ORIF - Plate fixation
1. Anatomy
The blood supply to the talus is very compromised with a fracture dislocation scenario. The posterior tibial artery has branches medially. The dorsalis pedis has branches anteriorly. The peroneal artery has branches laterally. They are all connected through a sling of vessels that lie within the sinus tarsi.
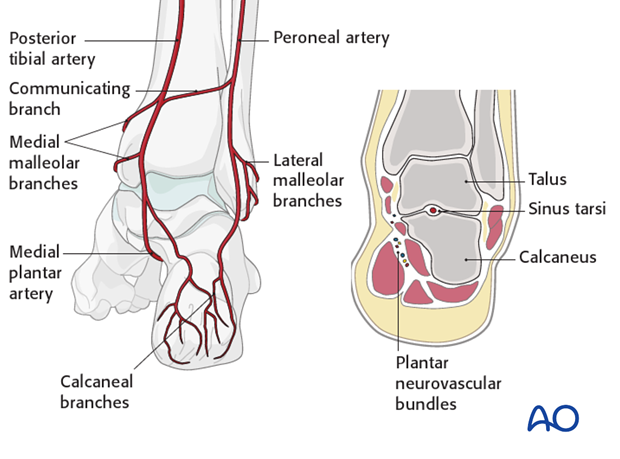
The deltoid branch of the posterior tibial artery must be protected. It is an important point for blood supply entry into the medial talus. This is the reason why a medial malleolar osteotomy is successful as it protects the talar blood supply.
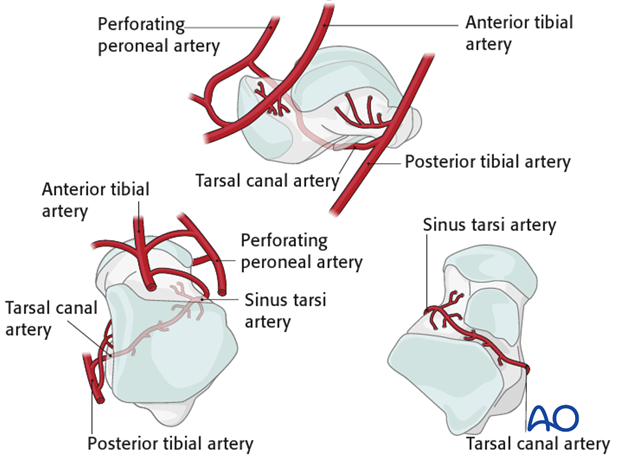
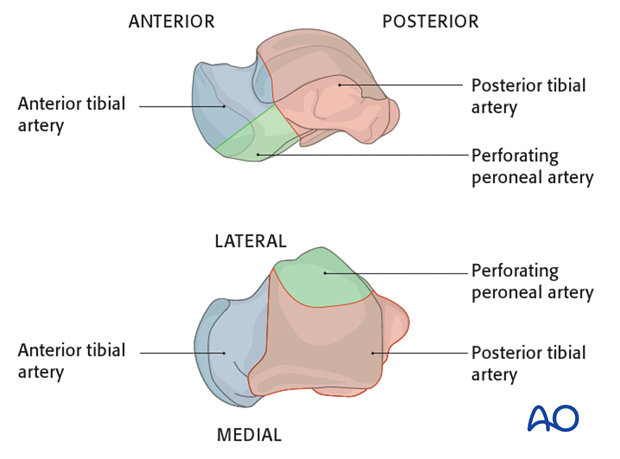
The deltoid branches are important to supply blood to the medial talar neck and talar body. Branches from the dorsalis pedis supply the talar head and most of the dorsal talar neck. The artery of the tarsal canal coming from branches off of the posterior tibial artery supply most of the talar body.
The peroneal artery has the least contribution laterally.
2. Emergency reduction
Emergency action
The high-energy displaced fractures of the talar neck with, or without, dislocation of the talar body, often present with severe soft-tissue injuries, including open fractures, or both. To prevent further soft-tissue damage, urgent closed reduction is mandatory. Once that has been carried out, even only to the point of improving the position, if not completely reducing the fracture, one can begin preoperative planning of further and definitive care.
