Anterior corpectomy and stabilization
1. Preliminary remarks
Preoperative planning
Based on CT and MRI imaging, a plan should be prepared to determine:
- The size and optimal location of implants used
- Whether spinal cord decompression is necessary and if so, the amount of tissue to remove in order to achieve sufficient spinal cord decompression
Every case will be unique, and we will here illustrate just one example.
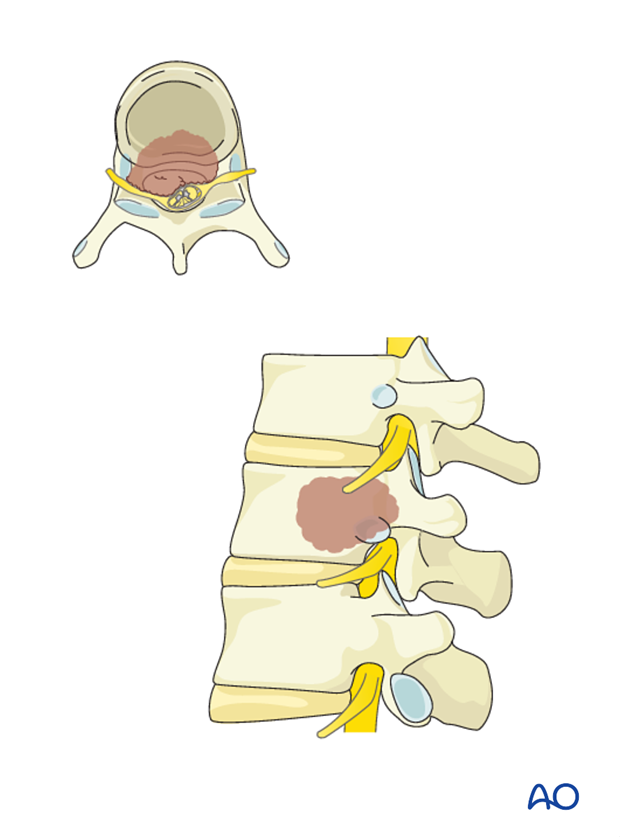
The anterior stabilization can be used as a stand-alone method in patients with tumors in the vertebral body without tumor extension into the posterior elements.
When resection of anterior and posterior column is required in the surgical management of metastatic spine disease, bilateral posterior pedicle fixation above and below the anterior construct should be used.
Use of dexamethasone
Administration of dexamethasone (10 mg bolus, 4 mg every 6 hours) is recommended as soon as ESCC causing neurologic deficit is diagnosed. Dexamethasone should be stopped or tapered as soon as spinal cord decompression is completed.
Embolization
Embolization procedures are recommended to reduce operative blood loss in hyper vascular tumors, especially for larger resections.
2. Patient positioning and surgical approach
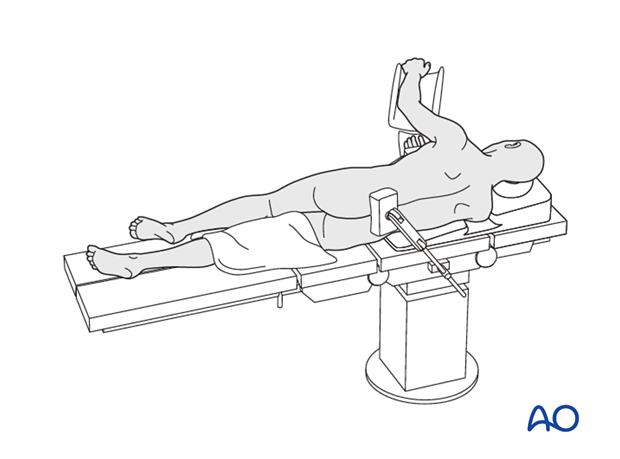
For this procedure the patient is placed in the lateral decubitus. Depending on the level involved one of the following approaches can be used:
3. Anterior decompression
Timing
A patient who is experiencing neurologic deficit from solid tumor ESCC resulting in loss in ability to ambulate, in the absence of medical and oncological contraindications, requires urgent surgical decompression.
Expeditious diagnosis and prompt surgery are recommended to improve the probability of neurological recovery.
Discectomy
For a complete corpectomy, discectomy is performed both above and below the involved vertebra.
Special consideration for thoracic spine
In cases where it is necessary to decompress the spinal cord, it may be necessary to remove the rib head and pedicle to identify the spinal canal.
In this case, the rib head is removed with a burr or osteotome.
After this step the procedure is identical for the thoracic and the lumbar spine and the illustrations will be shown without rib.
