Minimally invasive lateral approach to the tibia
1. Indications
The lateral approach is used for minimally invasive osteosynthesis if the medial soft tissues are injured.
This approach is also used when a precontoured plate (e.g. LISS plate) is placed laterally, for fixation of proximal and mid-tibial fractures.
Distally, the shape of the tibia and the overlying soft tissues make it difficult to contour a plate and place screws.
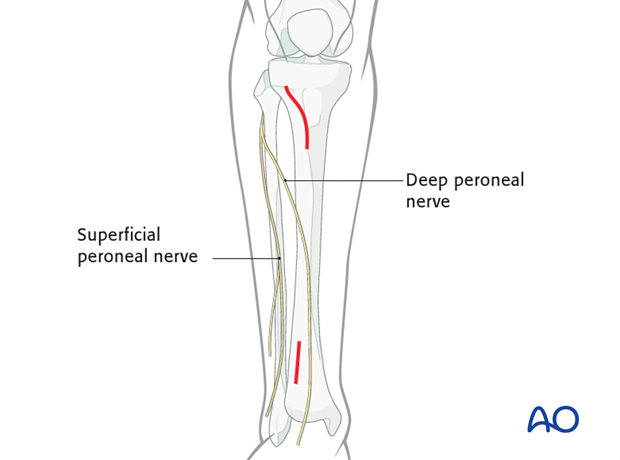
Over the distal third of the tibia (for plates longer than approximately 25 cm), a short incision is advisable in this region to expose and retract the deep peroneal nerve and anterior tibial vessels, to avoid their being trapped by a submuscular plate, or injured by percutaneous screws.
2. Anatomy
Triangular shape of the tibia
The lateral and posterior surfaces of the tibia are covered by muscle. The anteromedial surface has only a thin layer of subcutaneous tissue and skin. This surface provides less blood supply to the underlying bone.
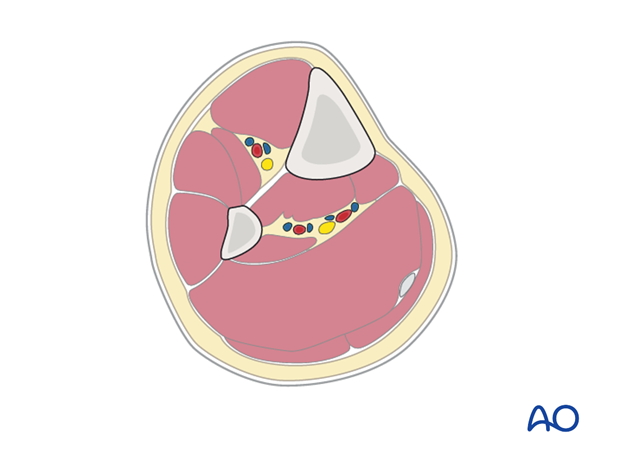
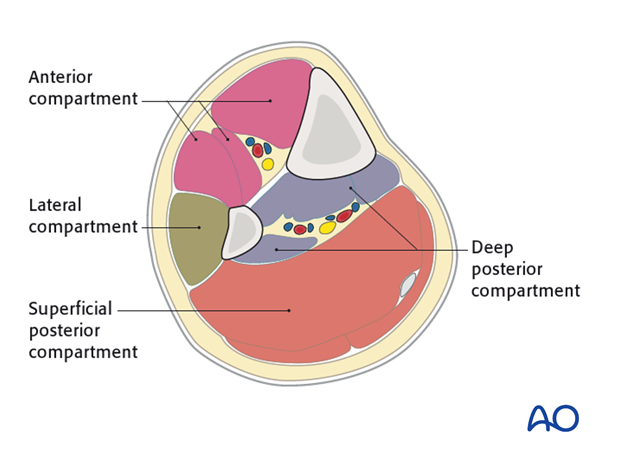
The lower leg has four compartments:
- Anterior
- Lateral
- Deep posterior
- Superficial posterior
The anterior compartment has three muscles and one main artery and nerve: Tibialis anterior, extensor hallucis longus, extensor digitorum longus; the anterior tibial artery and deep peroneal nerve.
The lateral compartment has two muscles and one nerve. The muscles are the peroneus longus and brevis and the superficial peroneal nerve.
The deep posterior compartment has three muscles and two arteries and one nerve: The muscles are the tibialis posterior, the flexor hallucis longus and the flexor digitorum longus. It also has the peroneal artery and the posterior tibial artery as well as the tibial nerve.
The superficial posterior compartment has just two muscles in it: The gastrocnemis and soleus muscles and the sural nerve.
