ORIF - Lag screws with protection plate
1. Principles
General considerations
Open reduction and internal fixation (ORIF) with lag screws and a neutralization plate is a high-risk and difficult technique for these injuries.
The utmost care must be taken to prevent excessive stripping of the soft tissues from the intermediate fragments, as the blood supply to these is usually tenuous.
The surgeon should consider less invasive techniques such as closed intramedullary nailing, indirect reduction and bridge plating, or external fixation.
Indications
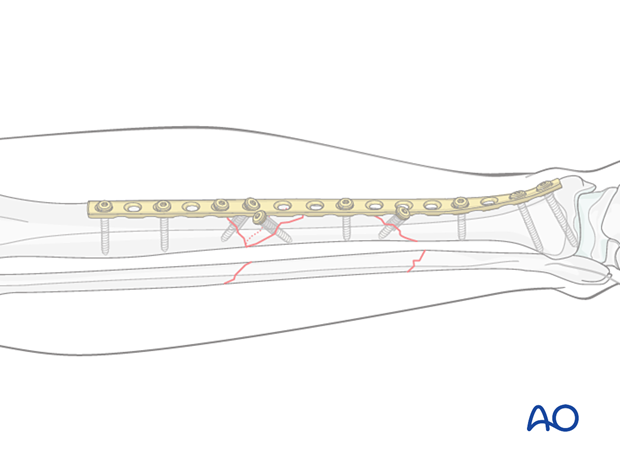
Segmental fractures with significant periarticular involvement may be best suited for plate fixation. Long oblique or spiral fracture patterns are appropriate for lag screws and a neutralization plate.
Surgical tactics
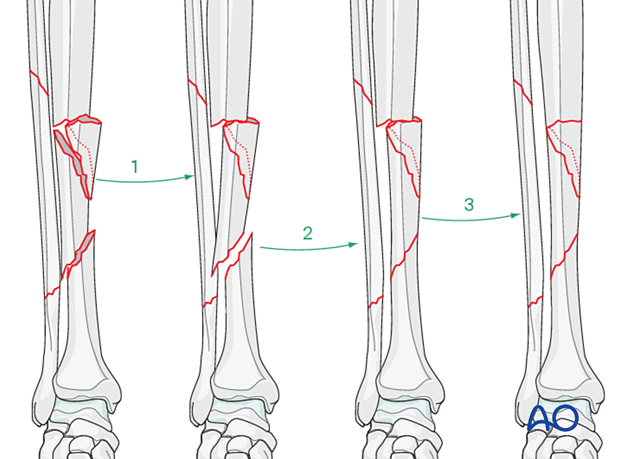
If open reduction and lag screw fixation with a neutralization plate is selected, the appropriate surgical tactic is to reduce sequentially the number of fractures, fixing one fracture plane at a time. The idea is to go from three fracture lines to two, to one, starting with the simplest fracture.
Fracture stabilization
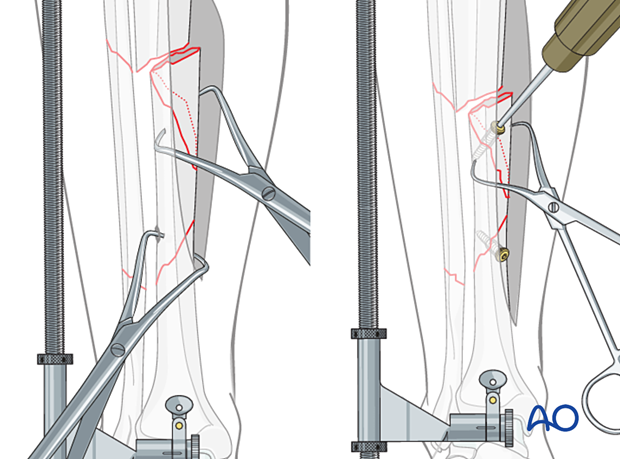
Another principle is that fracture stability should be increased in progressive steps. Since instability risks soft-tissue disruption, it is important that provisional stabilization protects the soft tissues during successive steps of reduction and fixation.
Initial stabilization of a complex diaphyseal fracture is often best obtained with a bridging distractor or external fixator. Strategically placed bumps to support the leg may also help.
