ORIF through sequential approaches
1. General considerations
General remarks for sequential approach
Any anterior approach ( modified Stoppa or ilioinguinal approach) can be combined with any posterior approach. Here a combination of the Stoppa approach with the patient in a supine position and, after repositioning to prone, the Kocher-Langenbeck approach is illustrated as the easiest and most reliable combination.
Sequence of treatment
In a sequential approach, the Stoppa window will be used to control all of the anterior column and free fragments of the quadrilateral surface.
The posterior approach will then complete the posterior column reduction and fixation.
The sequence of reduction of the associated both column fractures traditionally begins with reduction of the iliac wing to the intact ilium.
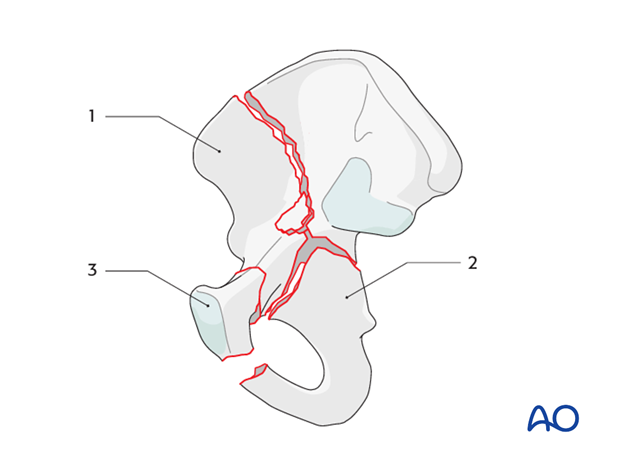
However, small inaccuracies at the level of the iliac crest can lead to significant malreduction at the joint line. Sequential reduction of the pelvic brim first, followed by reduction and stabilization of the high and mid portions of the anterior column (1) is more successful. If there is low anterior column involvement (3), this is subsequently reduced.
The posterior column (2) and any associated posterior wall component will be reduced and stabilized through the second approach.
Planning/templating
Preoperative templating is essential for understanding the complexity of an acetabular fracture.
When using implants on the innominate bone, it is important to know the best starting points for obtaining optimal screw anchorage (see General stabilization principles and screw directions).
2. Principles of reduction
Introduction
Some fractures can be treated with use of the Stoppa window only. The lateral window from the ilioinguinal approach will supplement this.
The Stoppa approach allows better control of the periacetabular column than the ilioinguinal approach, such that instead of beginning the reduction at the crest and then using the pelvic brim plate to neutralize the reduction, the pelvic brim plate is used to drive the reduction as well as stabilize it.
Indirect visualization
Unusually for a significant joint, articular reduction of acetabular fractures is indirect. The articular surface of the hip joint is not seen directly. Reduction must be assessed by the appearance of the extraarticular fracture lines and intraoperative fluoroscopic assessment. Some fracture lines are palpated manually but not seen directly such as transverse fracture lines on the quadrilateral plate.
Marginal impaction in the posterior wall fracture can be seen directly prior to final closure of the cortical fragment.
Quality of reduction
Posttraumatic arthrosis is directly related to the quality of reduction - the better the reduction, the greater the chance of a good or excellent result.
3. Application of traction
It is critical to ensure hip flexion to allow enhanced exposure of the iliac fossa and true pelvis.
The associated both column fractures result from a force applied to the greater trochanter, with medialization of the femoral head. In order to allow manipulation of both the anterior and posterior column fragments, the femoral head must be distracted. This is typically accomplished with the application of lateral and/or longitudinal traction.
The application of traction also provides indirect reduction, particularly of the anterior column.
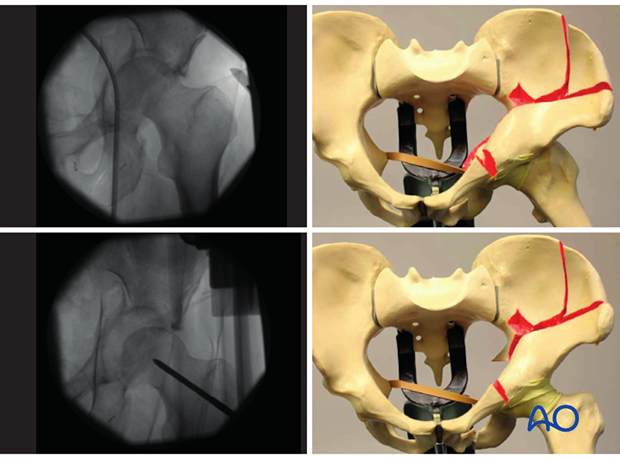
Traction can be applied in several ways with:
- The use of a fracture table that allows longitudinal and lateral traction
- The intermittent help of an assistant (may be unreliable in long procedures)
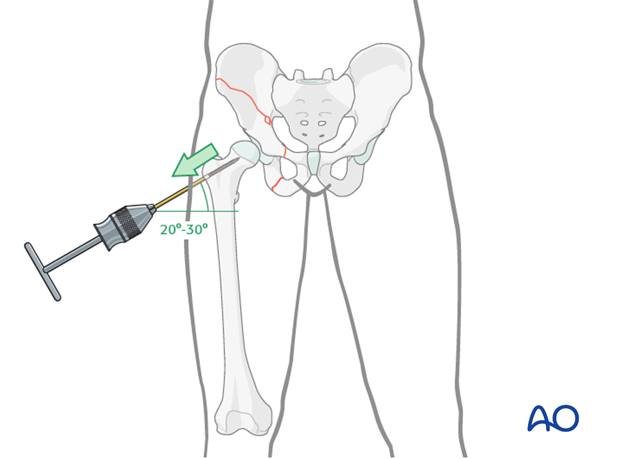
Apply longitudinal traction to the lower limb, and lateral traction through the greater trochanter.
Both these forces should be tuned until the best effect is obtained.
In some surgeon’s experience, the use of a traction table post or other traction frame is helpful during this operation.
