MIO - Bridge plating
1. Principles
Bridge plating
Comminuted diaphyseal fractures are usually treated best with relative stability techniques, such as IM nailing, bridge plating, or, occasionally, external fixation.
Bridge plating uses the plate as an internal, extramedullary splint, fixed to proximal and distal intact fragments. The intermediate fracture zone is left untouched, bypassed by the plate. Anatomical reduction of comminuted wedge fragments is not necessary. Direct exposure injures the soft-tissue attachments, which provide blood supply and aid realignment when length is restored.
When soft-tissue attachments are preserved, fracture healing is predictable.
Correction of length, rotation and axial alignment of the main shaft fragments can usually be achieved indirectly, using traction and soft-tissue tension.
Relative fracture-site stability, provided by the bridging plate, supports indirect healing (callus formation).
Pearl
ORIF of an associated fibula fracture as a first step often indirectly reduces the tibia, restoring length and approximate rotational and axial alignment.

Bridge plate insertion
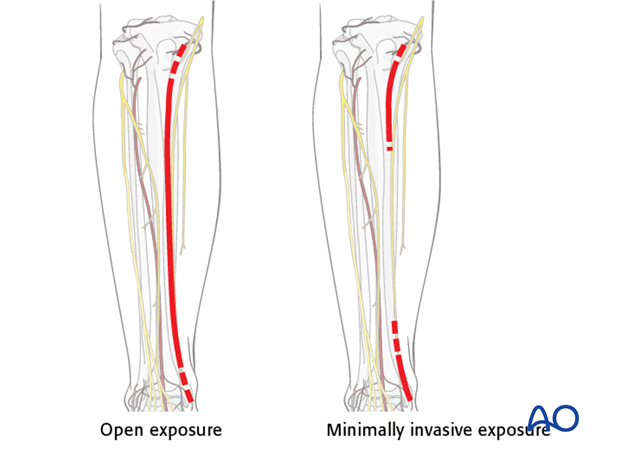
Bridge plates can be inserted either with an open exposure that carefully preserves soft-tissue attachments to the fracture fragments, or with a minimally invasive approach that leaves skin and soft tissue intact over the fracture site.
With the minimally invasive (MIPO) approach, incisions are made proximally and distally, and the plate is inserted through an extraperiosteal tunnel. This should be done using image intensification (if available).
2. Patient preparation and approaches
Patient preparation
This procedure is normally performed with the patient in a supine position.
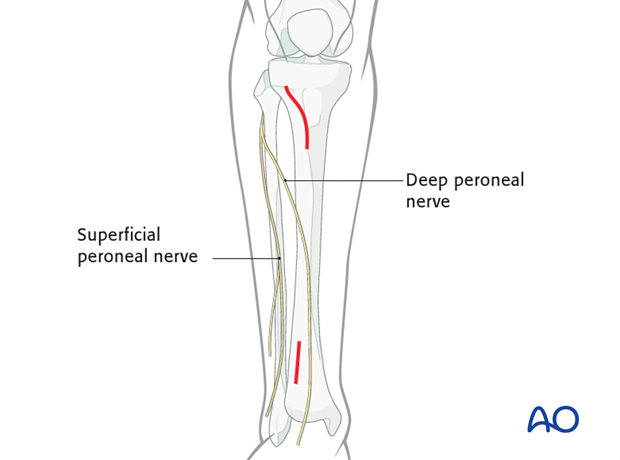
Lateral approach (MIO)
The lateral approach is used for minimally invasive osteosynthesis if the medial soft tissues are injured.
This approach is also used when a precontoured plate (eg, LISS plate) is placed laterally, for fixation of proximal and mid-tibial fractures.
