Tension band fixation
1. Principles
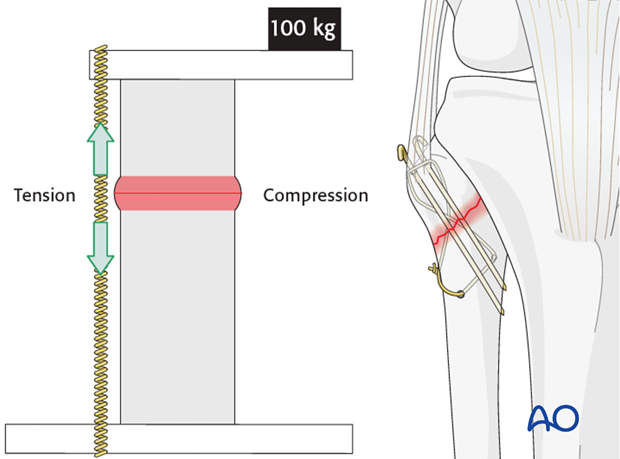
Tension band principle
A tension band converts tensile force into compression force at the opposite cortex.

This is achieved by applying a device eccentrically, on the convex side of a curved bone.
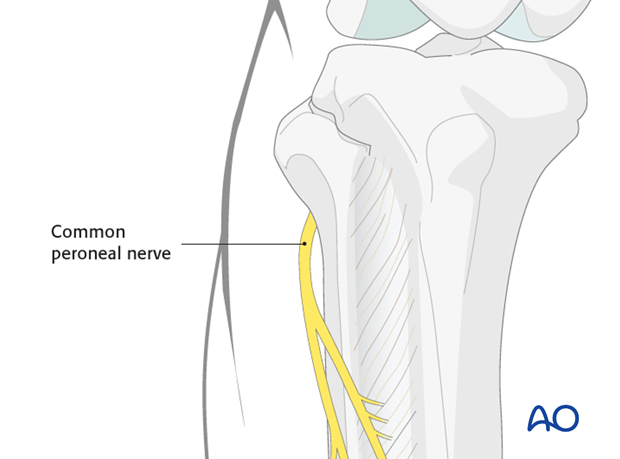
Peroneal nerve
The peroneal nerve runs around the fibular neck. So be careful with the reduction and clamp placement.
Because of the presence of the common peroneal nerve in the immediate neighborhood the choice of tension band wiring in these cases is a dangerous one.
If the fragment appears to be too small for screw fixation or if it is comminuted, tension band wiring may be indicated.
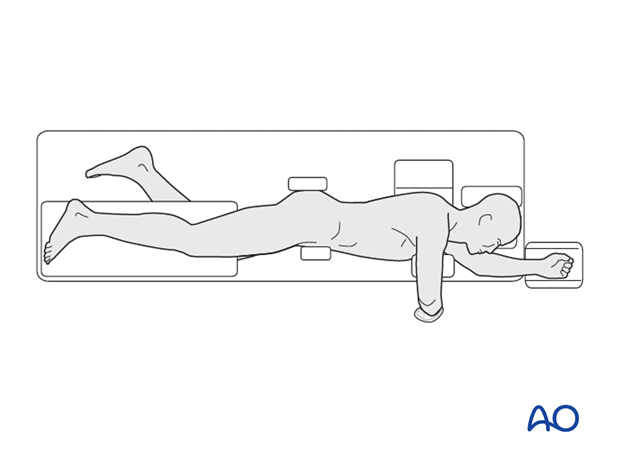
2. Patient preparation
This procedure is normally performed with the patient in a lateral position.
3. Approaches
Safe zones for percutaneous instrumentation
Inserting percutaneous instrumentation through safe zones reduces the risk of damage to neurovascular structures.
Anterolateral approach
For open reduction an anterolateral approach is used.
