ORIF - Lag screws outside protection plate
1. Principles
For the treatment of simple oblique fractures in the diaphyseal area, an absolute stability plate construct can be considered.
For this, direct anatomical reduction and interfragmentary compression are necessary.
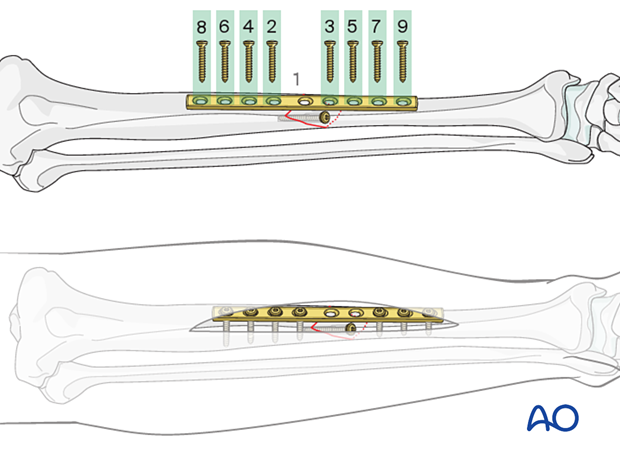
Choosing the method of interfragmentary compression
The method of interfragmentary compression is determined by the fracture geometry and the plane of the obliquity.
In example one, shown here, the apex of the fracture is in the center of the anteromedial or anterolateral surface of the tibia.
In this case, the fracture can be compressed with a compression plate with a supplementary lag screw through the plate.
The apex of the fracture should be underneath the plate.
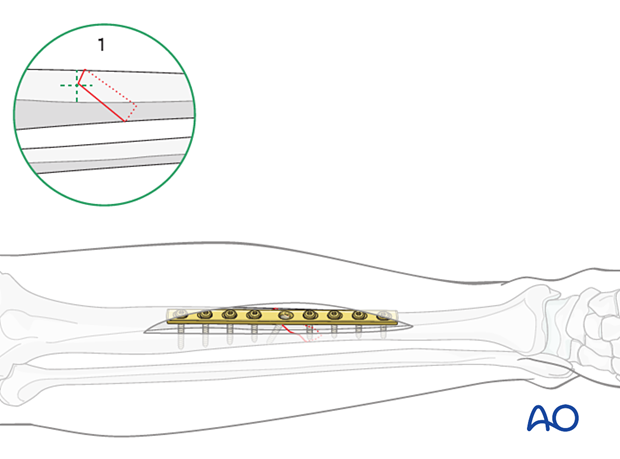
In example two, shown here, the apex of the fracture is not in the center of the anteromedial or anterolateral surface but is either posterior or anterior.
In this case, compression must be done with a lag screw, inserted either inside or outside the plate. In this case, the plate is used in protection rather than compression mode. The apex of the fracture is not underneath the plate but is either anterior or posterior to it.
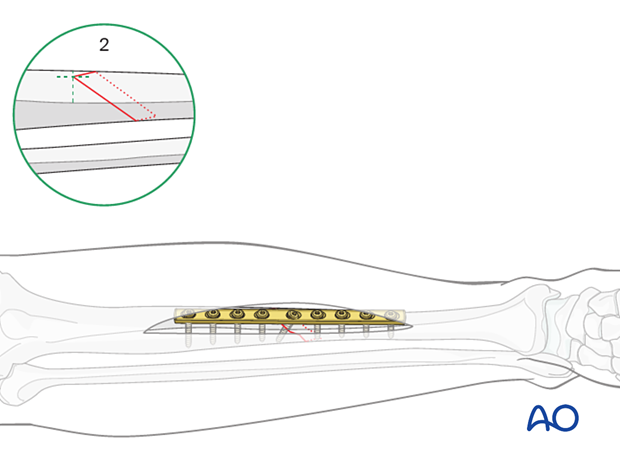
In example three, shown here, the apex of the fracture lies on the tibial crest.
In this case, a lag screw outside of the plate (applied in protection mode) is usually required.
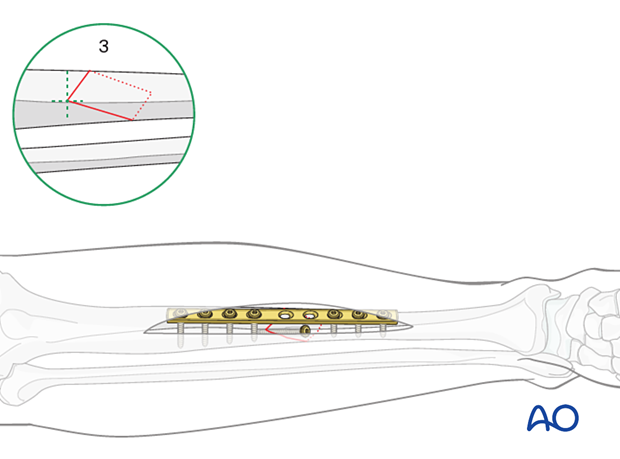
2. Patient preparation and approaches
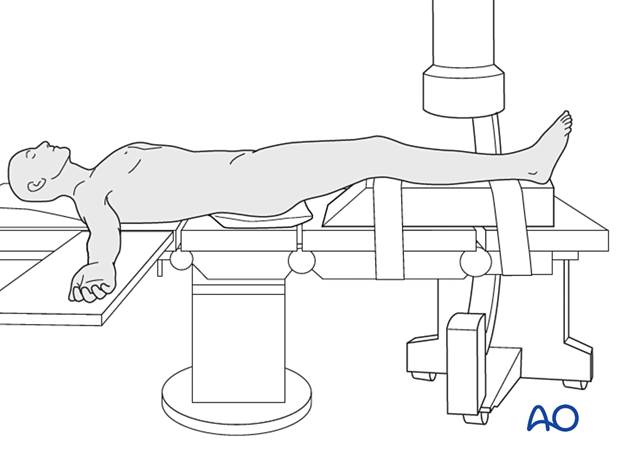
Patient preparation
This procedure is normally performed with the patient placed in a supine position.