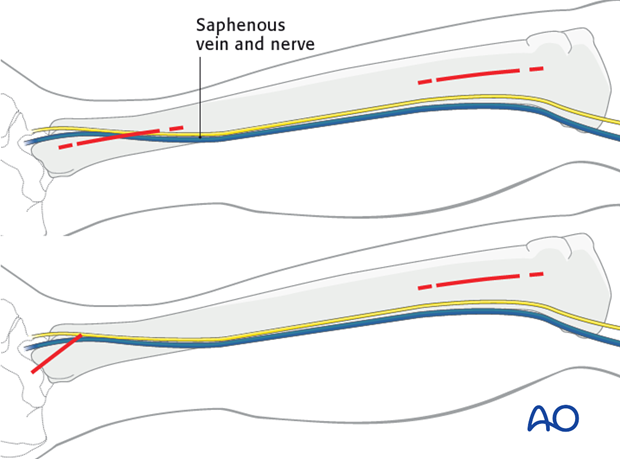
Medial approach (MIO)
Minimally invasive fixation of tibial fractures is preferably done through the medial approach, especially for distal fractures.
3. Reduction
Manual traction
It is important to restore length, axial alignment and rotation.
Apply longitudinal traction to the foot until the cortices of the two main fragments are in contact, thus restoring length.
When length is restored, correct the axial and rotational alignment.
Compare length, alignment and rotation with the uninjured side.
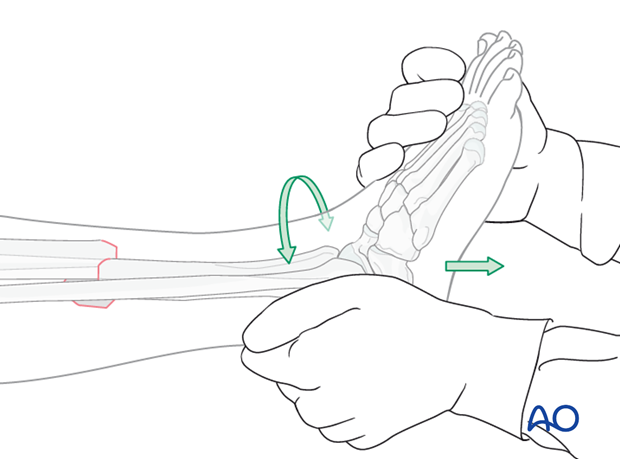
Reduction aids
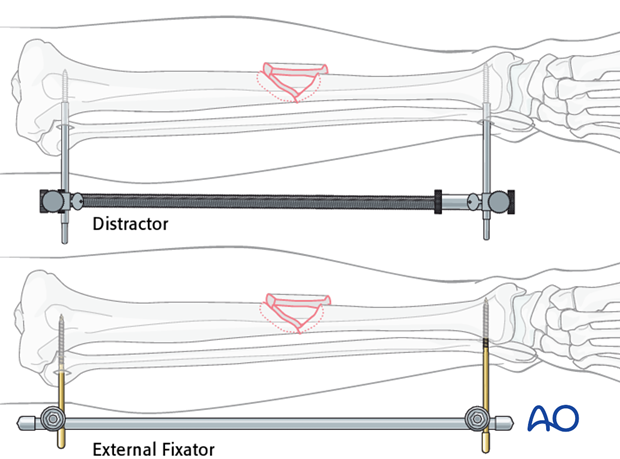
If reduction cannot be achieved by manual traction, use a large distractor. Place a Schanz pin in both the proximal and distal main fragments. Distraction is applied across these pins by turning the distractor knob.
If a distractor is not available, an external fixator can be used instead.
Rotational alignment is aided by inserting the Schanz pins in the same plane. Reduction must be confirmed before proceeding.
4. Plate selection and preparation
Choice of implant
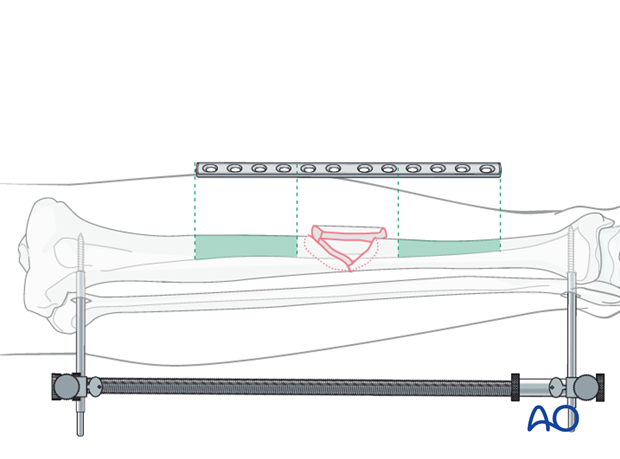
Bridge plating should span a long section of the bone. A good rule of thumb is that the plate should be at least three times as long as the fracture zone. Thus, the proximal and distal thirds of the plate are anchored to the intact bone segments.