Note
Excessive traction may limit fracture fragment mobility and interfere with reduction.
Teaching video
AO teaching video: Use of the distractor on the pelvis
4. Cleaning of the fracture site
Fracture sites are prepared by preliminarily increasing the displacement and then removing early callus and granulation tissue.
Joint distraction is extremely useful to facilitate this debridement.
5. Anterior column: reduction
Reduction of periacetabular fracture
The anterior column is reduced to the posterior ilium.
Restore the iliac fossa concavity by correcting external rotation and medial displacement of the deeper part of the anterior column fragment.
If required a small incision can be made in order to rotate the iliac wing internally using a ball spike pusher applied to the proximal posterior portion, near the pelvic brim, of the anterior column and a Farabeuf clamp positioned on the ASIS.
If indicated, use a Schanz screw that is driven into the AIIS combined with lateral traction on the femur to obtain the complete reduction.
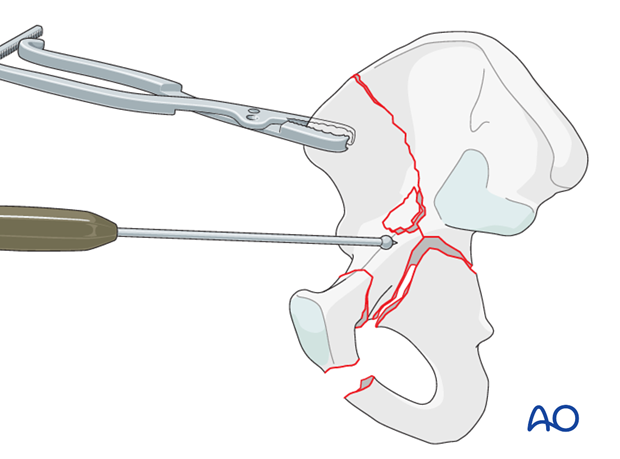
Use of a large symmetric reduction forceps (“King Tong”)
Additionally, or as an alternative, apply a large symmetric “King Tong” clamp around the anterior column and the fixed portion of the iliac wing to obtain correct rotation of the iliac wing and to restore the iliac fossa concavity.
Note
Excessive internal rotation will open the fracture on the opposite side.
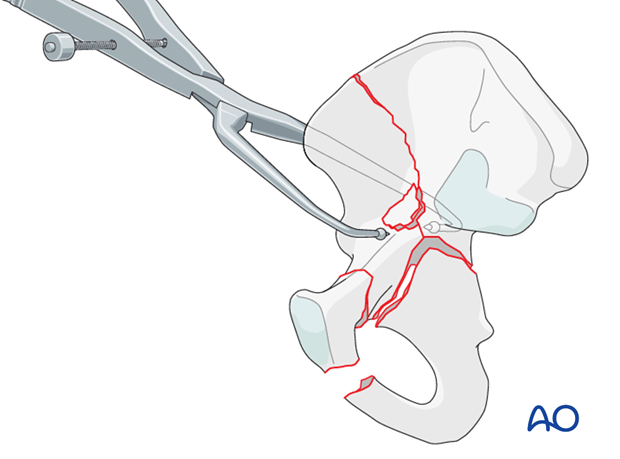
Plate as reduction aid
A powerful aid to reduction is a plate attached to the stable, posterior part of the ilium.
This plate is undercontoured to provide a push to the anterior column along the pelvic brim.
Place the distal part of the plate over the free anterior column fragment. Fix the plate with two cortical screws into the stable portion of the iliac wing. As its screws are tightened, the plate presses the anterior fragment into alignment with the intact ilium.
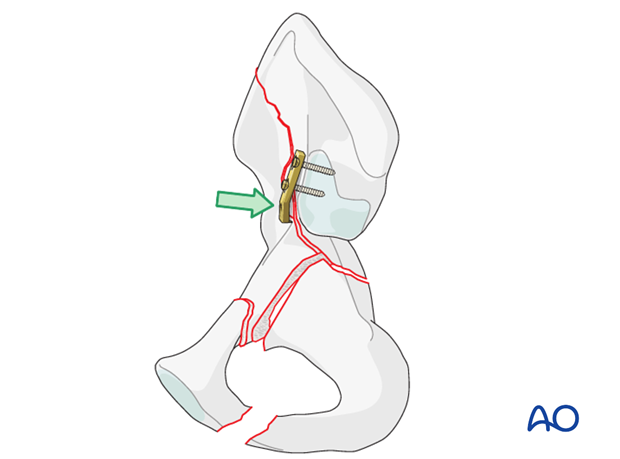
The reduction plate can be assisted with lateral femoral traction and the use of a Farabeuf clamp in the ASIS to obtain correct reduction.
Final fixation with a long reconstruction plate along the pelvic brim may require removal of the reduction plate.
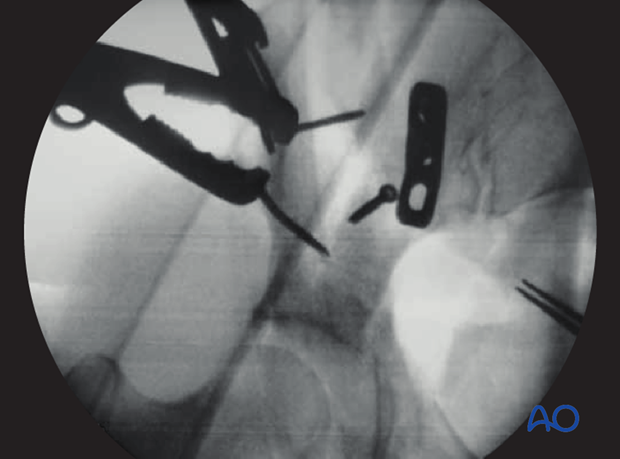
Reduction of the iliac wing
Once the periacetabular fracture is controlled reduction of the iliac wing to the intact ilium (portion of the ilium that remains normally associated with the sacrum) can begin if required.