If a satisfactory reduction of the fragments can not be achieved, or if one is dealing with an open fracture, then an urgent operative intervention is mandatory.
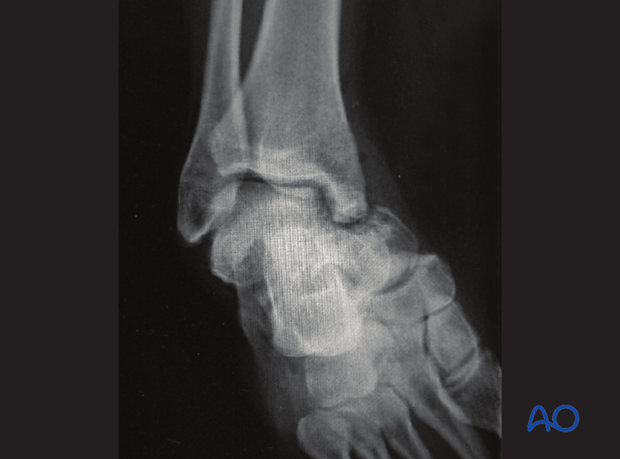
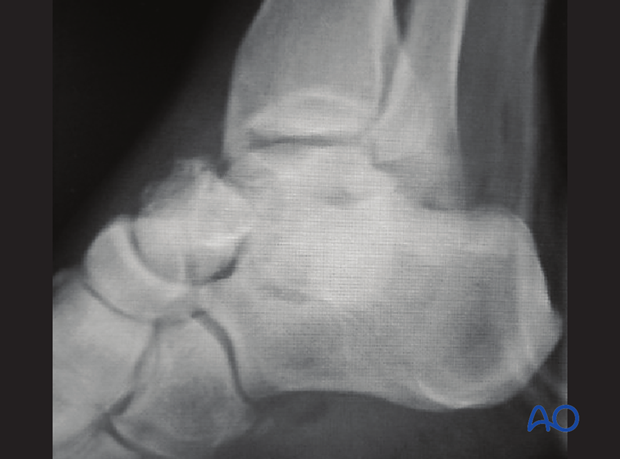
This image shows a talar neck fracture dislocation with medial displacement and comminution before reduction.
Closed reduction technique
Which side is injured is obvious by looking at the foot that it is swollen and deformed. It is useful to look at the patient’s other normal foot to determine individual anatomy.
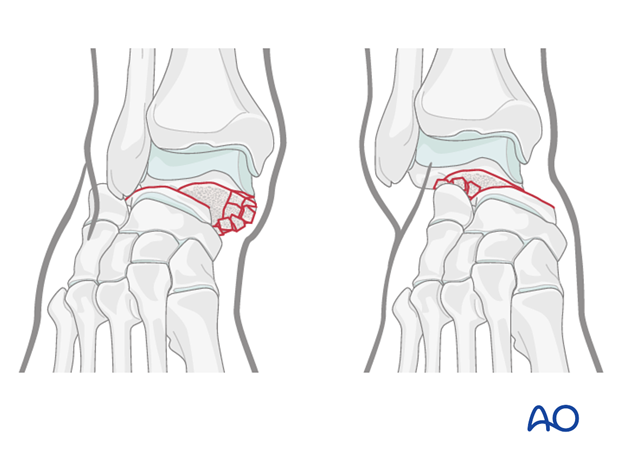
The talar body will stay with the tibia, yet the talar head and calcaneous will sublux medially or laterally.
Traction
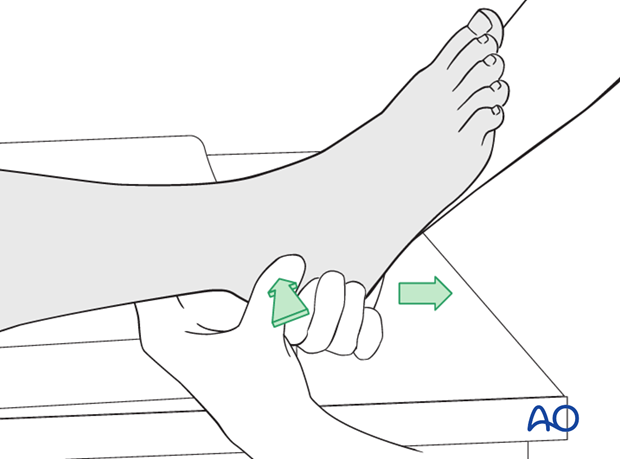
The reduction maneuver is facilitated by longitudinal traction and reversal of the force and its direction.
