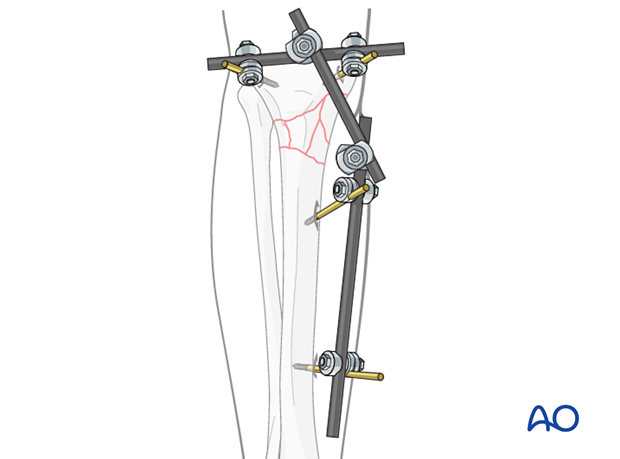
Non-bridging external fixator (definitive)
1. Principles of modular external fixation with large pins
The modular external fixator is optimal for temporary use. It is rapidly applied without need for intraoperative x-rays and can be adjusted later.
The external fixator for proximal tibial fractures consists of two partial frames, one along the tibial crest and a proximal one parallel to the joint line.
Details of external fixation are described in the basic technique for application of modular external fixator.
Specific considerations for the proximal tibia are given below.
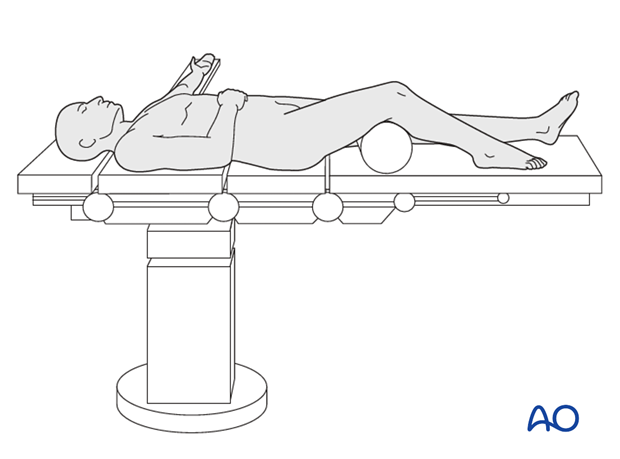
2. Patient preparation
This procedure is normally performed with the patient in a supine position.
3. Pin insertion (tibial head and shaft)
Pin placement
For safe pin placement make use of the safe zones and be familiar with the anatomy of the lower leg.
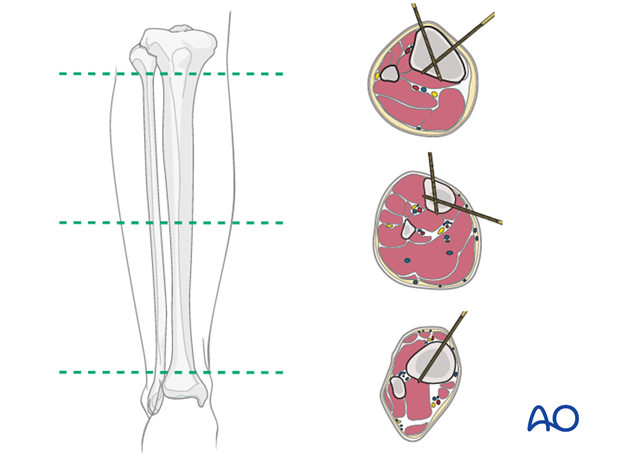
Pin insertion into proximal tibia and tibia shaft
Insert the proximal pins infradorsally to avoid the joint.
Insert the two distal pins in the sagittal plane medially to the tibial crest.
The AP direction of the pins in the proximal fragment avoids running of these pins intraarticularly. By inserting the pins in the distal fragment in an AP direction, the penetration of muscles can be avoided.
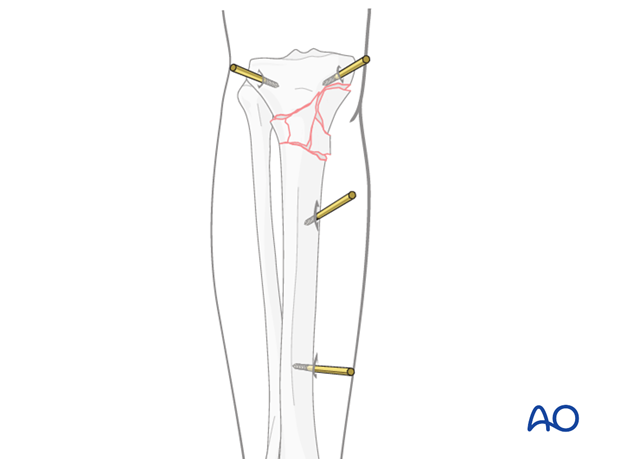
Tibial pin placement
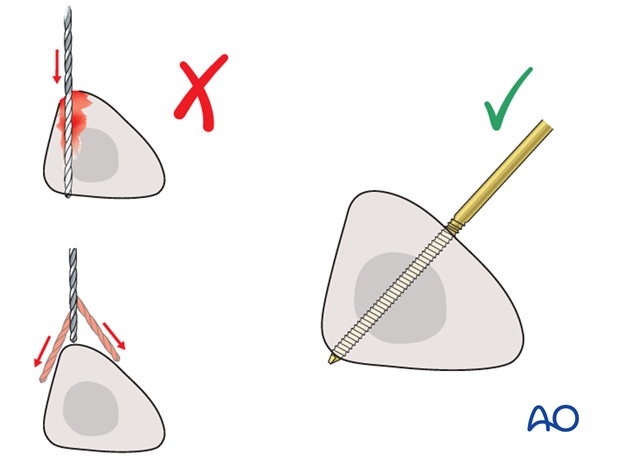
Drilling a hole in the thick tibial crest may be associated with excessive heat generation and there is a risk the drill bit may slip medially or laterally damaging the soft tissues. As the anteromedial tibial wall provides adequate thickness for the placement of pins, this trajectory is preferable. A trajectory angle (relative to the sagittal plane) of 20-60° for the proximal fragment and of 30-90° for the distal fragment is recommended.