High fractures will be adequately controlled by the fixation at the pelvic brim. It may be necessary to supplement this with the addition of a lateral window.
With an approach through a small lateral window, direct reduction and screw or plate fixation can be completed.
Start reduction from the proximal aspect of the iliac wing. Reduce accessory fragments of the iliac wing, if present.
It is important to restore the normal curvature of the iliac wing, and not to straighten it excessively.
Pointed reduction forceps applied to the iliac crest can serve as handles for reduction, and also for temporary fixation.
Alternatively, apply a Farabeuf clamp over screws placed into the crest on each side of a fracture line.
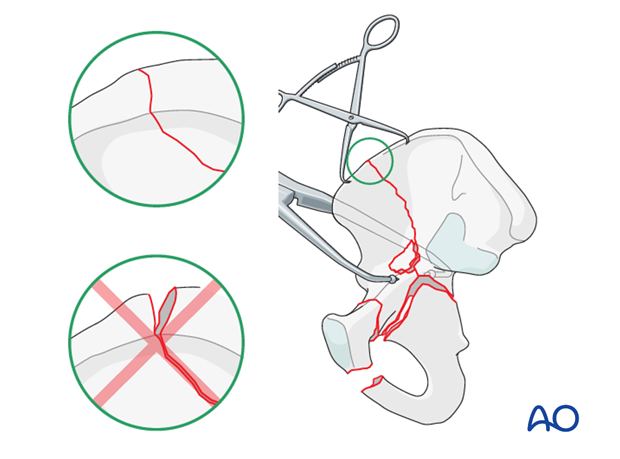
Fixation of the iliac wing
Iliac wing fractures can be fixed with lag screws (3.5 mm) near the crest.
Alternatively, one can use pelvic reconstruction plates applied to the inner surface of the iliac crest.
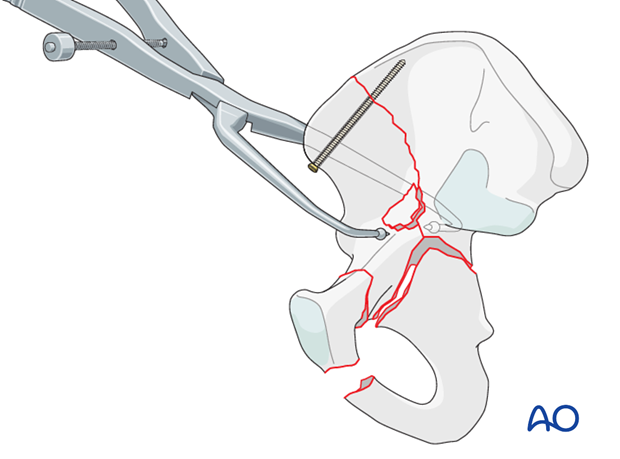
Pelvic brim fragment
Very commonly, there is a large separate fragment of bone just above the point that the anterior column fracture crosses the pelvic brim. This fragment must be reduced anatomically to allow a read of the anterior column reduction.
Manipulation with a dental pick and pressure with a ball spike pusher are helpful.
Once successfully reduced, provisional fixation with a K-wire may be useful. If the fragment is large enough, a 2.4 mm or a 3.5 mm screw can secure this fragment.
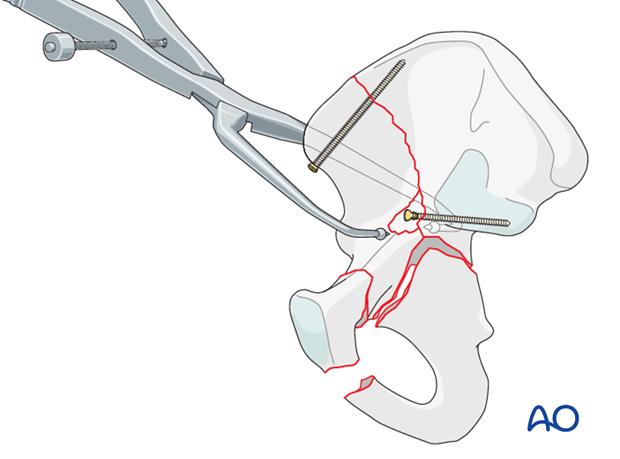
6. Anterior column: fixation
Components of fixation
Depending on the fracture configuration, a combination of the following fixation methods may be used:
- Small fragment lag screws stabilizing the anterior column to the reconstructed ilium
- A contoured pelvic brim buttress plate. This plate can be contoured to extend across the low anterior column to the pubis, as required by the specific fracture. Of note, fixation of the posterior column commonly occurs through the pelvic brim buttress plate as illustrated.
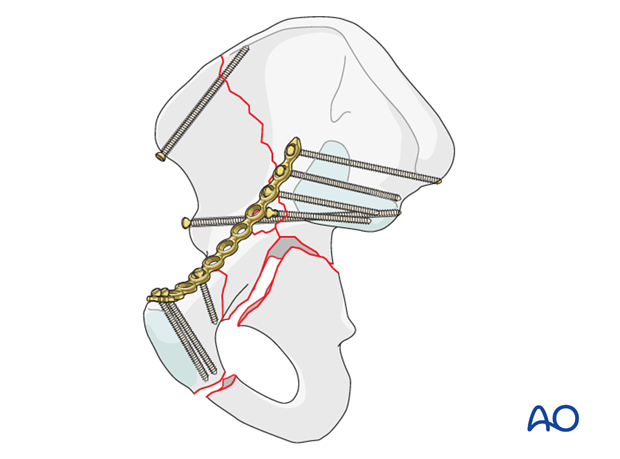
Iliac screws
Stabilize the anatomically reduced anterior column to the reconstructed ilium with one or more screws between the inner and outer cortex.
Small fragment screws placed along the iliac crest stabilize the proximal fracture line. Alternatively, one can use pelvic reconstruction plates applied to the inner surface of the iliac crest.
