ORIF of protrusio fractures
1. Principles
Successful treatment of acetabular fractures is critical to achieve component ingrowth, pain control, and long-term survivorship of the arthroplasty.
Supplemental anterior column buttress plating is indicated when cage fixation is likely to be inadequate in insolation.
For further information about standard techniques for ORIF in native acetabular fractures, please refer to the acetabulum section of the AO Surgery Reference.
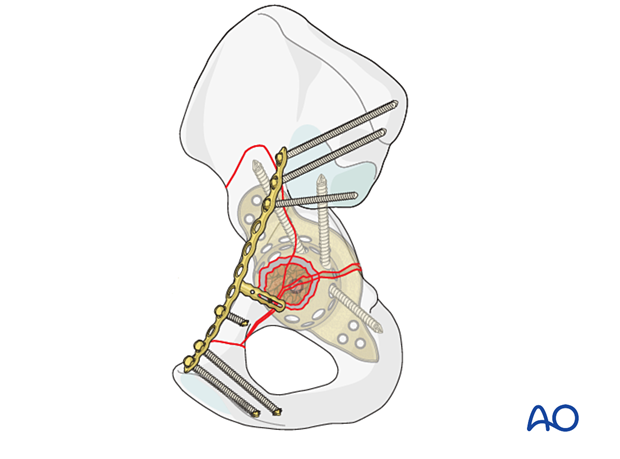
2. Approach
Protrusion through the medial wall of the acetabulum can occur from any approach. Careful attention should be paid to the visualization of any soft tissue at the base of the acetabulum while reaming.
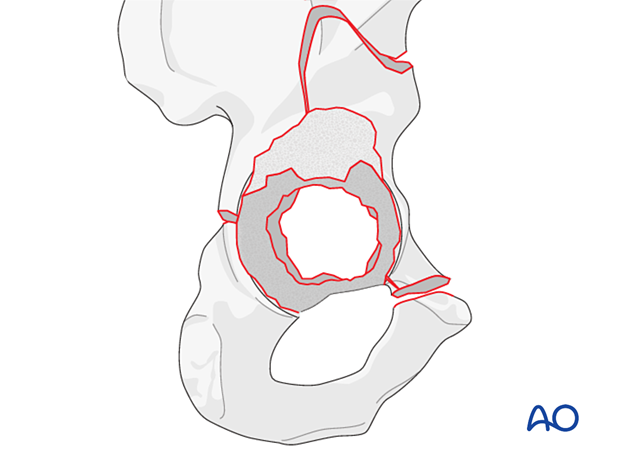
A simple protrusion does not typically lead to an unstable acetabular cup unless there is an underlying deformity of the pelvis. Instability might be present if the protrusion is more complex and involves the columns of the acetabulum (pelvic discontinuity). They are best addressed through an additional anterior intrapelvic approach, with the patient in supine position.
3. Cup removal
In the setting of infection, loosening, or osteolysis, cup removal may lead to acute bone loss and/or the creation of periprosthetic fractures. If this destabilizes the acetabular support of the arthroplasty, fracture specific reduction and fixation techniques are necessary. Depending on the fracture pattern, ORIF with plate and screw and/or column fixation may be indicated.
It is critical to remove the cup without causing additional fractures or bone defects.
Liner removal
The cup liner is removed prior to cup removal.
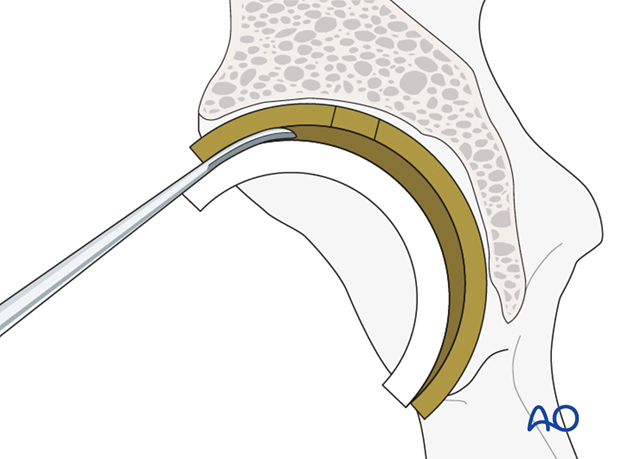
Cup screw removal
Ensure that all the cup screws are removed prior to attempting to remove the cup itself.

Acetabular component removal
The acetabular component is removed. Details on how to remove an acetabular cup are described in the basic technique for acetabular cup removal.
