Open reduction, resorbable pin fixation
1. Introduction
Preliminary remarks
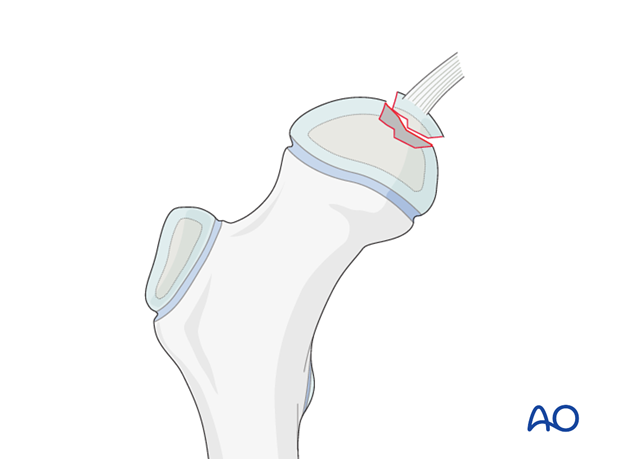
Large osteochondral fragments can be reattached with resorbable pins.
For good fixation, the pins must be inserted in a divergent manner so that the fragment cannot move.
2. Patient preparation and approach
Patient preparation
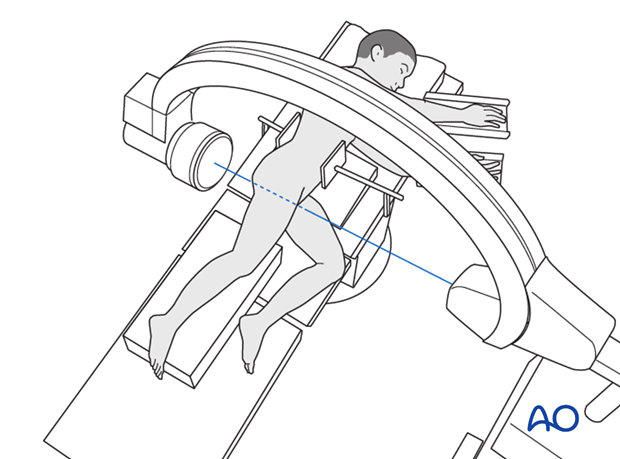
This procedure is normally performed with the patient in a lateral position.
Approach
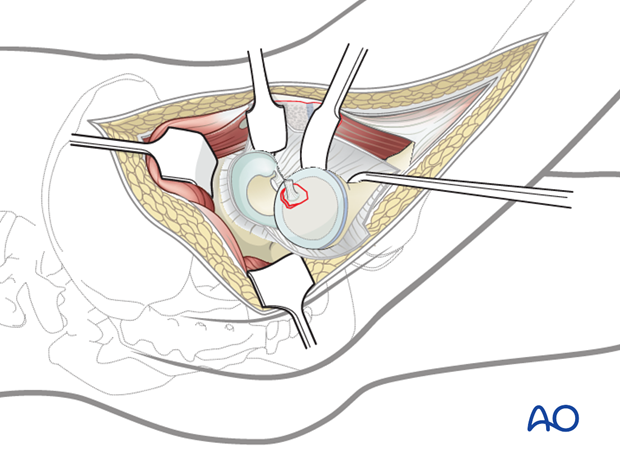
The preferred approach is via a surgical hip dislocation. This approach offers optimal assessment, reduction, and fixation.
3. Reduction
Once the femoral head is dislocated, the fragment is reduced anatomically.
If there is a delay to surgery, swelling of the cartilage of the fragment may be seen. This may need to be trimmed in order to reduce it fully.
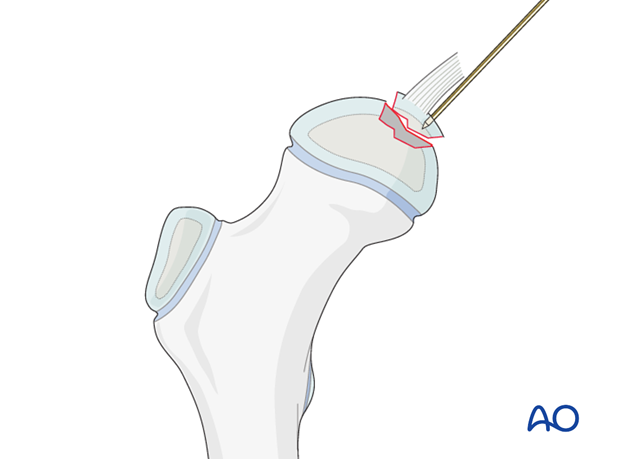
The fragment is held in place with finger pressure and one or two 1.2 or 1.6 mm K-wire(s) are temporarily inserted to hold the reduction.