Usually a narrow large fragment plate (4.5 mm) is chosen.
An angular stable (locking) plate is a good option in osteoporotic bone, and also for fractures with a short end segment. An angular stable plate need not be contoured precisely to fit the bone, since it functions as an internal fixator. The locking screws do not pull the main bone fragments to the plate. Thus, alignment remains unchanged when the screws are tightened.
Contouring the plate
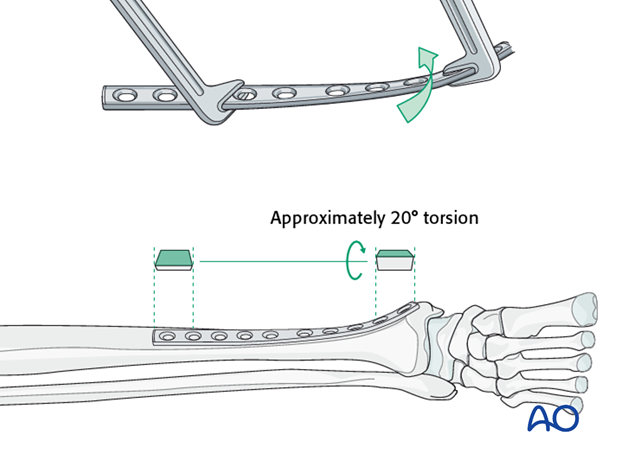
Minimal contouring will be necessary over the fracture site. However, it may be helpful to contour the ends to fit the bone where the plate will be affixed.
To match the orientation of the anteromedial surface of the distal tibia, the distal end of the plate will need to be twisted.
Pearl: plate positioning
If the fracture extends proximally, generally a locking plate is placed laterally because the implant allows us to deal with more proximally located fractures, and may avoid damaged medial soft tissues.
In distal fractures, the preference is to place the plate medially. Anterior and lateral soft tissues (tendon, nerve and blood vessels) make safe placement of the plate laterally difficult.
5. Definitive fixation
Plate insertion - MIPO technique
If minimally invasive plate osteosynthesis (MIPO) is chosen, the plate can be inserted either through the proximal or distal incision.
The tunnel for the plate should be prepared first, either with a specialized tunneling tool, with blunt instruments (e.g. Cobb elevator), or provisionally with the plate, using a handle.

Insertion of first screw
Fixation begins at the extremes of the plate, either proximally, or distally. First position one end of the plate in the middle (anterior to posterior) of the exposed bone surface.
Drill with a 3.2 mm drill bit and drill guide through the plate hole. Measure for screw length, tap with a 4.5 mm tap and a protective sleeve and insert the first screw, but do not completely tighten it.
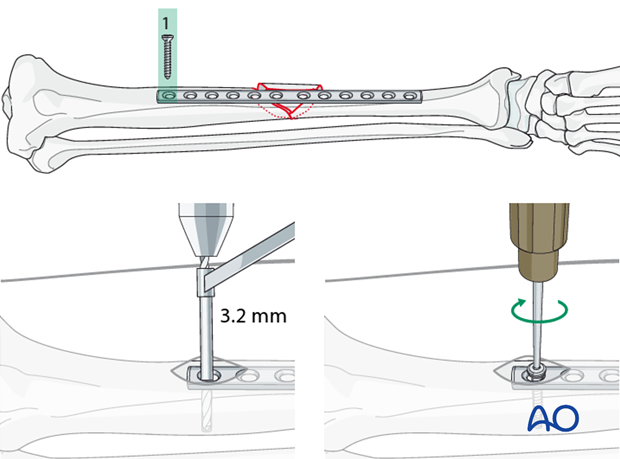
Insertion of the second screw
At this point, length, rotation and coronal alignment should be checked and, if necessary, corrected.