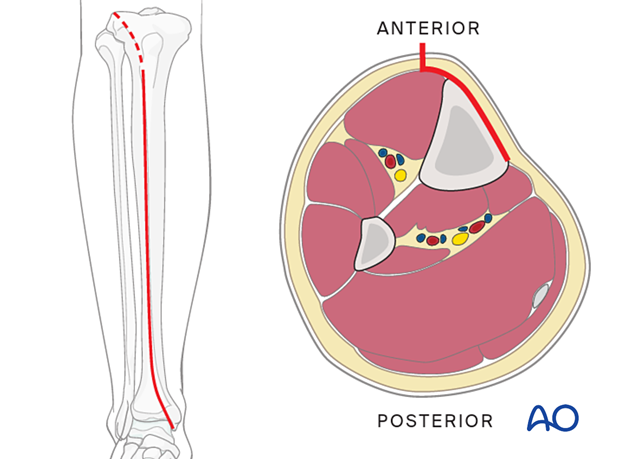
Anteromedial approach
An anteromedial approach can be used if the soft-tissue envelope allows. The advantage of this approach is that it removes no muscle from the fracture fragments. Also, the medial surface of the tibia is normally flat, and conventional plates can be contoured to fit it or pre-contoured plates used with minimal or no modification.
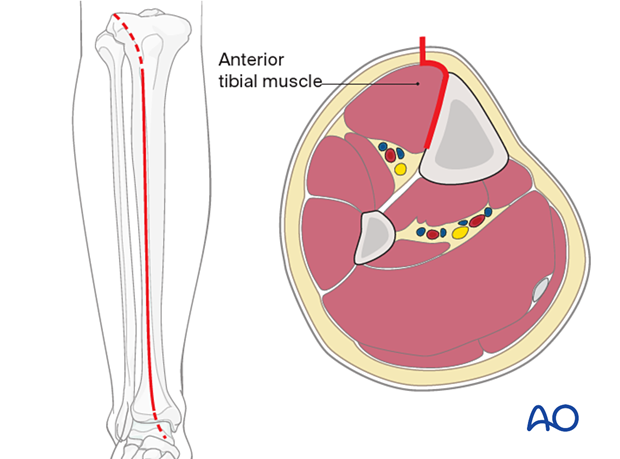
Anterolateral approach
The anterolateral approach can also be used if the plate is best placed on the lateral surface of the tibia. It can also be used when the medial soft tissues are compromised.
3. Open reduction
Introduction
Open, or direct, reduction is necessary to achieve the required anatomical reduction.
Mobilize just enough of the periosteum around the fracture edges to assess the quality of the reduction. Take care to protect the periosteum wherever possible.
Pointed reduction forceps are preferred because they do less damage to the soft tissues.
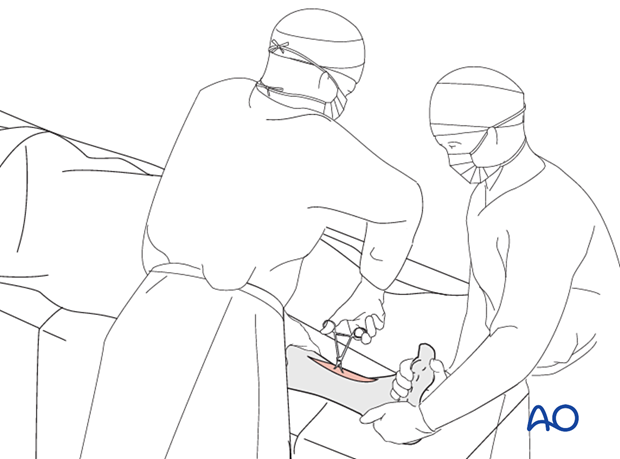
Manual traction
As a first step, length and rotation must be restored. This may be possible with manual traction. Otherwise, mechanical aids such as a large distractor, or bone spreader, should be considered.
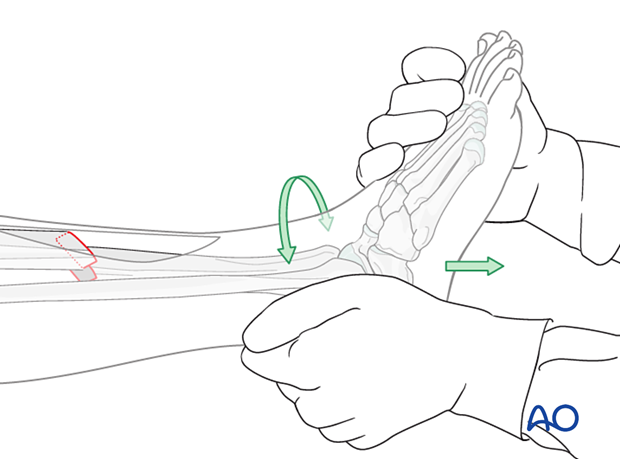
Reduction of the fracture
Once length and rotation are restored, pointed reduction forceps are used to compress and anatomically reduce the fracture. The tips of the forceps should be applied perpendicular to the plane of the fracture, just like a lag screw. Place the forceps outside the intended path of the lag screw.
