Complete femoral revision with hinged knee
1. Introduction
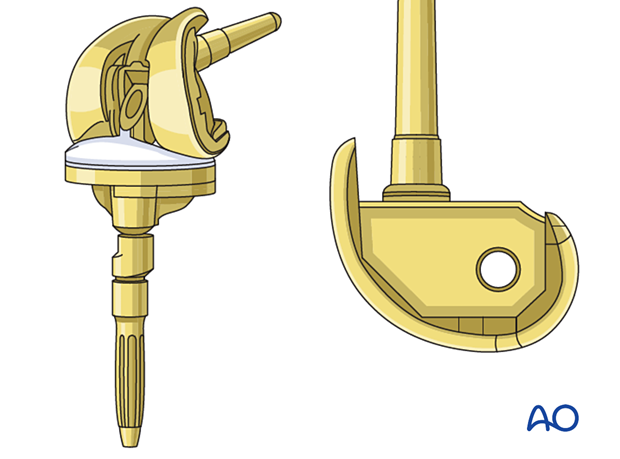
A hinged prosthesis is indicated when there is sufficient metaphyseal bone stock but inadequate ligament support. If the bone stock is either insufficient or of poor quality, the distal femoral replacement prosthesis is used.
The tibial component for the primary arthroplasty is not compatible with the hinged femoral component. It is, therefore, necessary to revise the tibial component.
2. Preoperative planning
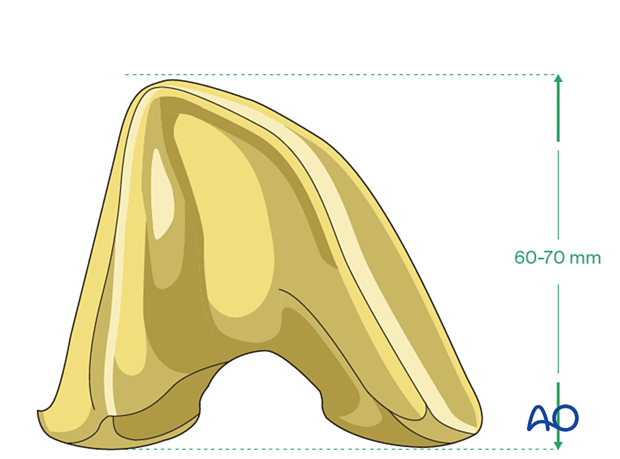
Length of hinged femoral component
The length of the hinged femoral component is most often in the range of 60-70 mm. Careful preoperative planning is performed to determine if such a component is appropriate for the remaining distal femur bone stock.
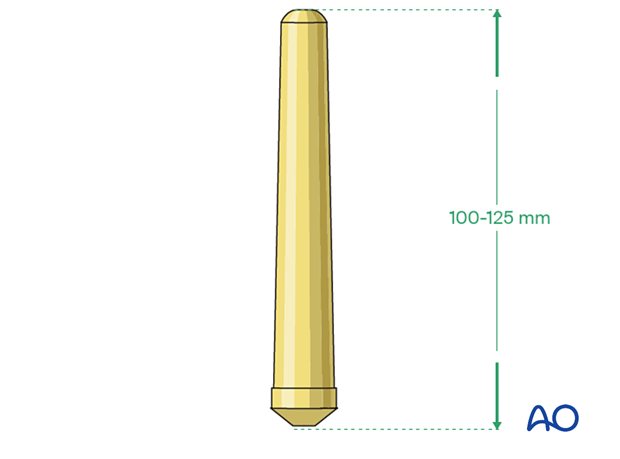
Femoral stem
The length of the stem for the hinged femoral prosthesis is typically 100-125 mm.
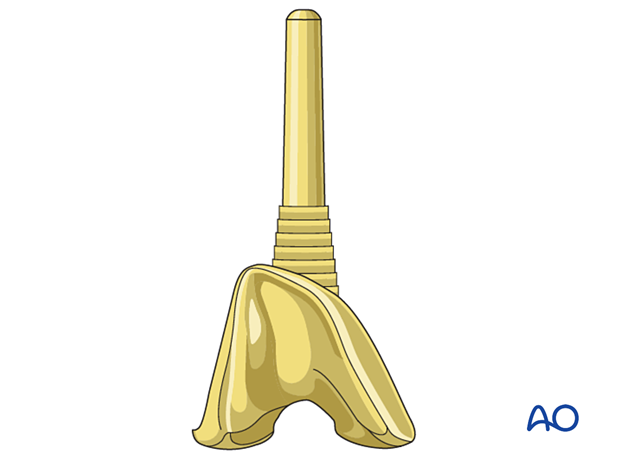
Supplemental metaphyseal fixation
The surgeon may consider using supplemental metaphyseal fixation.