If successful, normal anatomy will be restored. The deforming force may have been a medially directed force, or laterally directed force, depending upon whether this is a medially or laterally displaced injury.
Usually, with type 2 talar neck fractures, a successful reduction is accompanied by reestablishment of normal foot anatomy.
Splintage with follow-up radiology will now determine whether the closed reduction is successful.
Multiple attempts of closed reduction are not advised as they can further injure the soft tissue.
3. Open reduction
Preoperative considerations
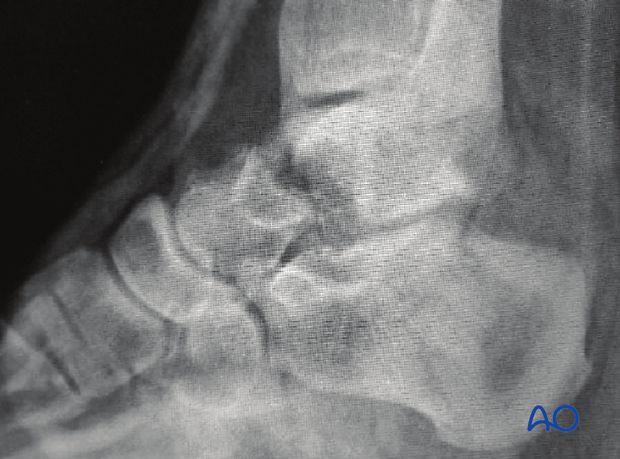
This image demonstrates a severe talar neck fracture with comminution that has been reduced, allowing for preoperative planning. This has markedly helped the soft tissues that had previously been compromised.
CT examination can be helpful when there is any question about displacement or requirements for debridement of the subtalar joint. Along the spectrum of injury, increasing displacement presupposes that there is more subtalar and tibiotalar osteochondral injury. This often requires surgical approaches for debridement and fixation of these fracture types.
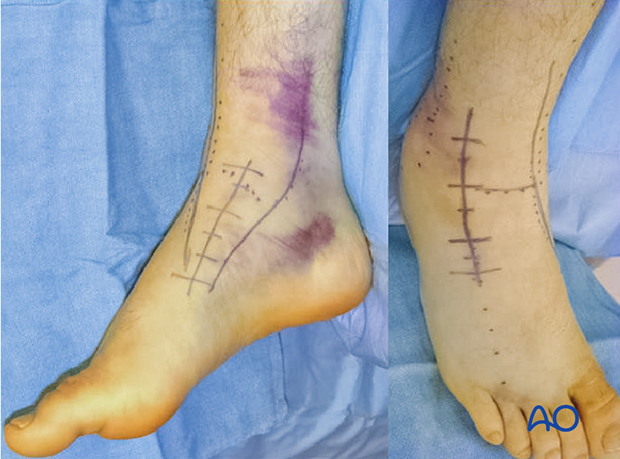
Exposure
The combined anteromedial and anterolateral incisions are optimal for all talar neck fractures that are treated operatively. These two exposures ensure adequate visualization for reduction and fixation.
Helpful adjuncts in surgery when doing an open reduction include joysticks, external fixator, small distractor, or lamina spreader. A headlamp helps with visualization, and an image intensifier will guide the reduction of this difficult fracture.
If a reduction can not be achieved with the standard two anteromedial and anterolateral approaches, then a medial malleolar osteotomy is the most common tactic that is used.
An alternative is the lateral malleolar osteotomy.
The medial malleolar osteotomy is performed by extending the anteromedial approach to provide access for the osteotomy. Remember that the deltoid ligament and the osteotomy fragment must be kept as one to preserve blood supply to the talar body.