Iliac corridor screws can be applied beginning lateral to the anterior inferior iliac spine (AIIS) and directed into the posterior innominate bone, just lateral to the sacroiliac joint. This corridor is commonly large enough to accommodate two 3.5 screws or a 4.5 screw. Care should be taken to avoid perforating the inner or outer cortex of the ilium prematurely. C-arm imaging can be used to ensure that these screws stay between the surfaces to the posterior border of the bone.
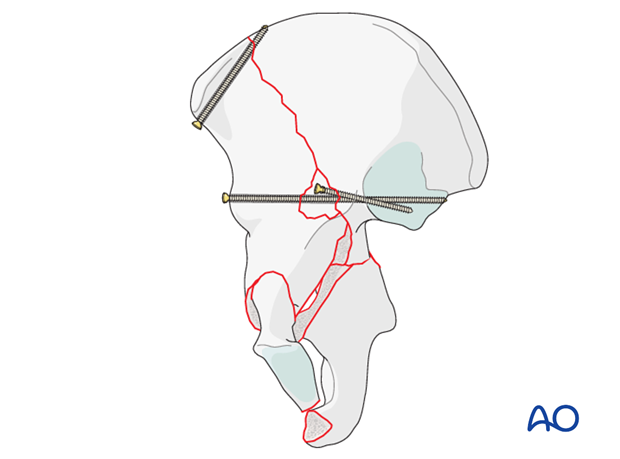
Contouring and applying a pelvic brim plate
Most commonly a pelvic brim plate will be used for the final construct. It will be contoured and applied to the anterior column at this point, though the fixation of the posterior column is performed after subsequent reduction.
The plate must be long enough to provide adequate fixation of both posterior and anterior injuries. This typically requires extension to the pubic body.
The use of a malleable template aids plate contouring.
Because the primary purpose of this plate is to buttress the anterior column, posterior contouring is most critical. For this reason, plate fixation normally starts posteriorly and proceeds anteriorly. Final adjustment of the plate profile can be achieved in situ, due to plate malleability.
Tools for in situ plate contouring include the ball spike for pushing, ...
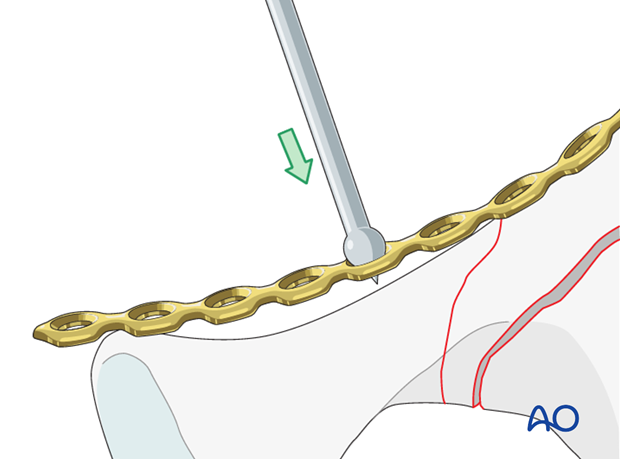
... and large and small fragment screwdrivers for torsional adjustment.
Apply the plate along the pelvic brim spanning from the innominate bone adjacent to the SI joint to the pubis.
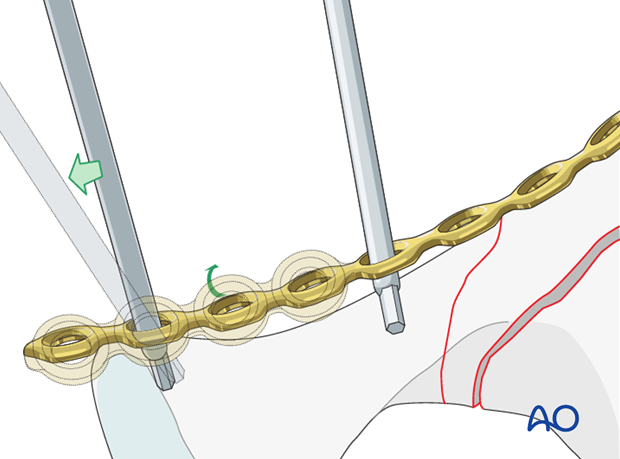
Plate fixation of the anterior column
The cranial most screws are placed parallel to the SI joint, anchoring the plate to the sciatic buttress. This provides assistance with the reduction (as previously described) as well as definitive buttress stabilization of the anterior column.
Screws can be placed through the plate into the reduced anterior column fragment, depending on the fracture morphology.
At this point, it is critical to ensure that no screws cross into the posterior column fracture or fragment. This would block the reduction of the posterior column fragments.
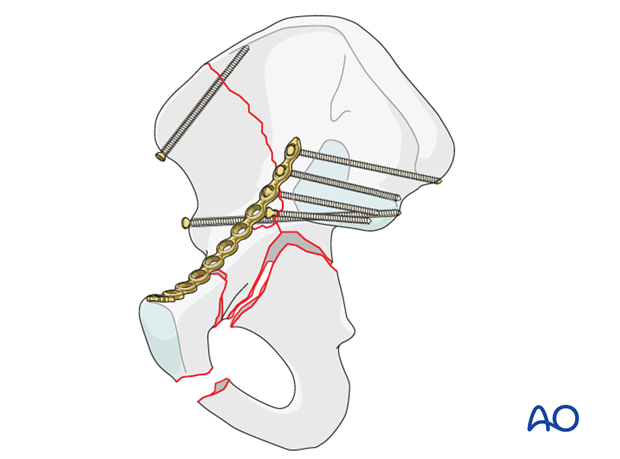
Reduction of distal anterior column fracture
Once the posterior column is definitively reduced and fixed, reduction of the distal anterior column may be required.
Indications for anatomic reduction and fixation of the distal anterior column include cases in which this fracture is articular involving the distal anterior wall and segmental fractures of the anterior column
This reduction is commonly accomplished utilizing pointed reduction forceps.