Different surgical techniques are involved with the use of a sleeve or a cone.
3. Patient preparation
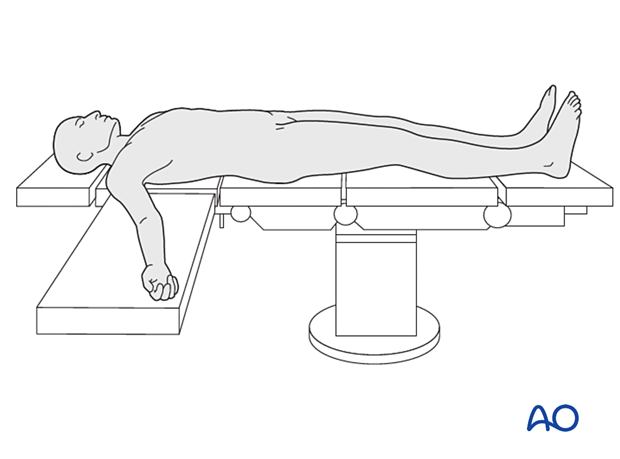
The patient is placed in the supine position. A radiolucent table may facilitate intraoperative fluoroscopy if required.
4. Surgical approach
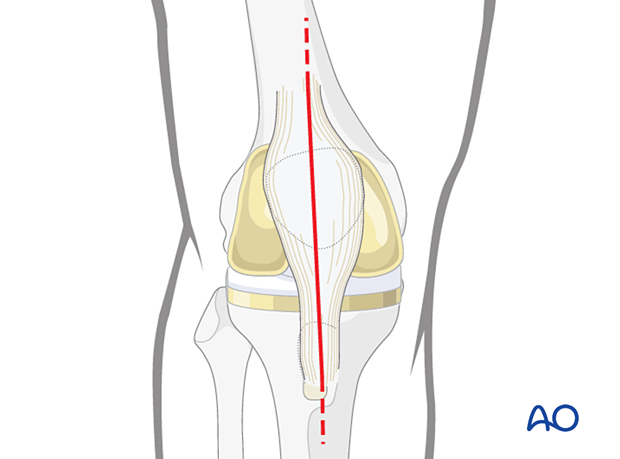
This procedure requires an adequate visualization of the knee joint. The most commonly used is a midline skin incision followed by a medial parapatellar arthrotomy. A proximal and distal extension may be necessary to achieve sufficient visualization and soft tissue releases.
5. Femur
Removal of the femoral component
Dissection is carried out around the fractured distal femur using the electric cautery. The collateral ligaments and the posterior joint capsule are detached from the distal femur if needed. Care must be undertaken to avoid injury to the neurovascular structures, and to the extensor mechanism of the knee.
The femoral component is removed with the distal bony fragment.
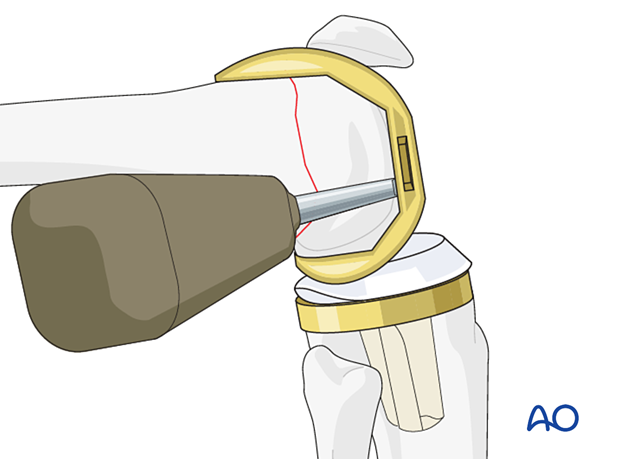
Preparation of the femur
Additional bone cuts may be required specific to the particular prosthetic system selected.