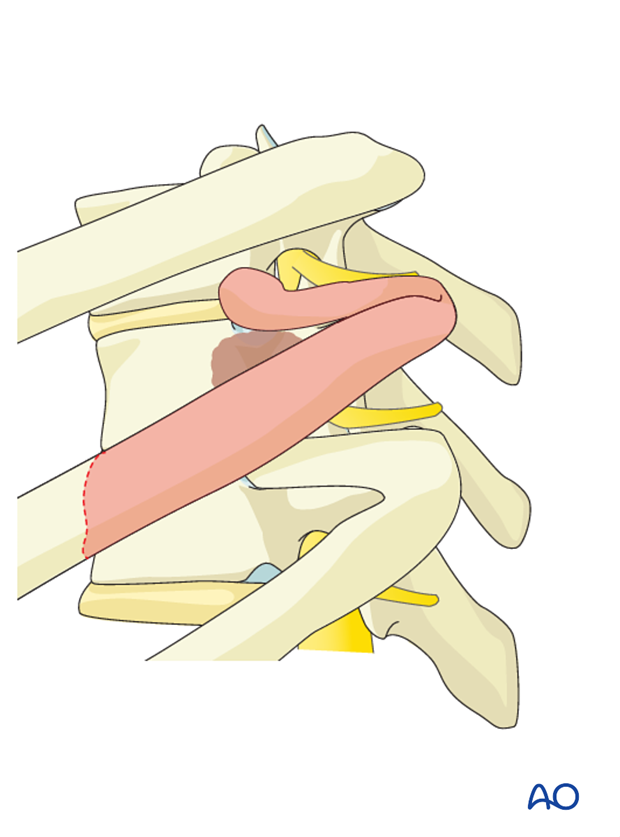
The pedicle is identified and removed with a high speed burr and Kerrison rongeur. This allows identification of the exiting nerve root and location of the dural tube.
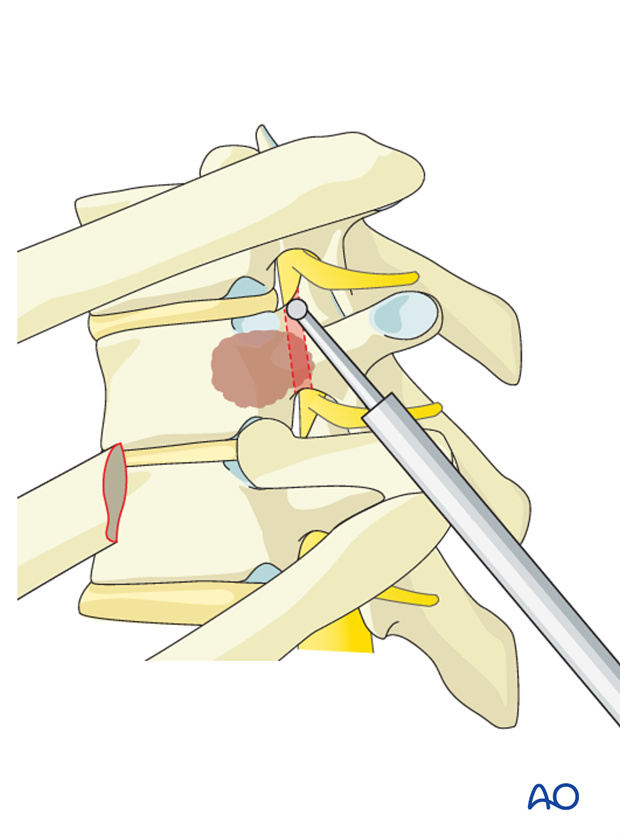
Attention is now given to the disc itself. A bony opening is created in the shape of a triangle where the larger base is located adjacent to the spinal canal, removing a portion of the respective endplates above and below the disc.
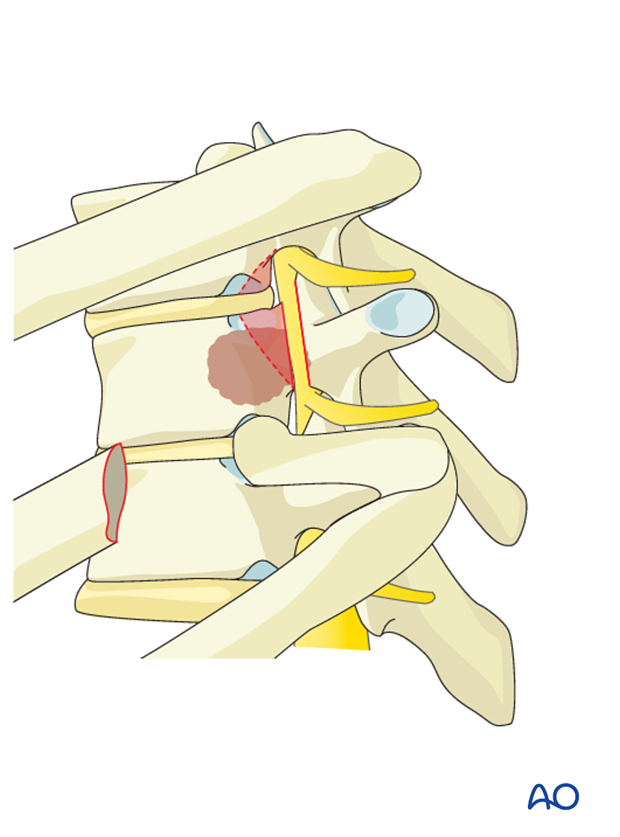
The disc and adjacent endplates are removed through expansion of the bony opening, working anteriorly and inferiorly. This allows minimal if any manipulation of the spinal cord.