With some complex fractures, a plate that bridges the fracture zone may be applied provisionally before or during the application of interfragmentary lag screws.
2. Patient preparation and approaches
Patient preparation
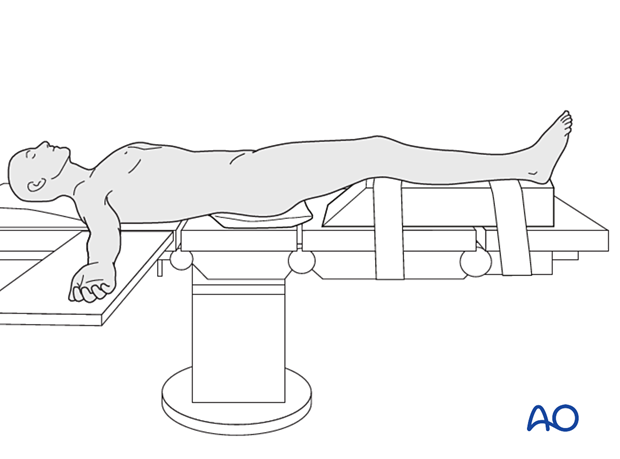
The patient is placed in a supine position on a radiolucent table or a standard operating table with a radiolucent extension. A pad is placed underneath the buttock to prevent external rotation.
A large foam bolster or cushion is placed under the affected leg to raise it above the opposite leg and facilitate lateral C-arm images.
Anteromedial approach
An anteromedial approach is preferred if the soft tissues allow. The advantage of this approach is that it does not remove muscle from the fracture fragments. Also, the medial surface of the tibia is normally flat, and conventional plates can be contoured to fit it or pre-contoured plates used with minimal or no modification.
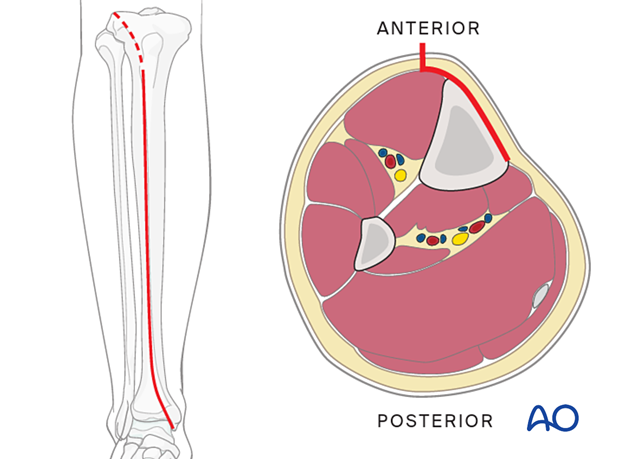
Anterolateral approach
The anterolateral approach should be chosen if the soft tissues do not allow for an anteromedial approach. It is difficult to use this approach distally due to soft-tissue interference and the challenge of contouring the plate along the lateral aspect of the tibia.
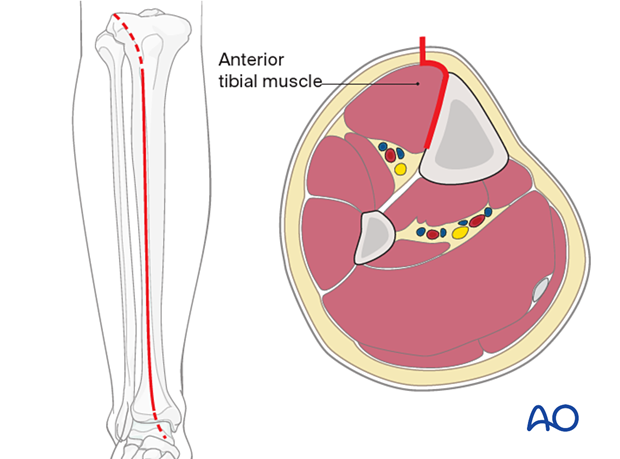
3. Reduction
Reduction principles
The key to all fracture reduction is restoring axial length.
Ways of gaining length are:
- Manual traction
- Distractor/external fixator
- Articulated tension device (ATD)
- Push-pull screws
If any shortening is present, distraction should be applied and maintained before fracture consolidation occurs. Otherwise, callus and vascular soft tissues will need to be released from bone fragments to permit reduction. This may require provisional external fixation. Even if the delay before reduction and fixation is short, progressive intraoperative lengthening is easier and less traumatic if aids for distraction are routinely employed.