Again, position the plate centrally on the exposed bone surface. Then insert the distal screw similarly to the first.
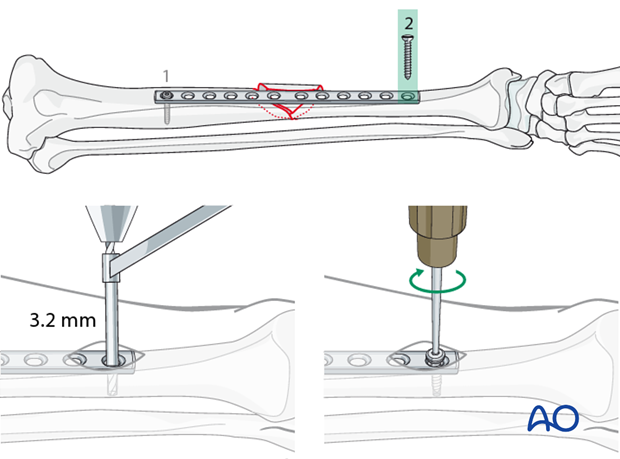
Correcting sagittal displacement
Some sagittal displacement (anterior or posterior angulation) can be corrected after the second screw has been inserted by placing a rolled towel as a fulcrum under the fracture site.
If image intensification is available, check the completed reduction before inserting further screws.

Insertion of the remaining screws
Alternating from one main fragment to the other, insert the remaining screws.
For these screws, additional small incisions over the plate are necessary.
A minimum of three screws on each side should be used.
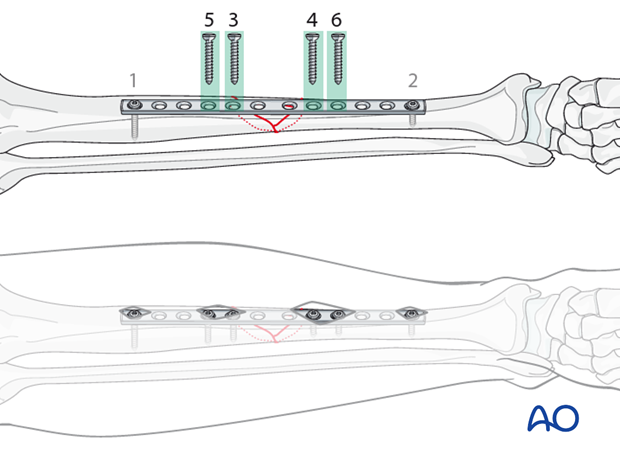
6. Pearl: screws in locking plates
If a locking plate is used, placing the locking screws adjacent to the bridged zone should be avoided.
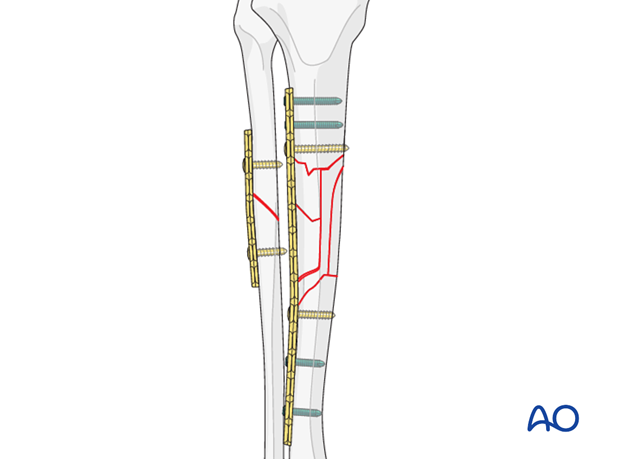
7. Postoperative care
Perioperative antibiotics may be discontinued before 24-48 hours.
