone: When placing screws within 10 mm of the acetabular rim, the screw trajectory must be parallel to the joint surface/cartilage.
- Green zone: Screws placed medial to the danger zone can be angled posteriorly but still avoiding intraarticular penetration.
Fragments that are small and peripheral can be challenging to stabilize due to the difficulty of interfragmentary screws penetrating the articular surface.
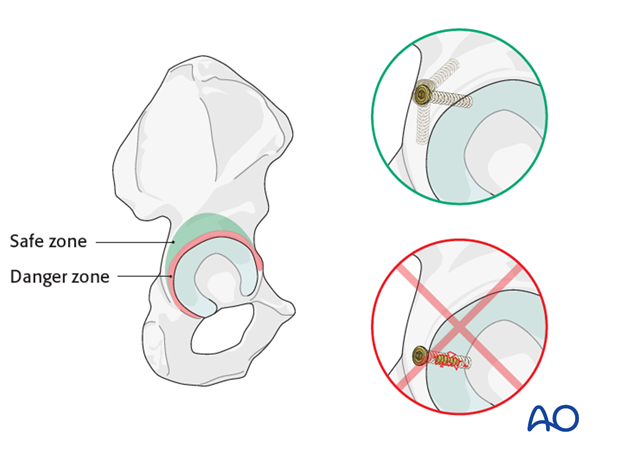
Plate fixation
The direction of displacement of the superior posterior wall fragments tends to be more cranial than traditional posterior wall fragments. Therefore, if buttress plates are to be used, they need to be applied in a different position.
Typically, buttress plates are placed anteriorly and cranially at the apex of the fracture. Depending on fracture morphology, interfragmentary screws inserted through the plate may be utilized. Or as illustrated, these plates may act as true buttress plates and thus do not require any distal fixation.
Regardless, multiple points of interfragmentary fixation are required independent of buttress plating.
In very large fragments, multiple buttress plates may be placed at different points at the apex to prevent displacement.
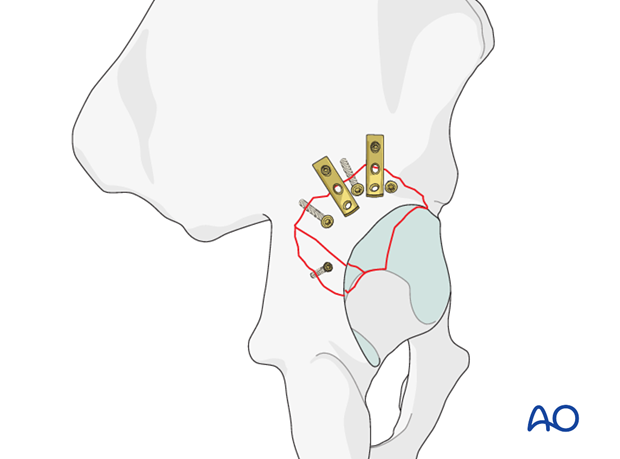
Depending on the fracture morphology, a single plate across the fragment may be preferred. This plate again does prevent cranial wall displacement and exerts a buttressing effect.
Interfragmentary screws are still required. In this case smaller fragment screws have been used not to obstruct plate location.
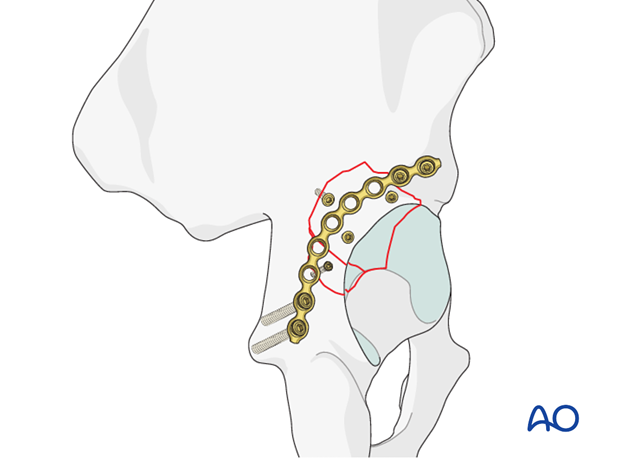
An additional reconstruction plate along the acetabular rim may be required in very large fragments. This will take careful contouring and be facilitated with a malleable template. Also, this plate may overlie mini fragment interfragmentary screws.