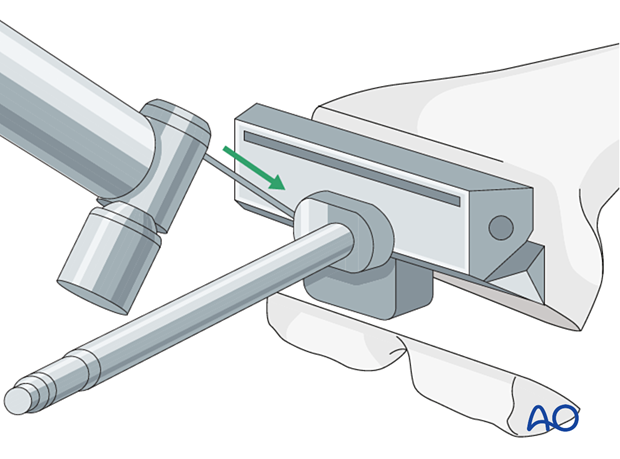
The femoral canal is prepared with reamers of increasing size. The depth of the reaming is determined by the length of the selected stem.
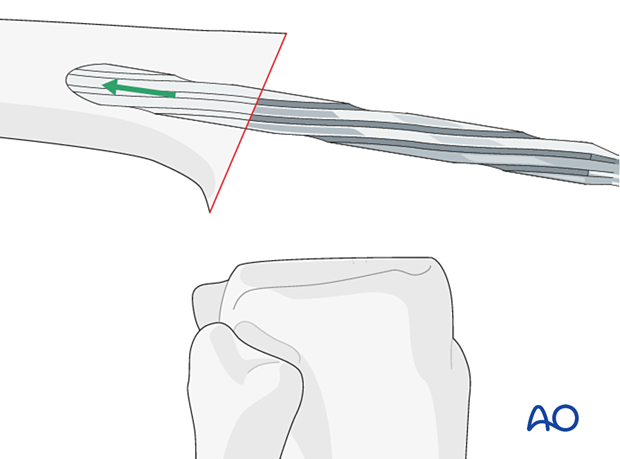
The diameter of the stem is determined by the reamer diameter which achieves cortical contact with the diaphyseal bone. One should allow for at least 2 mm of cement mantle around the stem if cement fixation is used.
If cementless stem fixation is selected, line to line fit of the reamer to the final stem diameter is used.
If a femoral sleeve or a cone is selected, appropriate instruments are used to prepare the distal femur.
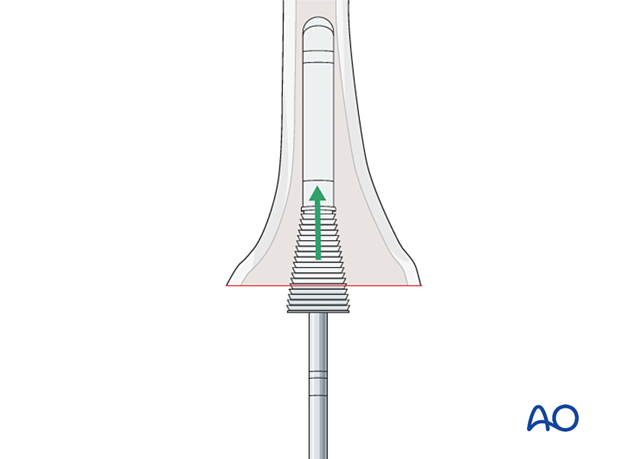
6. Tibia
Tibial revision techniques are described under the treatment: complete tibial revision with hinged knee.
7. Trial
The trial components are assembled, and a trial reduction is performed.
Gap balancing with the proper thickness of the polyethylene insert is performed.
