Revision of a reverse glenoid baseplate
1. Introduction
Periprosthetic glenoid fractures in cases of reverse glenoid baseplates can occur, either due to shear forces with incorrect component placement or due to long-standing and progressive lateral column scapula notching.
Traumatic periprosthetic glenoid fractures around reverse baseplate components are very rare, and usually occur after a fall.
Preoperative planning
Preoperative planning should include the decision to consider:
- Revision to another reverse or custom replacement
- Conversion to a hemiarthroplasty
- Conversion to an excision arthroplasty
An early sign of glenoid baseplate loosening is progressive notching involving the central peg or peripheral screws of the component. Additionally, notching of the lateral column of the scapula may occur.
The amount of glenoid bone loss is of tremendous importance to the revision strategy.
Modern revision planning software makes it possible to quantify the glenoid defect.
Preoperative CT planning is mandatory when deciding on a strategy of metallic (including augmented designs) or bony reconstruction.
Low-grade infection influences the decision-making process on whether a revision can be a one-stage or a two-stage procedure.
These principles are applicable for stemless, short, and standard stems.
Further details about prosthesis design can be found here.
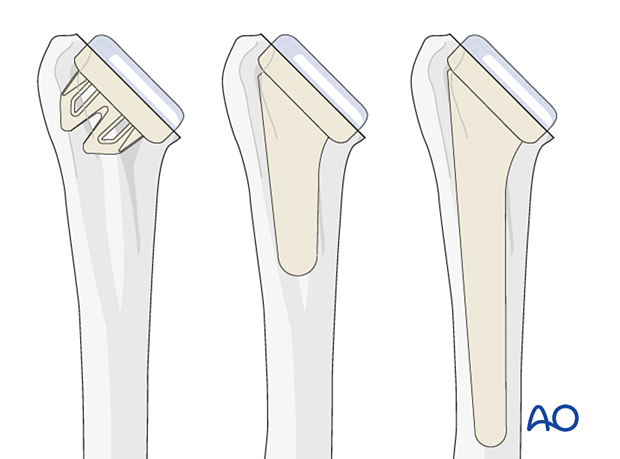
A short stem configuration is shown in this description.
2. Preparation
The standard patient position is the beach chair position with inclination of about 30°. An arm holder may be helpful but is not essential.
Intraoperative fluoroscopy can be helpful.
Patient positioning should be discussed with the anesthetist.

Bone graft
If augmentation or reinforcement of the glenoid fracture or defect is required, bone allograft may be utilized. Structural bulk allograft or morselized allograft are indicated for specific conditions of the glenoid.
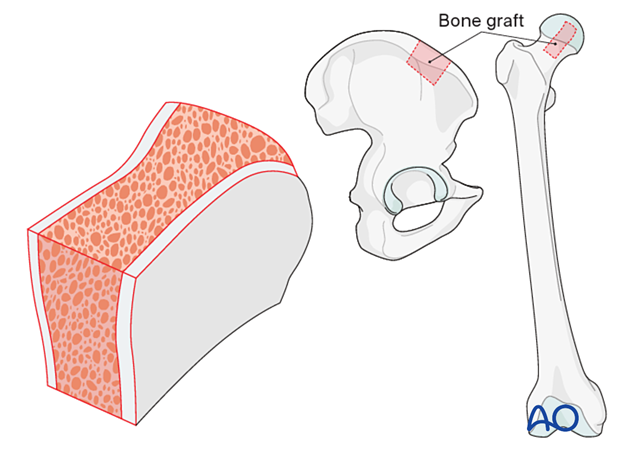
If allograft is not available be prepared to take cortico-cancellous or cancellous graft from the iliac crest (autograft) as shown.
The procedure is done under perioperative antibiotics.
3. Approach
The standard approach used is the deltopectoral approach, which can easily be extended proximally and distally.
Previous incisions should be used if this approach was performed correctly during the primary operation. Do not hesitate to perform a new skin incision if the approach used in the primary was inaccurate.