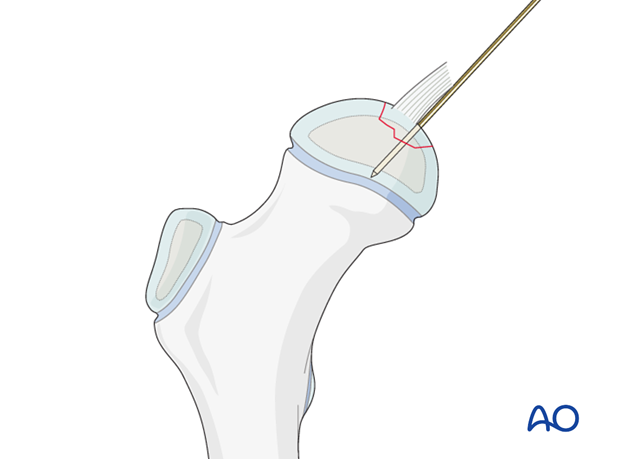
4. Fixation
Pin insertion
When the fragment is perfectly reduced, two, three, or four divergent drill holes (according to the size of the fragment) are made for the resorbable pins.
Completely intraepiphyseal placement is preferred.
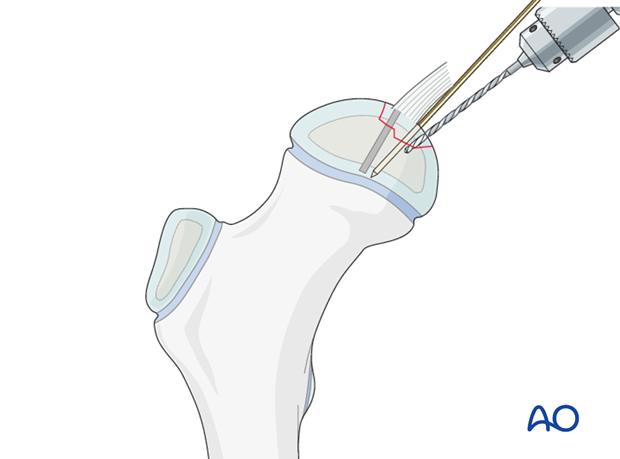
The pins are inserted and cut at the level of the joint surface.
The K-wires are then carefully removed so as to avoid disturbing the pins.
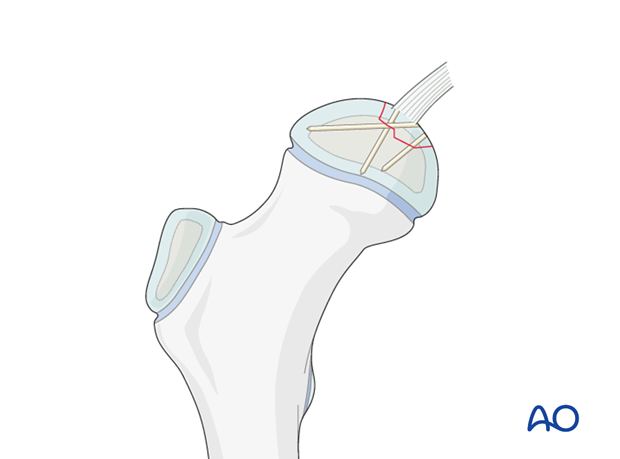
Alternatively, pins with heads are impacted so that the heads are just beneath the surface of the cartilage.
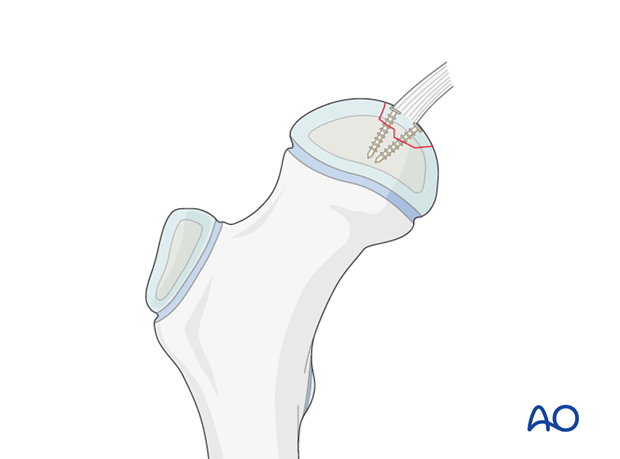
Hip reduction
Once the fixation is completed, the hip is reduced and free movement of the head without moving the fragment is checked.
5. Aftercare
Introduction
After surgical stabilization, the construct should be sufficiently robust to allow protected weight bearing. Smaller children may not be able to comply with this and may need immobilization.

Infection
See the additional material on postoperative infection.
Range of movement
Only controlled range of motion, without forced movements, is permitted for 4-6 weeks postoperatively.
Weight bearing
Full weight bearing is permitted after wound healing.
Sports
Swimming can be allowed as soon as partial weight bearing is permitted.
Contact sports should be avoided for at least six months.
Follow-up x-rays
X-rays are generally taken immediately after the surgery and at 6 and 12 weeks.