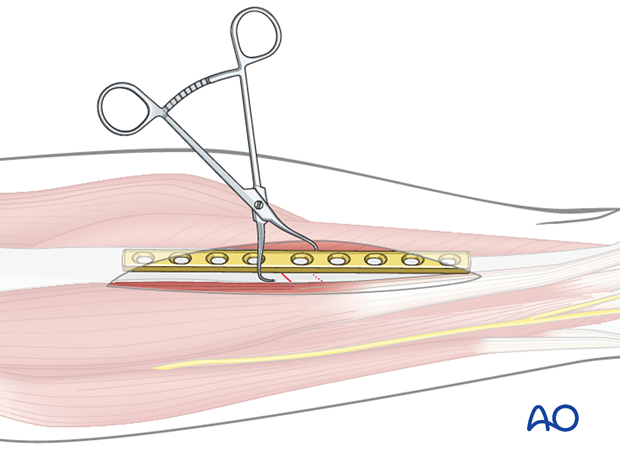
Provisional fixation with pointed reduction forceps
Use pointed reduction forceps to provisionally stabilize the fracture. Select a position for the forceps so that it will not interfere with the planned position of the screw and the plate.
Also, consider that the forceps can be positioned either medially or laterally. Choose the position that allows the most stability with the least soft-tissue damage.
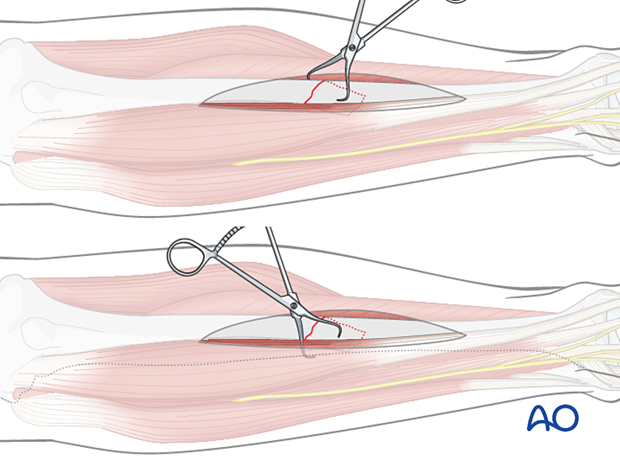
4. Confirm fracture plane
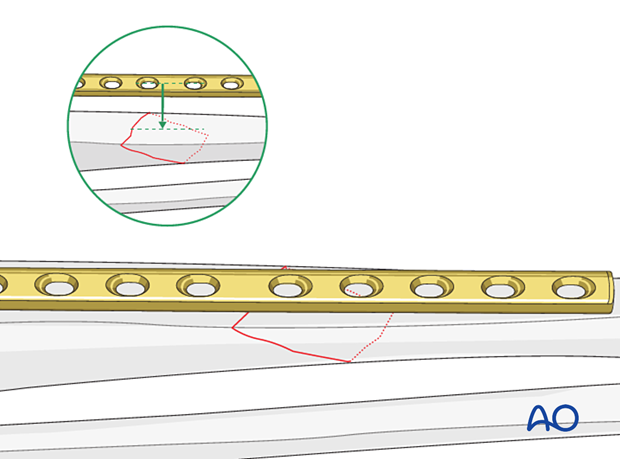
Confirm that the fracture apex lies on the tibial crest. This indicates that the lag screw must lie outside the plate.
If the fracture apex is on the anteromedial or anterolateral surface and the plate can be applied over it, a compression plate with a lag screw should be applied instead.
If the plate cannot be applied over the fracture apex, a lag screw either outside or through a protection plate should be employed.
5. Lag screw insertion
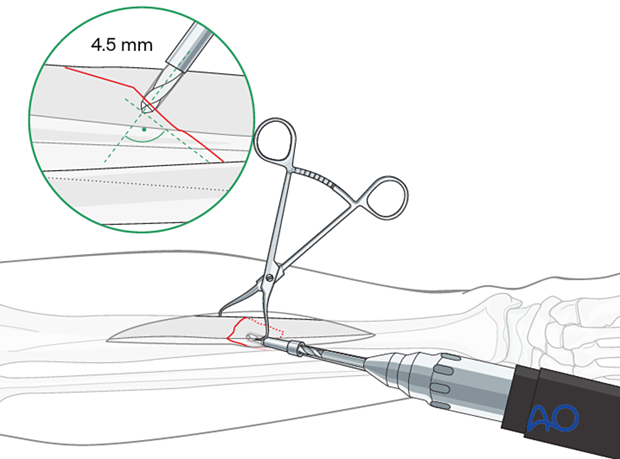
Drill the gliding hole for the lag screw
Using the appropriate drill guide and drill bit, drill a gliding hole in the near cortex. This screw must not interfere with planned plate placement.
Ensure that the direction of the drill is as perpendicular to the fracture plane as possible.
More information about lag screw insertion is provided here:
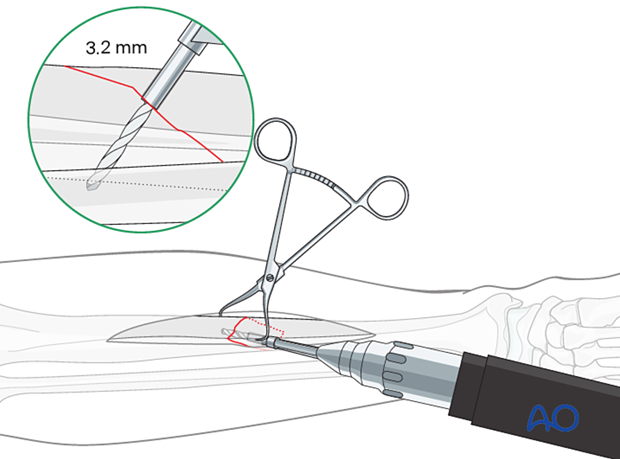
Drill the thread hole
Insert the drill guide through the plate and the gliding hole. Use the appropriate drill bit to drill for the core diameter of the chosen screw just through the far cortex.