The distal end of the plate is precontoured to fit the concavity at the base of the ischium.
The proximal end of the plate curves cranially and anteriorly along the superior rim of the acetabulum and is rooted near the AIIS.
The optimal plate positioning is very peripheral/lateral, along the acetabular rim. Therefore, screws placed close to the acetabulum need to be angled superficially so as not to perforate the articular surface.
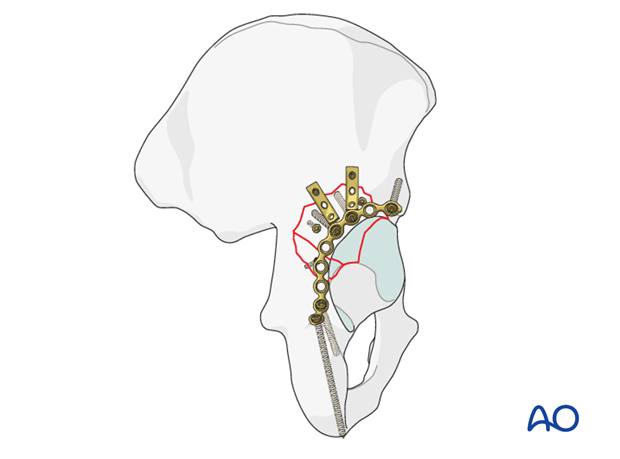
Pearl: spring hook plates
Stabilization of the posterior wall fragments sometimes requires spring hook plates to resist shearing forces on the fragment which are inserted either instead of lag screws, or before them to resist the shear created by the compression.
The spring hook plates should extend medially beyond the posterior wall buttress plate. These supplementary plates provide additional buttress support for the comminuted fragments.
The hooks must press on the bone fragments and not into the labrum.
Spring hook plates are available precontoured or made from small fragment one third tubular plates. For details see the corresponding basic technique.
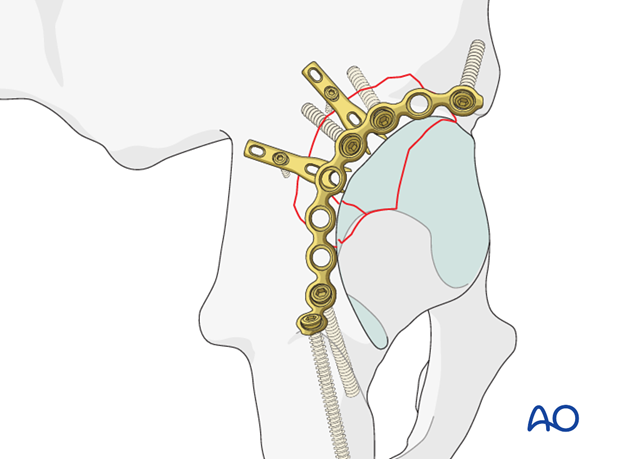
8. Radiographic assessment
Intraoperative confirmation of hardware position
There are multiple ways to verify that lag and plate screws are extraarticular. This is particularly important with any screws placed peripherally in the red zone.
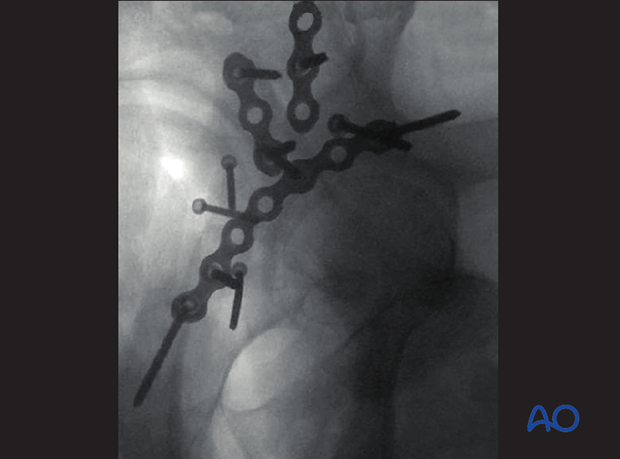
Intraoperative fluoroscopy can be used to verify that all implants are extraarticular in the majority of cases. In this case the image was obtained by rotating the C-arm into an excessive obturator oblique orientation. Alternatively, a direct lateral of the acetabulum may demonstrate the implants to be extraarticular.