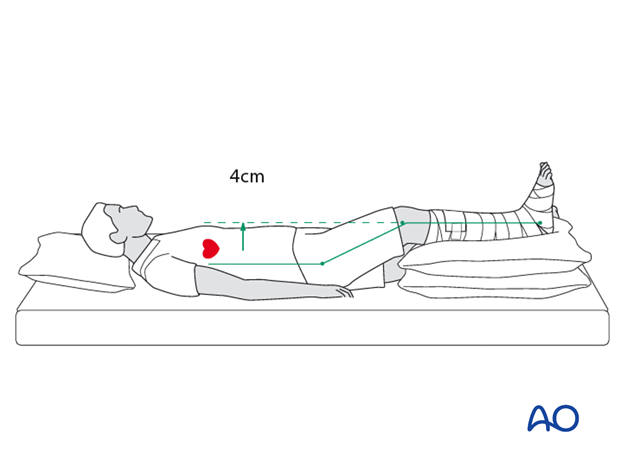
After surgery, the patient’s leg should be slightly elevated, with the leg placed on a pillow, 4 cm above the level of the heart.
Attention is given to:
- Pain control
- Mobilization without early weight bearing
- Leg elevation when not walking
- Thromboembolic prophylaxis
- Early recognition of complications
Soft-tissue protection
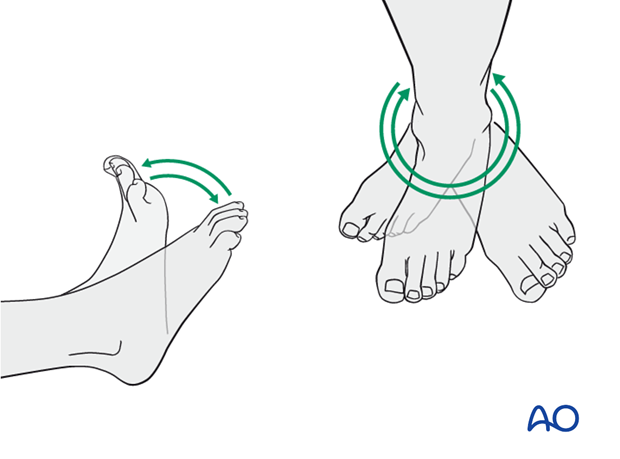
A brief period of splintage may be beneficial for protection of the soft tissues, but should last no longer than 1–2 weeks. Thereafter, mobilization of the ankle and subtalar joints should be encouraged.
Mobilization
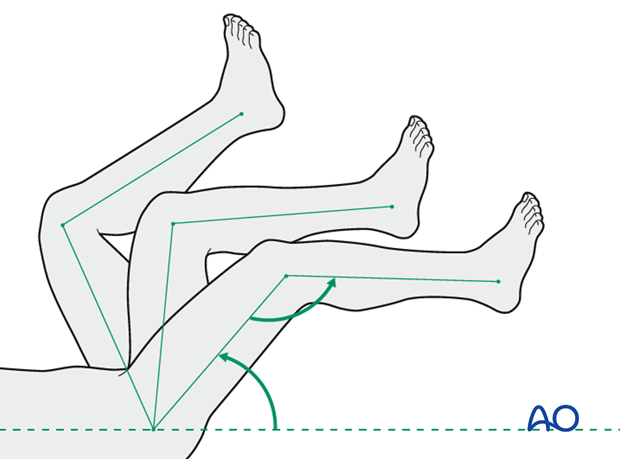
Active and assisted motion of all joints (hip, knee, ankle, toes) may begin as soon as the patient is comfortable. Attempt to preserve passive dorsiflexion range of motion.
Weight bearing
Limited weight-bearing (15 kg maximum), with crutches, may begin as tolerated, but full weight bearing should be avoided until fracture healing is more advanced (10-12 weeks).
Follow up
Follow-up is recommended after 2, 6 and 12 weeks, and every 6-12 weeks thereafter until radiographic healing and function are established. Depending on the consolidation, weight bearing can be increased after 6-8 weeks with full weight bearing when the fracture has healed by x-ray.
Implant removal
Implant removal may be necessary in cases of soft-tissue irritation by the implants. The best time for implant removal is after complete bone remodeling, usually at least 24 months after surgery. This is to reduce the risk of refracture.