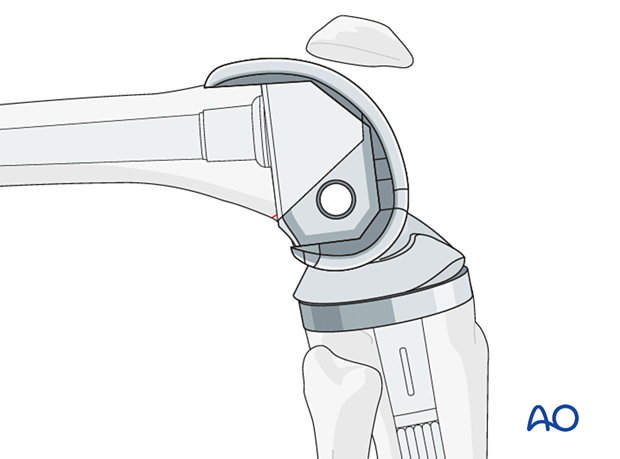
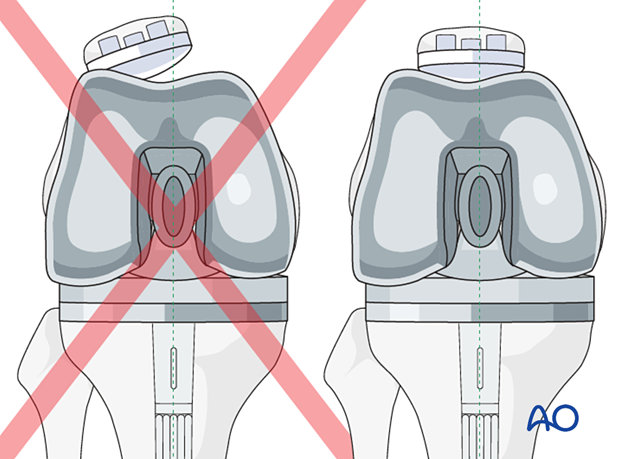
Patella tracking is carefully assessed to ensure no instability or impingement throughout the entire range of knee motion.
8. Components insertion
Bone preparation for cementing
The femoral bone surface and the canal are lavaged to remove any debris. The bone surface and the canal are dried before proceeding.
Cement restrictors
The cement restrictors are inserted into the femoral and tibial canals to allow for a 1 cm cement mantle between the stem tips and the restrictors.
Supplemental femoral metaphyseal fixation
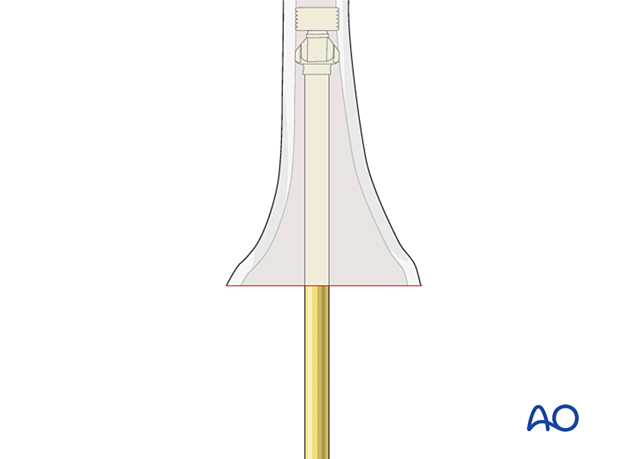
If supplemental metaphyseal fixation of the femoral component is used, different techniques are involved with the use of a sleeve or a cone. If a cone is used, the cone is inserted first, then the stemmed femoral component is cemented into the cone.
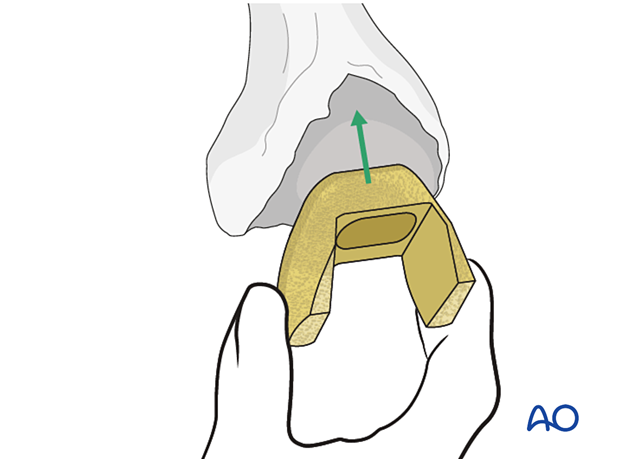
If a sleeve is used, the sleeve and the stemmed femoral component are assembled together first, then the monobloc implant is inserted into the femur.