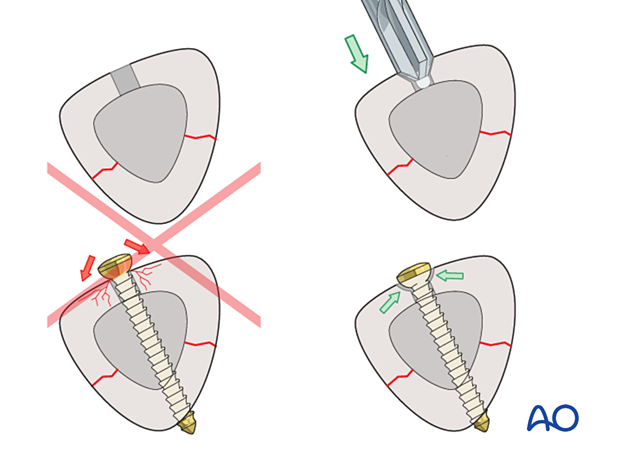
Countersinking in diaphyseal bone
There are two important reasons for countersinking:
- It ensures that the screw head has the maximal contact area with the bone, so that its compressive forces are widely distributed
- A countersunk screw head is less prominent and leads to less soft tissue irritation
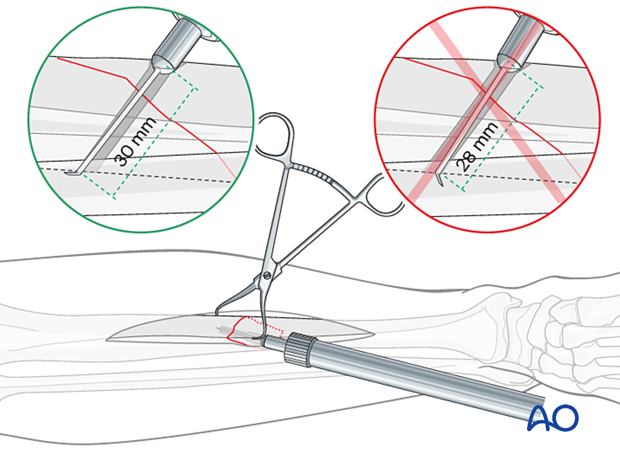
Measure for screw length
Use a depth gauge to measure for screw length.
Measure the longer side of an oblique drill hole, as shown, to ensure sufficient screw length.
A screw should protrude 1–2 mm through the opposite cortex to ensure thread purchase. If a screw is too long, it may irritate the surrounding soft-tissue envelope in which the tip protrudes.
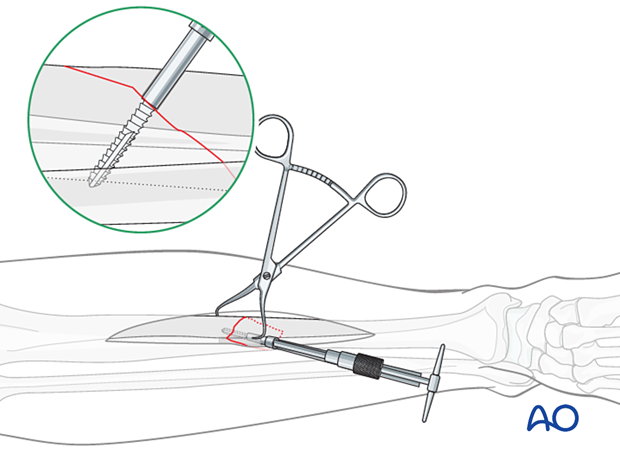
Tap the thread hole
Use a tap and the corresponding drill sleeve to tap the thread hole for the chosen screw size (if self-tapping screws are not used).
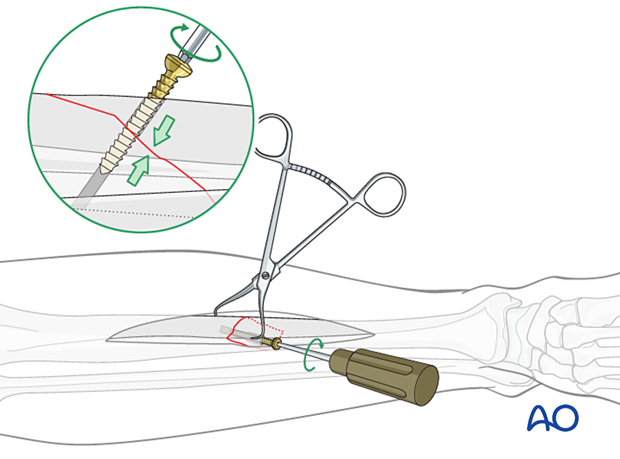
Insert the lag screw
Insert the lag screw and carefully tighten it. Confirm that the fracture is reduced anatomically and compressed.
6. Plate fixation
Plate selection and preparation
The chosen plate should allow the following:
- A hole near the middle of the fracture, for the first lag screw to be inserted as perpendicular as possible to the fracture plane
- Sufficient length for at least four screws proximal and distal to the fracture zone
Remember that whenever the plate is placed distally, it must be twisted and bent to match the shape of the tibia in that region.