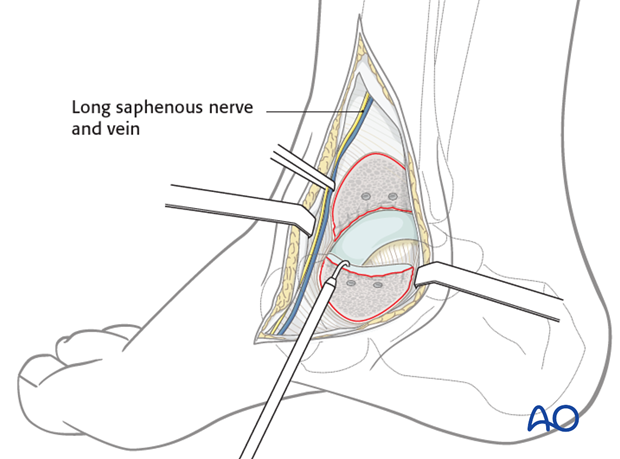
Open manipulation
Care should be taken to preserve all soft-tissue attachments (blood supply) to the talar body.
Two approaches should be used.
When the combined approaches are used and the reduction can not be obtained, then there is a series of steps for successfully obtaining the reduction.
Firstly, elevators and joysticks are advised, followed by the use of external fixators and distractors.
Lastly, the medial malleolar osteotomy would be performed as the most invasive, yet most definitive, tool.
Image intensification would be used at every step.
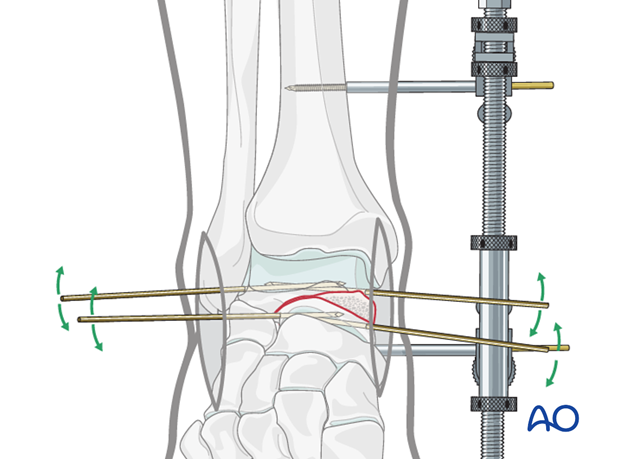
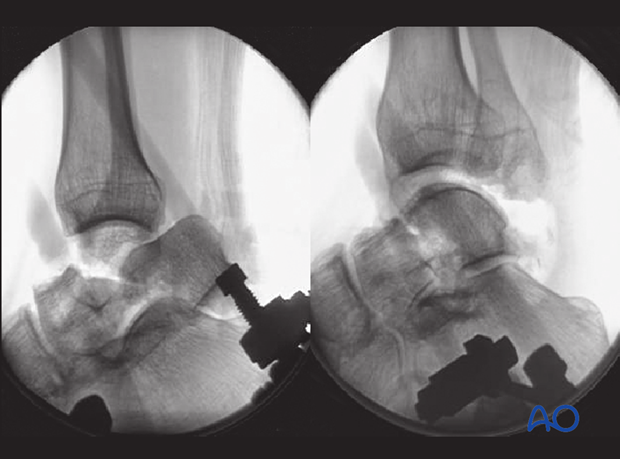
The images demonstrate a medial distractor with a patient under general anaesthetic with maximum muscle relaxation. The talar neck fracture has been reduced by distraction using the distractor which allowed derotation and reduction of the body into its anatomical position. The second image demonstrates the talar neck reduction with tibiotalar distraction still maintained.
4. Fixation
Preliminary fixation
K-wires are helpful to achieve preliminary fixation. K-wire placement is very important when using cannulated screws or plates, as the position of the wires can help with definitive screw and/or plate fixation. X-ray imaging of the other foot is helpful for comparison.
The lateral talar neck is usually not as comminuted as the medial side and can be reduced using fracture interdigitations and screw or plate fixation in a compression mode.