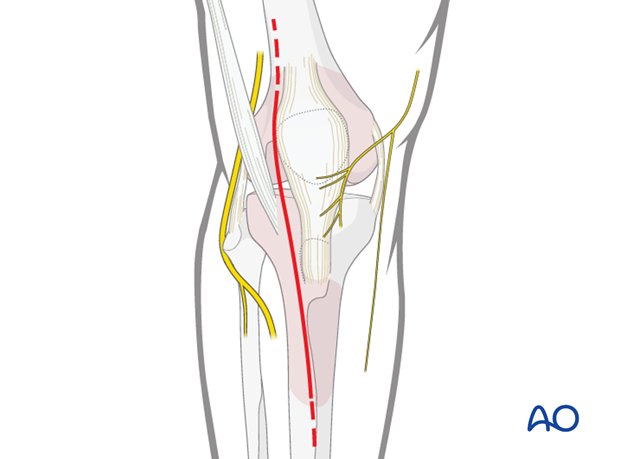
4. Reduction
After direct exposure of ligaments and the avulsed fibular head, reduction may be achieved with the use of a small clamp that is placed on the fibula and the bone fragment. Protect the peroneal nerve which runs below the tendon of biceps femoris and then winds around the fibular neck from back to front in contact with bone.
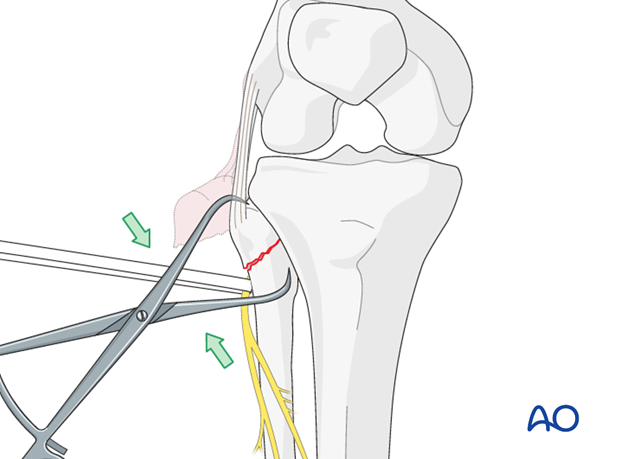
5. Fixation
Tension band wiring
If the fragment appears to be too small for screw fixation, K-wire fixation is possible in a proximal lateral to distal medial direction. In this case tension band wiring is required to fix the fracture under compression and prevent re-displacement.
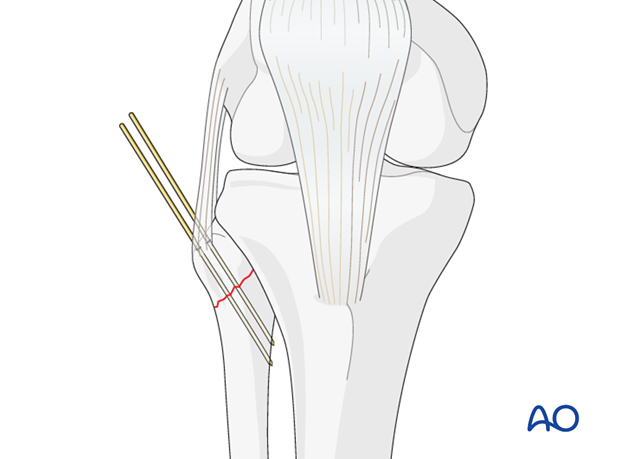
Identify the common peroneal nerve and retract it carefully.
After insertion of the K-wires a drill hole is created in the proximal fibular shaft 1.5 cm distal to the fracture. A figure-of-eight cerclage is applied.