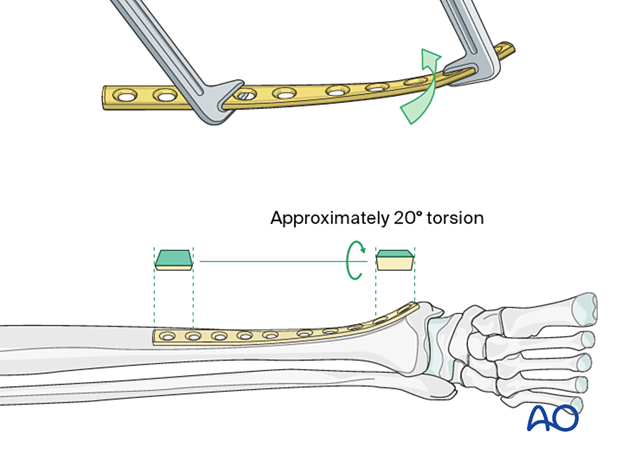
Insertion of screws
Insert the screws alternating between the proximal and distal fragments. Start with the screws closest to the fracture plane and work your way outwards.
Drill for the fixation screws. At least four screws should be used on the proximal fragment, and at least four screws on the distal fragment.
Use cortical screws for the diaphysis.

7. Aftercare
Perioperative antibiotics may be discontinued before 24 hours.
Attention is given to:
- Pain control
- Mobilization without early weight bearing
- Leg elevation in the presence of swelling
- Thromboembolic prophylaxis
- Early recognition of complications
Soft-tissue protection
A brief period of splintage may be beneficial for protection of the soft tissues but should last no longer than 1–2 weeks. Thereafter, mobilization of the ankle and subtalar joints should be encouraged.
Mobilization
Active, active assisted, and passive motion of all joints (hip, knee, ankle, toes) may begin as soon as the patient is comfortable. Attempt to preserve passive dorsiflexion range of motion.
Weight bearing
For fractures treated with plating techniques, limited weight bearing (15 kg maximum), with crutches, may begin as tolerated, but full weight bearing should be avoided until fracture healing is more advanced (8–12 weeks).
For fractures treated with intramedullary nailing, weight bearing as tolerated, with crutches, may begin immediately.
Follow-up
Follow-up is recommended after 2, 6, and 12 weeks and every 6–12 weeks thereafter until radiographic healing and function are established. Weight bearing can be progressed after 6–8 weeks when x-rays have indicated that the fracture has shown signs of progressive healing.
Implant removal
Implant removal may be necessary in cases of soft-tissue irritation caused by the implants. The best time for implant removal is after complete bone remodeling, usually at least 12 months after surgery. This is to reduce the risk of refracture.
8. Case
This is a simple spiral fracture of the tibial shaft with a proximal fibular neck fracture.
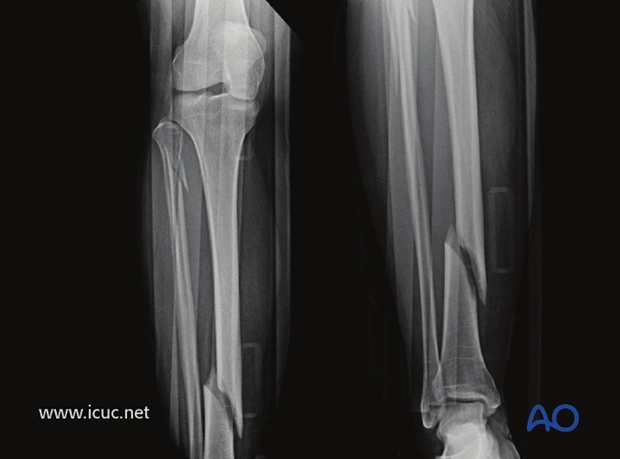
Lateral image of the same fracture.
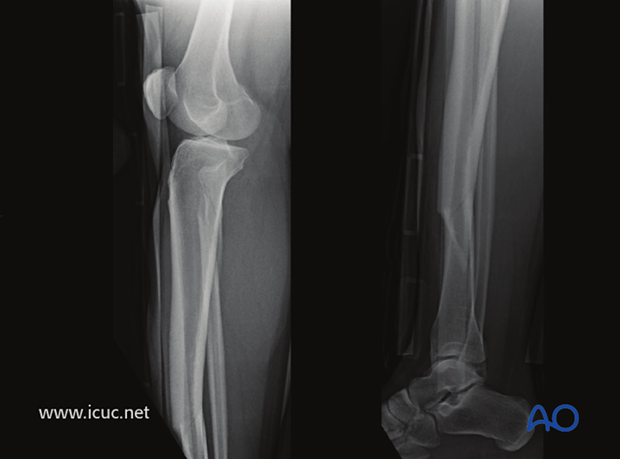
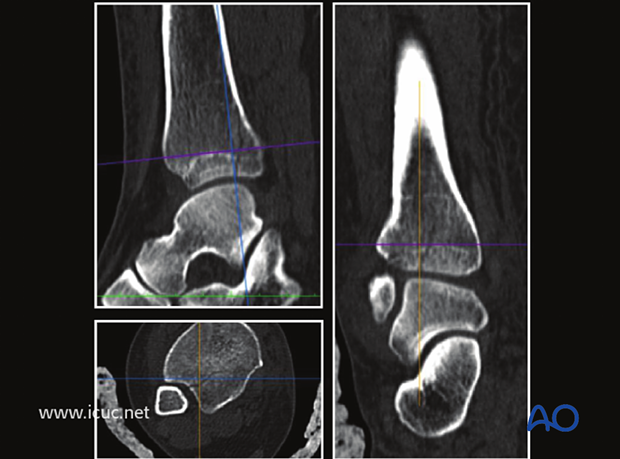
Because of the spiral nature of this fracture type, it may have a component that goes into the tibiotalar joint. A CT scan was used to assess this.