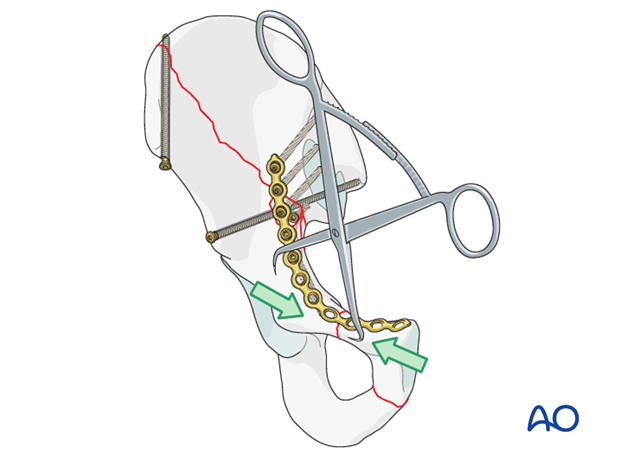
Fixation of distal anterior column fracture
Once the low anterior column and segmental portions of the anterior column have been successfully reduced, fixation through the previously contoured pelvic brim plate can be achieved.
Additional in situ contouring can be required as previously described.
Additional screws in the medial superior ramus and pubic body are inserted as needed.

7. Posterior column: reduction
Repositioning of the patient and Kocher-Langenbeck approach
At this stage of the surgery the anterior exposure is closed, the patient is repositioned prone and the posterior column exposed through the Kocher-Langenbeck approach.
The nature of the posterior column and posterior wall fracture which occurs as part of the associated both column fracture is often less displaced and less mobile than occurring in isolation.
It may be possible therefore to control the entire posterior injury with a single plate after reduction of both elements.
Ischial Schanz screw as handle
A Schanz screw is placed into the ischial tuberosity to act as a handle or joystick. This is a key aid for manipulating the posterior column fragment.
The orientation of the screw is directed from lateral to medial and is typically applied through the muscular insertions overlaying the tuberosity. The muscles do not need to be elevated from the bone to allow screw placement.
Care should be taken to avoid blocking the fracture environment with this screw. A proximal to distal trajectory should be avoided, as the Schanz screw will block subsequent adjuncts for fracture reduction at the retroacetabular surface.
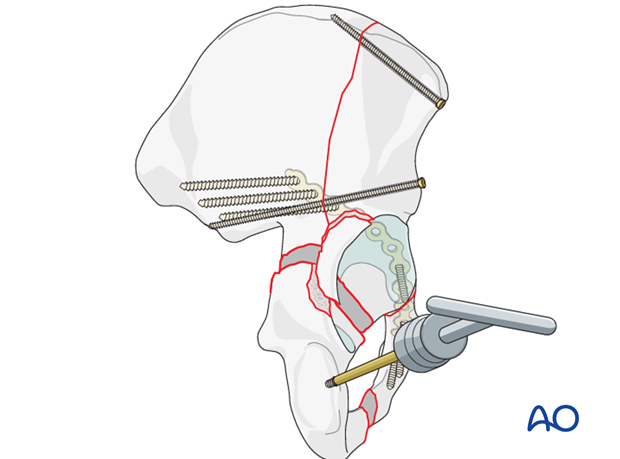
Use of pointed push pull devices
Fracture adjustment requires fine manipulation at the fracture itself. There are several adjuncts that can accomplish this fine adjustment.
Rotation and fine adjustment of this fragment is aided with a bone hook, sharp dental hooks, and/or ball spike pusher.
Manipulation with a hook placed as shown demonstrates mobility of the posterior column, and helps in the reduction. If reduction is difficult, check the fracture site for interposed debris.
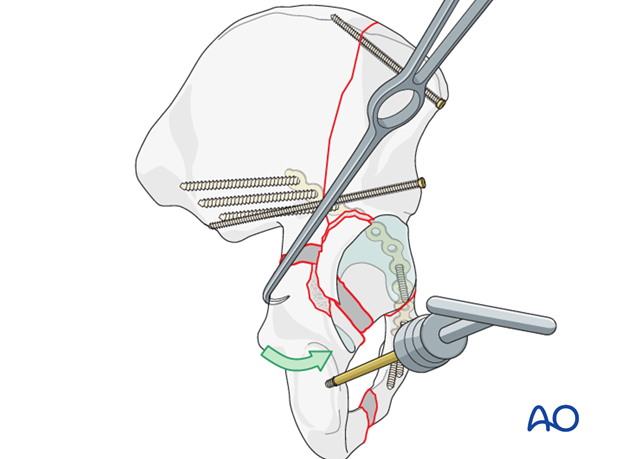
Use of pointed reduction forceps
The pointed reduction forceps is a very powerful way of manipulating the reduction along the fracture line and applying compression.
Due to the convexity of the bone, small holes may need to be drilled into the cortex to allow clamp application, and to prevent the points from slipping.
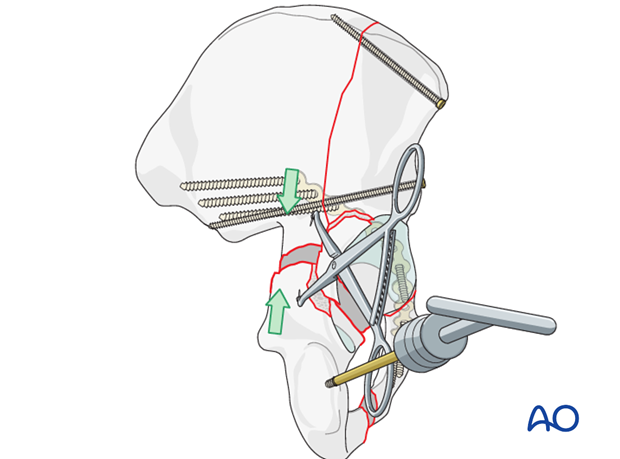
Use of a Farabeuf clamp
This clamp has jaws shaped to fit around screw heads. It can be used to compress fracture surfaces with two properly placed 3.5 mm cortical screws. They should be securely placed, and a little prominent, to be grasped by the clamp.