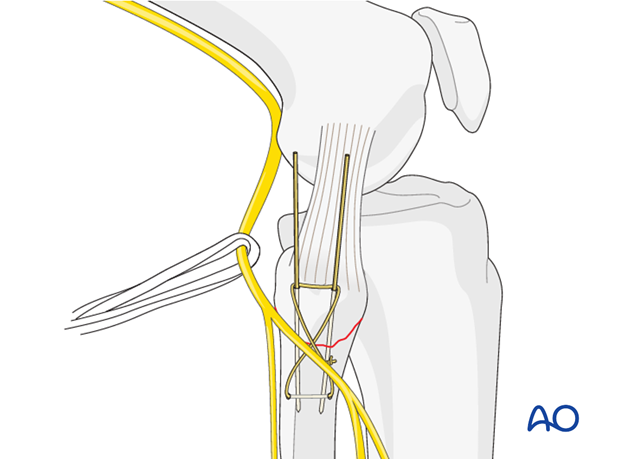
After tightening of the cerclage wire both K-wires and the cerclage are shortened.
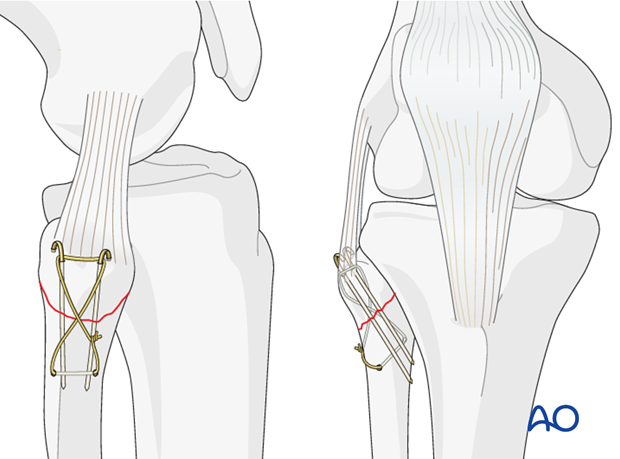
Any injury to the posterolateral corner should be repaired very early in the healing process. Residual knee instability will be the result if the posterolateral corner is not dealt with definitively at an early stage.
Secondary reconstruction provides worse results than early posterolateral corner repair (the posterolateral corner).
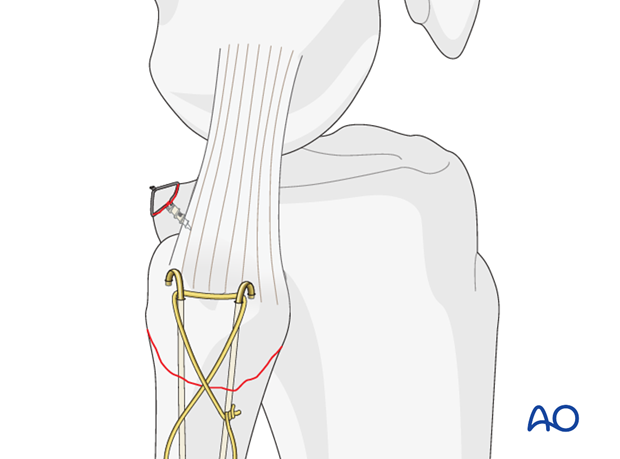
6. Aftercare
The neurovascular status of the extremity must be carefully monitored. Impaired blood supply or developing neurological loss must be investigated as an emergency and dealt with expediently.
Functional treatment
Functional treatment shall be applied for 2 – 3 days with patient still resting in bed starting on postoperative day 1.
The goal of early active and passive range of motion is to achieve a full range of motion within the first 4 – 6 weeks. Maximum stability is achieved at the time of surgery.
In noncompliant patients consider the use of a hinged knee brace.
Weight bearing
The patient can be fully weight bearing but care must be taken not to apply a varus distracting force. For this reason, crutches are advisable as a means of protection.
Follow up
Wound healing should be assessed on a short term basis within the first two weeks. Subsequently, an 8 week follow-up is usually performed.
Implant removal
Implant removal is not mandatory and should be discussed with the patient.