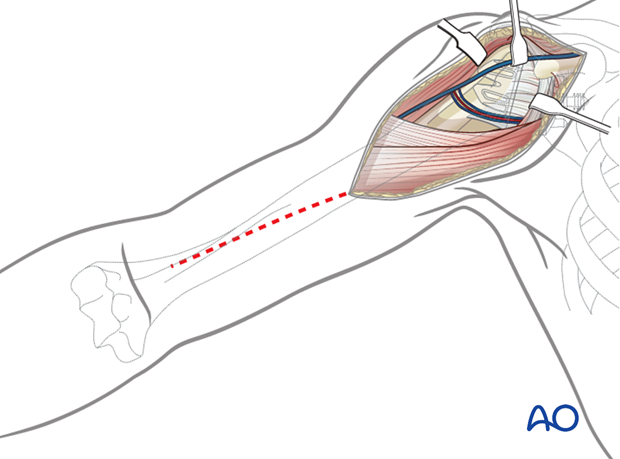
Soft-tissue management
Be prepared for extensive soft-tissue release and a more difficult subscapularis takedown technique before executing the arthrolysis needed to access the glenoid. Take biopsies for cultures.
In advanced chronic cases, metallosis, in the case of a central metal peg, or granulomatous synovial hypertrophy, in the case of a central polyethylene peg, may be present. A subtotal synovectomy is required in advanced stages.
4. Revision to a reverse implant
Revision of a reverse to a reverse component is possible in most cases.
Glenoid exposure and exchange
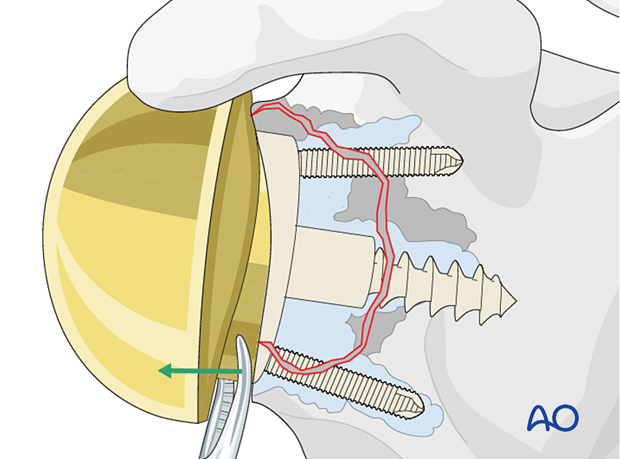
Management of the glenoid bone loss is closely related to the configuration of the remaining glenoid vault.
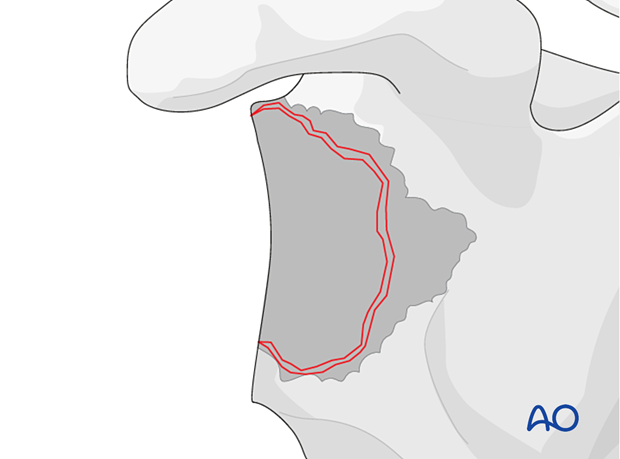
To facilitate stable fixation of a reverse baseplate, it may be necessary to reconstruct the glenoid vault using bone graft.