Properly placed, this clamp can both de-rotate the posterior column, and approximate the fracture fragments.
Care should be taken, as poor clamp placement may pressure the sciatic nerve.
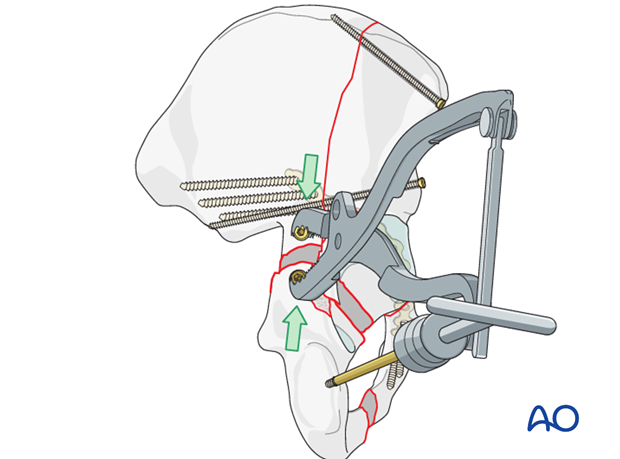
Use of a Jungbluth clamp
The Jungbluth pelvic reduction clamp is a similar alternative, which requires a larger exposure and also depends upon proper screw placement so that the forces applied by the clamp correctly realign the fracture.
A proximal screw is placed in the superior portion of the iliac wing above the acetabulum.
A distal screw is placed in the posterior column above the ischial tuberosity.
Their positions determine the direction of applied force, and this must be perpendicular to the fracture plane.
The use of the screw-dependent clamps (the Jungbluth and Farabeuf) creates the potential problem of screw traffic. Care must be taken to avoid placing these screws in the way of provisional and definitive fixation screws.
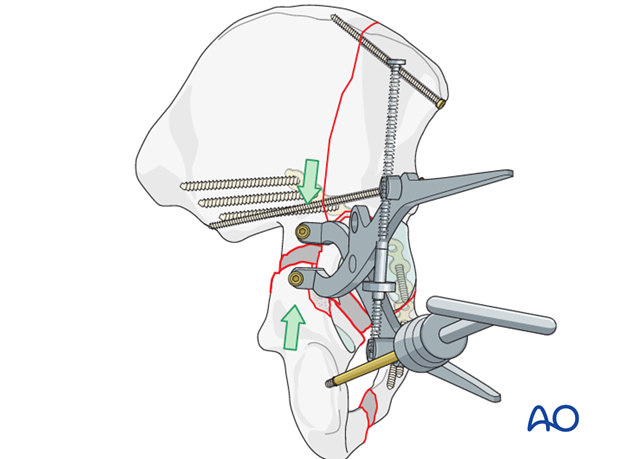
Articular surface reduction
Displace the wall fragment as necessary to see the posterior column reduction. Reduction must be perfect. The posterior column fragment must be manipulated into anatomical alignment with instruments as described above. Manipulation of the T-handle Schanz screw is a significant aid.
Pulling it posteriorly will help to close the fracture. Translation and rotation may require assisting instruments.
To mobilize the posterior column in cases older than 3 weeks, cut the sacrospinous ligament at its insertion. Alternatively, osteotomize the ischial spine.
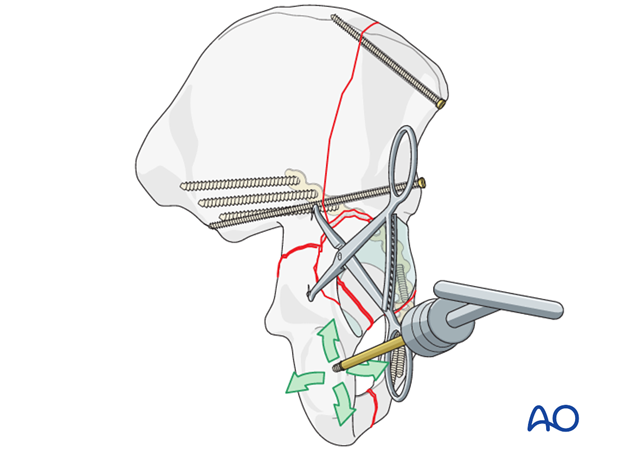
Examine the result
Examine the reduction by inserting a finger or an appropriate instrument along the quadrilateral plate.
With a satisfactory reduction, the quadrilateral surface should have no palpable gap or step-off.
Reduction can also be checked by opening the hip capsule with an incision parallel to the acetabular border, avoiding damage to the labrum. Inspection of the joint surface demonstrates reduction.
If the posterior column is satisfactorily reduced, it will be possible to place the posterior wall fragment into its bed anatomically, and this should be confirmed.
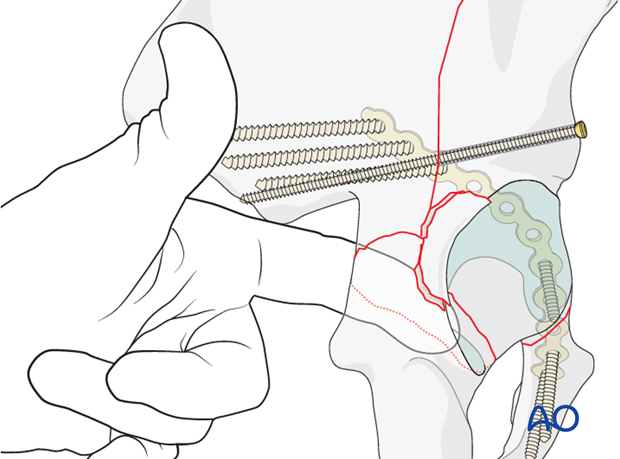
8. Posterior column: initial fixation
Interfragmentary lag screw
In the posterior column the screw is placed in the distal fragment into the posterior buttress of the ilium. The trajectory of this screw often requires a percutaneous insertion through the posterior gluteus musculature. Great care must be taken not to compromise the sciatic nerve.