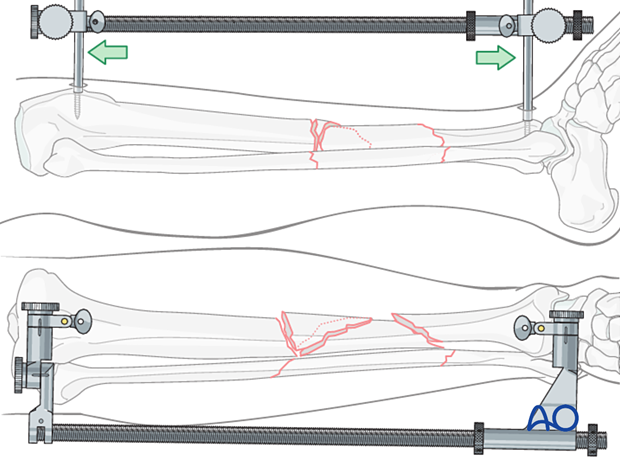
Example: Large distractor or external fixator
A large distractor is very helpful for reduction. Schanz pins are placed in the proximal and distal fragments. Distraction is applied across these pins by turning the nut on the threaded rod.
If the plate is to be placed medially, then the distractor should be placed anteriorly.
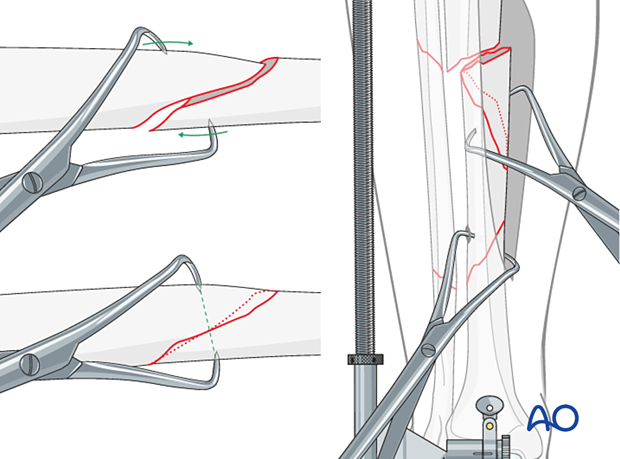
Final reduction of the fracture
Final reduction of the fracture is done with pointed reduction forceps.
Placement of the reduction forceps is key. Each point must be placed in anticipation of where it will be with the fracture reduced once length is restored.
These forceps will often be placed almost along the line of an ideal lag screw.
Provisional fixation
At this point, the individual fractures can be either provisionally fixed with reduction forceps or definitively fixed with lag screws.
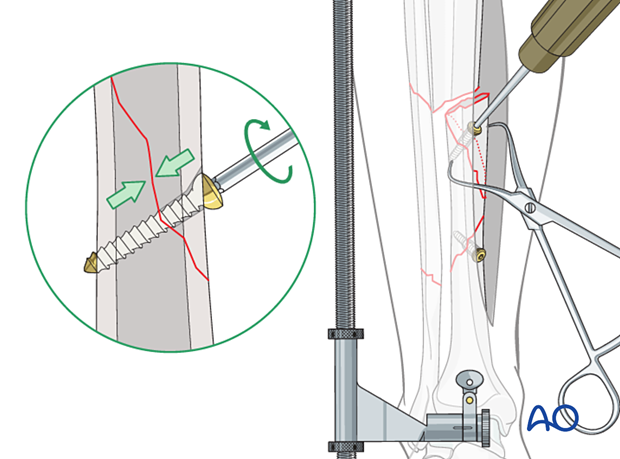
4. Lag screw placement and plate insertion
Lag screw insertion
Lag screws should be inserted where possible without interfering with plate placement. Some lag screws will be outside the plate and some lag screws will be through the plate.