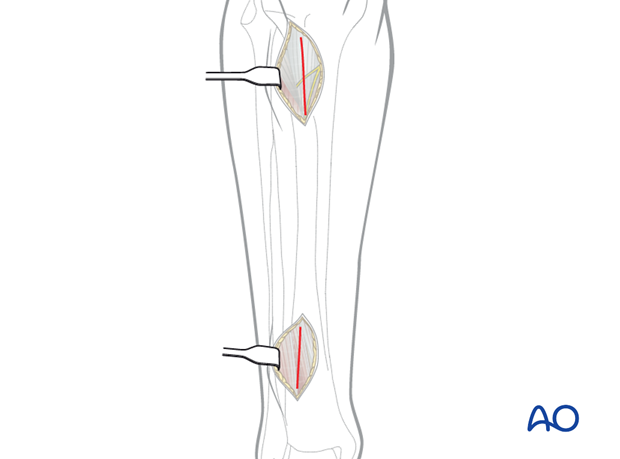
3. Skin incisions
The proximal incision, approximately 5 cm long, begins distal to the tibial tubercle and 1.5 – 2 cm lateral to the tibial crest. The proximal portion should curve slightly posteriorly.
The distal incision is made to prevent neurovascular injury from percutaneous screws. The anterior tibial vessels and deep peroneal nerve cross the anterolateral surface of the tibia approximately at the junction of its third and fourth quarter.

4. Deep dissection
Incise the fascia a few millimeters lateral to the tibial crest.
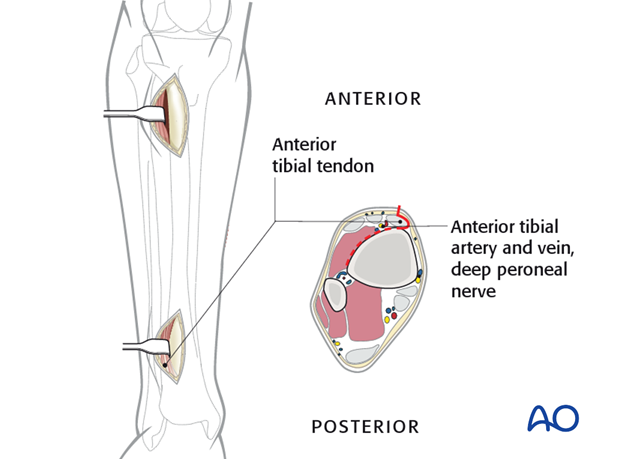
At the distal incision dissect the tibialis anterior tendon from the bone, preserving the paratenon.
Retract the tendon together with the deep peroneal nerve and the anterior tibial vessels to the lateral side.
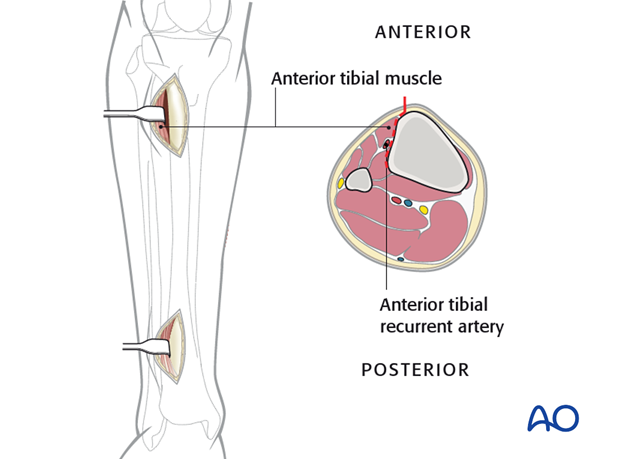
At the proximal incision, dissect the tibialis anterior muscle from the bone without stripping the periosteum.
Retract the tibialis anterior muscle laterally.
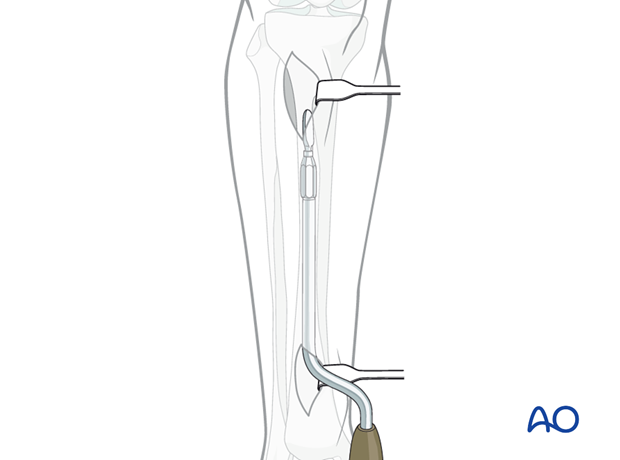
Use a soft-tissue elevator, a tunneler, as shown, or a plate, to prepare a tunnel between the anterior tibial muscle and the periosteum.
Protect the anterior tibial vessels and deep peroneal nerve distally. Depending on how distal the plate is placed, they should be gently retracted laterally, or lifted anteromedially, so the tunnel can be placed under the neurovascular bundle, with direct observation.