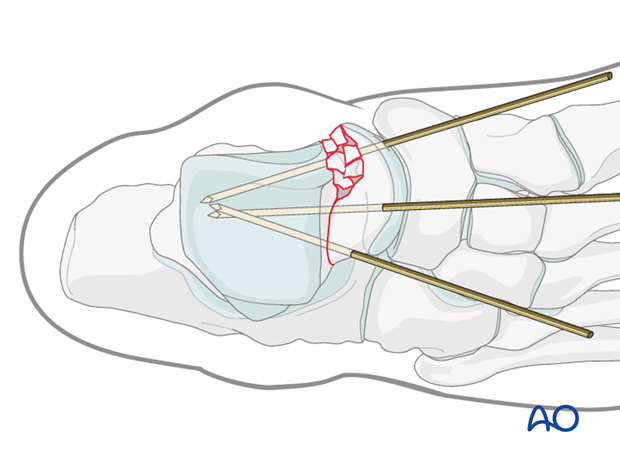
The medial K-wires are often best placed through the medial portion of the talar head articular cartilage.
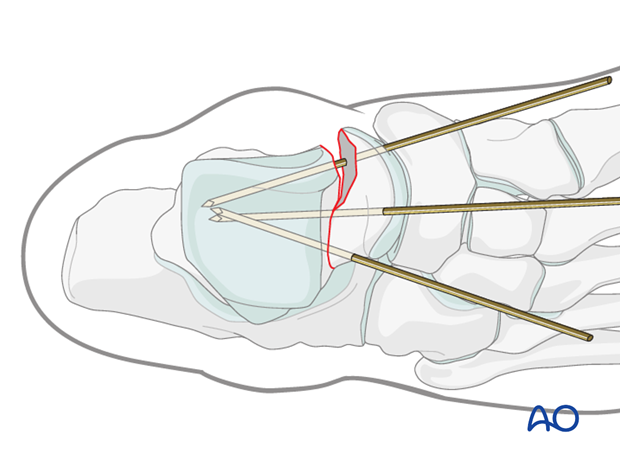
Sometimes, comminution is so extensive that image intensification and surgeon’s acumen is the best estimate for medial side reduction. Multiple K-wires are placed to assist in estimates of the best reduction, ensuring no shortening of the medial talus (medial column of the foot) and fixation is planned with a mini fragment plate.
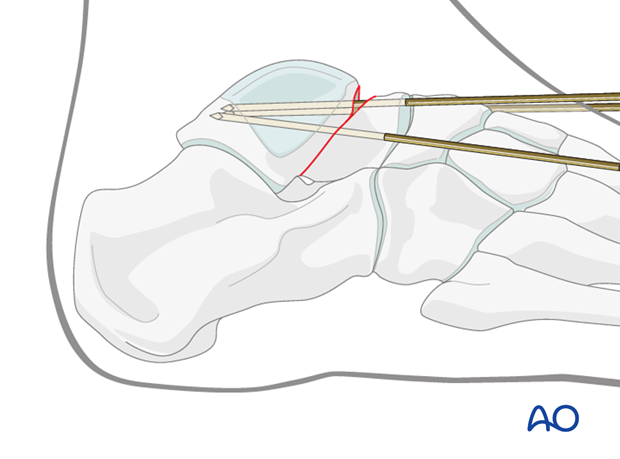
Plate fixation
With the K-wires placed appropriately and with image intensification verifying accurate reduction, a plate is contoured both medially and laterally through the anteromedial and anterolateral combined approaches.
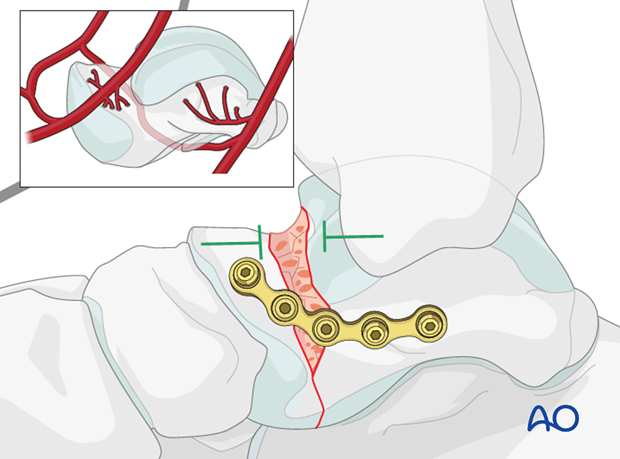
The medial plate will fit along the medial neck with screws into the head and the body, leaving the mid-portion overlying the comminution free of screws.