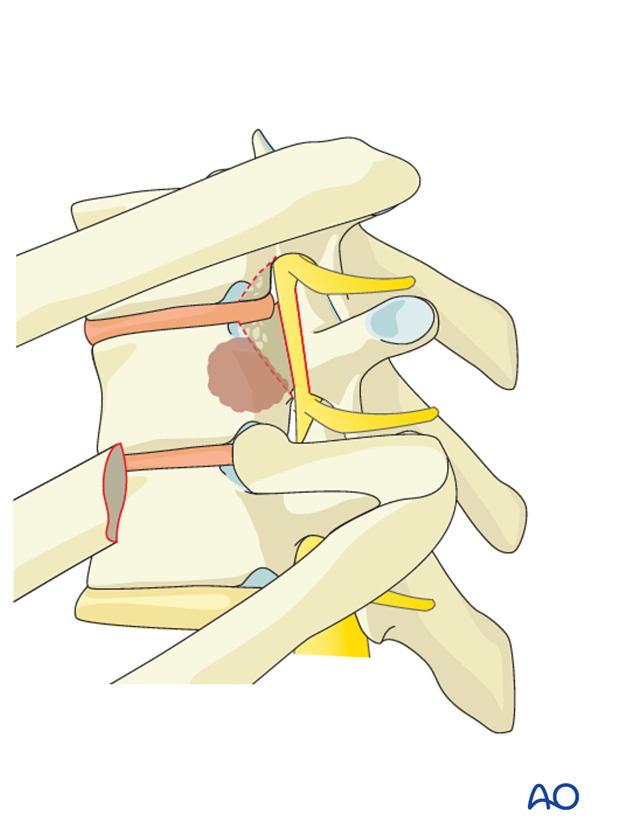
The disc is often removed by incising the annulus fibrosis and using a series of Kerrison rongeurs and curettes.
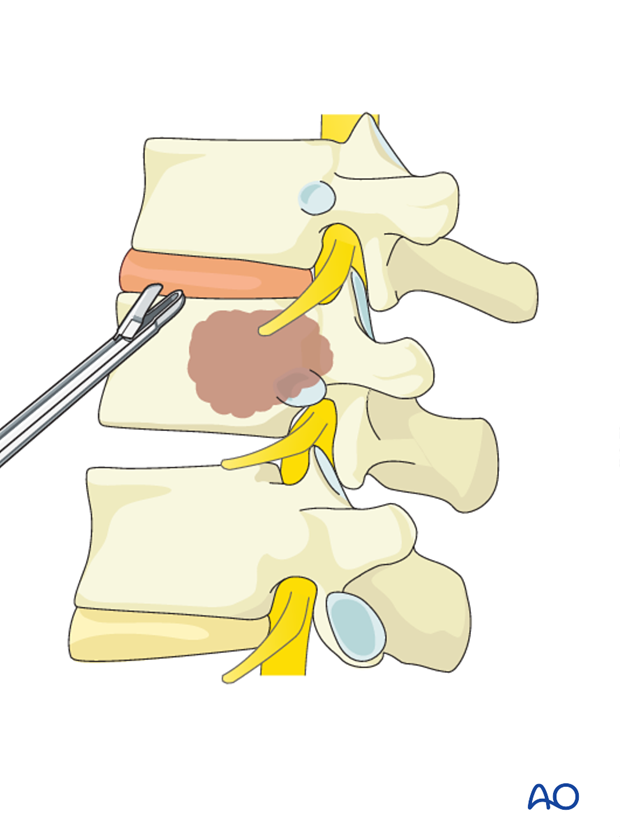
Corpectomy
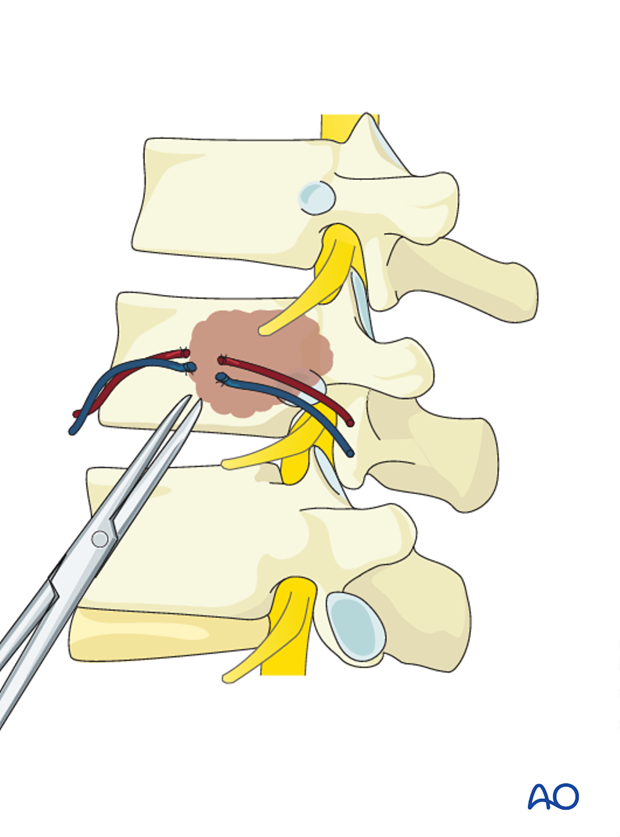
Before performing a corpectomy, the segmental vessels must be identified.