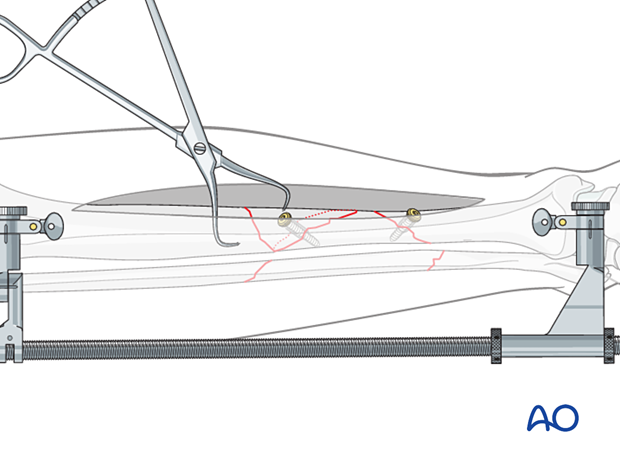
Plate application
Once a plate of the proper length is selected, it must be properly contoured. Instructions for these steps follow.
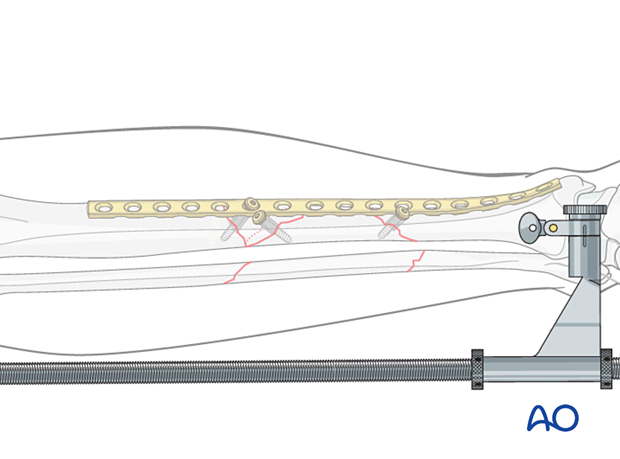
5. Plate selection and preparation
Choice of plate
Plate length is based upon symmetry above and below the fracture zone. In the case of a segmental fracture, the fracture zone includes all fracture lines. In C-type fractures, at least 3–4 screw holes on either side of the fracture zone are necessary. Another guideline, when fracture location permits, is that the plate should be roughly three times the length of the fracture zone.
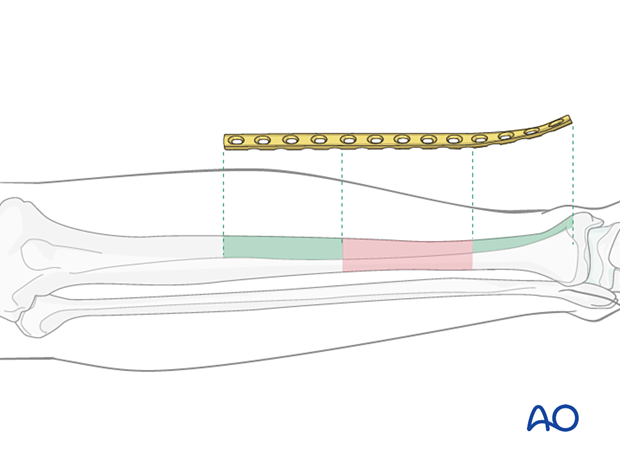
When the fracture zone is very distal or proximal, there may not be enough room for symmetric plate length in the segment nearest the articular surface. In this situation, a plate with multiple hole options in the metaphysis is chosen to improve fixation in the short periarticular segment.
A locking plate may be indicated if bone quality is poor or when the fracture extends into softer metaphyseal bone.
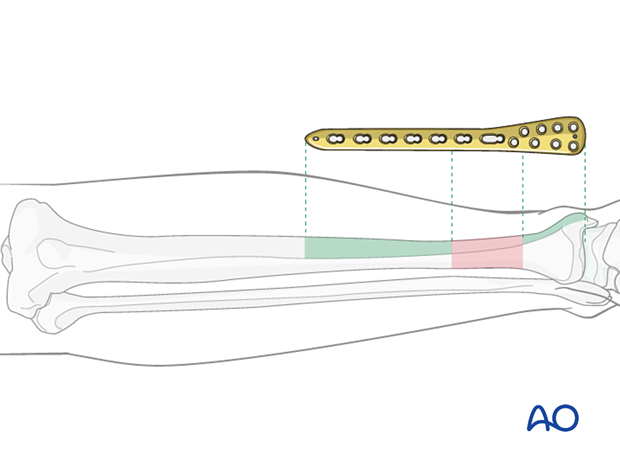
Traditionally a 4.5 mm plate has been advised for the tibial shaft. Advantages include increased plate thickness and larger screw size for added strength. These plates are difficult to contour and may be too prominent, however.