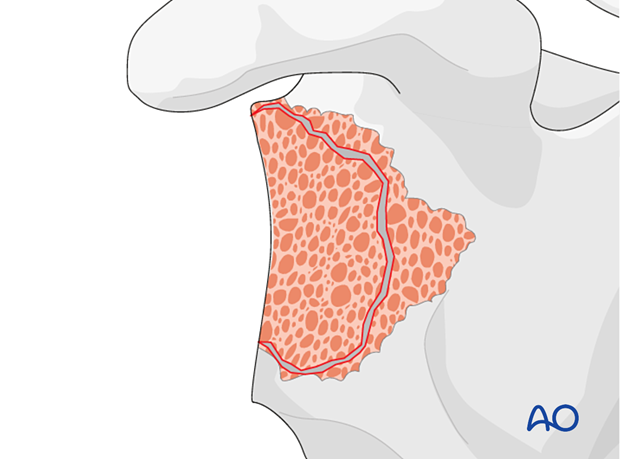
Glenoid reconstruction
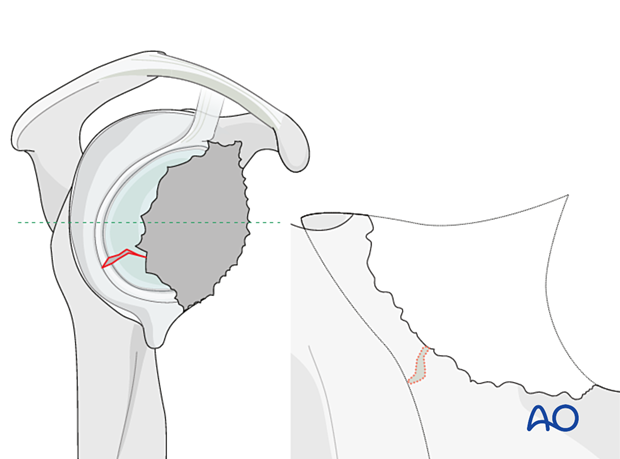
Using bone – contained defectsIn cases of mild glenoid contained defects (Type 1 according to Gohlke) impaction bone grafting is performed and a reverse base plate is implanted.
The illustration on the left is a representative cross section of the glenoid vault shown in the right diagram.
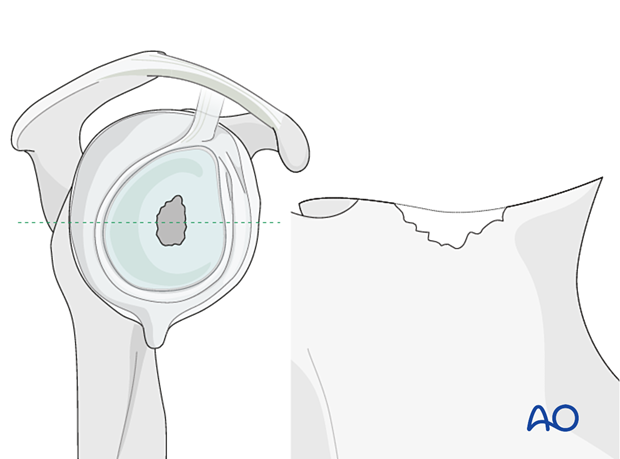
In cases of large, contained defects (Type 2) a structural allograft or autograft is impacted followed by implantation of the base plate.
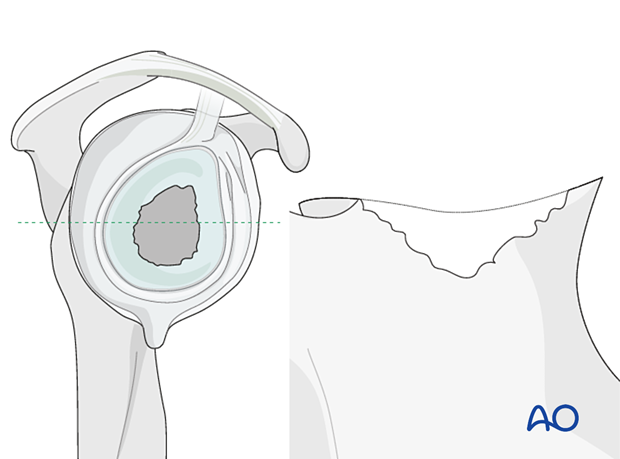
In non-contained defects with either anterior or posterior wall insufficiency (Type 3) a structural allograft or autograft is used and fixed with two or three screws.