After identifying the segmental vessels, these should be ligated in the mid vertebral body away from the neural foramen.
Note: There is no segmental artery in L5.
After removal of the cranial and caudal discs, the vertebral body (but not the posterior third) is removed using a combination of Leksell rongeurs and osteotomes.
A rim of vertebral body is left anteriorly to facilitate fusion.
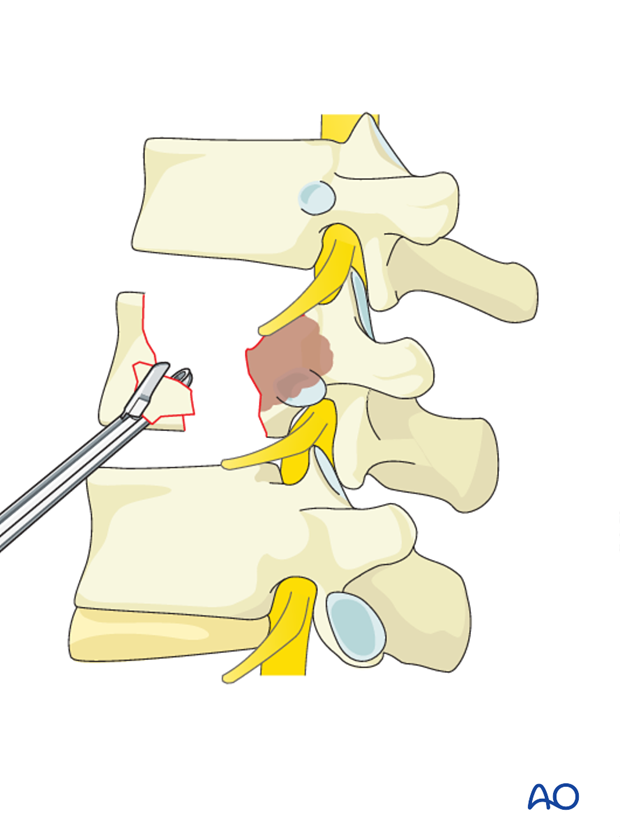
The tumor is removed in a piecemeal fashion working towards the posterior part of the vertebral body.
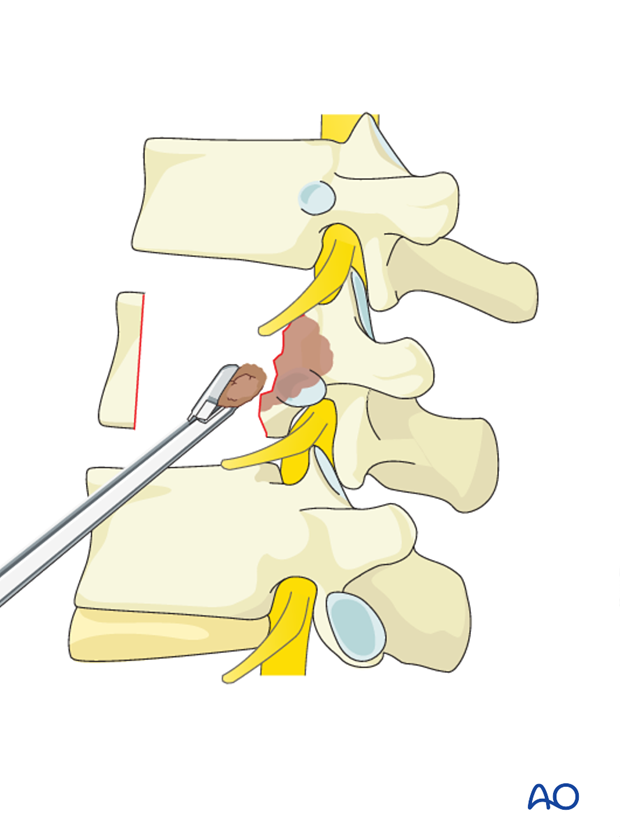
The spinal canal is decompressed by the resection of the posterior wall of the vertebral body.
The posterior cortex should be thinned with the burr to an eggshell. Retropulsed tumor and bone fragments can be removed with curettes and thin footplate Kerrison punches.