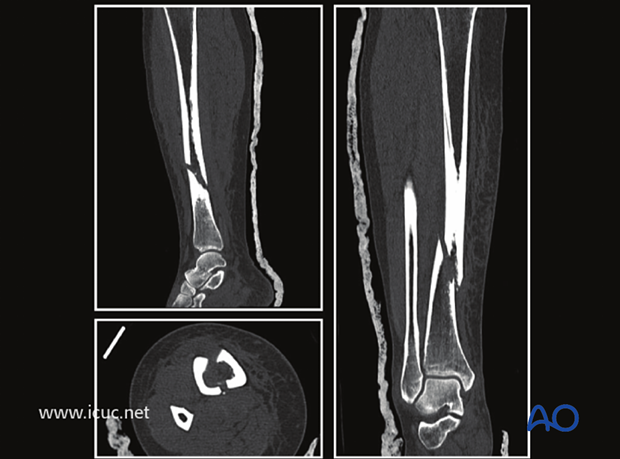
A CT scan at the malleolar level showed that the fracture continued into the tibiotalar/ankle joint but with minimal displacement.
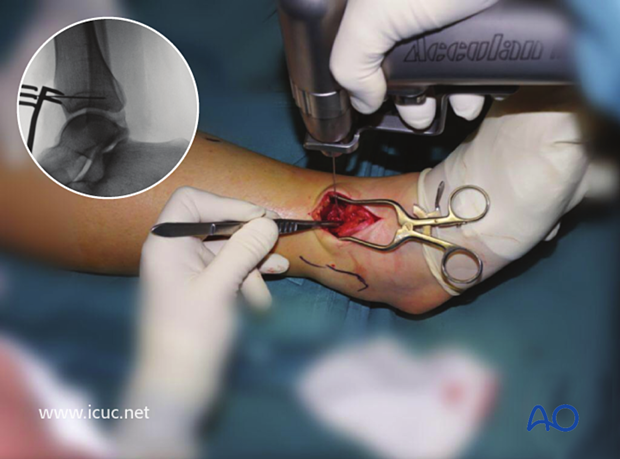
Before plating the tibia, a lag screw was placed across the fracture site just above the ankle to prevent the intraarticular component from displacing.
A K-wire was inserted to ensure that the fracture did not displace during lag screw insertion.
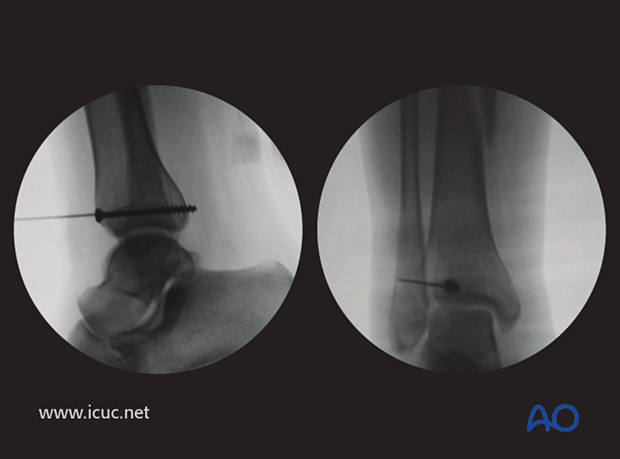
The lag screw was placed just above the joint line in the AP plane. This lag screw is probably 2 mm too long.
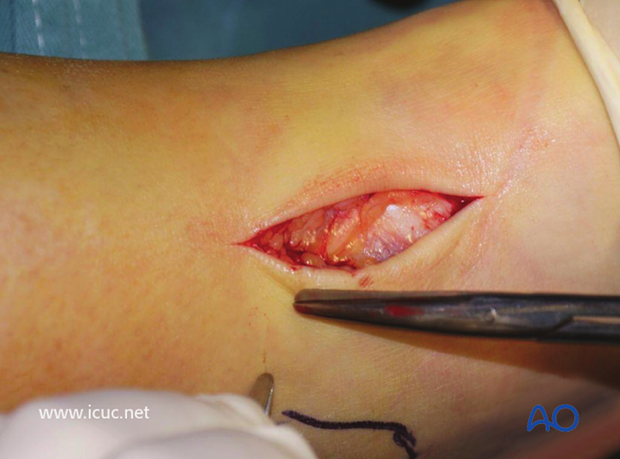
The fracture was reduced with the help of a distractor with pins in the calcaneus and the proximal tibia. Note the small incision directly anterior, perpendicular to the fracture plane, positioned so that the fracture can be reduced under direct vision.
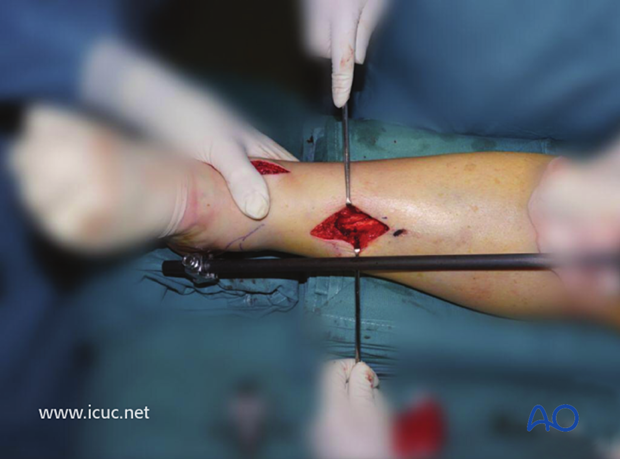
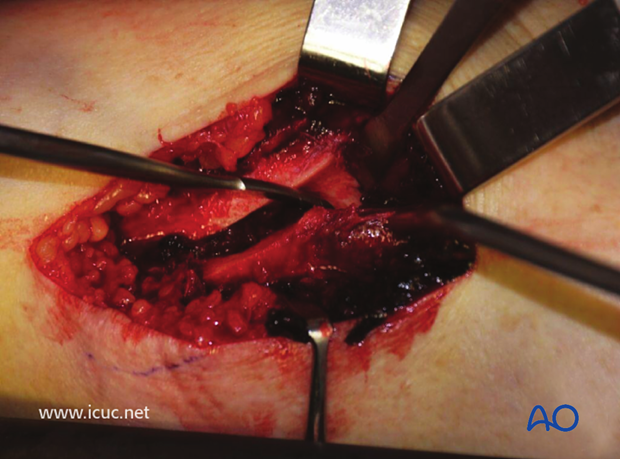
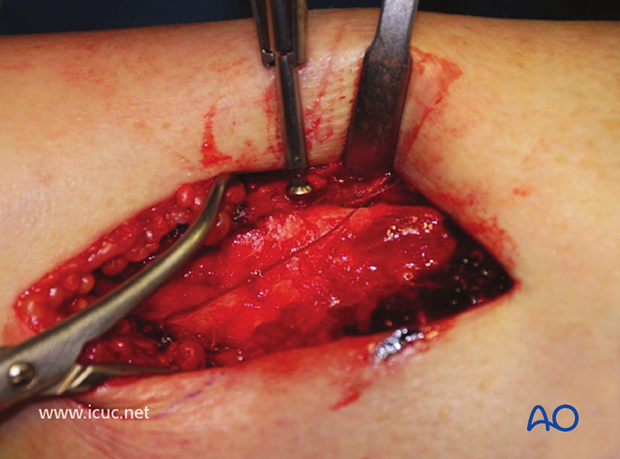
The fracture has been exposed but not yet reduced.