With this fixation, medial talar neck shortening or collapse will not occur.
If medial talar neck comminution is very severe with a resultant bone defect, then primary bone graft might be considered.
The lateral plate will fit along the lateral neck and process of talus.
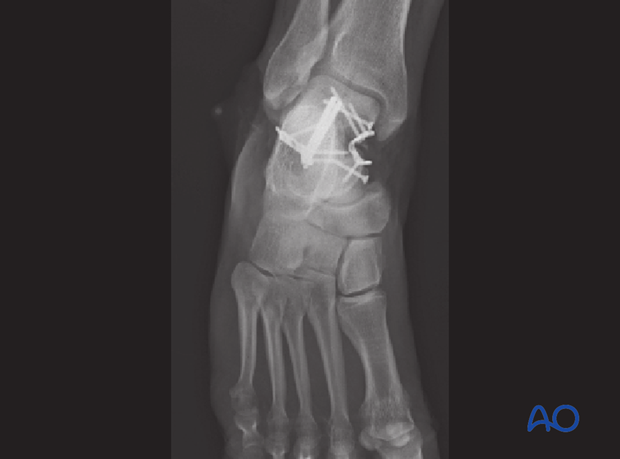
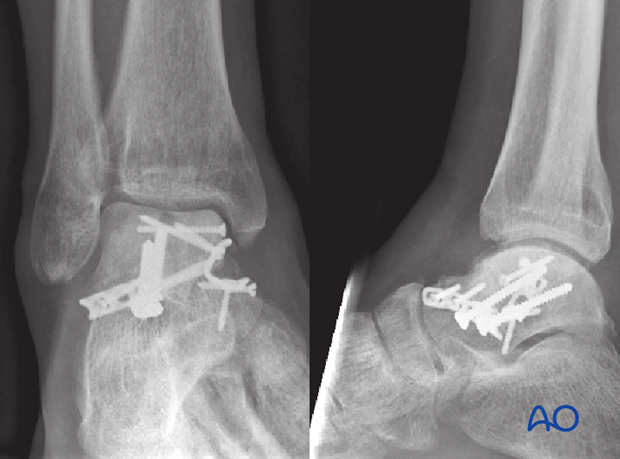
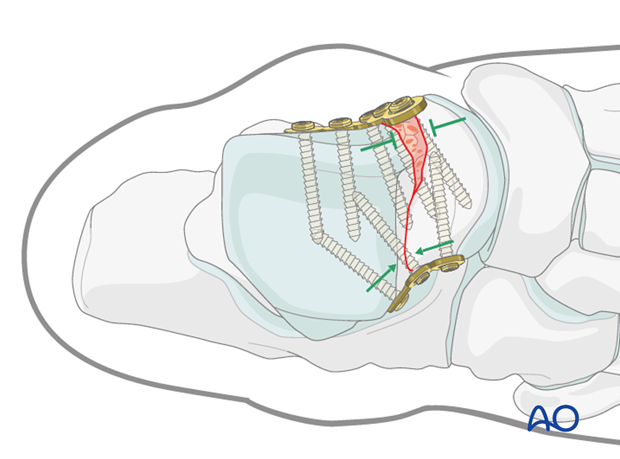
The talus is 60% articular surface, and the surgeon must be very careful that definitive screw placement does not compromise any articular surfaces.
The fixation used is mini-fragment 2.4 mm and 2.7 mm screws. The medial plate prevents loss of medial length, and the lateral plate acts as a compression plate to resist fracture gapping.
5. Aftertreatment
After surgery, a posterior splint with the foot in neutral position is applied. Early range of motion of the ankle and subtalar joint is advised.
Weight bearing should be restricted for a minimum of 8-12 weeks. Follow-up visits with x-rays should be at 2, 6 and 8, or 12, weeks.
Range-of-motion exercises are important to commence as soon as they are tolerated in order to restore a good range of motion.
Radiography at 12 weeks will confirm whether healing has occurred. Once bony union has been achieved, graduated weight-bearing can commence.
Patients with talar neck fractures should not begin weight bearing as long as there is pain at the fracture site.