This is optimally done under loupe or microscopic magnification.
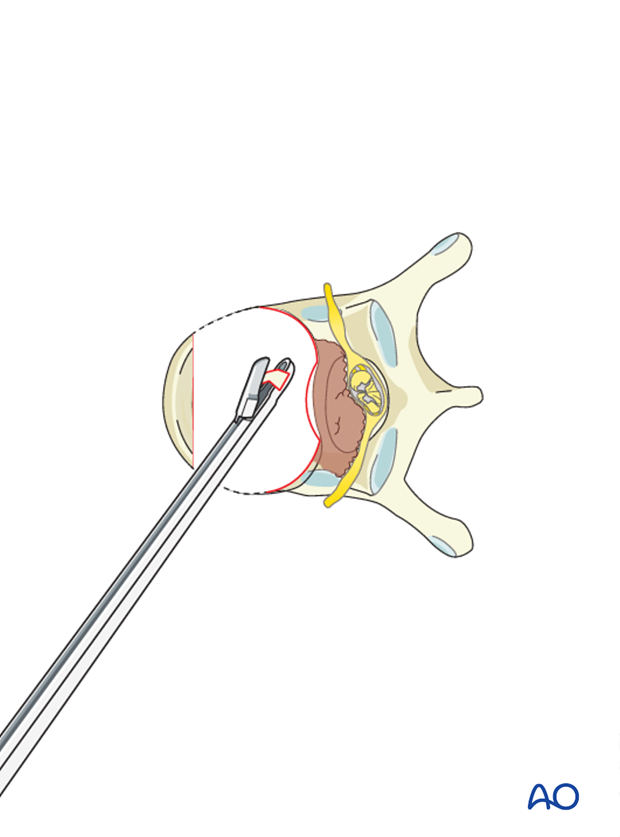
Pearl: Care should be taken to protect the dura. Epidural venous bleeding can be troublesome at times, so meticulous hemostasis with bipolar cautery, cottonoid patties, and hemostatic adjuncts can be helpful.
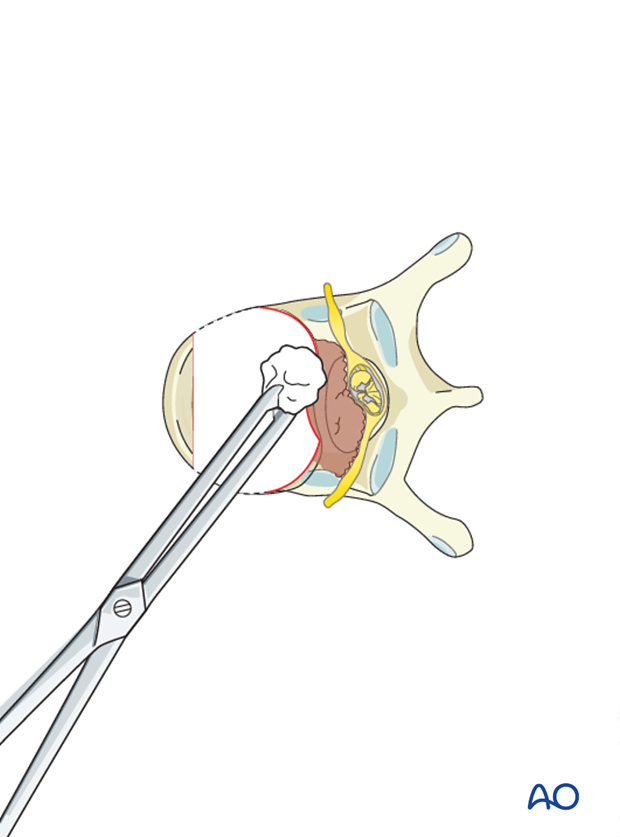
4. Reconstruction
Anterior reconstruction of the disc space or vertebral body following a complete corpectomy can be performed using a prosthesis and/or PMMA.
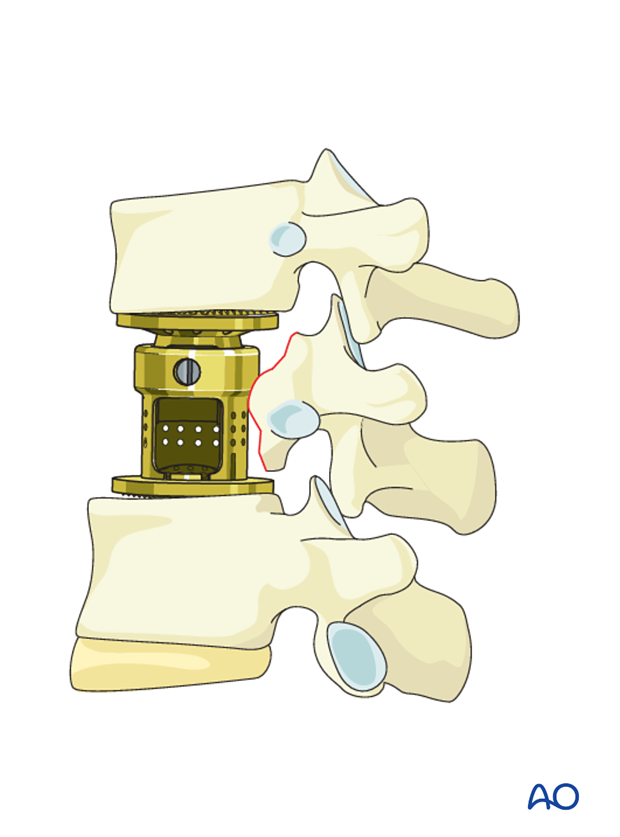
Additional bone grafting can be used from the removed rib, or allograft.