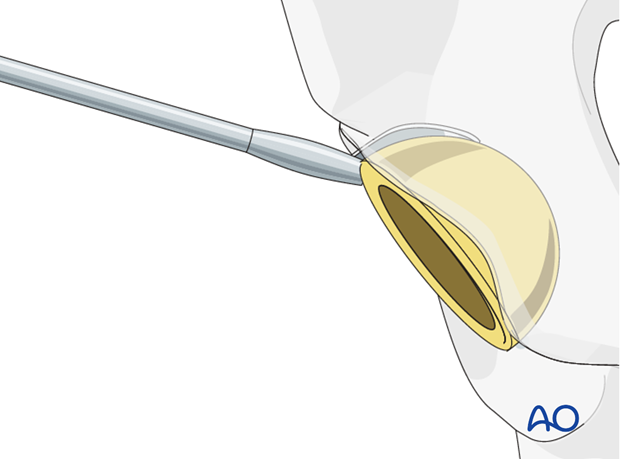
4. Reduction and fixation of protrusio fractures
Fracture reduction
Protrusio and/or central dislocation type fractures should be reduced if the cup does not have adequate support. This requires buttress fixation.
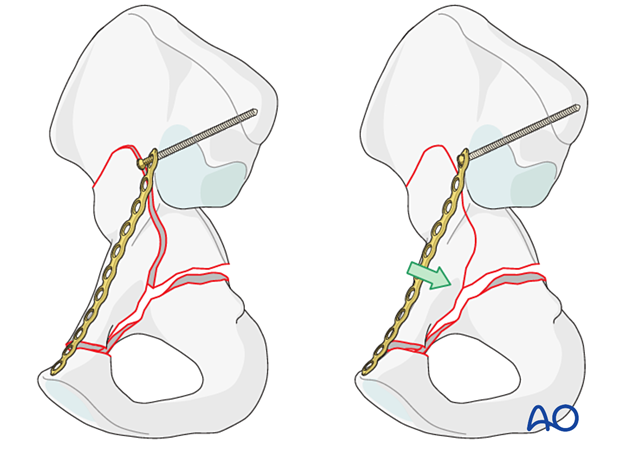
Protrusio preventing intraoperative cup stability
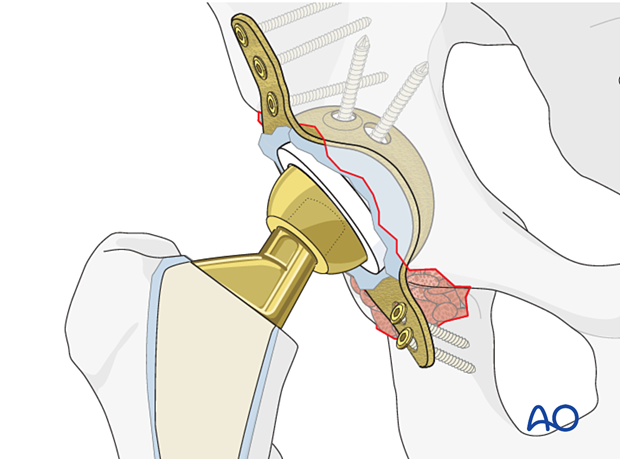
Protrusio or central dislocation type fractures that prevent cup stability intraoperatively are open reduced. Stability is typically achieved with a brim plate applied to buttress the anterior wall or column and if necessary, a quadrilateral buttress plate can be applied.
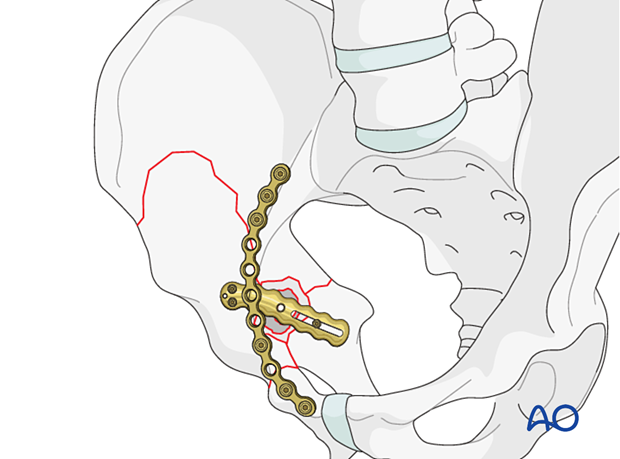
Radiographic confirmation
Reduction and stabilization of the fracture should be confirmed using fluoroscopy.
5. New acetabular cup/cage implantation
Multihole cup
A multi-hole cup is used when there is enough acetabular support.
For further details about the multihole pressfit cup implantation please refer to the treatment: Revision of cup to multihole pressfit cup.