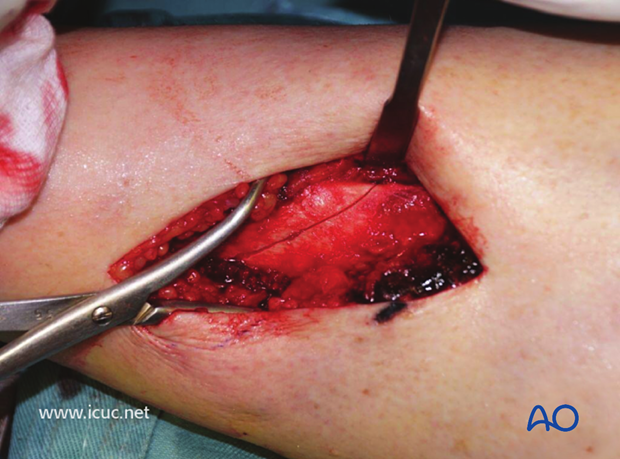
The fracture has now been reduced and is held with a sharp Weber clamp.
The pilot hole for a cortical lag screw is drilled from anterior to posterior.
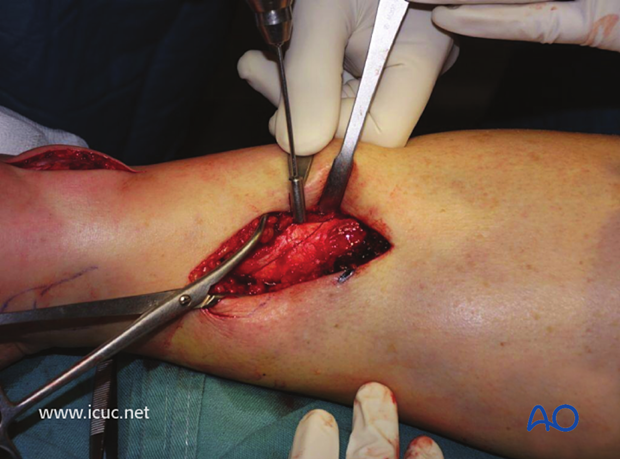
After tapping and countersinking, the cortical lag screw is inserted. Care is taken not to overtighten it as this might create a new fracture.
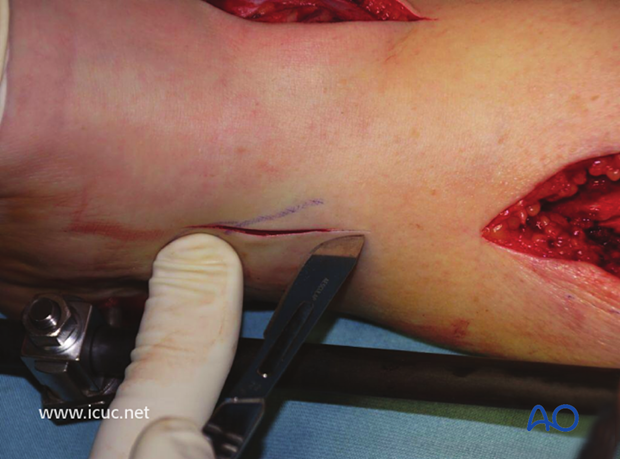
The distal incision for the minimally invasive osteosynthesis (MIO) plate insertion is made on the medial side, taking care not to damage the saphenous vein and nerve.
The appropriate length locking compression plate (LCP) is selected and contoured.
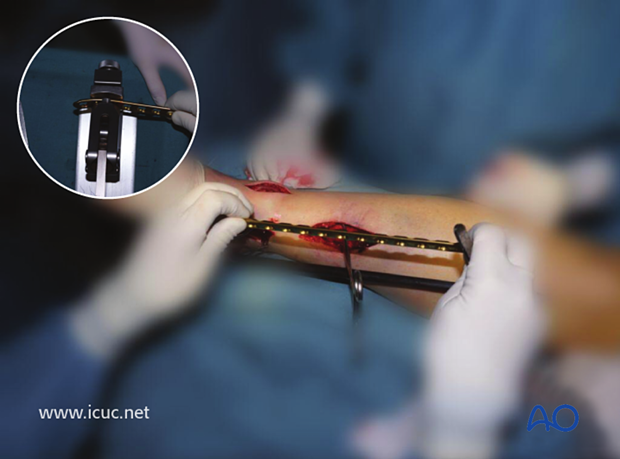
A small amount of distal contour allows for the medial malleolar flare.