If intraoperative fluoroscopy is insufficient, surgeon should verify that all implants are extraarticular by direct vision. One method is to drill for the interfragmentary screw, displace the fragment to verify that the hole is extraarticular, then re-reduce the fragment and place the screw after visualizing that the hole has not penetrated the cartilage.
Postoperative assessment
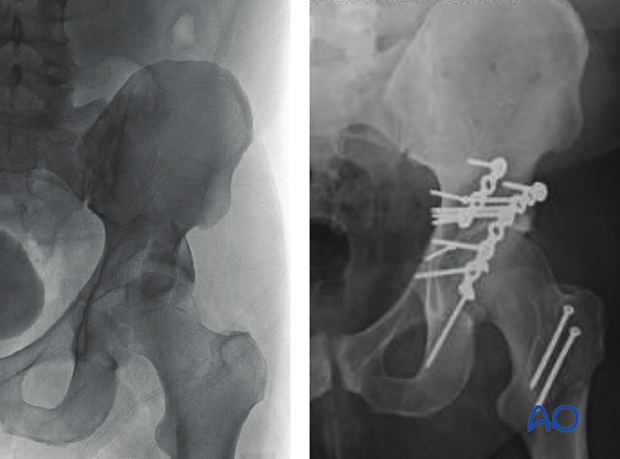
Postoperative radiographs are evaluated to ensure
- Concentric reduction of the femoral head without evidence of residual subluxation
- Anatomical reduction of the radiological roof
- Anatomical reduction of the caudal extent of the wall fragment with the ischium
- Extraarticular nature of all implants
- Anatomic reduction and secure fixation of the trochanteric osteotomy
9. Postoperative care
During the first 24-48 hours, antibiotics are administered intravenously, according to hospital prophylaxis protocol. In order to avoid heterotopic ossification in high-risk patients, the use of indomethacin or single low dose radiation should be considered. Every patient needs DVT treatment. There is no universal protocol, but 6 weeks of anticoagulation is a common strategy.
Wound drains are rarely used. Local protocols should be followed if used, aiming to remove the drain as soon as possible and balancing output with infection risk.
Specialized therapy input is essential.
Follow up
X-rays are taken for immediate postoperative control, and at 8 weeks prior to full weight bearing.
Postoperative CT scans are used routinely in some units, and only obtained if there are concerns regarding the quality of reduction or intraarticular hardware in others.
With satisfactory healing, sutures are removed around 10-14 days after surgery.
Mobilization
Early mobilization should be stressed and patients encouraged to sit up within the first 24-48 hours following surgery.
Mobilization touch weight bearing for 8 weeks is advised.
Weight bearing
The patient should remain on crutches touch weight bearing (up to 20 kg) for 8 weeks. This is preferable to complete non-weight bearing because forces across the hip joint are higher when the leg is held off the floor. Weight bearing can be progressively increased to full weight after 8 weeks.
With osteoporotic bone or comminuted fractures, delay until 12 weeks may be considered.
Implant removal
Generally, implants are left in situ indefinitely. For acute infections with stable fixation, implants should usually be retained until the fracture is healed. Typically, by then a treated acute infection has become quiescent. Should it recur, hardware removal may help prevent further recurrences. Remember that a recurrent infection may involve the hip joint, which must be assessed in such patients with arthrocentesis. For patients with a history of wound infection who become candidates for total hip replacement, a two-stage reconstruction may be appropriate.
Sciatic nerve palsy
Posterior hip dislocation associated with posterior wall, posterior column, transverse, and T-shaped fractures can be associated with sciatic nerve palsy. At the time of surgical exploration, it is very rare to find a completely disrupted nerve and there are no treatment options beyond fracture reduction, hip stabilization and hemostasis. Neurologic recovery may take up to 2 years. Peroneal division involvement is more common than tibial. Sensory recovery precedes motor recovery and it is not unusual to see clinical improvement in the setting of grossly abnormal electrodiagnostic findings.