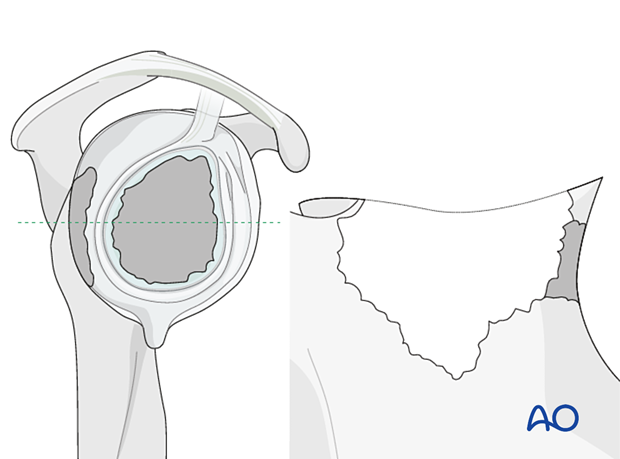
In non-contained defects with severe medialization (Type 4) the same technique is applied.
The decision to perform a one versus two-stage base plate implantation depends on several factors:
- Initial size of the defect
- Primary stability of graft fixation
- Specific implant features
- Surgical experience
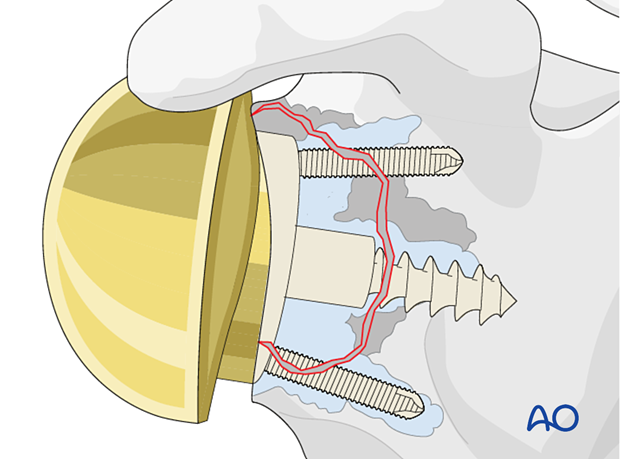
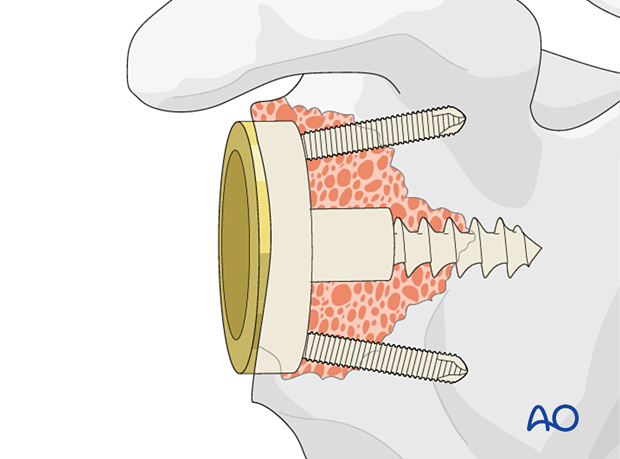
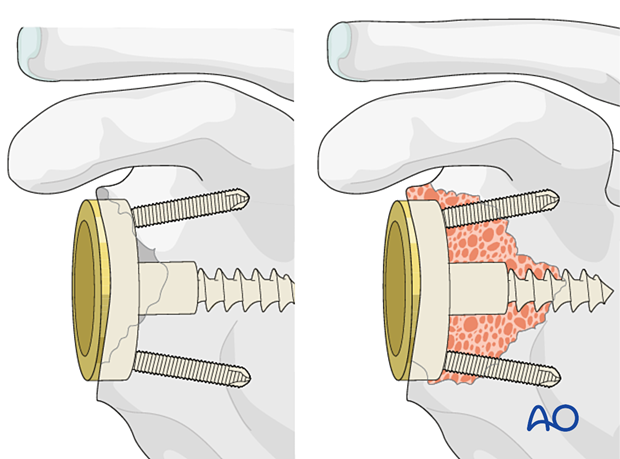
In all cases it is important to gain primary fixation in native bone. A reverse baseplate is shown with a central screw fixed into native bone with peripheral anti-rotation screws.