A 3.5 mm plate offers improved contourability and multiple screw options in metaphyseal (end-segment) zones. As these plates are thinner, they are less stiff than the large fragment plates.
Another consideration is the choice between an anatomically pre-contoured plate or one which the surgeon contours. For plates that need to be contoured, the following steps must be employed.
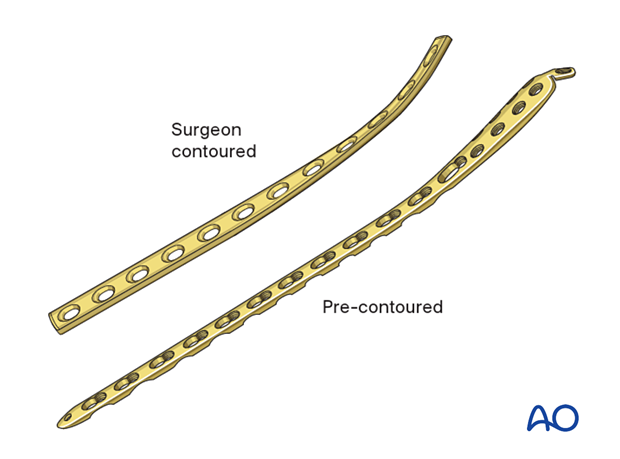
Plate contouring
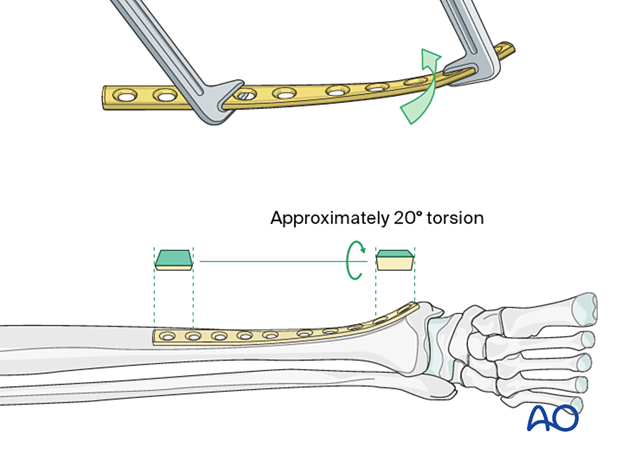
Twisting the plateThe anteromedial surface of the tibial shaft twists internally approximately 20° as it approaches the medial malleolus.
The first step of plate contouring is to twist the plate so it matches the tibial surface upon which it will lie.
If the plate is bent before it is twisted, the process of twisting will alter the bend that has been created.
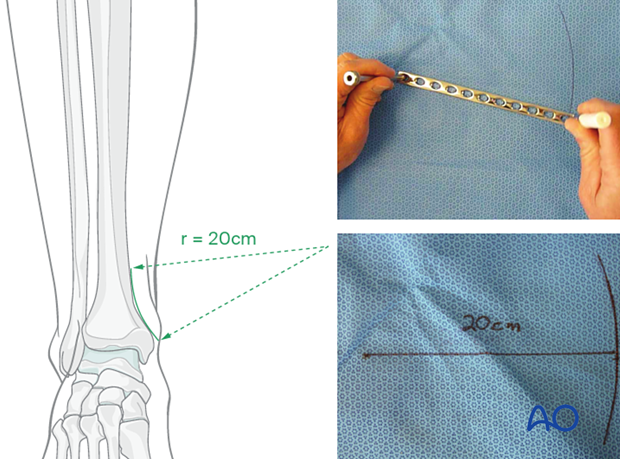
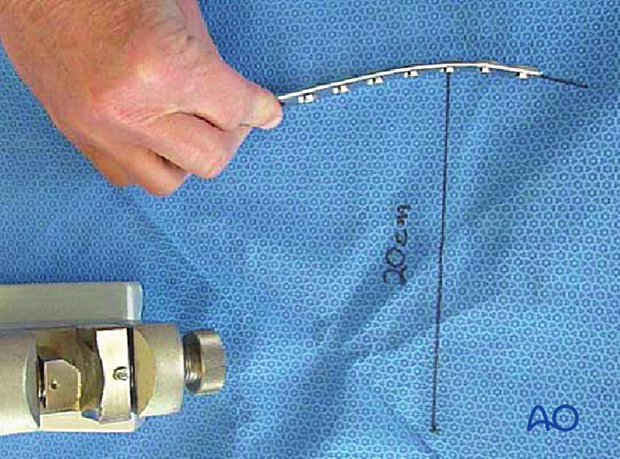
Depending upon the plate location, more or less bending of the plate will be required to match the contour of the intact (or reduced) bone. Much of the medial tibial shaft is quite straight, so little bending is required. The distal medial surface has a significant concavity, with a typical radius of curvature of 20 cm, as illustrated.