The gliding hole may be drilled before reduction to ensure its proper placement.
Screw placement must allow optimal plate positioning as described below.
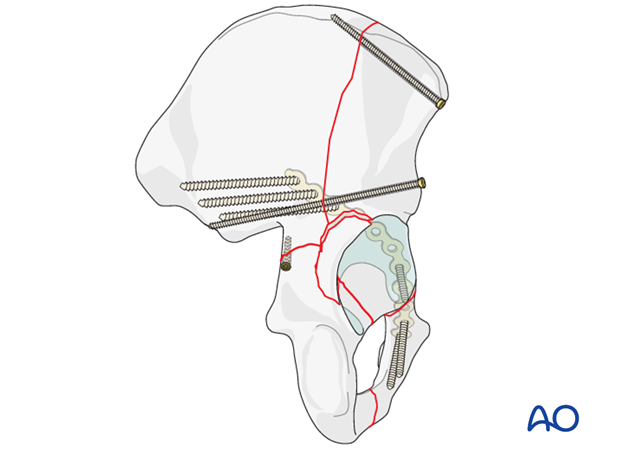
9. Posterior wall: reduction and fixation
Reduction with a ball spike pusher or pelvic reduction forceps
Reposition the wall fragment in its bed and compress it into place. Remember that this may be more difficult should the fragment be comminuted.
A ball spike pusher can be used to compress and maintain the reduction until definitive fixation.
It may be necessary to stabilize the fragment with a K-wire or two before proceeding.
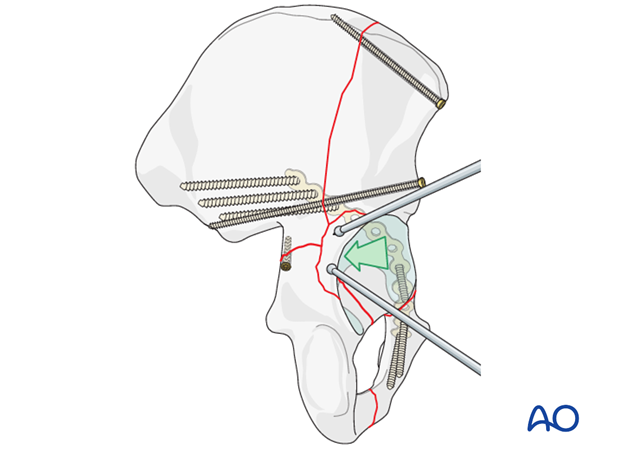
Alternatively, this can be done with a pelvic reduction forceps with pointed ball tips.
One tip is inserted through the greater sciatic notch, against the quadrilateral lamina. The other is placed on the wall fragment and the clamp is tightened.
Confirm reduction before proceeding.
It is important to avoid placing fixation screws into the hip joint. Thus the surgeon must remember the joint location which will be obscured by posterior wall reduction.
One may even consider drilling the posterior wall gliding holes before reduction.
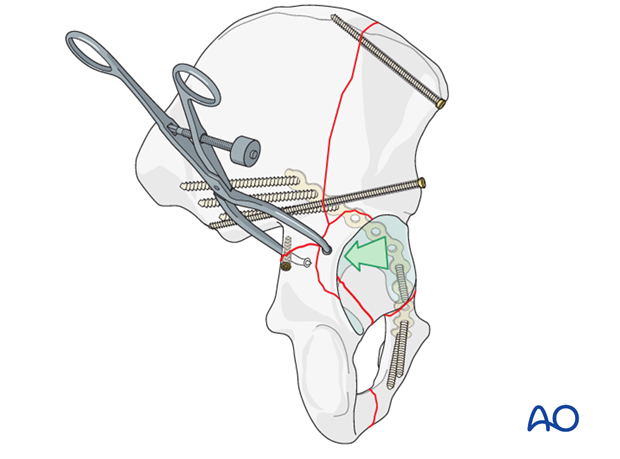
Lag screw fixation
Typically the medial edge of the posterior wall fragment is very thin. Screws should be placed laterally enough to capture a thicker part of the bone, while carefully avoiding the joint.
Predrilling the fragment before reduction may be helpful.
These lag screws may be in the way of the posterior plate. If possible, place them medially to it, or place the plate over the screw heads.
Typically, 2.7 mm screws can be used, having “drilled” the hole with a long 2 mm wire.
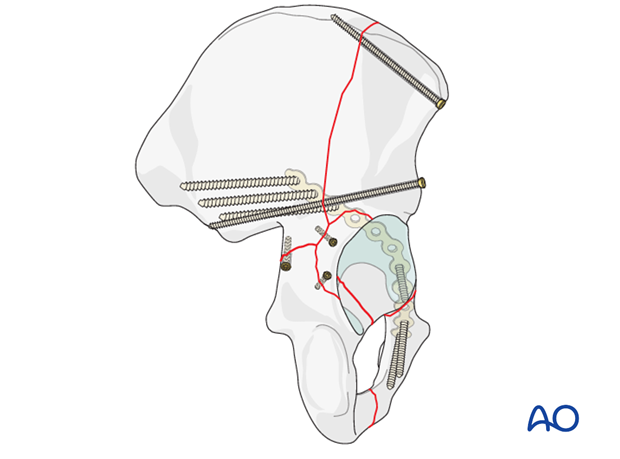
10. Finalizing the fixation
Contouring of the plate with a template
In addition to the lag screws, a reconstruction plate will be applied. The two points of fixation will provide torsional stability to the ultimate construct.
A reconstruction plate is chosen to reconstitute the structural stability of the native posterior column and the sciatic buttress. Ideally, it will be applied to the mid-column and contoured to obtain purchase in the strong bone of the sciatic buttress to control both the column and the wall fragments.
An aluminum template can be bent to fit the pelvis in the optimal location. The plate positioning will be limited cranially by the superior gluteal nerve and vascular pedicle. The distal end of the plate will be contoured to optimize screw positioning down the ischial ramus.