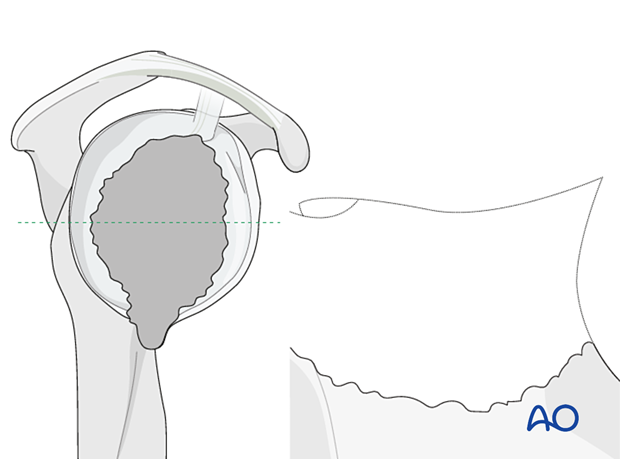
In Type 5 defects with loss of the glenoid vault bony reconstruction should always be performed as a two-stage operation.
Custom implants are often required.
Off-the-shelf augmented base plates may be used in isolation or with bony reconstruction to achieve optimized fixation to the scapula.
Customized implants are not uniformly available and evidence for their role remains to be established.
Advantages include:
- Single-stage procedure
- Personalized to the patient and structural defect
- Optimized function
- Durability
- Time zero structural support
- No risk of graft reabsorption
Disadvantages include
- Lack of availability
- Cost
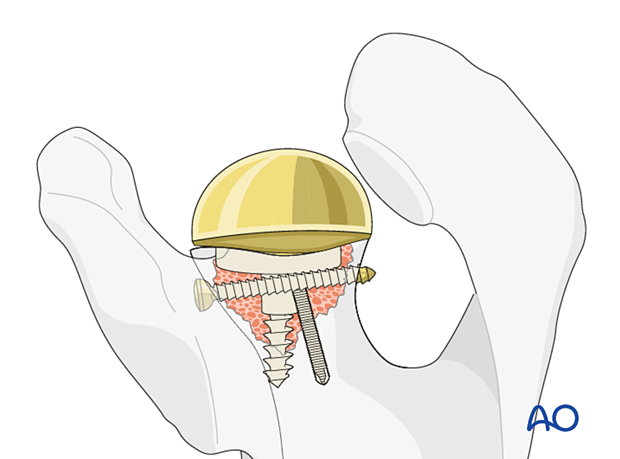
A glenosphere is impacted on the baseplate.
At the end of the procedure a trial component is used to check for stability. Then the final polyethylene liner is implanted, and the shoulder is reduced.
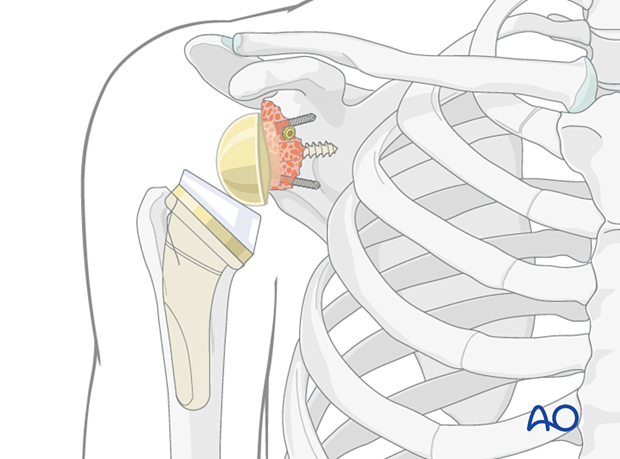
5. Aftercare
Postoperative phases
The aftercare can be divided into four phases of healing:
- Inflammatory phase (week 1–3)
- Early repair phase (week 4–6)
- Late repair and early tissue remodeling phase (week 7–12)
- Remodeling and reintegration phase (week 13 onwards)
Full details on each phase can be found here.