A 20 cm radius can be drawn on a sterile drape and used as a template for plates to be used in this location.
The plate can be bent with bending irons alone, but bending with a bending press is preferable, because it gives more control.
In either case, the bending is done in small steps to produce a smooth contour. Contouring only takes place over the distal 10–12 cm of the plate. When finished, the plate should match the 20 cm radius of curvature.
6. Plate application
Plate fixation
After the properly contoured plate is applied, the first screws are placed to obtain interfragmentary compression and to anchor the plate proximally and distally.
At this point, stability is provided by the plate, and the distractor or external fixator can be removed. Remaining screws are added as required.
Remember that it is not necessary to fill every hole in the plate, particularly in the diaphysis.

7. Aftercare
Perioperative antibiotics may be discontinued before 24 hours.
Attention is given to:
- Pain control
- Mobilization without early weight bearing
- Leg elevation in the presence of swelling
- Thromboembolic prophylaxis
- Early recognition of complications
Soft-tissue protection
A brief period of splintage may be beneficial for protection of the soft tissues but should last no longer than 1–2 weeks. Thereafter, mobilization of the ankle and subtalar joints should be encouraged.
Mobilization
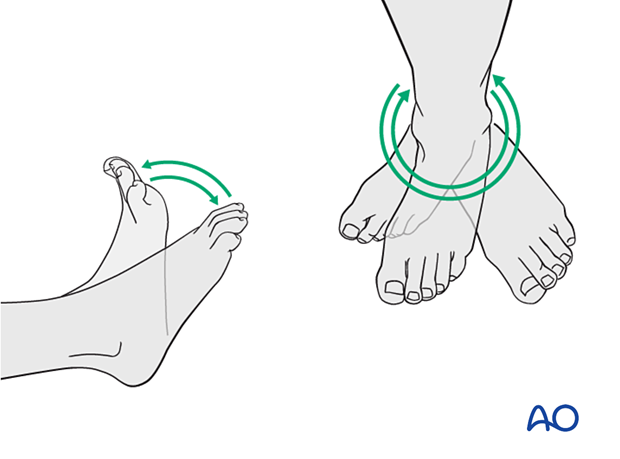
Active, active assisted, and passive motion of all joints (hip, knee, ankle, toes) may begin as soon as the patient is comfortable. Attempt to preserve passive dorsiflexion range of motion.
Weight bearing
For fractures treated with plating techniques, limited weight bearing (15 kg maximum), with crutches, may begin as tolerated, but full weight bearing should be avoided until fracture healing is more advanced (8–12 weeks).
For fractures treated with intramedullary nailing, weight bearing as tolerated, with crutches, may begin immediately.
Follow-up
Follow-up is recommended after 2, 6, and 12 weeks and every 6–12 weeks thereafter until radiographic healing and function are established. Weight bearing can be progressed after 6–8 weeks when x-rays have indicated that the fracture has shown signs of progressive healing.
Implant removal
Implant removal may be necessary in cases of soft-tissue irritation caused by the implants. The best time for implant removal is after complete bone remodeling, usually at least 12 months after surgery. This is to reduce the risk of refracture.