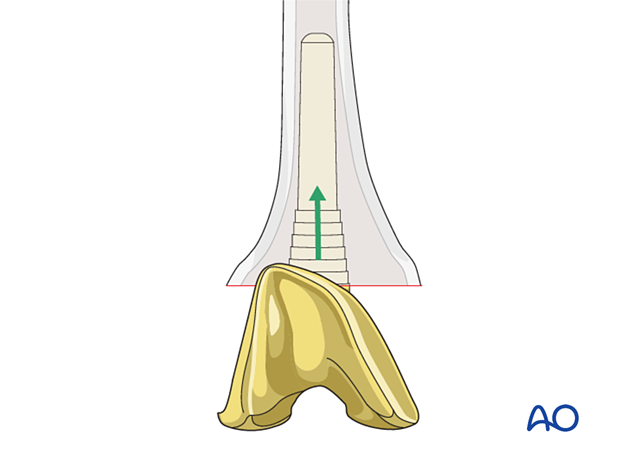
Insertion of the femoral component
The femoral component (including any augment) is seated with 3-5° of external rotation to the mid coronal axis of the femoral shaft to allow for proper patellar tracking. The femoral rotation is also aligned to the tibial component to achieve a symmetrical flexion gap.
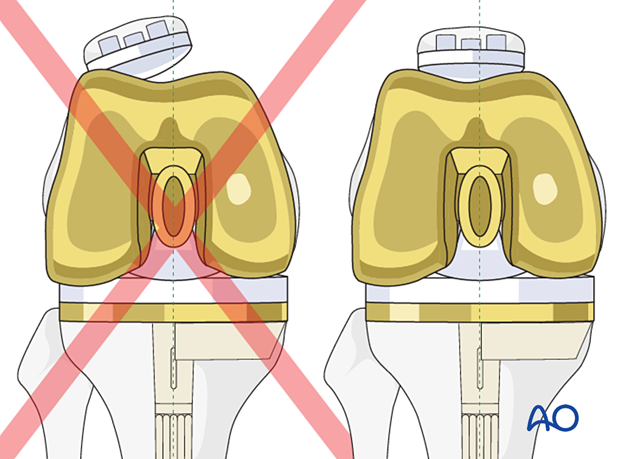
9. Final reduction
The selected polyethylene bearing along with the bushings for the hinged articulation are assembled and coupled together.
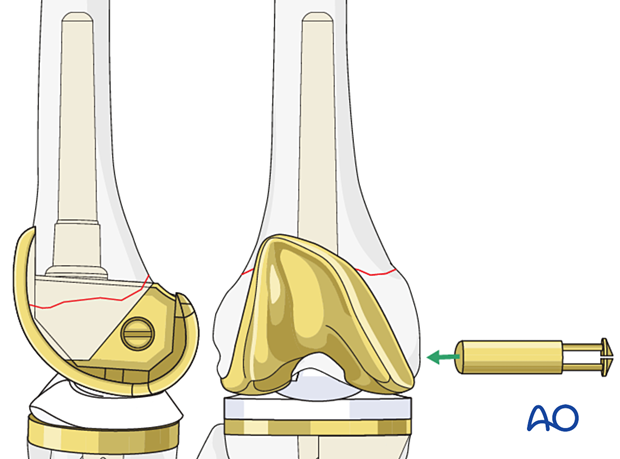
If patellar tracking is not ideal, a lateral retinacular release and medial imbrication can be performed.
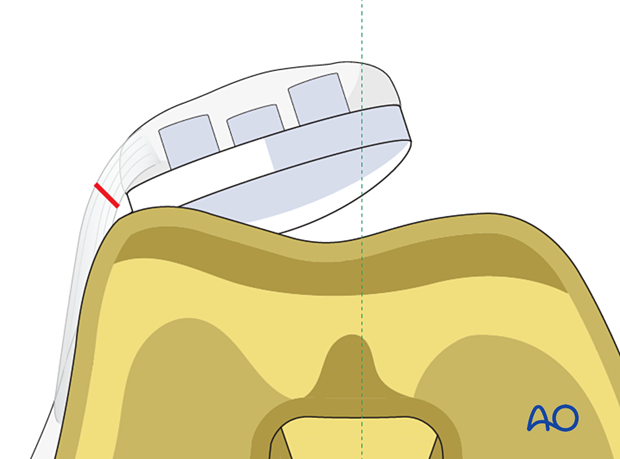
10. Aftercare
The patient can be mobilized with full weight-bearing and active range of motion immediately after surgery.