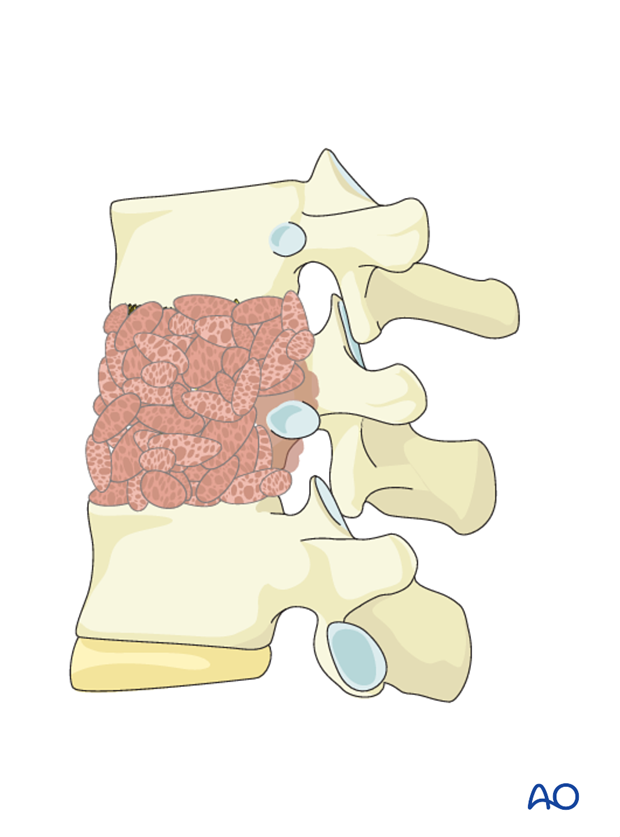
5. Stabilization
Anterior plating
After reconstruction, the construct has to be further stabilized. Various plating systems are available for this purpose eg:
- Screw first systems (typically MIS)
- Plate first systems (typically open systems)
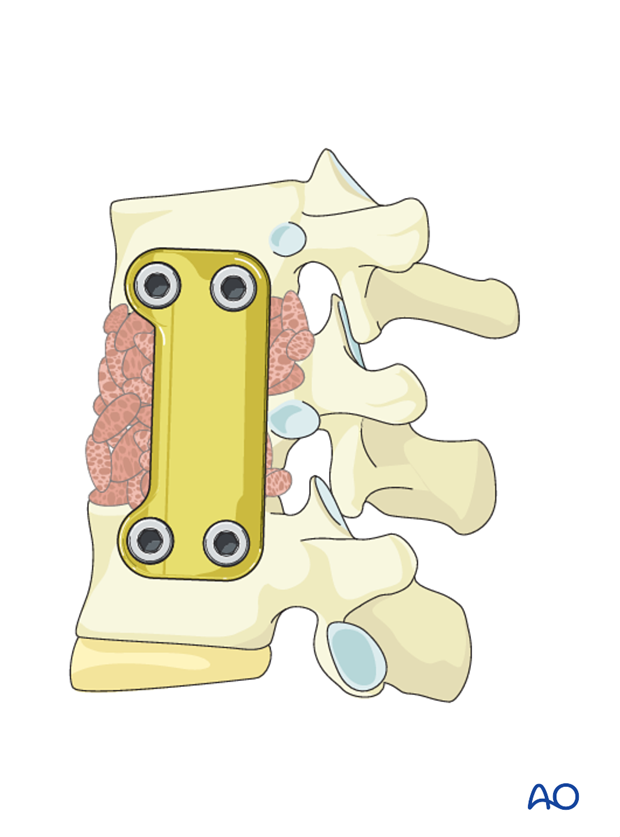
Application of plate instrumentation
A measuring forceps is used to determine the appropriate plate length.

A plating template is applied to the remaining vertebral bodies to ensure the plate fits flush on the bone.