The proximal incision is made.
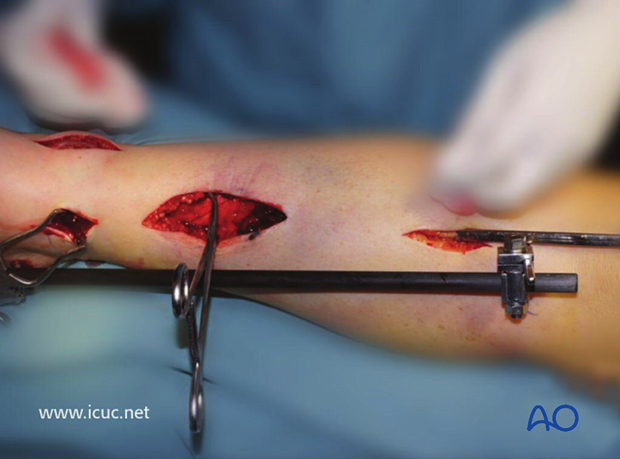
The plate is slid under the soft tissues along the surface of the bone. In this case, the plate required further contouring so it was removed, adjusted, and reinserted.
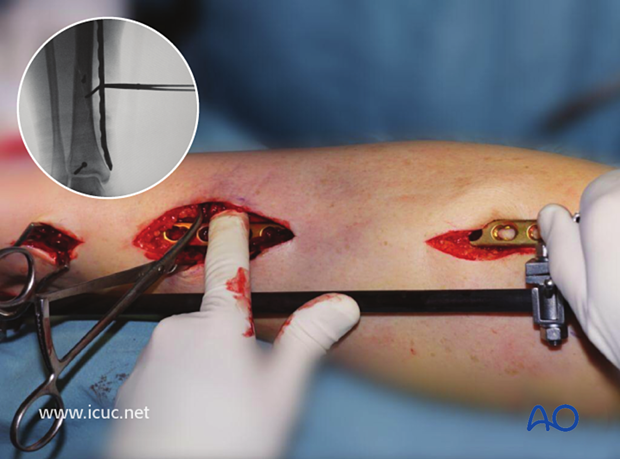
Final AP x-rays of minimally invasive osteosynthesis (MIO) plating using the near far principle for screw placement. It is important to remember that any screw that crosses a fracture line should be used with the lag technique.
As the fracture was well reduced, and held with two lag screws, the surgeon felt that only two distal screws and two proximal screws were required to achieve sufficient stability.
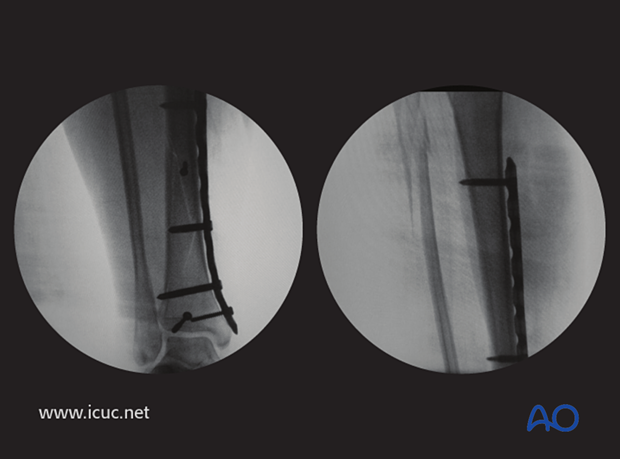
AP lateral x-rays at 6 weeks, show the reduction has been maintained and the fracture is healing.
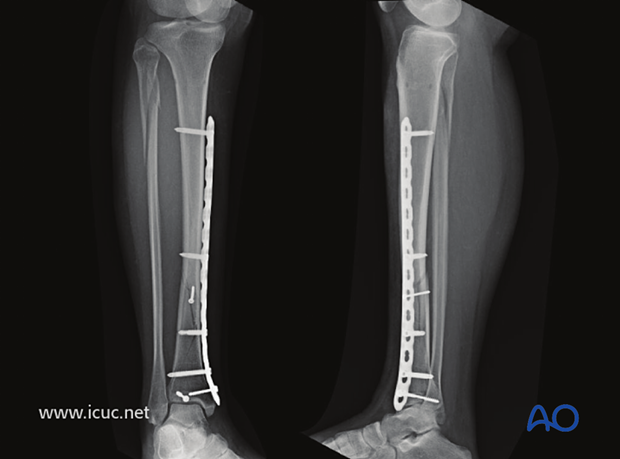
Healed tibial fracture at 6 months.
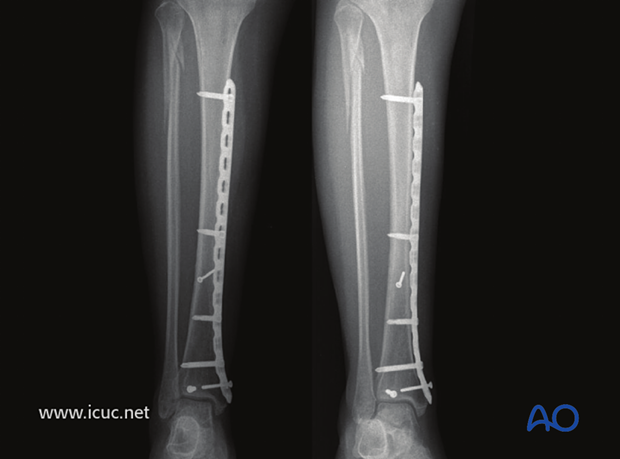
Clinical image of good outcome at 30 weeks.