The plate contour should enforce the vectors required for the reduction.
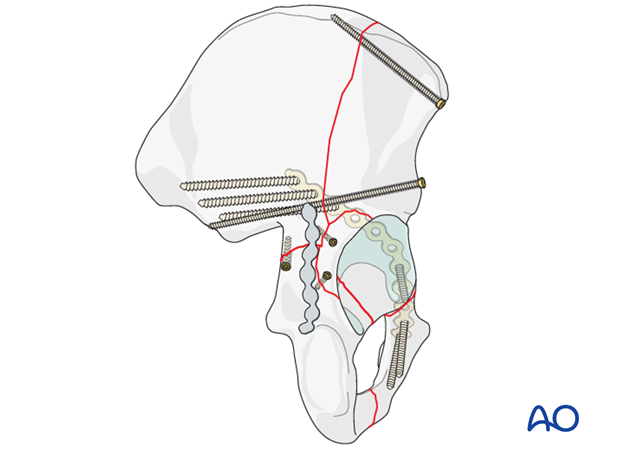
Application of the reconstruction plate
Definitive stabilization is obtained by adding the reconstruction plate spanning the posterior column and anchored securely to the ilium and ischium.
The screws placed in the periarticular portion of the plate must be positioned carefully to avoid intraarticular perforation. This becomes more probable as the plate is positioned laterally and closer to the acetabular rim.
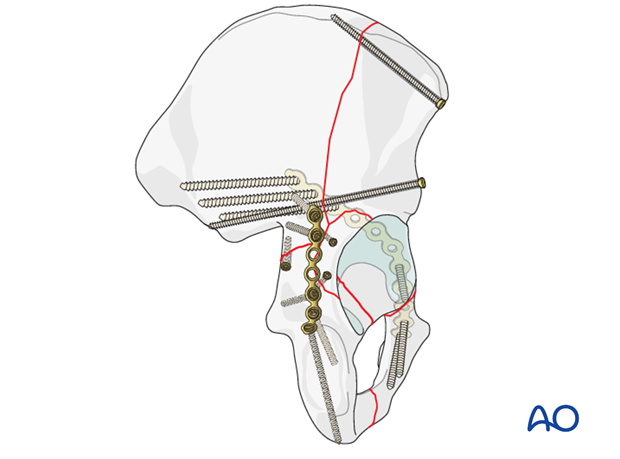
Pitfall: Injury to gluteal vessels and nerve
Proximally, retraction and plate and screw placement may result in neurovascular injury. Careful retraction and attention to plate location are essential to protect these fragile structures.
11. Final radiographic assessment
Once all fixation is in place, confirm the appropriate appearance of AP, obturator oblique and iliac oblique views and check the location of any screw that is placed near the hip joint.
The AP view should be inspected to assure that congruence has been obtained. The femoral head should have the same relationship to the radiological roof, the anterior rim and the posterior rim as on the contralateral side.
The pelvic brim plate should be secured to the intact ilium just lateral to the SI joint. The screws placed in the mid-section of the plate securing the posterior column reduction should be close to the ilioischial line.
If the low anterior column was affected, the obturator foramen profile and symphysis should be inspected to assess the quality of the distal reduction.
The obturator oblique should be inspected to ensure that there is no residual subluxation of the femoral head. The reduction of the anterior column should be assessed.
Both columns should be reduced to the intact ilium such that the ‘spur sign’ is no longer visible.
If a posterior wall fragment was involved, it should be seen as reduced and stabilized.
The iliac oblique should be inspected to ensure that the posterior column reduction is anatomic.
The restoration of the iliac wing should be confirmed.
Postoperatively, obtain formal high-quality radiographs of AP and both oblique views.
12. Postoperative care
During the first 24-48 hours, antibiotics are administered intravenously, according to hospital prophylaxis protocol. In order to avoid heterotopic ossification in high-risk patients, the use of indomethacin or single low dose radiation should be considered. Every patient needs DVT treatment. There is no universal protocol, but 6 weeks of anticoagulation is a common strategy.
Wound drains are rarely used. Local protocols should be followed if used, aiming to remove the drain as soon as possible and balancing output with infection risk.
Specialized therapy input is essential.
Follow up
X-rays are taken for immediate postoperative control, and at 8 weeks prior to full weight bearing.
Postoperative CT scans are used routinely in some units, and only obtained if there are concerns regarding the quality of reduction or intraarticular hardware in others.
With satisfactory healing, sutures are removed around 10-14 days after surgery.
Mobilization
Early mobilization should be stressed and patients encouraged to sit up within the first 24-48 hours following surgery.
Mobilization touch weight bearing for 8 weeks is advised.
Weight bearing
The patient should remain on crutches touch weight bearing (up to 20 kg) for 8 weeks. This is preferable to complete non-weight bearing because forces across the hip joint are higher when the leg is held off the floor. Weight bearing can be progressively increased to full weight after 8 weeks.
With osteoporotic bone or comminuted fractures, delay until 12 weeks may be considered.
Implant removal
Generally, implants are left in situ indefinitely. For acute infections with stable fixation, implants should usually be retained until the fracture is healed. Typically, by then a treated acute infection has become quiescent. Should it recur, hardware removal may help prevent further recurrences. Remember that a recurrent infection may involve the hip joint, which must be assessed in such patients with arthrocentesis. For patients with a history of wound infection who become candidates for total hip replacement, a two-stage reconstruction may be appropriate.
Sciatic nerve palsy
Posterior hip dislocation associated with posterior wall, posterior column, transverse, and T-shaped fractures can be associated with sciatic nerve palsy. At the time of surgical exploration, it is very rare to find a completely disrupted nerve and there are no treatment options beyond fracture reduction, hip stabilization and hemostasis. Neurologic recovery may take up to 2 years. Peroneal division involvement is more common than tibial. Sensory recovery precedes motor recovery and it is not unusual to see clinical improvement in the setting of grossly abnormal electrodiagnostic findings.