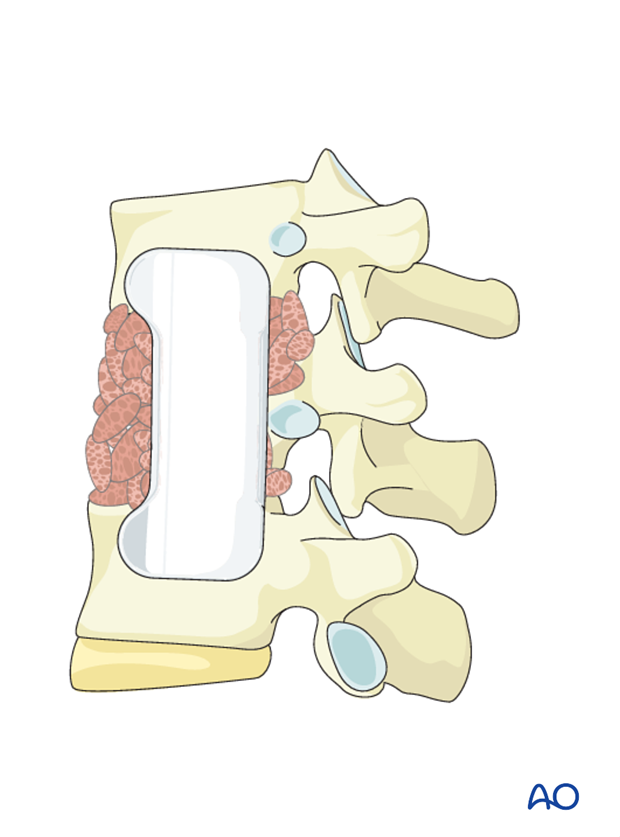
A drill guide is used to drill holes within the vertebral body.
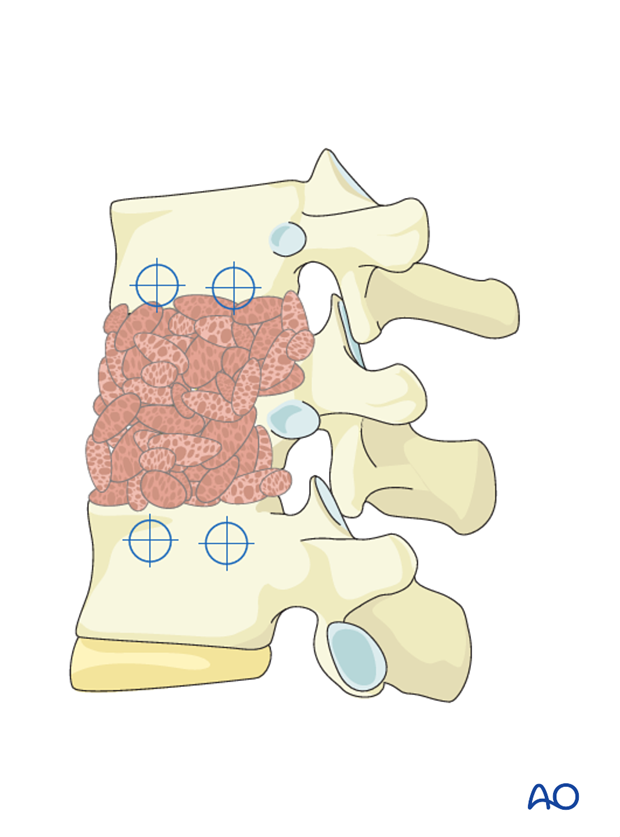
Pearl: Make sure that the screw path is parallel to the vertebral endplates and does not violate the spinal canal.
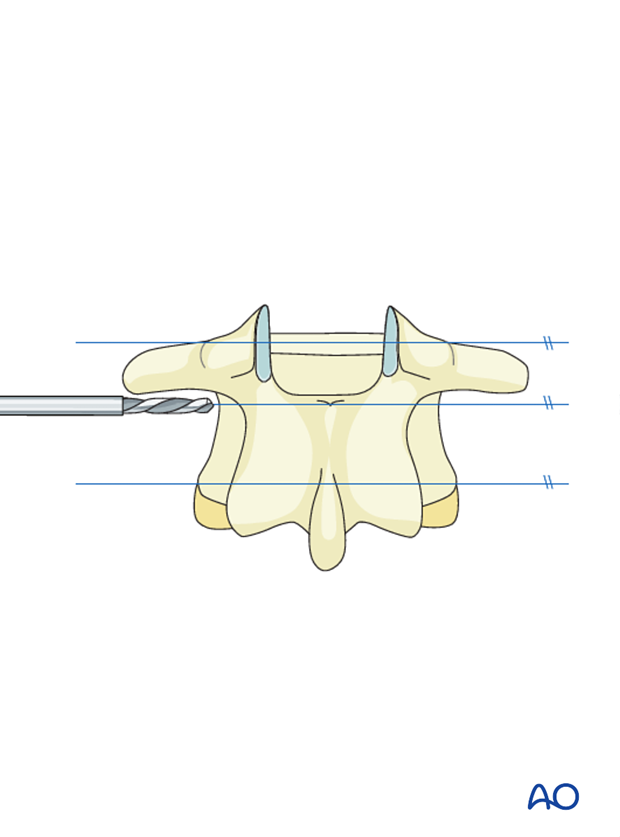
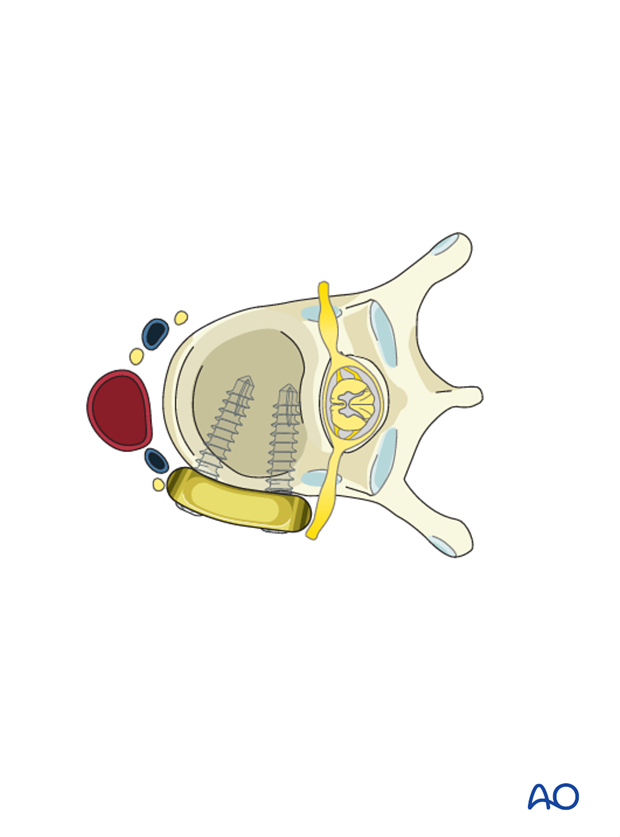
The screws are then inserted affixing the plate to the vertebral bodies. A variety of plating systems allow for distraction or compression.

Pearl: It is important to make sure the plate is as posterior as possible to avoid impingement on any vascular structure.
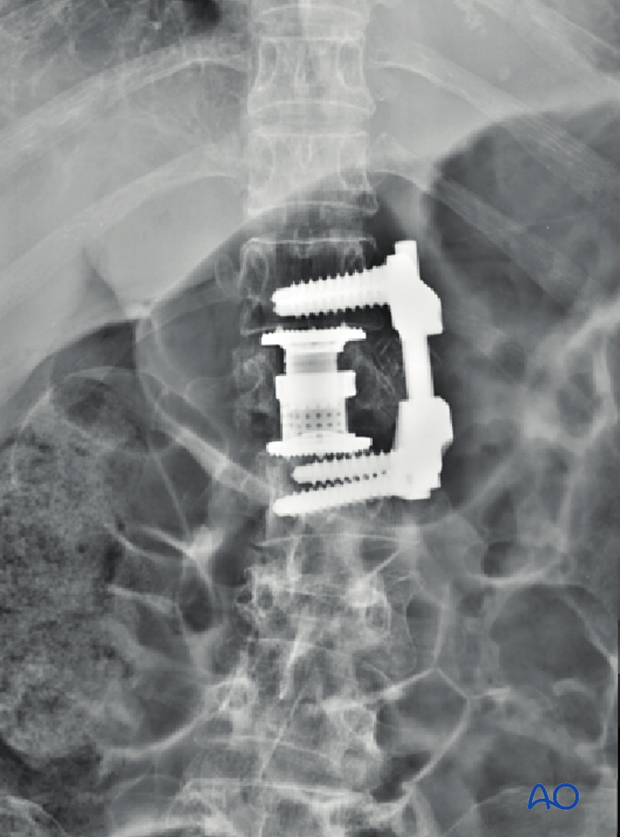
6. Intraoperative imaging
Prior to wound closure, intraoperative imaging is performed to check the adequacy of reduction, position, and length of screws and the overall coronal and sagittal spinal alignment.
7. Aftercare
Patients are made to sit up in the bed on the first day after surgery. Bracing is optional but preferably omitted for patient comfort. Patients with intact neurological status are made to stand and walk on the first day after surgery.
Patients can be discharged when medically stable or sent to a rehabilitation center if further care is necessary.
During admission adequate caloric intake of a high-quality diet should be monitored.
Patients are generally followed with periodical x-rays and (optionally) MR imaging at 6 weeks, 3 months, 6 months, and 1 year to monitor for tumor recurrence and hardware failure.
Postoperative radiation is required to avoid tumor recurrence. SBRT is usually initiated within two weeks following surgery. Conventional radiotherapy is usually initiated 2-4 weeks after surgery to reduce the risk of wound healing disturbances.
The radiation modality is selected based on tumor histology and history of prior radiation.