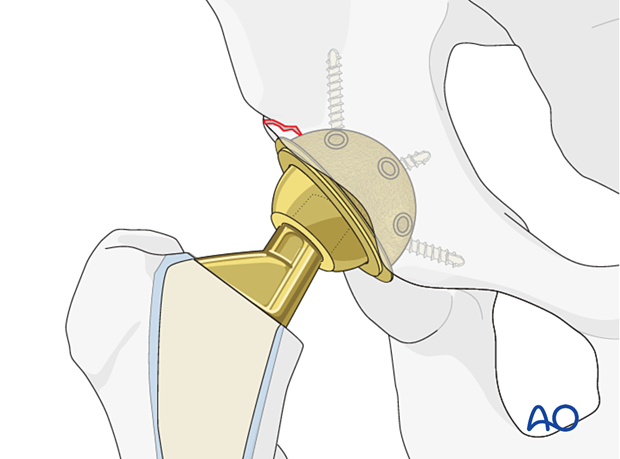
Antiprotrusio cage
If there is any concern regarding acetabular stability, use a cage to support the cup.
Use the antiprotrusio cage in the following situations:
- Restoration of cup containment must be established.
- Restoration of acetabular column stability must be established.
- Minimize fracture progression and comminution.
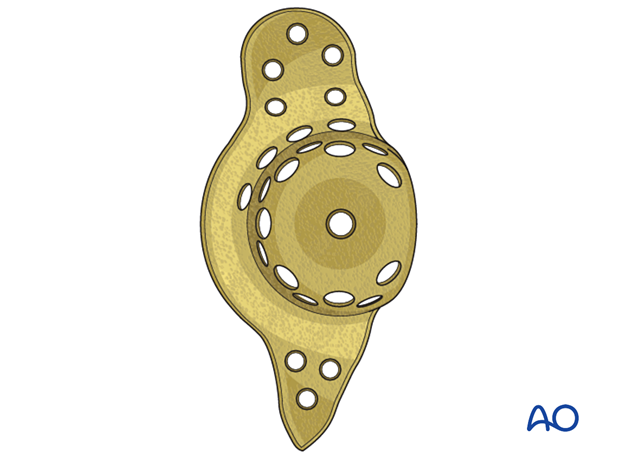
For further details about the antiprotrusio cage implantation please refer to the treatment: Revision of cup to antiprotrusio cage.
6. Aftercare following ORIF
Postoperative management
Postoperative management should include careful monitoring of hematocrit and electrolytes particularly in the elderly patients.
Postoperative IV antibiotics should be administered up to 24 hours.
Consideration should be given to anticoagulation for a minimal course of 35 days. If there are thromboembolic complication this treatment is extended.
Drains can be discontinued when output is less than 30 to 50 cc per 12 hours.
Patient mobilization
Immediate mobilization of the patient should commence. If fracture stability will allow, the patient should be made weight bearing as tolerated as soon as possible. Long periods of limited weight bearing are extremely detrimental to patient recovery.
Precautions against hip dislocation
Hip precautions can be extremely important in patients who have suffered intraoperative acetabular fracture. Much work has been done to minimize the surgical exposure during hip arthroplasty to decrease the risk of dislocation. These advantages are typically removed when acetabular stabilization need to be performed. A dislocation in the postoperative course of such a patient can be disastrous.
Patients are instructed to follow standard hip precautions against dislocation based upon the surgical approaches for hip arthroplasty.
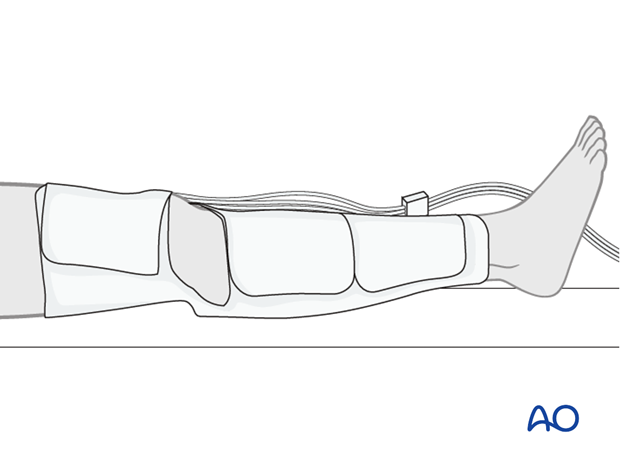
Wound healing
Avoidance of edema postoperatively is critical for both wound healing and patient mobilization. This can be aided by pneumatic compression devices. If negative pressure wound therapy is utilized, it can be discontinued after 5 to 7 days. Staples or sutures are typically removed at 14 to 21 days.