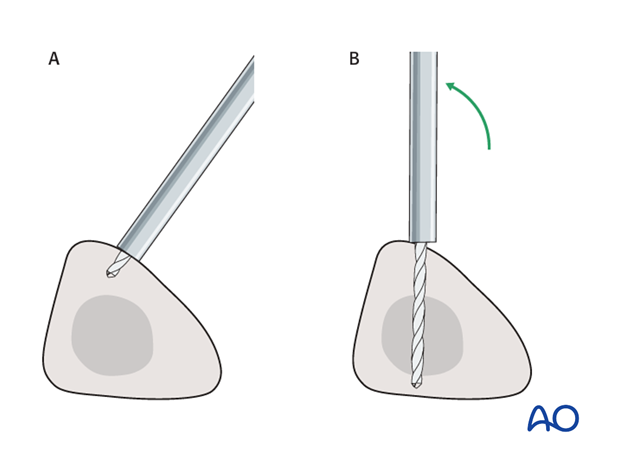
Alternatively, in order to avoid the frame catching on the opposite leg, the pins may be placed more anteriorly. The drill bit is started with the tip just medial to the anterior crest, and with the drill bit perpendicular to the anteromedial surface (A). As the drill bit starts to penetrate the surface, the drill is gradually moved more anteriorly until the drill bit is in the desired plane (B). This should prevent the tip from sliding down the medial or lateral surface.
4. Frame construction / reduction and fixation (knee)
Reduction
Using the partial frames as handles, manually reduce the fracture in length, rotation and axis.
Restore length with a bolster behind the knee to give slight flexion.
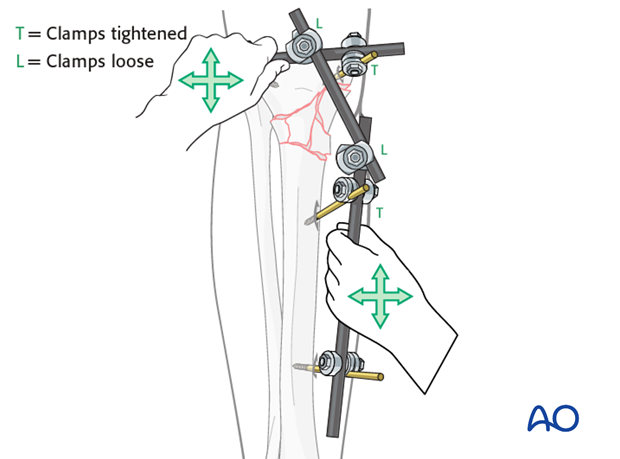
5. Aftercare following nonbridging external fixation
Compartment syndrome and nerve injury
Close monitoring of the tibial compartments should be carried out especially during the first 48 hours after surgery to rule out compartment syndrome.
The neurovascular status of the extremity must be carefully monitored. Impaired blood supply or developing neurological loss must be investigated as an emergency and dealt with expediently.
Pin-site care
Various aftercare protocols to prevent pin track infection have been established by experts worldwide. Therefore, no standard protocol for pin-site care can be stated here. Nevertheless, the following points are recommended:
- The aftercare should follow the same protocol until removal of the external fixator.
- The pin-insertion sites should be kept clean. Any crusts or exudates should be removed. The pins may be cleaned with saline and/or disinfectant solution/alcohol. The frequency of cleaning depends on the circumstances and varies from daily to weekly but should be done in moderation.
- No ointments or antibiotic solutions are recommended for routine pin-site care.
- Dressings are not usually necessary once wound drainage has ceased.
- Pin-insertion sites need not be protected for showering or bathing with clean water.
- The patient or the carer should learn and apply the cleaning routine.
Pin loosening or pin track infection
In case of pin loosening or pin track infection, the following steps need to be taken:
- Remove all involved pins and place new pins in a healthy location.
- Debride the pin sites in the operating theater, using curettage and irrigation.
- Take specimens for a microbiological study to guide appropriate antibiotic treatment if necessary.
Before changing to a definitive internal fixation an infected pin track needs to heal. Otherwise infection will result.
Mobilization
Unless there are other injuries or complications, mobilization may be performed on day 1. Static quadriceps exercises with passive range of motion of the knee should be encouraged. Early active range of motion of knee and ankle is encouraged.
Following any injury, and also after surgery, the neurovascular status of the extremity must be carefully monitored. Impaired blood supply or developing neurological loss must be investigated as an emergency and dealt with expediently.
The goal of early active and passive range of motion is to achieve as full range of motion as possible within the first 4 - 6 weeks.
Optimal stability should be achieved at the time of surgery, in order to allow early range of motion exercises.
Weight bearing
Partial weight bearing may be allowed. Weight bearing is usually avoided in the treatment of articular fractures.
The timing and how much weight may be taken through the fracture will be influenced by:
- Patient factors
- Fracture configuration
- Stability of the fixator construct
Follow up
See patient 7-10 days after surgery for a wound check. X-rays are taken to check the reduction.
Frequency of outpatient follow-up depends on the complexity of the injury and on the compliance of the patient. The follow-up visits should not be spaced more than three weeks apart.